A 15-year-old’s refusal to attend school for three weeks because of a severe acne breakout isn’t an overreaction—it’s a documented response to the psychological toll that severe facial acne inflicts during adolescence. When dermatologists and mental health professionals examine cases like this, they consistently find that acne-induced school avoidance represents a real psychiatric symptom, not a character flaw or teenage dramatics. The teenager wasn’t being difficult; she was experiencing genuine distress that made the thought of facing peers feel unbearable.
Parents often minimize severe acne because they remember their own teenage breakouts and moved past them. What they miss is the intensity of modern social environments—the constant exposure to idealized images on social media, the proximity to peers in classrooms, and the neurological reality that adolescent brains are hypersensitive to perceived social judgment. For some teens, severe acne becomes a legitimate barrier to functioning in school settings, and that barrier is medical, not behavioral.
Table of Contents
- Why School Refusal Due to Acne Is a Real Psychiatric Response in Teens
- The Psychological Weight of Severe Breakouts During Teen Years
- How Severe Acne Disrupts School Attendance and Social Functioning
- When to Take Teen Acne Seriously vs. Distinguishing Minor Breakouts
- The Intersection of Acne and Anxiety Disorders in Teenagers
- Professional Help: Dermatology and Mental Health Support Together
- Moving Forward: Supporting Teens With Severe Acne in School Environments
- Conclusion
Why School Refusal Due to Acne Is a Real Psychiatric Response in Teens
Adolescence is the period when the brain’s social comparison networks are most active and most fragile. A study published in the Journal of the American Academy of Dermatology found that approximately 40% of teenagers with moderate to severe acne experience symptoms consistent with clinical depression or anxiety. For the most severe cases, that percentage climbs higher. School refusal connected to acne severity isn’t laziness; it’s a symptom of depression or social anxiety disorder triggered by the visible skin condition. The mechanism is straightforward: a 15-year-old with a severe breakout covering their forehead, cheeks, and jawline faces real social consequences.
Peers comment. Teachers notice. The teenager becomes hyperaware of every reflection in every window. Unlike an illness that keeps you home legitimately, acne is visible, making the sufferer feel exposed and judged. This creates what psychologists call “appearance anxiety”—a specific form of social anxiety tied directly to physical appearance. When appearance anxiety reaches clinical levels, school becomes a trigger environment, and the teen’s brain responds with avoidance.

The Psychological Weight of Severe Breakouts During Teen Years
Unlike adults, who have developed more stable self-concepts, teenagers are still constructing their identities. Acne arrives at exactly the wrong developmental moment—when peer acceptance feels like survival, when self-worth is still malleable, and when the prefrontal cortex (responsible for rational risk assessment) isn’t fully developed. A severe breakout doesn’t just affect the skin; it disrupts the teenager’s sense of who they are and how others perceive them. The limitation here is that not all severe acne creates the same psychological impact. A teenager with strong social support, prior experiences with managing challenges, or who already feels confident may experience severe acne without school refusal.
Conversely, a teen with existing anxiety, social isolation, or perfectionist tendencies may find even moderate acne psychologically overwhelming. The visibility and severity of acne matter, but so do the teenager’s existing mental health baseline and social circumstances. Research in dermatology now recognizes “acne-related quality of life impairment” as a measurable construct. Teenagers with severe acne show measurable decreases in school performance, increased absenteeism, and elevated rates of depression and anxiety. When a 15-year-old refuses school for three weeks, parents should recognize this as a warning sign that the acne has crossed from a cosmetic concern into a mental health crisis—not because acne causes acne to hurt (though sometimes it does), but because the social and psychological weight has become intolerable.
How Severe Acne Disrupts School Attendance and Social Functioning
The cascade of effects is predictable. Week one: the teen wakes up with a severe breakout and doesn’t want to go to school. Parents might push back, seeing it as avoidable. Week two: the acne hasn’t improved; anxiety about school has intensified. The teenager now has missed assignments, which creates additional stress.
Week three: school refusal has solidified into a pattern. The teen’s anxiety has become conditioned—not just to the acne, but to the thought of facing everyone at school, explaining their absence, and catching up on work. A real-world example: a 15-year-old girl developed cystic acne along her jawline and chin after switching birth control. Within days, she stopped raising her hand in class, started eating lunch in the bathroom, and developed a tremor when she had to speak in front of the class. By week two, she was refusing to attend school at all. Her mother believed she was exaggerating; her father suggested she “just wear makeup.” What neither parent recognized was that the teenager’s anxiety had become physiological—her body was responding to the perceived threat of social exposure the same way it would respond to actual physical danger.
When to Take Teen Acne Seriously vs. Distinguishing Minor Breakouts
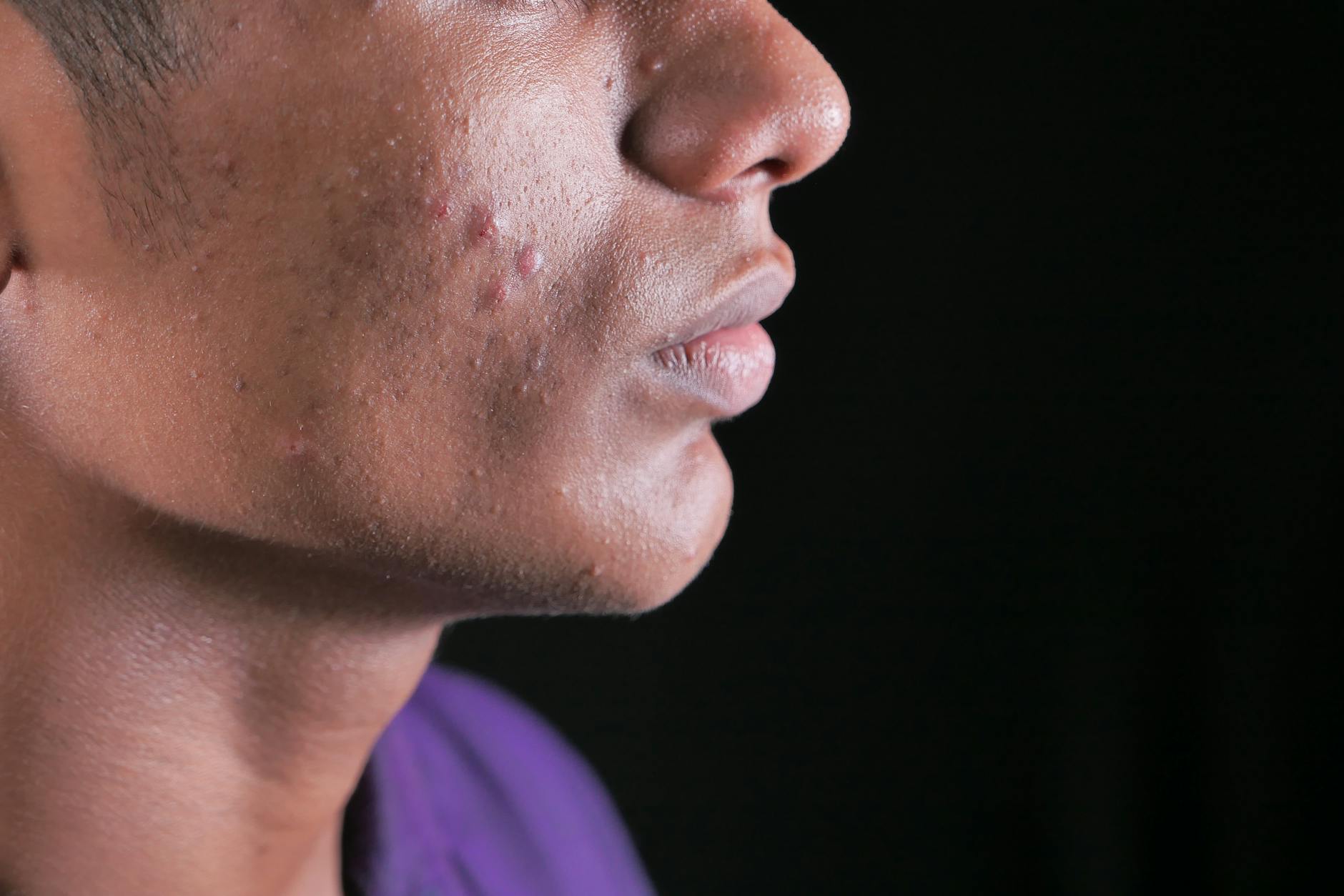
Not every breakout warrants school avoidance, and it’s important to distinguish between normal teenage acne and the severe cases that indicate a mental health response. Minor to moderate acne—a few breakouts on the forehead or occasional spots on the cheeks—is developmentally normal and typically doesn’t trigger clinical anxiety. Severe acne, by contrast, covers large areas of the face or body, may include cystic or nodular lesions that are painful, and creates visible scarring or deep inflammation.
The tradeoff parents face is between validating their teen’s distress and enabling avoidance. A balanced approach means taking the complaint seriously enough to schedule a dermatology appointment within days (not weeks), while also setting expectations that school attendance continues unless a medical provider recommends otherwise. If a teenager is refusing school because of acne, that’s a sign to prioritize treatment—but also to involve a mental health professional to address the anxiety component simultaneously. Treating only the acne without addressing the anxiety often leaves the teen vulnerable to relapse, even if their skin clears.
The Intersection of Acne and Anxiety Disorders in Teenagers
Severe acne and clinical anxiety don’t always co-occur, but when they do, each intensifies the other. A teenager with pre-existing social anxiety disorder will experience acne far more severely than a similarly affected peer without anxiety. Conversely, sudden-onset severe acne can trigger anxiety disorder in a teen who previously had no mental health concerns. This bidirectional relationship means that waiting for the acne to clear before addressing anxiety is ineffective—both conditions need treatment simultaneously.
A critical warning: untreated acne-related anxiety can develop into broader avoidance patterns. A teen who misses three weeks of school due to acne anxiety is at risk for continued school refusal even after their skin improves, because they’ve now experienced three weeks of success (from an anxiety perspective) through avoidance. The avoidance itself becomes reinforced, independent of the original trigger. This is why mental health intervention is essential during the acute phase, not after.

Professional Help: Dermatology and Mental Health Support Together
The most effective treatment for severe acne with concurrent school refusal involves coordination between a dermatologist and a mental health provider. The dermatologist addresses the skin condition with evidence-based treatments—prescription retinoids, oral antibiotics, hormonal treatments if appropriate, or isotretinoin for the most severe cases. Simultaneously, a therapist or counselor addresses the anxiety using cognitive-behavioral therapy (CBT), which is specifically effective for appearance anxiety and avoidance behaviors.
An example of comprehensive treatment: a 15-year-old with severe acne meets with a dermatologist who prescribes a combination treatment plan with a timeline for improvement. In parallel, the teen starts weekly therapy sessions addressing anxiety about returning to school, using exposure techniques and cognitive restructuring to challenge catastrophic thoughts about peer judgment. The teen continues attending school (with parental and school support) even as skin treatment begins working. Within six weeks, skin improvement is visible, and anxiety has decreased because the teen hasn’t missed more school and has developed coping skills independent of skin clearance.
Moving Forward: Supporting Teens With Severe Acne in School Environments
Parents who recognize that their teen’s acne-related school refusal is real—not an exaggeration or manipulation—are better positioned to provide effective support. This means taking the complaint seriously, arranging rapid dermatological care, and simultaneously communicating with the school about the situation. Some schools offer accommodations like alternative testing spaces or modified schedules while a teen addresses acute mental health concerns related to a visible condition.
The path forward also involves normalizing the conversation about acne’s psychological impact. When parents respond to severe acne with minimization (“everyone gets acne,” “it’s just a phase”), they inadvertently reinforce the message that the teen’s distress isn’t valid. A more supportive response acknowledges both the skin condition and the emotional toll: “This looks painful, and I understand why you’re feeling self-conscious. Let’s get you to a dermatologist this week, and we’ll also talk to someone about managing the anxiety.” This approach validates the teen’s experience while moving toward solutions.
Conclusion
A 15-year-old refusing school for three weeks because of severe acne isn’t overreacting—she’s displaying a proportionate response to a condition that has real psychological consequences during adolescence. Parents who encounter this situation should recognize it as a medical and mental health emergency, not a behavioral problem.
The teen isn’t being difficult; she’s in genuine distress that requires professional intervention on multiple fronts. The path forward involves rapid dermatological care, mental health support to address anxiety and avoidance patterns, and family communication that validates the teen’s experience while maintaining expectations for functioning and school attendance. With coordinated care addressing both the skin and the psychological toll, most teens recover fully and develop resilience that extends beyond the acne itself.
You Might Also Like
- New JAK Inhibitor Cream in Clinical Trials…Originally for Eczema Now Being Tested for Severe Inflammatory Acne
- He Was 9 When He Developed Acne Before Starting Puberty…Precocious Acne Is Becoming More Common
- He Was 11 When He Was Too Young for Most Prescription Acne Treatments…Pediatric Dermatologists Have Limited Options
Browse more: Acne | Acne Scars | Adults | Back | Blackheads





