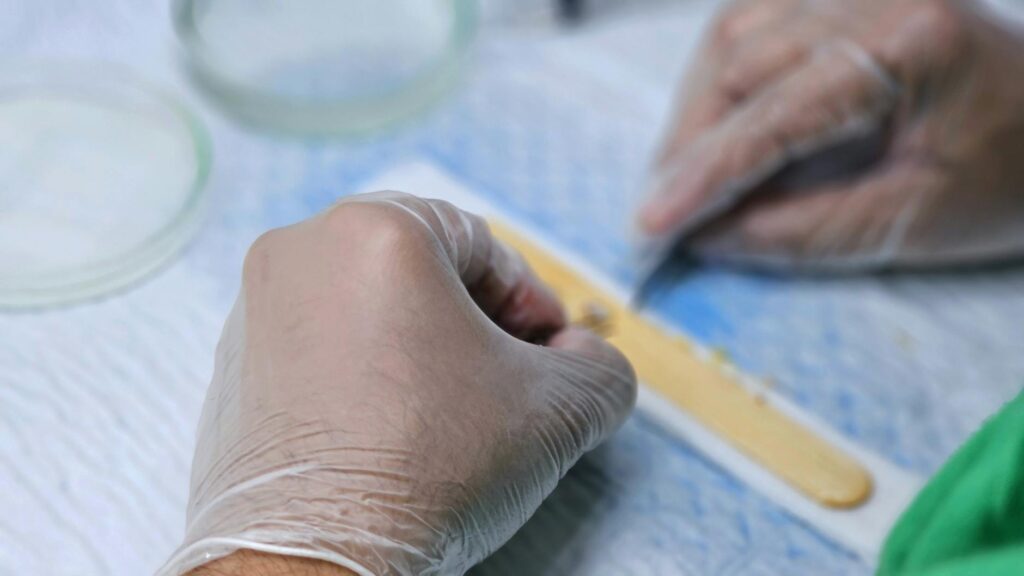
Yes, microbiome replacement creams are currently in clinical trials, and they do work by introducing beneficial bacteria to replace harmful strains on the skin. Multiple formulations are advancing through development phases, with some showing promising results for acne and inflammatory skin conditions. AOBiome’s B244, which introduces Nitrosomonas eutropha bacteria, completed Phase 2b trials and demonstrated positive efficacy for both acne vulgaris and atopic dermatitis, with the company preparing to move into Phase 3 global trials. The concept sounds futuristic, but it’s based on decades of microbiome research showing that acne and other skin conditions aren’t just about oil production or dead skin cells—they’re fundamentally about which bacteria live on your skin and what they produce.
When harmful bacteria like Cutibacterium acnes dominate your skin microbiome, they trigger inflammation and breakouts. By transplanting beneficial bacterial strains that compete with these harmful species, researchers are essentially rebalancing your skin’s ecosystem rather than scorching it with antibiotics or harsh chemicals. Unlike products currently on shelves, these clinical-trial formulations are live, bioactive products with documented safety testing. This distinction matters: a cream containing dead bacterial extracts behaves very differently from one with living microorganisms, which is why regulatory agencies are scrutinizing these products carefully before approval.
Table of Contents
- How Do Microbiome Transplant Creams Replace Harmful Bacteria?
- Clinical Trial Results and Current Development Status
- Which Microbiome Creams Are Closest to Market?
- How to Use Microbiome Creams (When They’re Available)
- Safety Concerns and Regulatory Hurdles
- Microbiome Creams vs. Traditional Acne Treatments
- What’s Next for Microbiome-Based Skin Therapeutics
- Conclusion
- Frequently Asked Questions
How Do Microbiome Transplant Creams Replace Harmful Bacteria?
The mechanism is competitive exclusion. When you apply a microbiome cream containing beneficial bacteria, those organisms colonize your skin, take up physical space on the follicle walls and skin surface, and consume nutrients that harmful bacteria would otherwise use. They also produce compounds—like antibacterial peptides and organic acids—that actively inhibit the growth of acne-causing species. Over time, the bacterial landscape shifts from a harmful-dominated community to one favoring beneficial strains. AOBiome’s B244 works by introducing Nitrosomonas eutropha, a bacterium that oxidizes ammonia on the skin’s surface, lowering pH in the process. A lower skin pH creates an environment where C.
acnes struggles to thrive, while beneficial commensals flourish. In the Phase 2b trial results, patients using B244 showed meaningful reductions in acne lesion counts over eight weeks. Compare this to traditional topical antibiotics like clindamycin, which kill bacteria broadly across your microbiome—sometimes creating antibiotic-resistant superbugs in the process. The transplant approach is more surgical and selective. Roseomonas mucosa, tested in separate trials, showed a different advantage: when applied to skin affected by eczema, it reduced the abundance of Staphylococcus aureus, a pathogenic species that worsens eczema flares. The beneficial bacteria essentially crowded out the troublemakers. This is why microbiome creams aren’t one-size-fits-all—different beneficial strains address different skin problems by targeting different harmful competitors.

Clinical Trial Results and Current Development Status
The evidence so far is encouraging but still preliminary. AOBiome’s B244 Phase 2b trial was an 8-week, randomized, placebo-controlled study that showed statistically significant improvements in inflammatory acne lesions. The partnership announced in January 2024 with Maruho Co., Ltd. signaled that Phase 3 trials were moving forward globally—a crucial step because Phase 3 involves larger patient populations and longer observation periods to confirm safety and efficacy at scale. Roseomonas mucosa trials published results showing that a six-week cream application reduced eczema severity scores by meaningful margins in both adults and children, decreased the amount of steroid medication patients needed, and notably reduced the burden of pathogenic S.
aureus on the skin. However, here’s the limitation: these trials were relatively small and short-term. We don’t yet have long-term data on whether patients can sustain improvements after stopping treatment, whether the beneficial bacteria persist on skin long-term, or how the microbiome reshapes itself months or years later. Vitreoscilla filiformis (Vf) lysate cream, tested in a 2008 double-blind placebo-controlled trial with 75 patients, showed measurable improvement in mild atopic dermatitis. More recently, a Lactobacillus-based cream designed to reduce body odor was tested in a 25-volunteer trial and successfully shifted the microbial balance, decreasing odor-causing Actinobacteria and Corynebacterium while boosting beneficial Lactobacillus. These results validate the principle, but most microbiome therapeutics remain in research or early clinical phases with regulatory questions still unresolved.
Which Microbiome Creams Are Closest to Market?
AOBiome’s B244 is the furthest along in regulatory pathways, having completed Phase 2b and entering Phase 3 preparation. If Phase 3 succeeds, approval could theoretically arrive within 2-4 years, though predicting regulatory timelines is risky. The company has also been transparent about safety: in trials, B244 was well-tolerated with no serious adverse events reported. This is important because introducing live organisms to skin requires careful toxicity assessment, especially in vulnerable populations like immunocompromised individuals.
Roseomonas mucosa products are still in academic and early-stage clinical development, with published journal data but no announced commercial partnerships yet. Vitreoscilla filiformis lysate formulations already exist in some moisturizers and topicals sold as cosmetics or medical devices (rather than pharmaceuticals), which means they’ve bypassed some regulatory hurdles—but they’re dead, processed bacterial extracts, not live culture transplants. If you’re looking for a microbiome cream you can actually buy today, some Vf lysate products are available, but they’re not equivalent to the live formulations in active clinical trials. The distinction matters practically: a dead bacterial extract might provide beneficial compounds, but it doesn’t establish a competing population of living bacteria that can persist and reproduce on your skin. That’s why the clinical-trial formulations—the ones still in development—are generating so much research attention.

How to Use Microbiome Creams (When They’re Available)
Once approved and on the market, microbiome creams will likely require application instructions quite different from standard acne treatments. You won’t want to use them alongside harsh actives like high-concentration benzoyl peroxide or strong retinoids, which would kill the beneficial bacteria you’re trying to establish. Dermatologists will probably recommend a simplified routine: gentle cleanser, microbiome cream, and perhaps a non-irritating moisturizer. The goal is to let the bacterial transplant establish itself without constant antimicrobial assault. Application frequency will matter. Most topical treatments work best when applied consistently—likely once or twice daily—to maintain the beneficial bacterial population.
This is a tradeoff compared to, say, adapalene, which you apply nightly and your skin eventually adjusts to. With a microbiome cream, consistency is essential because the living bacteria can be disrupted by incomplete coverage or gaps in treatment. If you miss applications, the balance might shift back toward harmful bacteria, and you’d need to rebuild. Storage and shelf-life will differ from standard creams. A product containing living bacteria can’t sit in a hot car or bathroom for months. It will require refrigeration or special stabilization, making it less convenient than a tube of benzoyl peroxide. This is a real limitation: microbiome products will demand more user compliance and care in handling.
Safety Concerns and Regulatory Hurdles
The biggest caveat: microbiome therapeutics are not yet standardized or fully regulated. Live microbial products are considered drugs in most jurisdictions, which means they must clear rigorous safety testing. A key concern is that introducing any foreign organism—even a beneficial one—carries theoretical risks in vulnerable populations. Immunocompromised patients, those with severe autoimmune conditions, or people with damaged skin barriers might respond differently than the healthy volunteers in clinical trials. Most microbiome creams will likely carry restrictions on use in these populations until more data accumulates. There’s also the question of long-term colonization and unintended effects.
Once you introduce a beneficial bacterium, can you reliably remove it if side effects emerge? If a person develops an adverse reaction to Nitrosomonas eutropha weeks into treatment, stopping the cream might not immediately stop the bacteria’s presence on skin. This is why regulatory agencies are moving cautiously, requiring extended observation periods and robust adverse-event monitoring. The current lack of standardized regulation for live microbial products means early approved creams will likely be restricted to dermatologists’ prescriptions rather than over-the-counter sales. Another practical warning: a microbiome cream from one manufacturer won’t necessarily work the same as one from another, because the bacterial strains, concentrations, and formulation vehicles differ. There’s no “microbiome transplant cream” category yet—each formulation is unique and must be tested independently. This is very different from benzoyl peroxide, where a 5% formulation is chemically identical regardless of brand.

Microbiome Creams vs. Traditional Acne Treatments
How do these stack up against what dermatologists typically recommend today? Benzoyl peroxide kills acne bacteria indiscriminately, which works fast (results in 4-8 weeks) but disrupts your entire skin microbiome, not just the harmful species. Retinoids like adapalene normalize skin cell turnover and reduce sebum, addressing root causes of acne but leaving your microbiome untouched. Oral antibiotics like doxycycline reduce bacterial counts system-wide while also having anti-inflammatory effects, but they drive antibiotic resistance and can disrupt your gut microbiome. Microbiome creams take a completely different approach: they accept that bacteria on skin aren’t inherently bad—instead, they’re trying to establish the right balance. For someone with active acne, benzoyl peroxide will likely work faster initially.
But if you’re prone to recurring acne despite multiple courses of antibiotics, or if your skin is sensitive to harsh treatments, a microbiome cream might eventually offer a more stable, less disruptive solution. The tradeoff is patience: microbiome rebalancing takes weeks to months, not days. The comparison becomes interesting for chronic conditions like atopic dermatitis, where overuse of topical steroids causes skin barrier damage and further dysbiosis. A Roseomonas mucosa cream that actively reduces pathogenic bacteria while restoring beneficial strains could reduce steroid dependence in a way that hydrating creams alone cannot. This is why dermatologists are watching these trials closely—the potential use cases extend beyond acne to eczema, rosacea, and other inflammatory skin conditions driven partly by dysbiosis.
What’s Next for Microbiome-Based Skin Therapeutics
The field is moving rapidly. AOBiome’s Phase 3 trials will likely determine whether B244 achieves regulatory approval and sets a precedent for other live-bacteria creams. If Phase 3 succeeds, expect similar products from other biotech companies to accelerate through trials, knowing there’s a viable pathway to market.
The timeline is realistically 3-5 years before the first microbiome cream reaches dermatologists’ offices, probably as a prescription for moderate acne or eczema. Beyond individual products, the bigger shift is conceptual: dermatology and skincare are moving away from the “kill everything” paradigm and toward microbiome-conscious approaches. Even before live bacterial creams hit the market, new products are being designed to support beneficial bacteria rather than eliminate them—through prebiotic ingredients that feed good bacteria, or by avoiding harsh antimicrobials that disrupt the balance. The microbiome cream research happening now is laying the scientific foundation for an entirely different approach to skin health over the next decade.
Conclusion
Microbiome transplant creams are real, they’re in clinical trials, and they do work by introducing beneficial bacteria to replace harmful species. AOBiome’s B244 and other formulations have shown promising results for acne and eczema, with the furthest-along products entering Phase 3 testing. However, these are not yet available to consumers, and most will remain prescription-only even after approval due to safety considerations and regulatory requirements for live microbial products.
The key takeaway: if you’re struggling with acne or eczema that hasn’t responded to traditional treatments, microbiome creams represent a genuinely novel approach worth watching. They won’t replace benzoyl peroxide overnight, and they demand patience and consistent application. But they offer a vision of dermatology where the goal isn’t to kill bacteria—it’s to rebalance your skin’s ecosystem so beneficial strains naturally outcompete the harmful ones. For now, stay informed through your dermatologist about when these products might become available for your specific condition.
Frequently Asked Questions
Can I buy a microbiome transplant cream now?
Not the live-culture formulations in active clinical trials. Some products containing Vitreoscilla filiformis lysate (dead bacterial extracts) are available as cosmetics or medical devices, but they’re not equivalent to the living bacterial transplants being tested in Phase 2 and Phase 3 trials. Real microbiome creams will likely require a dermatologist’s prescription.
Will microbiome creams work for my acne if antibiotics didn’t?
Possibly, especially if your acne flares after you stop taking antibiotics. Oral antibiotics disrupt your microbiome globally, which often leads to rebound acne. A microbiome cream that establishes beneficial bacteria could theoretically provide more lasting improvement. However, this will depend on the specific product and your skin’s unique biology.
Are microbiome creams safe for sensitive skin?
Unknown in most cases. Clinical trials have shown good tolerability in the tested populations, but sensitive skin often reacts unpredictably to new products. Early-stage microbiome creams will likely carry restrictions limiting use in people with severe barrier damage or immunocompromise. Talk to a dermatologist before assuming it’s safe for your skin type.
How long until microbiome creams are approved and available?
If Phase 3 trials progress smoothly, the first FDA approvals could arrive in 3-5 years. That’s optimistic; regulatory approval could take longer. Products approved in other countries might reach markets before the US, so international availability could come sooner.
Can I use a microbiome cream with my current acne routine?
Probably not without modifications. You’ll need to stop using benzoyl peroxide, strong retinoids, and oral antibiotics to let the beneficial bacteria establish themselves. Your dermatologist will advise on how to safely transition from your current routine.
Will microbiome creams make acne worse before it gets better?
Possibly. When you shift the bacterial balance, some patients experience a brief “adjustment period” where breakouts worsen before improving—similar to how retinoid therapy sometimes causes purging. This is observed in some clinical trials but not consistently. Your dermatologist will help determine whether worsening is expected or a sign to discontinue use.
You Might Also Like
- New Topical Antiandrogen Cream in Clinical Trials…Blocks Hormones at the Skin Level Without Systemic Side Effects
- New Bacteriophage Therapy in Clinical Trials…Uses Viruses That Target P. Acnes Bacteria Without Antibiotic Resistance
- Clarisonic Brush Costs $200…Manual Cleansing Costs Free and Gentler on Skin
Browse more: Acne | Acne Scars | Adults | Back | Blackheads