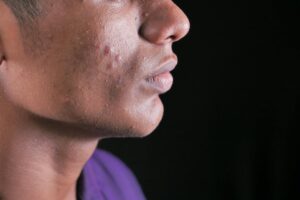
Malassezia yeast causes acne-like bumps because it thrives inside hair follicles, feeding on sebum and triglycerides, and triggering an inflammatory immune response that produces uniform, itchy papules and pustules across oil-rich areas of the skin. Unlike traditional acne vulgaris, which is driven by the bacterium Cutibacterium acnes and tends to produce varied lesion types including blackheads and deep cysts, Malassezia folliculitis creates clusters of small, monomorphic bumps that look strikingly similar to bacterial acne but fail to respond to standard acne treatments. A person might spend months cycling through benzoyl peroxide washes and retinoid creams with zero improvement, not realizing the culprit is a fungus that has been living on their skin since birth. This distinction matters more than most people realize. Dermatologists estimate that Malassezia folliculitis is frequently misdiagnosed as stubborn acne, particularly in teens and young adults with oily skin who present with forehead and chest breakouts.
The yeast itself, part of the Malassezia genus with species like M. globosa and M. restricta being the most common offenders, is a normal commensal organism found on virtually all human skin. Problems arise when conditions shift in the yeast’s favor, creating an overgrowth that overwhelms the follicle’s ability to self-regulate. This article breaks down the biological mechanism behind fungal acne, how to distinguish it from bacterial acne, what triggers flare-ups, and which treatments actually work versus those that make things worse.
Table of Contents
- What Is Malassezia Yeast and Why Does It Trigger Acne-Like Bumps?
- How to Tell the Difference Between Fungal and Bacterial Acne
- What Triggers Malassezia Overgrowth on the Skin
- Which Treatments Actually Work for Malassezia Folliculitis
- Skincare Ingredients That Feed Malassezia and Make Things Worse
- The Role of Diet and Internal Factors in Malassezia Flare-Ups
- Long-Term Management and Preventing Recurrence
- Conclusion
- Frequently Asked Questions
What Is Malassezia Yeast and Why Does It Trigger Acne-Like Bumps?
Malassezia is a genus of lipophilic (fat-loving) fungi that colonize human skin shortly after birth. There are at least 18 recognized species, and most healthy adults carry several of them without issue. These yeasts cannot synthesize their own fatty acids, so they depend entirely on the lipids present in human sebum for survival. They produce lipase enzymes that break down triglycerides in sebum into free fatty acids and other byproducts. When this process happens inside a clogged or semi-occluded hair follicle, the metabolic byproducts — particularly oleic acid and other unsaturated fatty acids — irritate the follicular wall and provoke an inflammatory cascade. The immune system responds to this irritation by sending neutrophils and other inflammatory cells to the follicle, producing the visible redness, swelling, and pus that looks so much like a conventional pimple. The key difference is the trigger: in bacterial acne, C.
acnes bacteria proliferate and form biofilms within the follicle, while in fungal folliculitis, Malassezia organisms pack into the follicular infundibulum in large numbers. Under a microscope, a KOH preparation of a scraped fungal acne bump will reveal clusters of round yeast cells, sometimes described as having a “spaghetti and meatballs” appearance when hyphae are also present. A standard acne lesion tested the same way would show no such organisms. This is why a punch biopsy or simple skin scraping can be diagnostic when clinical presentation alone leaves the picture murky. Compared to bacterial acne, fungal folliculitis tends to appear suddenly and spread quickly across a region rather than developing gradually over weeks. Someone might wake up one morning after a sweaty weekend with dozens of small bumps across their upper back and chest that seemingly came out of nowhere. Bacterial acne rarely behaves this way — it builds slowly as individual pores become clogged and infected over time.

How to Tell the Difference Between Fungal and Bacterial Acne
The most reliable clinical clue is uniformity. Fungal acne bumps are almost all the same size, typically one to two millimeters in diameter, and they lack the diversity of lesion types seen in bacterial acne. With conventional acne, you’ll usually find a mix of open comedones (blackheads), closed comedones (whiteheads), inflamed papules of varying sizes, and sometimes deeper nodules or cysts. Fungal folliculitis skips the comedone stage entirely and presents as a crop of near-identical inflamed papules or pustules. The bumps also tend to be intensely itchy, which is unusual for standard acne — most bacterial pimples are painful or sore to the touch, but itching is not a primary symptom. Location is another differentiator. Malassezia folliculitis favors the trunk, upper arms, shoulders, and forehead — areas with high sebaceous gland density and frequent occlusion from clothing or hair.
While bacterial acne certainly appears in these areas too, fungal acne rarely affects the lower face and jawline the way hormonal bacterial acne does. However, if someone has both conditions simultaneously — which is not uncommon — the picture becomes considerably more confusing. A person with oily skin can absolutely have C. acnes-driven acne on their chin and Malassezia-driven folliculitis on their forehead at the same time. In those cases, a treatment plan targeting only one organism will produce partial improvement at best, and the persistent bumps in the untreated zone will seem inexplicably resistant. One important limitation of self-diagnosis: many online “fungal acne” guides rely heavily on the visual appearance and itch factor, but several other conditions mimic this presentation. Gram-negative folliculitis, eosinophilic folliculitis, and even early contact dermatitis can produce uniform itchy bumps. If over-the-counter antifungal treatments do not produce noticeable improvement within two to three weeks, that is a strong signal to see a dermatologist for a proper workup rather than continuing to self-treat based on internet photos.
What Triggers Malassezia Overgrowth on the Skin
The shift from harmless colonization to symptomatic overgrowth usually requires a change in the skin’s microenvironment. The most common trigger is prolonged occlusion combined with heat and moisture. Athletes, people living in tropical climates, and anyone who sits in sweaty workout clothes for hours after exercising are prime candidates. One well-documented pattern involves college students who develop widespread truncal folliculitis after starting a new gym routine — they exercise in synthetic fabrics, drive home, and sit around for another hour before showering. That window of warm, moist, sebum-rich skin underneath non-breathable clothing is precisely what Malassezia needs to shift from commensal to pathogenic densities. Antibiotic use is another significant and often overlooked trigger. Broad-spectrum antibiotics, particularly tetracyclines like doxycycline and minocycline, are first-line treatments for moderate bacterial acne.
These antibiotics suppress competing bacterial flora on the skin, effectively removing Malassezia’s main ecological competitors. With the bacterial population reduced, Malassezia faces less competition for follicular real estate and lipid resources, and its population can expand rapidly. This creates a frustrating paradox: a person takes antibiotics for acne, their bacterial pimples improve, but a new crop of itchy uniform bumps appears in their place. Without recognizing the fungal etiology, they may stay on antibiotics longer, further worsening the fungal overgrowth. Immunosuppression, whether from medications like corticosteroids and immunomodulators or from conditions like HIV, also predisposes people to Malassezia overgrowth. Topical corticosteroid use on the face and body is a particularly sneaky trigger because steroids suppress the local immune response that normally keeps yeast populations in check, and they can also thin the skin and alter sebum composition. A person applying a mid-potency steroid cream to what they believe is eczema on their forehead might actually be feeding a fungal folliculitis that worsens with each application.

Which Treatments Actually Work for Malassezia Folliculitis
The cornerstone of treatment is antifungal therapy, and the choice between topical and oral options depends on severity and distribution. For mild to moderate cases confined to a limited area, topical azole antifungals like ketoconazole two percent cream or econazole cream applied once or twice daily for two to four weeks are effective and carry minimal side effects. Ketoconazole two percent shampoo used as a body wash — lathered on, left in contact with the skin for five to ten minutes, then rinsed — is a popular and practical approach because it covers large surface areas efficiently. Selenium sulfide and zinc pyrithione shampoos work similarly by reducing Malassezia populations on contact, though they tend to be somewhat less potent than ketoconazole. For widespread or treatment-resistant cases, oral antifungals become necessary. Oral itraconazole, typically dosed at 200 milligrams daily for one to two weeks, is the most commonly prescribed systemic option and has strong evidence behind it.
Oral fluconazole is an alternative, though it has slightly less activity against some Malassezia species. The tradeoff with systemic antifungals is the risk of side effects, particularly hepatotoxicity with prolonged use, and drug interactions — itraconazole in particular interacts with a long list of medications metabolized by the CYP3A4 enzyme system. For this reason, dermatologists generally reserve oral therapy for cases that genuinely need it rather than prescribing it as a first-line convenience. One critical comparison: benzoyl peroxide, a staple of bacterial acne treatment, does have some antifungal properties and may provide mild benefit against Malassezia. However, it is far less effective than dedicated antifungal agents for this purpose. Salicylic acid similarly offers modest help by exfoliating the follicular opening and reducing the occlusive environment Malassezia exploits, but it will not resolve an active overgrowth on its own. Relying on these acne-focused products instead of proper antifungals is one of the most common reasons people plateau in their treatment.
Skincare Ingredients That Feed Malassezia and Make Things Worse
Perhaps the most counterintuitive aspect of managing fungal acne is that many popular skincare products actively promote Malassezia growth. Because the yeast feeds on specific lipids — particularly fatty acids with carbon chain lengths between 11 and 24 — any product containing these lipids as ingredients essentially provides a buffet for the organism. Common offenders include oils like coconut oil, olive oil, and jojoba oil; fatty alcohols like cetyl alcohol and cetearyl alcohol; esters like isopropyl palmitate and glyceryl stearate; and polysorbate emulsifiers. Many mainstream moisturizers, sunscreens, and even some “acne-fighting” products contain one or more of these ingredients. This does not mean every product containing a fatty acid will cause a flare-up, and individual sensitivity varies considerably. The dose matters, the formulation matrix matters, and the specific Malassezia species colonizing a person’s skin matters.
However, someone who has confirmed Malassezia folliculitis should audit their routine and switch to products formulated without these known feeding ingredients. Brands and community resources focused on “fungal acne safe” formulations have become increasingly available, cross-referencing ingredient lists against the known lipid preferences of common Malassezia species. The limitation here is that the science on exactly which lipid structures feed which species is still incomplete, so these safe lists are educated approximations rather than guarantees. A practical warning: switching to a fungal-safe routine while simultaneously treating with antifungals can cause a temporary worsening or “purge” as the skin adjusts. Stripping all lipids from a skincare routine can compromise the skin barrier, leading to increased transepidermal water loss, irritation, and paradoxically more sebum production as the skin tries to compensate. The goal is targeted ingredient avoidance, not complete lipid elimination from the routine.

The Role of Diet and Internal Factors in Malassezia Flare-Ups
The connection between diet and Malassezia folliculitis is less direct than the connection between diet and bacterial acne, but it exists through the mechanism of sebum production. Diets high in refined sugars and high-glycemic carbohydrates stimulate insulin and insulin-like growth factor 1, which in turn upregulate sebaceous gland activity and increase sebum output. More sebum means more lipid substrate for Malassezia within the follicle.
A college student who shifts from a relatively balanced diet to a steady intake of energy drinks, pizza, and late-night snacks during exam season might notice a corresponding uptick in follicular bumps — not because the food directly feeds the yeast, but because the hormonal cascade triggered by those foods creates a more hospitable environment for it. Stress operates through a similar indirect pathway. Elevated cortisol increases sebum production and can also modestly suppress aspects of cutaneous immunity, both of which favor Malassezia proliferation. While dietary and stress management alone will not cure an active case of fungal folliculitis, ignoring these factors while relying solely on topical antifungals often leads to a frustrating cycle of clearance and relapse.
Long-Term Management and Preventing Recurrence
Malassezia folliculitis has a high recurrence rate because the yeast is a permanent resident of human skin — you cannot eradicate it, only control its population density. Maintenance therapy is therefore a practical reality for many people prone to flare-ups. Using ketoconazole or zinc pyrithione wash once or twice weekly as a preventive measure after the acute infection has cleared is a widely recommended strategy that carries minimal risk.
Some dermatologists also recommend a single monthly dose of oral itraconazole for patients with particularly stubborn recurrence patterns, though the long-term safety data on this approach is still evolving. Looking ahead, research into the skin microbiome is beginning to reveal more sophisticated interventions. Probiotic approaches aimed at bolstering the bacterial competitors that naturally keep Malassezia in check, targeted bacteriophage therapy, and next-generation topical antifungals with fewer resistance concerns are all in various stages of investigation. For now, the most effective long-term strategy remains a combination of antifungal maintenance therapy, a skincare routine free of Malassezia-feeding ingredients, breathable fabrics, prompt post-exercise showering, and awareness of the triggers — particularly antibiotic use and occlusion — that tilt the balance in the yeast’s favor.
Conclusion
Malassezia folliculitis is one of the most commonly misidentified skin conditions, routinely mistaken for bacterial acne and treated with therapies that either do nothing or actively worsen the problem. The mechanism is straightforward: a lipid-dependent yeast that normally lives peacefully on the skin overgrows within hair follicles when conditions favor it, producing inflammatory byproducts that trigger uniform, itchy bumps. Recognizing the hallmarks — monomorphic papules, intense itch, trunk and forehead predominance, failure to respond to standard acne treatments — is the first step toward proper management.
Effective treatment requires antifungal agents rather than antibacterial ones, a skincare routine that avoids feeding the organism, and an honest assessment of lifestyle factors like occlusive clothing, shower timing, and antibiotic history. For those who confirm a Malassezia component to their skin problems, the improvement from targeted antifungal therapy is often dramatic and fast, sometimes visible within the first week. The ongoing challenge is maintenance, since the yeast will always be present and ready to exploit any shift in conditions. Building antifungal washes into a regular routine and staying vigilant about ingredient lists is not a temporary fix but a permanent adjustment — one that pays off in consistently clearer skin.
Frequently Asked Questions
Can I have fungal acne and regular acne at the same time?
Yes, and this is actually common. The two conditions are not mutually exclusive because they involve different organisms exploiting the same follicular environment. Treatment needs to address both — an antifungal for the Malassezia component and conventional acne therapy for the bacterial component. Using only one approach will leave the other condition untreated.
How quickly does fungal acne respond to antifungal treatment?
Most people notice visible improvement within five to seven days of starting appropriate antifungal therapy, whether topical or oral. Full clearance typically takes two to four weeks. If there is no improvement after three weeks of consistent antifungal use, the diagnosis should be reconsidered with a dermatologist.
Does fungal acne leave scars?
Malassezia folliculitis generally does not cause the deep scarring associated with severe cystic bacterial acne because the lesions are superficial. However, picking or squeezing the bumps can cause post-inflammatory hyperpigmentation, particularly in darker skin tones, which may take months to fade.
Is fungal acne contagious?
No. Malassezia yeast is already present on virtually every person’s skin. You cannot catch fungal folliculitis from someone else. The condition develops due to changes in your own skin environment that allow the resident yeast population to overgrow, not from exposure to an external source.
Can I use tea tree oil to treat fungal acne?
Tea tree oil does have antifungal properties and some people report improvement using it. However, it is significantly less potent than ketoconazole or other azole antifungals, and it can cause contact dermatitis in sensitive individuals. It is reasonable as a supplementary ingredient but unreliable as a primary treatment for active fungal folliculitis.
You Might Also Like
- Why Chemotherapy Causes Acne-Like Rashes
- Why Stopping Birth Control Causes an Acne Flare
- Why Insulin Resistance Causes Acne
Browse more: Acne | Acne Scars | Adults | Back | Blackheads