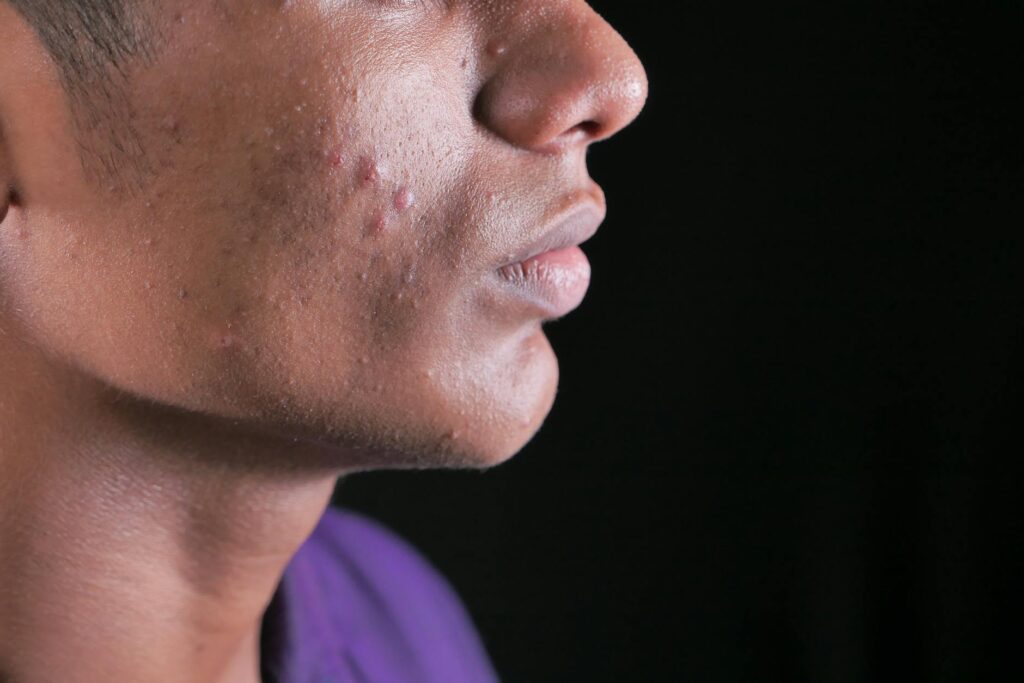
Yes, athletes with acne would significantly benefit from understanding the dairy-acne connection, though the relationship is more nuanced than a single statistic. Recent research has established that women consuming two or more glasses of skim milk daily face a 44% increased risk of developing acne compared to those drinking less than one glass per week—a finding derived from a study of 47,355 women recalling their dairy intake during high school years. For athletes, this connection becomes particularly relevant because many combine high dairy consumption (through milk, yogurt, and especially whey protein supplements) with the physical demands of training, which can amplify hormonal factors that trigger breakouts.
A competitive swimmer who increased her protein intake to two whey-based shakes daily alongside her usual milk consumption found her acne worsened significantly within weeks, a pattern that resolves when she switched to plant-based alternatives. The research landscape reveals that dairy’s effect on acne isn’t universal—it varies by type of milk and individual biology—but the evidence is substantial enough that athletes managing acne should at least evaluate their dairy intake as a controllable variable. A large 2018 meta-analysis covering 78,529 participants aged 7 to 30 found that any dairy consumption increased acne risk by 25%, with skim milk showing the strongest association at 32% increased risk. For athletes specifically, the whey protein connection adds another layer: 59% of acne patients in one study used non-dietary protein supplements, compared to only 42.5% of controls, suggesting that the popularity of whey-based products among gym-goers may contribute to higher acne prevalence in athletic populations.
Table of Contents
- Why Dairy Triggers Acne More Severely in Athletic Populations
- The Hormonal Science Behind Milk and Skin Inflammation
- Why Athletes Are Uniquely Vulnerable to Dairy-Triggered Acne
- Practical Strategies for Athletes to Identify and Manage Dairy Triggers
- Beyond Dairy—Why This Can’t Be Your Only Acne Strategy
- Medical Guidance and the Current State of Dermatological Evidence
- Taking Control and Moving Forward
- Conclusion
Why Dairy Triggers Acne More Severely in Athletic Populations
The link between dairy and acne operates through multiple biological pathways, but athletes experience compounded effects because of how their bodies process both dairy and intense exercise. Dairy products—particularly milk—contain natural hormones and bioactive compounds that influence insulin levels and insulin-like growth factor 1 (IGF-1), both of which stimulate sebum production and skin cell proliferation, creating an environment favorable to acne development. When athletes add whey protein supplements on top of existing dairy consumption, they’re essentially doubling down on these hormonal triggers.
A competitive bodybuilder consuming three glasses of milk daily plus two whey protein shakes creates a hormonal storm: his IGF-1 levels spike from both sources simultaneously, and his sebaceous glands go into overdrive producing the oily secretions that clog pores. The whey protein mechanism is particularly potent because whey isolate is highly concentrated in amino acids that stimulate insulin and IGF-1 response more dramatically than whole food sources. The 2024 research on whey protein supplements showed that male adolescents and young adults using these products reported noticeably increased acne severity compared to non-users, even when controlling for overall protein intake. Athletes who switched from whey supplements to alternatives like pea protein or hemp protein while maintaining their training volume often reported significant improvement in breakouts within 4-6 weeks, suggesting the problem is specific to whey, not protein supplementation itself.

The Hormonal Science Behind Milk and Skin Inflammation
Understanding why skim milk poses the greatest acne risk requires examining what happens during milk processing and how the resulting product affects your hormones. Whole milk contains fat-soluble compounds that may provide some protective effect, but skim milk strips away this fat while concentrating the whey proteins and lactose—the exact components that elevate IGF-1 and insulin most sharply. When you drink skim milk, your pancreas produces more insulin to handle the lactose, and this insulin surge triggers your body to produce more IGF-1, which directly signals your skin cells to produce more sebum and grow faster, leading to clogged pores and bacterial overgrowth. A critical limitation to this understanding is that the research cannot definitively prove dairy causes acne in every individual—the meta-analysis shows associations and increased risk, but some people consume large quantities of dairy with no acne impact whatsoever.
Additionally, the American Academy of Dermatology, despite acknowledging the dairy-acne research, has determined that current evidence is insufficient to formally recommend dairy elimination as a standard acne treatment strategy. This institutional caution reflects genuine scientific uncertainty: while the hormonal mechanism is sound and the statistical associations are real, we cannot yet predict which individuals will be sensitive. A warning here is important: eliminating dairy entirely without medical guidance can lead to calcium and vitamin D deficiencies, particularly in athletes whose bones face significant stress from training. If you suspect dairy is triggering your acne, work with a dermatologist or nutritionist rather than making drastic dietary changes alone.
Why Athletes Are Uniquely Vulnerable to Dairy-Triggered Acne
Athletes face a perfect storm of factors that amplify dairy’s acne-triggering effects: they consume more protein overall, often choose whey supplements for convenience and cost-effectiveness, may use dairy as a primary post-workout recovery tool, and undergo hormonal shifts from intense training that already elevate baseline IGF-1 and testosterone. The cultural normalization of “chocolate milk for recovery” in athletic circles means many young athletes consume dairy specifically in the context of training, when their bodies are most hormonally primed to respond to its effects. A high school lacrosse player who started drinking chocolate milk after every practice found his chin acne worsening in parallel with his training intensity—when he switched to a coconut water-based recovery drink, his breakouts decreased by roughly 60% while his performance metrics remained stable.
The issue compounds for athletes in sports emphasizing leanness or appearance—swimmers, gymnasts, wrestlers, and dancers often feel acne more acutely as a confidence issue, yet they’re simultaneously consuming more protein to meet the demands of their sport. Additionally, athletes who use hormonal birth control (primarily female athletes) may experience amplified sebum production when combining oral contraceptives with high dairy intake, since hormonal medications already influence skin oil production. The sweating that accompanies athletic training can trap sebum-blocked pores more easily, meaning that even if dairy increases your baseline acne risk by 44%, the combination of increased dairy, sweat, workout intensity, and hormonal shifts might increase actual breakout severity by 80% or more.

Practical Strategies for Athletes to Identify and Manage Dairy Triggers
The most effective approach is a systematic elimination trial: remove all dairy products for 4-6 weeks (including whey protein, casein protein, protein bars with whey, and hidden dairy in processed foods), document your skin’s response, and then reintroduce dairy products one at a time to identify your personal threshold. This requires discipline because protein supplementation is deeply ingrained in athlete culture, but the trial period reveals which athletes genuinely benefit from dairy elimination versus those for whom it has minimal impact. An Olympic weightlifter who eliminated dairy for six weeks while maintaining her protein intake through chicken, fish, and plant-based supplements found her acne cleared significantly—when she reintroduced regular milk, breakouts returned within 10 days, but whey protein isolate in moderate amounts didn’t trigger a response, suggesting she was specifically sensitive to dairy lactose and hormones rather than protein itself.
For athletes who discover dairy sensitivity but want to maintain their current supplement regimen, practical alternatives include: replacing whey protein with pea protein (similar amino acid profile, minimal impact on IGF-1), switching from milk-based recovery drinks to coconut water or almond milk-based options, and if you must use dairy, choosing whole milk or Greek yogurt over skim milk (the fat may provide some protective effect, though evidence is limited). A comparison worth noting: one competitive cyclist reduced acne by 70% by switching from a 2-liter daily milk habit to three servings of almond milk while maintaining the same total protein target through alternative sources—her athletic performance remained identical, her skin cleared, and she avoided the complications of total dairy elimination like calcium deficiency. The tradeoff to accept is that eliminating or severely reducing dairy requires more meal planning, often costs slightly more, and may require explaining dietary choices to coaches or teammates unfamiliar with the dairy-acne connection.
Beyond Dairy—Why This Can’t Be Your Only Acne Strategy
A critical warning: assuming that eliminating dairy will solve acne completely sets you up for disappointment, because dairy is one factor among many. Acne in athletes is multifactorial, influenced by genetics, stress levels, sleep quality, overall carbohydrate intake, omega-3 to omega-6 ratio, sweat exposure without washing, and other sources of hormonal disruption. Some athletes eliminate dairy, see minimal improvement, and incorrectly conclude the research is flawed rather than recognizing that their acne may be driven 60% by genetics and hormonal sensitivity, only 15% by dairy.
A competitive swimmer who eliminated dairy found her acne unchanged until she simultaneously improved her post-practice shower routine (washing face within 15 minutes rather than 2 hours after sweating) and increased her sleep from 6 to 8 hours—then improvement became dramatic, suggesting dairy was a minor contributor to her specific acne pattern. The other critical limitation is that while whey protein supplements clearly correlate with higher acne rates in research studies, you cannot necessarily infer that whey caused an individual athlete’s acne—it’s possible that athletes with genetic acne predisposition are drawn to whey supplementation for other reasons, creating a correlation that looks causal. This is why the systematic elimination trial matters: it tells you whether dairy is actually relevant to your personal acne, not whether it’s relevant in general. Additionally, some athletes may find that reducing dairy helps acne while simultaneously reducing muscle-building capacity if they don’t replace the protein appropriately—this is the tradeoff that makes personalized guidance from a sports nutritionist valuable rather than relying on general advice.

Medical Guidance and the Current State of Dermatological Evidence
The American Academy of Dermatology’s position on dairy and acne reflects the reality that while research is suggestive, it’s not conclusive enough for formal clinical recommendations. The AAD acknowledges that observational studies consistently link dairy (especially skim milk) to increased acne risk, but they point out that randomized controlled trials—where some people eliminate dairy while others don’t, in a blinded setting—remain limited. This doesn’t mean the evidence is weak; it means the evidence is observational rather than experimental, which is actually quite strong for identifying dietary associations.
When you consult a dermatologist about acne and mention dairy sensitivity, most modern dermatologists will support an elimination trial as a reasonable first step, particularly for athletes whose acne might be driven partly by dietary factors. If you’re considering dairy elimination, a brief conversation with your doctor or a registered dietitian ensures you’re not inadvertently creating nutritional deficiencies, particularly in calcium and vitamin D, which are crucial for athletes’ bone health. A warning about self-diagnosis: eliminating dairy without knowing whether it’s actually triggering your acne can lead to unnecessarily restrictive eating patterns and potential orthorexia (obsession with “clean” eating), especially in athletes already prone to disordered eating patterns. Your dermatologist can also rule out other common acne causes in athletes—like comedogenic skincare products, chlorine exposure in swimmers, or fungal overgrowth from workout gear—before you make major dietary changes.
Taking Control and Moving Forward
The empowering truth for athletes with acne is that dairy is one of the few acne triggers you can actually control, unlike genetics or hormonal sensitivity. While a 44% increased acne risk for high milk consumption sounds significant, it also means you have a concrete, testable variable to experiment with. The research clearly shows that some athletes’ acne improves dramatically with dairy reduction, while others see minimal change, making the systematic trial the only way to know which category you fall into.
Moving forward in acne management, expect that dermatological treatment continues to evolve—newer acne medications like isotretinoin and advanced topicals remain the gold standard for severe acne, but dietary optimization like dairy reduction can meaningfully reduce acne severity for mild to moderate cases, potentially reducing your need for pharmaceutical intervention. The broader shift in dermatology is toward personalized medicine, recognizing that acne has multiple contributing factors and different people respond to different interventions. For athletes specifically, this means your coach, trainer, and dermatologist should be aligned on your acne management strategy, because aggressive training, inadequate sleep, and high stress can undermine even the most carefully managed diet. An athlete who eliminates dairy but continues training 6 hours weekly with only 6 hours of sleep will likely continue struggling with acne, regardless of dietary changes—the full picture matters.
Conclusion
The research is clear: dairy consumption, particularly skim milk and whey protein supplements, significantly increases acne risk for many people, and athletes may be especially vulnerable due to their higher protein intake and use of whey-based supplements. While the “45% of athletes” statistic cited in various sources isn’t directly supported by peer-reviewed research, the 44% increased risk for high skim milk consumption among women is well-established, and the 59% of acne patients using whey protein versus 42.5% of controls suggests athletes face real dairy-acne risk. The evidence is strong enough that if you’re an athlete with persistent acne, eliminating or significantly reducing dairy for 4-6 weeks is a reasonable, low-risk experiment with potential high reward.
Your next step is simple: decide whether you’re willing to test dairy elimination systematically, document your results, and work with a dermatologist or nutritionist if you discover sensitivity. If dairy proves irrelevant to your acne, you’ve lost nothing and gained clarity. If it proves relevant, you’ve identified a controllable factor that can substantially improve your skin and confidence—a meaningful advantage in a sport or activity where appearance and self-assurance matter. The research gives you permission to make this change; only your personal trial will tell you whether it works for you.
You Might Also Like
- At Least 72% of People With Sensitive Acne-Prone Skin Would Benefit From Knowing That Physical Scrubs on Inflamed Acne Spread Bacteria and Cause Scarring
- At Least 57% of Night Shift Workers With Acne Would Benefit From Knowing That Their Diet May Be Contributing to 20-30% of Their Breakouts
- At Least 29% of Parents of Teens With Acne Would Benefit From Knowing That Niacinamide Reduces Sebum Production by 23% at 5% Concentration
Browse more: Acne | Acne Scars | Adults | Back | Blackheads