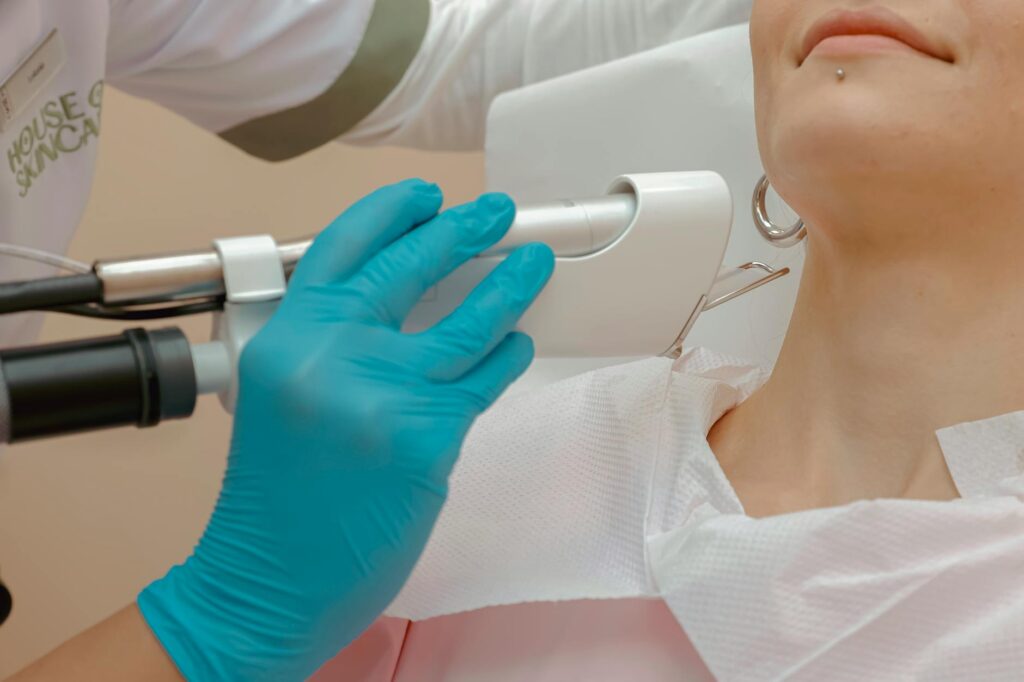
New sebaceous gland ablation devices using FDA-approved 1726 nm laser technology have entered clinical trials with impressive results: 87% of patients achieve clear or nearly clear skin at three months, with 93% maintaining those results at 12 months. These devices—including AviClear from Cutera and Accure from Accure Acne—promise to permanently reduce oil production in treated areas by destroying the glands responsible for acne. However, the word “permanently” requires important context: while the reduction is dramatic and durable, clinical evidence shows that roughly 16 to 20% of patients experience relapse within a year, suggesting that sebaceous glands retain some regenerative capacity. The appeal is straightforward.
For people with oily skin and persistent acne, a treatment that actually reduces the source of the problem—excess sebum—rather than just managing symptoms is genuinely novel. Traditional acne treatments work on the surface: antibiotics kill bacteria, retinoids unclog pores, hormonal treatments lower androgen levels. These new devices take a different approach entirely. They use laser energy to selectively heat and destroy sebaceous glands, sometimes reducing inflammatory lesions by 90% and allowing 56% of patients to stop taking acne medications entirely.
Table of Contents
- How Do FDA-Approved Sebaceous Gland Ablation Devices Work?
- What the Clinical Trials Actually Show
- FDA-Approved Options: AviClear and Accure
- Is This Treatment Right for Your Acne?
- The Permanence Problem: What Research Actually Shows
- Safety Profile and What to Expect During and After Treatment
- The Future of Sebaceous Gland Reduction Therapy
- Conclusion
How Do FDA-Approved Sebaceous Gland Ablation Devices Work?
The technology relies on selective photothermolysis—a principle where light at a specific wavelength is absorbed by a specific target without damaging surrounding tissue. The 1726 nm wavelength was chosen because sebaceous glands absorb this infrared light efficiently, while the epidermis and dermis pass most of it through. When the laser heats the glands to around 70°C, the tissue denatures and the gland’s ability to produce sebum is permanently compromised. The treatment is typically performed as a series of sessions—usually four monthly treatments for the laser-based devices—and focuses on acne-prone areas like the face, chest, and back.
What makes this different from older ablation methods is precision and tolerability. Older electrothermolysis approaches destroyed sebaceous glands with radiofrequency energy, but caused more thermal damage to surrounding skin. The 1726 nm lasers are gentler: patients report mild redness and swelling that resolves within hours to days, not the extended downtime of older techniques. This matters practically. Someone can have a treatment during lunch and return to work with minimal visible effects. The procedure works across a range of skin tones (Fitzpatrick types II through VI in the clinical trials), which is significant because acne treatments historically haven’t worked equally well for all skin types.

What the Clinical Trials Actually Show
The AviClear trials enrolled 104 patients with moderate-to-severe acne across darker and lighter skin types. By 12 weeks post-treatment, 79% had a 50% or greater reduction in inflammatory lesions. At 26 weeks, 87.3% showed at least 50% reduction. By the 52-week mark, nearly 68% of patients achieved a “clear” or “almost clear” rating on the Investigator’s Global Assessment scale. These aren’t marginal improvements.
For someone suffering with moderate-to-severe acne, a two-thirds chance of clear skin after four laser sessions is significant. The Accure trials, which used the same 1726 nm wavelength, showed similar patterns: 100% of patients achieved 50% lesion reduction at 12 weeks post-treatment, though this responder rate dropped slightly to 88% at 52 weeks. The fact that some patients lose ground over time is important context. It suggests that while the initial destruction of glands is effective, the body’s natural healing response can partially regenerate what was destroyed. This isn’t failure—68% clear skin at one year is still far better than what most people achieve with conventional acne treatments—but it’s not the same as the permanent destruction the marketing might suggest.
FDA-Approved Options: AviClear and Accure
Two devices currently have FDA approval for this technology. AviClear, made by Cutera, is the more widely available option and has the larger clinical dataset. The Accure system, from Accure Acne, uses the same wavelength but a different delivery mechanism. Both work, and both show similar efficacy rates, but they’re not identical. AviClear’s data includes longer follow-up (52 weeks for most patients), while Accure’s published data focuses on the 12-week period where efficacy is highest.
The practical difference matters if you’re considering treatment. AviClear is available in more dermatology clinics and aesthetic practices across North America, which means you have more options for treatment and more practitioners with experience using it. Accure is newer to market and less widely available, though this is changing as adoption increases. Cost, availability, and provider experience should all factor into your decision. Neither device is inexpensive—treatments typically run $3,000 to $5,000 for a series—so availability and comfort with your provider matters.

Is This Treatment Right for Your Acne?
Sebaceous gland ablation works best for people with moderate-to-severe acne who have already tried conventional treatments. If you have mild acne, starting with a retinoid, benzoyl peroxide, and possibly a hormonal treatment is more practical and less expensive. The laser-based devices make sense when conventional approaches have failed, or when your acne significantly impacts your quality of life. The trial population consisted of people who had moderate-to-severe acne and had generally tried other treatments first. Age matters too, though not in the way you might expect.
The clinical trials included adults, and the glands targeted are mature oil-producing glands. Teenagers with severe acne could theoretically benefit, but most dermatologists recommend trying conventional treatments first because of cost and because teenage acne sometimes resolves naturally as hormones stabilize. For adults—particularly those in their 20s, 30s, and beyond—with persistent acne and high sebum production, this treatment offers genuine relief. One notable benefit: 56% of patients in older studies became medication-free after gland ablation, meaning they could stop taking oral antibiotics, isotretinoin, or hormonal birth control. That’s a meaningful reduction in systemic medication burden.
The Permanence Problem: What Research Actually Shows
Here’s where marketing and reality diverge. The title promises “permanently reduces oil production,” and that’s technically true—the destroyed glands don’t grow back in their original form. But “permanently” doesn’t mean “forever in 100% of cases.” Research on older sebaceous gland ablation using electrothermolysis found that 16.7% of patients had clinically evident relapse one year after treatment. More recent 2023 research reveals why: sebaceous glands have regenerative capacity mediated by stem cells in the hair follicle bulge. Even when you destroy a sebaceous gland, the surrounding tissue contains progenitor cells that can generate new glandular tissue over time.
This is important to understand before you invest in treatment. If you’re expecting zero oil production for the rest of your life, you’ll be disappointed. The more accurate description is that these devices provide sustained, durable reduction in oil production and acne lesions for most people (around 80%) for at least a year. Some patients maintain clear skin for longer, while others see gradual return of acne over 12-24 months. This doesn’t make the treatment a failure—it’s still far superior to managing acne with daily medications—but it means some people may need a touch-up treatment every couple of years. You should discuss relapse likelihood and maintenance options with your dermatologist before committing to treatment.

Safety Profile and What to Expect During and After Treatment
The safety data from 52-week follow-up shows no severe adverse reactions in any of the trial participants. The mild side effects—erythema (redness) and edema (swelling)—resolve within hours to days. Some patients report mild discomfort during the procedure, though the laser pulses are quick. You won’t develop permanent scarring or nerve damage from these devices the way you might from older ablation methods. This is crucial because it means the barrier to trying the treatment is primarily financial, not medical.
The post-treatment timeline is straightforward: expect redness and possible mild swelling immediately after. You can return to normal activities the same day. Avoid intense exercise, saunas, and very hot water for a few days. Sun protection is essential because the treated skin is more susceptible to sun damage immediately post-procedure. Most people require four monthly treatments, with results improving over the course of those four months and continuing to improve for several months after the final treatment. By week 26 (roughly six months total from the first treatment), you’ll have a clear picture of how well the treatment worked for you.
The Future of Sebaceous Gland Reduction Therapy
The 1726 nm laser approach appears to have staying power. More devices are entering clinical trials using the same wavelength, and some manufacturers are refining the delivery to target specific gland depths or sizes more selectively. There’s also emerging interest in combining gland ablation with other acne treatments—for example, using the laser to reduce oil production while continuing a retinoid to address remaining comedones and post-inflammatory hyperpigmentation. The combination approach might improve outcomes for people with severe scarring or resistant acne.
One significant limitation remains: this technology still targets only gland destruction, not the bacterial or inflammatory components of acne. For people with acne caused primarily by Cutibacterium acnes overgrowth or dysbiosis, gland reduction alone might not provide complete clearance. Future treatments might combine sebaceous gland ablation with antimicrobial or anti-inflammatory agents. For now, however, the devices offer the most direct intervention available for the oil production component of acne—the one factor that contributes to nearly every acne case.
Conclusion
Sebaceous gland ablation devices using 1726 nm laser technology represent a genuine advance in acne treatment, delivering clear or nearly clear skin for approximately two-thirds of patients with moderate-to-severe acne. The FDA-approved devices (AviClear and Accure) have strong clinical data, excellent safety profiles, and work across diverse skin types. The technology deserves serious consideration if you’ve struggled with acne despite conventional treatments. However, the “permanently reduces oil production” claim requires nuance: while the reduction is substantial and durable, roughly 20% of patients experience some relapse over time, and regenerative capacity in sebaceous tissue means that permanent, lifelong clearance isn’t guaranteed for everyone. This is still far better than conventional acne management, but set realistic expectations before investing in treatment.
If you’re considering sebaceous gland ablation, consult with a dermatologist who has experience with these specific devices. Ask about their patient outcomes, relapse rates in their practice, and what maintenance protocol they recommend if acne returns. Confirm that your skin type and acne severity fit the ideal profile for treatment. And discuss cost and whether any insurance coverage applies (most insurers still classify this as cosmetic, though that’s changing as the evidence base grows). For the right candidate, this treatment can be genuinely transformative.
You Might Also Like
- New Topical Cannabinoid Cream in Clinical Trials…CB2 Receptor Activation Reduces Sebum Production in Lab Studies
- New Photoacoustic Therapy Device in Clinical Trials…Uses Sound Waves Combined With Light to Destroy Acne Bacteria
- New CRISPR Gene Therapy for Acne in Clinical Trials…Researchers Exploring Genetic Modification of Sebaceous Glands
Browse more: Acne | Acne Scars | Adults | Back | Blackheads