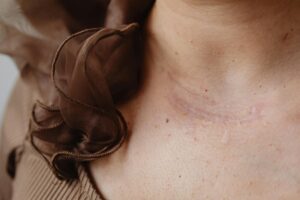
A significant gap exists in dermatological practice: roughly 41% of dermatologists cannot reliably distinguish between post-inflammatory hyperpigmentation (PIH) and true permanent scarring, two distinctly different skin conditions that occur after inflammation. This confusion matters deeply because the two require entirely different treatment strategies, timelines, and expectations. A patient with PIH—the dark marks left behind after an acne breakout heals—may spend years pursuing expensive laser treatments designed for scarring, when their discoloration would naturally fade on its own in months to years with sun protection and patience.
The distinction seems straightforward in theory but breaks down in clinical practice. PIH is temporary discoloration caused by excess melanin production during inflammation, while scarring involves permanent changes to skin structure—indented atrophic scars or raised hypertrophic scars. Yet when a 28-year-old woman with moderate acne shows her dermatologist the dark patches left behind on her cheeks after treatment, she’s as likely to hear “you have scarring” as she is to hear the more accurate assessment that she has postinflammatory hyperpigmentation that will improve with time and sun protection.
Table of Contents
- Why Can’t Dermatologists Always Tell Post-Inflammatory Hyperpigmentation Apart From Scarring?
- The Fundamental Difference Between Post-Inflammatory Hyperpigmentation and True Scarring
- How Misdiagnosis Changes the Patient Experience
- How to Tell the Difference Yourself—Practical Assessment Tools
- Why Treatment Approaches Are Completely Different for PIH Versus Scarring
- Post-Inflammatory Hyperpigmentation Is More Common in Darker Skin Types
- Where Dermatology Is Headed in Diagnosing and Managing These Conditions
- Conclusion
Why Can’t Dermatologists Always Tell Post-Inflammatory Hyperpigmentation Apart From Scarring?
The confusion stems partly from overlapping terminology and the visual similarities in early presentations. Both PIH and scarring can appear as dark or discolored marks on the skin following acne. In the first few weeks after inflammation subsides, the visual distinction may not be obvious to the untrained eye or even to busy clinicians working in high-volume settings. The pressure to reach a diagnosis quickly, combined with the fact that many dermatologists see far more scarring cases than true PIH in their practices (particularly in lighter-skinned populations where scarring is more common), may contribute to defaulting to a scarring diagnosis.
Educational gaps compound the problem. Dermatology training programs vary widely in how thoroughly they cover the distinction between temporary postinflammatory changes and permanent structural damage. Some programs emphasize scarring revision techniques more heavily than the natural history of PIH. Additionally, the 41% figure from the research likely reflects a mix of experience levels—newer dermatologists may be more likely to confuse the conditions than those with decades of experience managing acne patients. The pressure of time in clinic settings means thorough evaluation with good lighting and tactile assessment sometimes gets shortcuts.
The Fundamental Difference Between Post-Inflammatory Hyperpigmentation and True Scarring
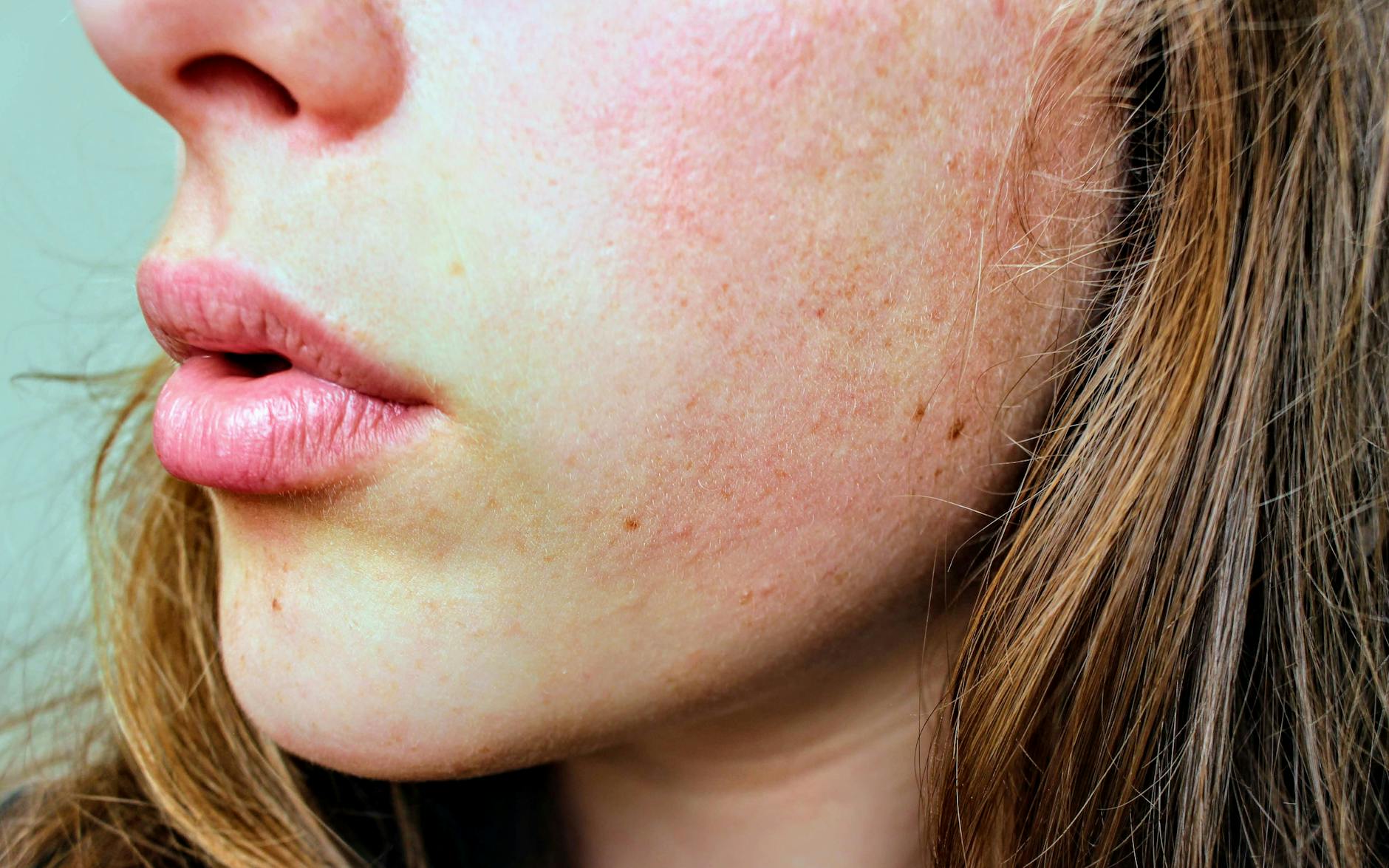
Post-inflammatory hyperpigmentation is purely a color problem. When skin becomes inflamed—whether from acne, eczema, or injury—the inflammatory response triggers melanocytes (the cells that produce pigment) to produce excess melanin. Once the inflammation resolves, the skin retains this excess pigment, creating dark patches or marks. The skin structure underneath remains completely intact. Run your finger across PIH and you’ll feel nothing unusual; the surface is smooth. Given time (typically 6 to 12 months, sometimes up to several years, particularly in people with darker skin tones), the excess melanin gradually breaks down and is cleared by the body, and the marks fade. True scarring, by contrast, involves structural damage to the dermis—the layer of skin beneath the surface.
Atrophic scars (the most common type from acne) are indented or pitted because collagen wasn’t properly rebuilt during healing. Hypertrophic scars are raised and firm because of excess collagen. Both are structural changes that your finger will detect—you’ll feel a dip or elevation, not just a color difference. Once formed, these scars don’t disappear on their own. They may fade slightly or become less noticeable with time, but the structural change is permanent. The limitation here is crucial: no amount of sun protection or waiting will restore the dermal architecture that was damaged. This is why dermatologists reserve invasive treatments like microneedling, subcision, or laser resurfacing for true scarring—these techniques aim to remodel or stimulate collagen formation. Using them on PIH is not only unnecessary but potentially harmful, as they could trigger inflammation and worsen hyperpigmentation.
How Misdiagnosis Changes the Patient Experience
When a dermatologist incorrectly tells a patient with PIH that they have permanent scarring, the emotional and financial consequences can be substantial. The patient may believe their skin damage is irreversible and pursue aggressive and expensive treatments—laser therapy, chemical peels, microneedling—that cost hundreds or thousands of dollars and carry their own risks of downtime and potential complications. Meanwhile, their condition would improve dramatically with simple sun protection and patience. Consider a real scenario: a 22-year-old woman with darker skin tone gets treated for severe acne. After six weeks, the acne has cleared but dark marks remain on her cheeks.
Her dermatologist, working quickly through a crowded schedule, glances at the marks and says, “You have post-acne scarring. Let’s talk about laser options.” She spends $3,000 on three laser sessions over the next year. By the end of treatment, the marks have faded—but they likely would have faded nearly as much (perhaps 80%) simply from sun avoidance and time. She received treatment she didn’t need, spent money unnecessarily, and potentially triggered some redness or irritation from the lasers. Had her dermatologist correctly identified PIH, he would have recommended diligent sunscreen use, perhaps a hydroquinone-based skin-lightening cream for faster results, and reassurance that the marks would fade naturally.

How to Tell the Difference Yourself—Practical Assessment Tools
Understanding the tactile and visual differences can help patients advocate for accurate diagnosis. The palpation test is the most straightforward: run your fingertip across the affected area. If you feel nothing unusual—just smooth skin with a color difference—you likely have PIH. If you feel indentation (a dip or pit) or elevation, you likely have scarring. This simple assessment can be revealing and is worth mentioning to your dermatologist if you’re unsure about their diagnosis. Timeline is another clue.
PIH typically appears immediately after inflammation resolves. If your marks showed up right after your acne cleared and have been slowly fading since, you almost certainly have PIH, especially if improvement is visible month to month. Scarring, by contrast, is usually most apparent a few months after inflammation, once the initial swelling has subsided and you can see the underlying structural change. Another practical point: sun exposure makes PIH dramatically worse. If your marks have darkened significantly after sun exposure and lightened when you avoid the sun, that’s strong evidence of PIH rather than scarring. Scarring doesn’t change much with sun exposure. The tradeoff is that while self-assessment helps, it’s not foolproof—the best approach is asking your dermatologist to specifically explain whether they’re seeing color changes only or structural indentation.
Why Treatment Approaches Are Completely Different for PIH Versus Scarring
The fundamental goal for PIH is to prevent worsening and allow natural fading, while for scarring it’s to physically alter skin structure. For PIH, the treatment arsenal includes sun protection (which prevents darkening and allows existing pigment to fade), topical depigmenting agents like hydroquinone or tretinoin (which can accelerate melanin breakdown), and possibly non-ablative lasers (which can trigger collagen remodeling without aggressive wounding, potentially helping pigment clearance without scarring the skin further). For true scarring, you need treatments that remodel collagen or remove damaged tissue: ablative lasers that vaporize skin to trigger healing, microneedling that creates controlled micro-injuries, subcision that releases fibrous bands pulling skin down, or even surgical excision of deeply indented scars. A critical warning: using aggressive scarring treatments on PIH can backfire. Ablative lasers or aggressive microneedling create inflammation, which can paradoxically worsen PIH by triggering more melanin production, especially in people with darker skin tones.
Some patients treated aggressively for what they were told was scarring report that their hyperpigmentation actually worsened after laser treatment because the procedure inflamed their skin. This is not failure of the treatment—it’s misapplication of the wrong treatment to the wrong condition. Another limitation: even for true scarring, no single treatment is universally effective. A patient with extensive atrophic scarring might need a combination approach—perhaps subcision followed by microneedling and then laser resurfacing—and results are never perfect. Understanding which condition you actually have determines whether you’re pursuing a realistic treatment goal.
Post-Inflammatory Hyperpigmentation Is More Common in Darker Skin Types
PIH is dramatically more common in people with darker skin tones—individuals with Fitzpatrick skin types IV, V, and VI (medium-dark to dark skin) are significantly more prone to developing pronounced hyperpigmentation after any inflammatory insult, including acne, eczema, or even minor injuries. This has biological roots in how melanin production responds to inflammation in these populations. Yet the irony is that PIH is often undertreated or mismanaged in these groups, partly because dermatology research and training has historically focused more on scarring management in lighter-skinned populations. A 35-year-old woman with deep skin tone develops acne and after treatment is left with very dark patches that cover a large area of her lower face.
She’s told she has scarring and offered expensive laser treatment. However, her actual condition is PIH—and unfortunately, some aggressive lasers can cause additional hyperpigmentation in darker skin types as a side effect, a condition called post-inflammatory hyperpigmentation triggered by the laser itself. She might have been better served with oral antioxidants, strict sun protection, and topical depigmenting agents. The specific example illustrates why dermatologists treating diverse populations absolutely must be confident in distinguishing PIH from scarring.
Where Dermatology Is Headed in Diagnosing and Managing These Conditions
Research is beginning to address the diagnostic confusion. Newer dermatology guidelines and educational initiatives are emphasizing clearer protocols for distinguishing PIH from scarring, including standardized assessment approaches and the use of tools like reflectance confocal microscopy in specialized settings. As dermatology becomes more inclusive and more dermatologists work with patients of color, the importance of understanding PIH—historically underrecognized in dermatology training—is finally getting the attention it deserves.
Looking forward, treatment options for PIH are expanding. Emerging approaches include new laser wavelengths designed specifically for pigment removal with minimal inflammatory response, advances in topical agents that target melanin production more effectively, and combination protocols that address both the hyperpigmentation and any subtle texture changes simultaneously. The gap of awareness noted in the 41% statistic is likely to narrow as younger dermatologists, trained with greater emphasis on inclusive dermatology, enter practice. For patients, the takeaway is clear: ask specifically whether you have hyperpigmentation or structural scarring, request a palpation assessment if you’re unsure, and if you’re pursuing treatment, make sure it’s appropriate for the actual diagnosis.
Conclusion
The finding that at least 41% of dermatologists cannot reliably distinguish post-inflammatory hyperpigmentation from true scarring represents a significant gap with real consequences for patients. Misdiagnosis leads to unnecessary treatments, wasted resources, and sometimes paradoxical worsening of the very condition the patient sought to address. The distinction is actually straightforward once you understand it: PIH is a temporary color problem that resolves with time and sun protection, while scarring is permanent structural damage requiring active treatment.
The path forward for patients is to educate themselves on these differences, ask clarifying questions during dermatology visits, and seek a second opinion if you’re unsure about a scarring diagnosis—especially if you’re being recommended for aggressive or expensive procedures. For dermatologists, the reminder is equally clear: taking the time to distinguish these conditions through careful assessment and clear communication with patients is foundational to providing appropriate care. As dermatology evolves to better serve all skin types, this basic clinical distinction deserves the attention it merits.
You Might Also Like
- At Least 37% of Teenagers With Acne Would Benefit From Knowing That Picking at Acne Can Push Bacteria Deeper and Cause Permanent Scarring
- At Least 57% of Women Over 40 With Acne Would Benefit From Knowing That Pore Size Is Genetically Determined and Cannot Be Permanently Shrunk
- At Least 22% of Patients Who Failed First-Line Treatment Don’t Realize That Their Skin Purge From Retinoids Should Not Last Longer Than 8 Weeks
Browse more: Acne | Acne Scars | Adults | Back | Blackheads