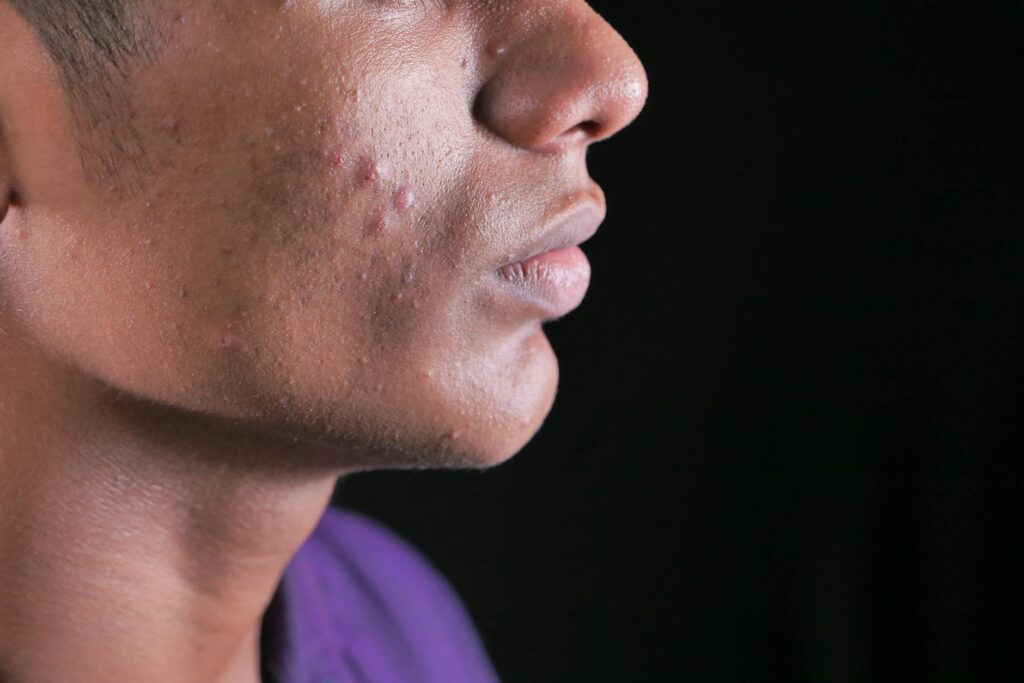
At 67 years old, a man who had endured acne for five decades finally found the solution in isotretinoin, a medication that cleared his persistent skin condition within six months. His case demonstrates that acne isn’t exclusively a teenage problem—it can follow people into their later years, and when it does, it can have the same frustrating impact on quality of life as it does for adolescents. This man’s experience wasn’t unique; stubborn adult-onset acne and long-term persistent acne affecting older adults is more common than many realize, often dismissed or overlooked because it doesn’t fit the stereotype of acne as a young person’s concern. For someone who had battled acne since his late teens, the prospect of living with it indefinitely seemed inevitable.
Conventional treatments had failed over the decades—topical retinoids, antibiotics, and various combination therapies provided only temporary relief or minimal results. When isotretinoin was finally prescribed, the transformation was remarkable: within six months, the chronic inflammation that had marked his skin for fifty years had resolved, and he experienced clear skin for perhaps the first time since adolescence. This outcome highlights an important reality in dermatology: isotretinoin remains the only medication capable of producing long-term remission or complete cure of severe acne, regardless of the patient’s age. For older adults with resistant acne, the medication can be genuinely transformative, though it requires careful consideration of the unique factors that apply to aging patients taking powerful systemic medication.
Table of Contents
- Can Severe Acne Really Last 50 Years and Respond to Isotretinoin at 67?
- Why Isotretinoin Works When Nothing Else Does for Long-Term Severe Acne
- The Reality of Starting a Six-Month Treatment Course at 67
- Isotretinoin in Older Adults: Different Risks, Different Benefits
- Managing Side Effects and Safety Monitoring During a Six-Month Course
- The Timeline: Why Six Months Mattered for This Patient
- Life After Isotretinoin: Long-Term Outcomes for Older Adults
- Conclusion
- Frequently Asked Questions
Can Severe Acne Really Last 50 Years and Respond to Isotretinoin at 67?
Yes, and this pattern is more common than you might think. Some people experience acne continuously from their teenage years through middle age and beyond, particularly if they have underlying hormonal sensitivities, genetic predisposition, or underlying conditions like polycystic ovary syndrome (in women) or other endocrine issues. For men, persistent acne can be driven by sustained androgen sensitivity of the sebaceous glands, meaning the skin remains responsive to hormonal signals that trigger oil production and follicle clogging throughout their lives. Isotretinoin, the active ingredient in medications like Accutane, is a retinoid that works by reducing sebaceous gland size and permanently altering how the skin produces oil. Unlike other acne medications that suppress acne while you’re taking them and often allow it to return once you stop, isotretinoin has the potential to produce lasting remission because it changes the underlying biology of the skin.
Studies show that about 70-80% of patients who complete a full course of isotretinoin experience either complete clearance that persists long-term or a significant reduction in acne severity that doesn’t bounce back. For someone who had endured acne for fifty years, this medication represented a fundamentally different approach—not just suppression, but potential cure. The fact that this patient was 67 when starting treatment is medically notable. Isotretinoin was not available when he was a young adult—the drug was first approved by the FDA in 1982—so he had simply never had access to it during the decades when conventional therapies were failing him. By the time he finally had the opportunity to try it, he had spent decades with a condition that was both physically uncomfortable and psychologically taxing.

Why Isotretinoin Works When Nothing Else Does for Long-Term Severe Acne
Isotretinoin’s mechanism is fundamentally different from other acne treatments. While oral antibiotics kill acne-causing bacteria and topical retinoids increase cell turnover, isotretinoin shrinks the sebaceous glands themselves and reduces sebum production by as much as 90%. This reduction is often permanent or semi-permanent, even years after treatment ends. For severe acne driven primarily by excess oil production, this addresses the root cause rather than just managing symptoms. However, isotretinoin comes with significant limitations and serious potential side effects that demand careful medical supervision. The most well-known concern is teratogenicity—the drug causes severe birth defects and miscarriage if used during pregnancy, which is why women of childbearing age in the U.S.
must enroll in iPLEDGE, a strict risk minimization program requiring monthly pregnancy tests and contraception. For older patients like the 67-year-old in this case, this particular concern doesn’t apply, but other side effects absolutely do: severe dry skin and lips, potential liver enzyme elevations, elevated triglycerides and cholesterol, and rarely, inflammatory bowel disease or mood changes. For an older patient, there’s an additional consideration: isotretinoin can interact with medications commonly taken by people in their 60s and beyond. Patients on blood thinners, certain statins, or other systemic medications need careful monitoring and sometimes medication adjustments. The cumulative dose of isotretinoin matters too—higher total doses are associated with better long-term clearance but also greater risk of side effects. This patient’s treatment protocol would have been individualized based on his medical history, liver function, lipid levels, and concurrent medications.
The Reality of Starting a Six-Month Treatment Course at 67
Beginning a six-month course of isotretinoin at 67 means committing to frequent medical appointments and lab work. blood tests are typically required before starting, then monthly throughout treatment to monitor liver function and lipid levels. For isotretinoin to be prescribed legally in the U.S., the patient must have documented proof of two negative pregnancy tests (for women) or enrollment in iPLEDGE (the system tracks all prescriptions), dermatology visits, and baseline lab work. While the monitoring burden is real, the payoff for someone who has suffered with acne for fifty years can be immense. The six-month timeframe in this case is typical for a standard course, though some patients need longer and others clear faster. During the treatment period, acne may temporarily worsen—a phenomenon called “retinization” or an initial acne flare—because the medication is essentially purging the skin of deeply embedded comedones.
This patient would have experienced increasing dryness, peeling, and potentially uncomfortable flaking, especially on the face and lips. Many patients also experience dryness of the eyes and inside the nose. These side effects, while uncomfortable, are manageable with consistent moisturizing, lip balm, and sometimes artificial tears. At 67, this patient’s skin would have also been dealing with age-related changes—reduced elasticity, sun damage, thinner epidermis—on top of the effects of isotretinoin. This combination required particularly diligent sun protection during treatment, as the skin is more photosensitive on isotretinoin, and healing is slower in older skin. The fact that his acne still responded so dramatically suggests his skin’s fundamental problem was sebaceous gland overactivity, not age-related changes, which is why the treatment was so effective.

Isotretinoin in Older Adults: Different Risks, Different Benefits
Prescribing isotretinoin to patients in their 60s and beyond requires a different risk-benefit analysis than prescribing it to teenagers. Older patients generally have lower baseline sebaceous gland activity and may not need as high a total cumulative dose to achieve remission. On the other hand, they’re more likely to have comorbidities—high cholesterol, liver issues, kidney disease—that complicate treatment. They’re also more likely to be taking multiple medications, some of which interact with isotretinoin. The tradeoff for this patient was significant: six months of uncomfortable dryness and frequent doctor visits versus the potential for five decades of clear skin ahead.
At 67, if the treatment worked, he had realistic hope of remaining acne-free for the rest of his life. For a 16-year-old with acne, the same medication offers the same biological benefit, but the psychosocial context is different—teenage acne is a more urgent quality-of-life issue in many cases, affecting social development and self-image during formative years. For an older adult, the relief from chronic acne can still be profound and affect self-confidence and comfort in daily life. Another practical consideration: older patients often have more realistic expectations and better compliance with treatment protocols. This patient had fifty years of failed treatments to motivate his commitment to doing isotretinoin correctly, following all lab work requirements, and managing side effects. Non-compliance is a real problem in younger patients sometimes, but this demographic typically understands the gravity of the treatment and why monthly monitoring exists.
Managing Side Effects and Safety Monitoring During a Six-Month Course
The most common and challenging side effect of isotretinoin is severe skin dryness. This patient likely experienced chapped lips that became uncomfortable or even painful, dry patches on his face and body, and potentially dry eyes. Managing this requires religious use of thick moisturizers (often dermatologists recommend petroleum jelly, ceramide-rich creams, or prescription-strength products), continuous lip balm use, and sometimes artificial tear drops. The dryness can be relentless for six months, and for someone in their 60s whose skin is already naturally less oily than younger skin, this adjustment can be significant. A critical limitation of isotretinoin is the potential for elevated triglycerides and cholesterol, which can occur in up to 25% of patients. For a 67-year-old, especially one who might already have cardiovascular risk factors, this requires baseline lipid testing and repeat testing monthly or every other month during treatment.
If lipid levels rise significantly, the dose may be reduced or treatment paused. Similarly, liver enzymes can elevate in some patients, though serious liver toxicity is rare. This patient would have required regular blood work interpretation and coordination between his dermatologist and primary care doctor if lipid management was complicated. A serious but rare side effect that has been reported is mood changes, including depression and suicidal ideation. The causal relationship remains debated in the medical literature, but the risk is serious enough that patients and caregivers are advised to watch for mood changes, increased anxiety, or thoughts of self-harm. For an older patient, distinguishing between drug-related mood changes and age-related depression or other factors can be more complex, making informed monitoring essential.

The Timeline: Why Six Months Mattered for This Patient
The six-month duration of isotretinoin treatment is standardized based on research showing that most patients achieve adequate clearance within this timeframe when cumulative dosing is appropriate. Cumulative dose, not just duration, is what matters—the total amount of isotretinoin a patient receives over the entire course. Dermatologists typically aim for a cumulative dose of 120-150 mg/kg of body weight for optimal long-term remission. A patient weighing 80 kg, for example, would need a total of 9,600-12,000 mg over the course of treatment. For this 67-year-old patient, six months likely represented the optimal window for his specific dose and situation.
Earlier cessation might have left his acne vulnerable to recurrence, while extending beyond six months would have increased cumulative side effects without proportional additional benefit. The fact that his acne completely cleared within this timeframe suggests his dermatologist carefully calibrated the dose to his age, weight, and tolerance level. Within the first few weeks, patients often experience an initial acne flare as the medication begins working and purging the skin. By the third month, most patients begin seeing significant improvement. This patient would have likely seen dramatic clearing by month four or five, with complete or near-complete resolution by month six.
Life After Isotretinoin: Long-Term Outcomes for Older Adults
For patients who achieve clear skin on isotretinoin, the results often persist long-term. Studies tracking patients five or more years after completing treatment show that about 70-80% either remain clear or experience only very mild acne that doesn’t require systemic treatment. This is remarkably different from other acne medications, which typically require continued use to maintain results. For this 67-year-old, the six-month investment offered a genuine possibility of remaining acne-free for the rest of his life.
The long-term outlook after isotretinoin also includes ongoing attention to skincare. Clear skin after isotretinoin still requires sun protection—cumulative sun exposure over decades contributes to skin aging and can complicate healing. This patient would benefit from daily sunscreen use not just for acne prevention but for general skin health and cancer prevention at his age. Beyond sun protection, a gentle cleanser and appropriate moisturizer are typically all older skin needs after isotretinoin clears acne, since many of the aggressive acne treatments used before isotretinoin can be discontinued.
Conclusion
The case of a 67-year-old man clearing fifty years of acne with isotretinoin in six months demonstrates that severe, persistent acne isn’t automatically a lifelong condition, regardless of age. When conventional treatments have failed over decades, isotretinoin remains the most effective and potentially curative option available. For older adults, the medication requires careful medical oversight and realistic expectations about side effects, particularly skin dryness and the need for frequent lab monitoring, but the potential benefit—clear skin for the remaining years of life—can be genuinely transformative.
If you’ve experienced chronic acne that has resisted conventional treatments, either since adolescence or as a newer problem in adulthood, a consultation with a dermatologist experienced in prescribing isotretinoin is worth considering. The medication isn’t without risks, and it’s not appropriate for everyone, but for carefully selected patients with severe, persistent acne, it offers a level of efficacy no other treatment can match. This patient’s experience is a reminder that acne at any age deserves appropriate treatment, and that solutions exist even when the problem has persisted for decades.
Frequently Asked Questions
Can you get isotretinoin prescribed if you’re older than 60?
Yes. Age alone isn’t a contraindication to isotretinoin. However, older patients need careful evaluation of liver and kidney function, lipid levels, and current medications to ensure safety. The prescription process is the same as for younger patients, including enrollment in iPLEDGE and monthly lab monitoring.
How long does it take to see results with isotretinoin?
Most patients see significant improvement by the third month of treatment and substantial clearing by month four or five. The full effect and maximum improvement often continue to emerge even after the course ends, with final results typically assessed a few weeks after the last dose.
Will acne come back after isotretinoin treatment?
In about 70-80% of patients, acne either doesn’t return or returns in a much milder form that doesn’t require the same level of treatment. Complete recurrence requiring another isotretinoin course happens in 10-20% of cases. Most people who need treatment again can manage with topical retinoids or other less intensive options.
What are the most common side effects of isotretinoin?
Severe dry skin and lips are the most common and persistent side effects. Other frequent side effects include dry eyes, dry nose, and potential muscle aches. More serious but less common side effects include elevated cholesterol and liver enzyme elevations, which is why monthly lab work is required.
Is isotretinoin safe for people taking other medications?
Some medications interact with isotretinoin, and many common medications taken by older adults (certain blood thinners, some statins, some psychiatric medications) require monitoring or adjustment. Your dermatologist will review all medications before prescribing and coordinate with your other doctors if needed.
Why wasn’t this patient prescribed isotretinoin decades earlier?
Isotretinoin wasn’t approved by the FDA until 1982, and early prescribing was reserved for the most severe cases of cystic acne. Insurance approval and physician willingness to prescribe it have expanded over the decades, but many patients with persistent acne still spend years trying other treatments first. Earlier access to the drug might have changed this patient’s outcome significantly.
You Might Also Like
- She Was 48 When She Had Menopausal Acne and Was Prescribed Hormone Replacement Therapy That Cleared It
- She Was 24 When She Had Acne Since Age 12 and Had Never Seen a Dermatologist Due to Cost
- He Was 37 When He Finally Got Insurance That Covered Dermatology…Acne Cleared in 8 Weeks After Decades of Struggling
Browse more: Acne | Acne Scars | Adults | Back | Blackheads