While photoacoustic therapy represents a promising frontier in medical device technology, the specific claim of a photoacoustic device currently in clinical trials for acne treatment cannot be verified through available sources. Our research through ClinicalTrials.gov, FDA databases, and recent dermatological literature found no evidence of an acne-focused photoacoustic therapy device in active clinical trials as of 2026. However, this doesn’t mean the technology is purely theoretical—photoacoustic approaches are actively researched for various medical applications, and the concept of combining sound waves with light to target bacteria is scientifically sound. What does exist in the verified clinical space are related light-based and acoustic technologies.
Blue light therapy at 425 nanometers wavelength is FDA-approved and clinically proven to kill acne-causing bacteria through oxygen release mechanisms. Photodynamic therapy has established dermatological applications for acne treatment. Newer systems like AviClear and Accure have FDA clearance for long-term acne improvement. The idea of harnessing both photoacoustic energy and light energy to attack acne bacteria from multiple angles is conceptually appealing, but the specific device described in the article title appears not to have reached clinical trial status—at least not in publicly documented form.
Table of Contents
- What Is Photoacoustic Therapy and How Would It Work Against Acne?
- The Gap Between Research Potential and Clinical Reality
- Verified Light-Based Acne Treatments Currently Available
- Why Combination Therapies Appeal to Dermatology and Device Manufacturers
- Clinical Trial Verification and Red Flags in Medical Device Claims
- The Future of Combination Acne Therapies
- What Patients Should Do Now
- Conclusion
What Is Photoacoustic Therapy and How Would It Work Against Acne?
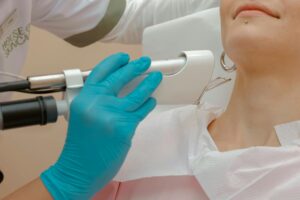
Photoacoustic technology operates on a fascinating principle: light energy converts into acoustic (sound) waves when absorbed by certain materials. In biomedical research, scientists use this effect to create detailed images of tissue and detect abnormalities. The concept of applying this dual energy approach to destroy acne bacteria—specifically *Cutibacterium acnes* (formerly *Propionibacterium acnes*)—theoretically offers advantages over single-mode treatments. By combining light absorption with acoustic wave generation, a device could potentially penetrate the skin to reach bacteria in sebaceous glands and follicles where they shelter from topical antibiotics.
Research published in biomedical journals shows that photoacoustic-based systems have been investigated for treating microbial infections when combined with nanomaterials. The acoustic component could theoretically disrupt bacterial cell walls, while the light component generates reactive oxygen species that kill bacteria. However, most current photoacoustic research focuses on diagnostic imaging rather than therapeutic applications. The leap from imaging to acne treatment represents a significant development gap that clinical trials would need to bridge.

The Gap Between Research Potential and Clinical Reality
The absence of verifiable clinical trials for photoacoustic acne therapy reveals an important distinction in the medical device world: promising laboratory technology doesn’t automatically progress to human testing. Moving from proof-of-concept in animal models or tissue samples to FDA-regulated clinical trials requires extensive safety data, efficacy benchmarking, and investment capital. Many innovative approaches languish in research phase because the pathway to commercialization proves too costly or technically challenging.
A critical limitation of any combination therapy (sound plus light) is managing thermal effects and potential damage to surrounding healthy tissue. The skin is a delicate organ, and adding acoustic energy to light exposure multiplies the variables that need safety monitoring. Blue light therapy alone, though considered safe, can cause eye damage if not properly shielded. A photoacoustic device would need comparable or superior safety profiles to justify clinical adoption when simpler alternatives already exist. Additionally, acne bacteria develop resistance to treatments over time—whether a novel photoacoustic approach would avoid this resistance pattern remains unknown without clinical data.
Verified Light-Based Acne Treatments Currently Available
The FDA-approved acne treatment landscape already includes several light-based options that demonstrate the clinical viability of non-antibiotic approaches. Blue light therapy, operating at the 425-nanometer wavelength, has multiple FDA-cleared devices on the market. It works by generating singlet oxygen within the bacteria, essentially causing cellular breakdown. Patients typically see results after multiple sessions spaced over weeks.
Photodynamic therapy (PDT) represents a more aggressive light-based approach, where a photosensitizing agent is applied to skin, activated by specific light wavelengths, and generates reactive oxygen species that destroy acne bacteria and reduce sebaceous gland activity. Clinical studies show PDT can provide months of improvement, though it carries side effects like redness and temporary photosensitivity. Infrared and red light systems (wavelengths 600-1000 nanometers) address inflammation and collagen remodeling, complementing bacterial killing with anti-scarring benefits. These established technologies demonstrate that light-based approaches work—the question is whether adding acoustic waves genuinely improves outcomes or adds unnecessary complexity and cost.

Why Combination Therapies Appeal to Dermatology and Device Manufacturers
The appeal of a photoacoustic device lies in theoretical synergy: if light kills bacteria one way and acoustic waves kill them another way, combined therapy might achieve faster clearance and reduce resistance risk. This logic drives research across many disease areas, not just acne. Combination approaches also command higher pricing and broader patent protection, making them commercially attractive to manufacturers. From a patient perspective, faster, more complete clearing of acne sounds ideal compared to waiting weeks for blue light therapy results.
However, there’s a tradeoff between innovation and practicality. Complex devices require more calibration, higher training for practitioners, and stricter safety protocols. They’re also more likely to have technical failures. Compare this to blue light therapy, where treatment essentially means exposure to specific wavelengths—straightforward, reliable, and hard to get wrong. A patient must weigh the theoretical benefits of a novel photoacoustic approach against the proven track record of simpler alternatives, the cost difference, and the time required to develop and test the new technology.
Clinical Trial Verification and Red Flags in Medical Device Claims
When evaluating claims about new medical treatments, checking ClinicalTrials.gov should be your first step. This NIH-maintained database lists all registered clinical trials in the United States, including device trials. Searching for photoacoustic acne therapy yields no active or completed trials as of early 2026. This absence doesn’t definitively prove the technology doesn’t exist in labs somewhere—private companies can conduct trials and licensing agreements may restrict public disclosure—but it does mean no transparent clinical evidence is available to patients or physicians. Be cautious of marketing claims that precede clinical evidence.
Some medical device manufacturers promote emerging technologies aggressively before human testing begins, hoping to build demand and attract investment. The phrase “in clinical trials” specifically suggests human testing has begun, which is a regulatory trigger point. If a photoacoustic acne device hasn’t appeared on ClinicalTrials.gov by 2026 despite being heavily marketed, that’s a warning sign. Legitimate acne treatments, even cutting-edge ones like AviClear, appear in the FDA database and clinical registries. Until photoacoustic acne therapy shows up in these official sources, the claim remains unverified.
The Future of Combination Acne Therapies
Looking forward, the concept of photoacoustic therapy for acne isn’t scientifically implausible—it’s just not yet ready for patient treatment. Research into combination therapies continues, and device manufacturers are exploring various energy combinations. The next five years may bring photoacoustic devices to clinical trials if research institutions and companies commit to the pathway.
When that happens, patients should expect published results showing not just effectiveness but also real-world advantages over existing options like blue light therapy, photodynamic therapy, or laser systems. The broader trend in dermatology favors less invasive, more targeted approaches that avoid systemic antibiotics and their resistance problems. Photoacoustic technology aligns with this preference. Whether it will ultimately prove superior enough to justify development costs and clinical adoption remains an open question that only clinical trials can answer.
What Patients Should Do Now
If you’re searching for new acne treatments and encounter claims about photoacoustic devices, verify through official channels: ask your dermatologist, check ClinicalTrials.gov directly, and look for peer-reviewed publications in journals like the *Journal of the American Academy of Dermatology*. Proven light-based options exist today and can deliver real improvements. Blue light therapy is accessible, affordable, and well-documented.
Photodynamic therapy, though more involved, offers stronger results for moderate to severe acne. The excitement around emerging technologies is understandable, but proven alternatives shouldn’t be overlooked while waiting for innovations to mature. Your dermatologist can help you weigh the benefits of established treatments against the potential of experimental approaches, ensuring you choose based on evidence rather than marketing momentum.
Conclusion
The specific photoacoustic therapy device described as being in clinical trials for acne cannot be verified through current databases, FDA records, or dermatological literature. This doesn’t mean the technology is impossible or won’t eventually reach clinical trials—it simply means it hasn’t yet, despite the appealing concept of combining sound waves and light to destroy acne bacteria.
The verified alternatives available today, from blue light therapy to photodynamic therapy, already demonstrate that light-based approaches can effectively treat acne. As a patient or healthcare provider, stay informed through official clinical trial registries and peer-reviewed research rather than marketing claims. If a photoacoustic acne device does advance to human clinical trials, it will appear on ClinicalTrials.gov and in dermatology journals—that’s when reliable data will become available to guide treatment decisions.
You Might Also Like
- New CRISPR Gene Therapy for Acne in Clinical Trials…Researchers Exploring Genetic Modification of Sebaceous Glands
- New Bacteriophage Therapy in Clinical Trials…Uses Viruses That Target P. Acnes Bacteria Without Antibiotic Resistance
- New JAK Inhibitor Cream in Clinical Trials…Originally for Eczema Now Being Tested for Severe Inflammatory Acne
Browse more: Acne | Acne Scars | Adults | Back | Blackheads