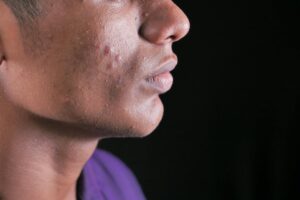
Demodex mites — microscopic arachnids that live in your hair follicles and oil glands — can trigger inflammatory breakouts that look virtually identical to acne but won’t respond to standard acne treatments. When these mites overpopulate, they clog follicles, provoke immune reactions, and release inflammatory substances as they die, producing papules, pustules, and redness that even experienced dermatologists sometimes misdiagnose as acne vulgaris. A 2023 study published in PMC found Demodex positivity in 42.6% of acne patients compared to just 12.3% of controls, a statistically significant difference that underscores how often these organisms play a role in what people assume is ordinary acne.
The distinction matters more than most people realize. If your breakouts are driven by Demodex overgrowth rather than the hormonal and bacterial processes behind classic comedonal acne, then retinoids, benzoyl peroxide, and antibiotics may do little or nothing for you. The fix requires acaricidal treatments — medications that kill the mites themselves. This article covers what Demodex mites actually are, how researchers have linked them to breakouts, why demodicosis is so frequently mistaken for acne, the surprising connection to rosacea, and what the latest 2025 research says about treatment options that work.
Table of Contents
- How Are Demodex Mites Connected to Skin Breakouts?
- Why Demodicosis Gets Misdiagnosed as Acne
- The Rosacea Connection and What It Reveals About Demodex
- Treatments That Actually Target Demodex Mites
- The Problem with Natural Remedies for Demodex
- When to Suspect Demodex Is Behind Your Breakouts
- Where Demodex Research Is Heading
- Conclusion
- Frequently Asked Questions
How Are Demodex Mites Connected to Skin Breakouts?
Two species of Demodex live on human skin. *Demodex folliculorum* takes up residence inside hair follicles, while *Demodex brevis* burrows into sebaceous glands. Both are tiny — between 0.15 and 0.4 mm — and research by Megan Thoemmes and colleagues found that 100% of adults over 18 carry them. At low densities of five or fewer mites per square centimeter, most people never notice. The mites feed on sebum and skin cells, and in normal numbers they are essentially harmless passengers on your face. Problems begin when that population explodes. When Demodex mites overpopulate — a condition called demodicosis — they physically clog follicles with their bodies and waste products.
The immune system responds with inflammation, producing red, swollen papules and pustules that are clinically indistinguishable from acne. Making things worse, when the mites die, their decomposing bodies release substances that further aggravate the inflammatory cascade. This creates a self-reinforcing cycle: inflammation damages the follicular environment, which can allow even more mites to accumulate. A 2012 meta-analysis of observational studies confirmed an overall association between acne vulgaris and Demodex infestation across multiple study populations. However, the relationship is not perfectly straightforward. A 2024 study in *Clinical, Cosmetic and Investigational Dermatology* found no significant difference in Demodex prevalence between patients with acne alone and healthy controls. The difference only became significant when acne patients also had nonspecific facial dermatitis — patchy redness, dry or scaly skin, and insect bite-like papules. This suggests Demodex may be more of a complicating factor in certain acne presentations than a universal cause of breakouts.

Why Demodicosis Gets Misdiagnosed as Acne
Demodicosis is a shape-shifter. It can present as pityriasis folliculorum (fine scaling around follicles), rosacea-like flushing and papules, folliculitis-like bumps, or perioral dermatitis-like clusters around the mouth. A 2022 PMC case report documented demodicosis imitating acne vulgaris so convincingly that the patient had been treated unsuccessfully with standard acne regimens before anyone thought to check for mites. This pattern of delayed diagnosis is common enough that a 2025 review paper published in *Infection* (Springer Nature) called Demodex a “neglected cause of skin disease” and urged greater clinical awareness. The practical consequence of misdiagnosis is wasted time and worsening skin.
Someone with Demodex-driven breakouts might cycle through benzoyl peroxide, topical retinoids, oral antibiotics, and even isotretinoin without meaningful improvement. Each failed treatment is demoralizing and potentially exposes the skin to unnecessary side effects. If your breakouts are concentrated around the nose, cheeks, and perioral area, if they include a fine scaly texture alongside papules, or if they have resisted multiple conventional acne treatments, Demodex overgrowth deserves consideration. However, it is worth noting that not every treatment-resistant breakout is demodicosis. Fungal acne (Malassezia folliculitis), hormonal acne along the jawline, and contact dermatitis can also mimic or complicate acne vulgaris. The key differentiator for Demodex is a skin scraping or biopsy — a simple in-office test where a dermatologist examines follicular material under a microscope to count mite density.
The Rosacea Connection and What It Reveals About Demodex
The strongest evidence linking Demodex to skin disease comes not from acne research but from rosacea studies. According to the National Rosacea Society, Demodex mites are found in 15 to 18 times greater numbers on the skin of rosacea patients compared to healthy subjects. That is not a subtle difference — it is an order-of-magnitude overpopulation that strongly implicates the mites in disease pathology. The mechanism goes beyond simple physical obstruction. Demodex mites carry a bacterium called *Bacillus oleronius*, and in a study funded by the National Rosacea Society, this bacterium stimulated an inflammatory immune response in 79% of patients with papulopustular rosacea.
Researchers Forton and colleagues went further, concluding after molecular, histologic, and clinical analysis that papulopustular rosacea is actually caused by Demodex rather than the other way around. This is a significant claim — it reframes a common skin condition as fundamentally a parasitic disease. For people dealing with breakouts, the rosacea research matters because it validates the biological plausibility of Demodex-driven skin inflammation. If mites can cause the bumps and redness of rosacea, it follows that similar overgrowth in a slightly different context could produce breakouts indistinguishable from acne. Anyone who has been told they have both acne and rosacea, or whose diagnosis seems to shift between the two, should ask their dermatologist about Demodex testing.

Treatments That Actually Target Demodex Mites
When Demodex overgrowth is confirmed, the treatment approach shifts entirely from acne-focused products to acaricidal agents — medications designed to kill the mites. Topical ivermectin 1% remains the clinical mainstay, offering dual acaricidal and anti-inflammatory action. In vitro studies show it achieves a median kill time of approximately 14 minutes. It is generally well tolerated, and a 2025 systematic review and meta-analysis in PMC confirmed its efficacy across multiple studies. A newer option, lotilaner 0.25% (marketed as Xdemvy), was FDA-approved for Demodex blepharitis and has shown the most consistent median kill time in laboratory testing at roughly 12 minutes. While its current approval is limited to eyelid disease, the data suggests potential for broader dermatologic applications.
For cases where topical therapy alone is insufficient, dermatologists may prescribe oral ivermectin combined with topical permethrin 5%, a regimen that attacks the mites from both systemic and surface-level routes. The tradeoff between these options involves access, cost, and side effect profiles. Topical ivermectin is the most widely available and best studied for facial skin conditions. Lotilaner is newer, potentially faster-acting, but approved for a narrower indication and often more expensive. Oral ivermectin is powerful but carries systemic side effects including dizziness and gastrointestinal discomfort. For most people with Demodex-driven facial breakouts, topical ivermectin is the reasonable starting point, with escalation to combination therapy if the initial approach falls short.
The Problem with Natural Remedies for Demodex
Tea tree oil appears frequently in online discussions about Demodex treatment, and it does have genuine acaricidal properties in laboratory settings. The critical limitation, however, is that tea tree oil is not effective at killing Demodex below 50% concentration, and at those high concentrations it is irritating to facial skin. Using diluted tea tree oil products at the 1% to 5% concentrations found in most commercial formulations is unlikely to deliver meaningful mite reduction, despite what product labels might imply. Lemongrass oil showed more promise in one in vitro study, achieving the fastest complete mite mortality at approximately 14.5 minutes.
But this result has not been validated in living human skin, where penetration, absorption, and tolerability are entirely different considerations than in a petri dish. Emerging agents like niclosamide and berberine outperformed tea tree oil in vitro with favorable safety profiles according to a 2025 meta-analysis in PMC, but these too require further clinical trials before they can be recommended with confidence. The broader warning here is about the gap between in vitro and clinical reality. A substance that kills mites in a laboratory dish may not penetrate the follicle adequately, may irritate the skin at effective doses, or may not maintain sufficient concentration long enough to eliminate a mite population that reproduces continuously. Anyone who has spent months applying tea tree oil to treatment-resistant breakouts without improvement should consider that the product may simply not be reaching therapeutic levels on their skin, and it may be time to pursue a prescription approach.

When to Suspect Demodex Is Behind Your Breakouts
Consider Demodex as a factor if your breakouts have a few specific characteristics. Persistent facial redness alongside papules and pustules, especially concentrated on the cheeks, nose, chin, and forehead, is suggestive. Fine scaling or a sandpaper-like texture around follicles is a hallmark of pityriasis folliculorum, one of the classic demodicosis presentations. Perhaps the most telling sign is treatment resistance — if multiple conventional acne therapies over months or years have failed to produce improvement, or if your skin initially responds but relapses quickly once treatment stops, Demodex overgrowth deserves investigation.
A standard skin surface biopsy or scraping is the diagnostic method. Your dermatologist applies a drop of oil to the skin, gently scrapes or presses a glass slide against the affected area, and counts mites under magnification. Densities above five mites per square centimeter are generally considered pathological. This is a quick, inexpensive test that can fundamentally change the treatment direction for people stuck in a cycle of failed acne regimens.
Where Demodex Research Is Heading
The trend in Demodex research is toward greater clinical recognition and more targeted treatments. The 2025 *Infection* review calling Demodex a neglected cause of skin disease reflects a growing push within dermatology to make mite testing more routine, particularly for patients with treatment-resistant inflammatory skin conditions. As lotilaner and emerging agents like niclosamide move through clinical development for broader dermatologic use, the treatment options available to patients should expand meaningfully in the coming years. Perhaps the most important shift is conceptual.
For decades, Demodex mites were treated as curiosities — ubiquitous but clinically irrelevant. The accumulating evidence from acne, rosacea, and blepharitis research tells a different story. These organisms are not always harmless commensals, and when they overgrow, the inflammatory consequences can be significant. Recognizing that some breakouts are mite-driven rather than bacteria-driven or hormone-driven opens the door to treatments that actually address the root cause.
Conclusion
Demodex mites do not cause the classic blackheads and whiteheads of comedonal acne, but their overgrowth triggers inflammatory breakouts — red papules, pustules, and irritated skin — that look nearly identical to acne vulgaris. The research consistently shows higher Demodex densities in patients with inflammatory skin conditions, and the 2023 finding of 42.6% positivity in acne patients versus 12.3% in controls makes it difficult to dismiss these mites as irrelevant bystanders. The clinical challenge is that demodicosis is frequently misdiagnosed, leaving patients on ineffective acne treatments for months or years.
If your breakouts have resisted conventional acne therapies, bring up Demodex testing with your dermatologist. A simple skin scraping can confirm or rule out overgrowth, and effective treatments — particularly topical ivermectin — are available and well studied. The distinction between mite-driven and bacteria-driven breakouts matters because the treatments are fundamentally different, and no amount of retinoid or benzoyl peroxide will address an arachnid problem.
Frequently Asked Questions
Does everyone have Demodex mites on their face?
Yes. Research has found Demodex mites on 100% of adults over 18. At low densities of five or fewer mites per square centimeter, they cause no symptoms and are considered normal skin fauna.
How do I know if my breakouts are from Demodex and not regular acne?
The most reliable method is a skin scraping performed by a dermatologist, who examines follicular material under a microscope to count mite density. Clinical clues include treatment-resistant papules and pustules, fine scaling around follicles, and persistent facial redness, particularly on the cheeks and nose.
Can I treat Demodex mites with tea tree oil?
Tea tree oil has acaricidal properties in laboratory settings, but research shows it is not effective below 50% concentration — a level that causes skin irritation. Commercial products containing 1% to 5% tea tree oil are unlikely to kill mites at therapeutic levels. Prescription topical ivermectin is significantly more reliable.
Is Demodex overgrowth the same thing as rosacea?
Not exactly, but they are closely related. Demodex mites are found in 15 to 18 times greater numbers in rosacea patients, and some researchers have concluded that Demodex actually causes papulopustular rosacea. However, rosacea involves additional factors like vascular reactivity that extend beyond mite overgrowth alone.
What is the most effective prescription treatment for Demodex?
Topical ivermectin 1% is the current clinical standard, offering both mite-killing and anti-inflammatory effects. For more severe cases, dermatologists may prescribe oral ivermectin combined with topical permethrin 5%. Lotilaner 0.25% is a newer FDA-approved option currently indicated for Demodex blepharitis.
Can Demodex mites come back after treatment?
Yes. Because Demodex mites are universally present on human skin, the goal of treatment is to reduce their population to normal levels rather than eliminate them entirely. Recurrence is possible, and some patients require maintenance therapy to keep mite densities in check.
You Might Also Like
- Why Fungal Acne Looks Like Regular Breakouts but Isn’t
- Why Certain Medications Cause Acne Breakouts
- Which Probiotic Strains Help with Acne Specifically
Browse more: Acne | Acne Scars | Adults | Back | Blackheads