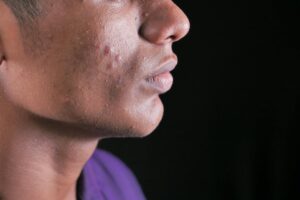
Cutibacterium acnes, the bacterium most people associate with breakouts and inflamed skin, is actually a normal and often beneficial resident of human skin. Far from being a straightforward villain, C. acnes plays a role in maintaining the skin’s acidic pH, competing against genuinely harmful pathogens, and contributing to the lipid balance that keeps skin hydrated. The reason you have this bacterium on your face right now — and have since adolescence — is because it evolved alongside human skin as part of a carefully balanced microbiome, not as an invader waiting to strike. The confusion stems from decades of dermatological messaging that framed acne as an infection to be eradicated. In reality, nearly every human carries C.
acnes on their skin, yet only a fraction develop significant acne. Research published in the Journal of Investigative Dermatology has shown that specific strains of C. acnes — not the species as a whole — are associated with acne, while other strains appear to actively protect skin health. A person with clear skin and a person with severe cystic acne may carry similar total quantities of C. acnes, but the strain composition tells a very different story. This article covers how C. acnes functions as a skin ally, which strains actually cause problems, why aggressive antibacterial approaches can backfire, and how emerging treatments aim to rebalance rather than destroy.
Table of Contents
- What Does Cutibacterium Acnes Actually Do on Healthy Skin?
- Which Strains of C. Acnes Cause Acne and Which Are Protective?
- How Antibiotics Disrupt the Skin Microbiome Beyond Killing Acne Bacteria
- Microbiome-Based Acne Treatments and How They Compare to Traditional Approaches
- When Killing C. Acnes Goes Too Far — The Rebound Effect
- C. Acnes in Contexts Beyond Acne — Surgical Infections and Implant Complications
- The Future of Personalized Skin Microbiome Management
- Conclusion
- Frequently Asked Questions
What Does Cutibacterium Acnes Actually Do on Healthy Skin?
C. acnes is a gram-positive, anaerobic bacterium that thrives in the oxygen-poor environment of hair follicles and sebaceous glands. It feeds on sebum, breaking down triglycerides into free fatty acids — a process that contributes to the skin‘s acid mantle, which hovers around a pH of 4.5 to 5.5. This acidic environment is inhospitable to many pathogenic organisms, including Staphylococcus aureus and Streptococcus pyogenes, both of which prefer a more neutral pH. In this sense, C. acnes functions as a gatekeeper, making the skin’s surface a hostile territory for bacteria that could cause genuine infections. Beyond pH regulation, C. acnes produces short-chain fatty acids like propionic acid, which have antimicrobial properties of their own. A 2013 study from the University of California, Los Angeles, found that certain C.
acnes strains secrete a protein called RoxP, an antioxidant that may protect skin cells from oxidative stress caused by UV exposure and pollution. Compare this to Staphylococcus epidermidis, another common skin commensal: while S. epidermidis also provides colonization resistance against pathogens, it does not contribute to sebum metabolism or produce the same antioxidant compounds. The two species work in tandem, each filling a different ecological niche on the skin’s surface. It is worth noting that the mere presence of C. acnes in a skin culture does not indicate disease, a point that older clinical practices sometimes got wrong. Culturing skin swabs and finding C. acnes was once treated as evidence of bacterial involvement in acne, leading to antibiotic prescriptions that may not have been necessary. The current understanding is more nuanced: what matters is not whether C. acnes is present, but which strains dominate and whether the surrounding environment — sebum overproduction, follicular hyperkeratinization, inflammation — has shifted the balance.

Which Strains of C. Acnes Cause Acne and Which Are Protective?
Not all C. acnes strains are created equal. Genomic studies, particularly a landmark 2013 paper in the Journal of Investigative Dermatology, used ribotyping and multilocus sequence typing to classify C. acnes into distinct phylotypes. Type IA-2 and type IC strains are significantly more common in acne patients and tend to carry virulence factors that amplify inflammation — including CAMP factor genes and genes involved in biofilm formation. These strains are more adept at triggering the innate immune system, provoking toll-like receptor 2 (TLR2) responses in keratinocytes and sebocytes that lead to the redness, swelling, and pain associated with inflammatory acne lesions. Type II and type III strains, by contrast, are more frequently found on the skin of individuals without acne. These strains appear to lack many of the inflammatory virulence factors and may actively modulate immune responses in ways that maintain tolerance rather than triggering alarm. A 2016 study from Washington University in St.
Louis went further, demonstrating that applying filtrates from healthy-skin-associated C. acnes strains could inhibit the growth of acne-associated strains in vitro. The implication is striking: some C. acnes strains may function as natural probiotics, keeping their more aggressive cousins in check. However, if a person’s skin environment shifts — due to hormonal changes during puberty, polycystic ovary syndrome, or even dietary factors that increase insulin-like growth factor 1 — the balance between protective and pathogenic strains can tip. Increased sebum production provides more fuel for all C. acnes strains, but the aggressive strains tend to outcompete their benign counterparts under high-sebum conditions. This means that strain typing alone does not predict acne outcomes; the host environment matters enormously. A person carrying type IA-2 strains may never develop acne if their sebum production remains moderate and follicular shedding stays normal.
How Antibiotics Disrupt the Skin Microbiome Beyond Killing Acne Bacteria
For decades, oral and topical antibiotics — tetracyclines, erythromycin, clindamycin — were the default treatment for moderate to severe acne. These drugs do reduce C. acnes populations and can produce visible improvement, but they operate like carpet bombing when precision strikes would be more appropriate. Broad-spectrum antibiotics do not distinguish between pathogenic and protective C. acnes strains, and they simultaneously decimate other commensal organisms that contribute to skin health. A well-documented example is the rise of antibiotic-resistant C. acnes strains. Data from the British Society for Antimicrobial Chemotherapy has shown that resistance rates to erythromycin among C.
acnes isolates exceed 50 percent in some European countries, rendering the drug largely useless for those populations. Clindamycin resistance often follows, since the two antibiotics share a similar mechanism of action. Patients who have cycled through multiple antibiotic courses may find that they have selectively bred the most resistant — and often most virulent — strains on their own skin, while wiping out the protective ones. The 2024 guidelines from the American Academy of Dermatology now explicitly recommend limiting antibiotic courses to three months and always pairing them with benzoyl peroxide to reduce resistance development. The collateral damage extends beyond C. acnes. Oral antibiotics alter the gut microbiome, which has its own emerging connections to skin health through the gut-skin axis. Patients on long-term doxycycline for acne frequently report gastrointestinal side effects, and there is growing evidence that disruption of gut flora can influence systemic inflammation in ways that paradoxically worsen skin conditions over time. This does not mean antibiotics should never be used — for severe nodulocystic acne, they remain an important tool — but their role is increasingly viewed as short-term and transitional rather than foundational.

Microbiome-Based Acne Treatments and How They Compare to Traditional Approaches
The recognition that acne involves microbial imbalance rather than simple infection has opened the door to treatments that aim to restore healthy strain ratios rather than sterilize the skin. Several companies and research groups are developing topical probiotics and bacteriophage therapies specifically targeting pathogenic C. acnes strains while leaving beneficial ones intact. Phage therapy is particularly promising. Bacteriophages are viruses that infect and kill specific bacterial strains with remarkable precision. Researchers at UCLA and other institutions have identified phages that selectively target acne-associated C. acnes strains without affecting the protective phylotypes.
In early-stage clinical work, phage preparations applied topically reduced inflammatory lesion counts comparably to benzoyl peroxide but without the dryness, peeling, and bleaching side effects that make benzoyl peroxide difficult for many patients to tolerate. The tradeoff is that phage therapy is not yet commercially available for acne, and questions remain about whether bacteria can develop phage resistance in a clinical setting, as they readily do in laboratory conditions. Topical prebiotics — formulations containing compounds that preferentially feed beneficial C. acnes strains — represent another approach. Some skincare lines now include fermented ingredients or specific fatty acid profiles designed to favor type II and III strains. The evidence for these products remains largely preclinical, and consumers should be skeptical of marketing claims that outpace published data. Compared to retinoids, which address acne through a completely different mechanism (normalizing follicular keratinization and reducing sebum production), microbiome-based approaches are still in their infancy. For most patients today, a retinoid remains the single most effective long-term acne treatment, but the two approaches are not mutually exclusive and may eventually be combined.
When Killing C. Acnes Goes Too Far — The Rebound Effect
One of the least discussed consequences of aggressive anti-acne regimens is the rebound effect that occurs when treatment is abruptly stopped. Patients who have used strong antibacterial agents — whether antibiotics, high-concentration benzoyl peroxide, or antiseptic washes — for extended periods can experience a flare of acne that is worse than their baseline when they discontinue treatment. This happens in part because the skin microbiome has been depleted of its normal diversity, creating open ecological niches that pathogenic strains are well-positioned to fill. A related warning applies to the popular practice of using alcohol-based toners, harsh sulfate cleansers, or physical scrubs in an attempt to “kill bacteria” on the skin. These approaches strip the acid mantle and damage the stratum corneum, paradoxically increasing transepidermal water loss and triggering compensatory sebum overproduction. The result is skin that is simultaneously dry, irritated, and oily — an environment where the most aggressive C. acnes strains thrive.
Dermatologists increasingly advise patients to use gentle, pH-balanced cleansers and to treat the skin barrier as an ecosystem worth protecting, not an obstacle to scrub through. There is also the matter of biofilms. Pathogenic C. acnes strains can form biofilms within follicles — structured bacterial communities encased in a polysaccharide matrix that is remarkably resistant to both antibiotics and the host immune response. Aggressive topical treatments may kill planktonic (free-floating) bacteria on the surface while leaving biofilm communities untouched deep within pores. When surface competition is eliminated, biofilm-associated bacteria can repopulate the skin without the competitive pressure that protective strains once provided. This is one reason why acne often returns in the same locations: the biofilm architecture persists even when the skin appears clear.

C. Acnes in Contexts Beyond Acne — Surgical Infections and Implant Complications
C. acnes is not only a skin commensal; it is also a recognized cause of postoperative infections, particularly in shoulder surgery. Orthopedic surgeons have long known that C. acnes colonizes the deeper layers of shoulder skin at unusually high densities, and standard preoperative skin preparation with chlorhexidine or povidone-iodine often fails to eliminate it from the follicular reservoir. Studies have reported C.
acnes isolation rates of 30 to 40 percent in culture samples taken from the glenohumeral joint during shoulder arthroplasty, even with proper sterile technique. This surgical context underscores an important point: the same organism that causes no harm on intact skin can become a serious pathogen when introduced into a joint space or around an implant. C. acnes infections of prosthetic joints are notoriously indolent, sometimes taking months or years to become symptomatic, and they are difficult to treat because the bacterium forms biofilms on implant surfaces. Understanding that C. acnes is a permanent and ineradicable skin resident — not a contaminant that can be sterilized away — has led to changes in surgical protocols, including the use of preoperative benzoyl peroxide washes for several days before shoulder procedures.
The Future of Personalized Skin Microbiome Management
The trajectory of acne research points toward a future where treatment is guided by individual microbiome profiling rather than one-size-fits-all protocols. Several direct-to-consumer skin microbiome testing kits already exist, though their clinical utility remains limited by incomplete reference databases and a lack of standardized interpretation frameworks. As strain-level genomic data accumulates and is correlated with treatment outcomes, it will become increasingly feasible to prescribe targeted interventions — specific phage cocktails, probiotic formulations, or even strain-replacement therapies — based on a patient’s unique microbial signature. The broader shift is philosophical as much as technological.
Decades of treating skin bacteria as the enemy produced a generation of patients conditioned to strip, scrub, and sterilize their skin. The emerging science makes clear that a healthy skin microbiome, including its C. acnes populations, is an asset that warrants protection. The most effective acne strategies of the future will likely be those that work with the microbiome rather than against it, suppressing pathogenic strains while nurturing the ones that have been quietly defending your skin all along.
Conclusion
Cutibacterium acnes is not the straightforward enemy that decades of acne treatment marketing made it out to be. It is a complex, strain-diverse organism that contributes to skin barrier defense, pH regulation, and pathogen resistance in its beneficial forms, while specific strains drive inflammation and breakouts in susceptible individuals. The distinction between helpful and harmful C.
acnes — and the recognition that indiscriminate killing of all strains often makes things worse — represents one of the most important shifts in modern dermatology. For anyone managing acne, the practical takeaway is to favor targeted, barrier-respecting treatments over broad-spectrum antimicrobial warfare. Retinoids, judicious short-course antibiotics paired with benzoyl peroxide, gentle cleansing, and patience with the skin’s recovery process will serve most people better than aggressive regimens that treat every bacterium as an invader. As microbiome-based therapies mature, the options will only expand — but the underlying principle will remain the same: healthy skin is not sterile skin, and the bacteria living on your face are, for the most part, doing you a favor.
Frequently Asked Questions
Is Cutibacterium acnes the same thing as Propionibacterium acnes?
Yes. The organism was reclassified and renamed from Propionibacterium acnes to Cutibacterium acnes in 2016 based on genomic analysis. Older studies and some product labels still use the previous name. They refer to the same bacterium.
Can I test which strains of C. acnes I have on my skin?
Some direct-to-consumer microbiome testing kits claim to identify skin bacteria at the strain level, but the clinical usefulness of these tests is still limited. There is no widely accepted protocol for using strain data to guide acne treatment in routine practice. This may change within the next several years as research databases grow.
Does benzoyl peroxide kill all C. acnes strains equally?
Benzoyl peroxide works by generating free radicals that are broadly toxic to anaerobic bacteria, so it does not discriminate well between strains. However, because it works through oxidative damage rather than a mechanism bacteria can easily develop resistance to, it remains effective even against antibiotic-resistant strains. The tradeoff is that it also reduces beneficial strain populations.
Should I stop washing my face to protect my skin microbiome?
No. Gentle cleansing with a pH-balanced, non-foaming or mildly foaming cleanser removes excess sebum, dead skin cells, and environmental debris without significantly disrupting the microbiome. The problem is over-cleansing — using harsh surfactants, alcohol-based products, or scrubbing multiple times daily — which strips the acid mantle and damages commensal populations.
Are probiotic skincare products effective for acne?
The evidence is early and mixed. Some small studies show that topical application of certain Lactobacillus or Bifidobacterium strains can reduce inflammation and improve acne, but formulation stability, strain viability on the skin, and optimal dosing are all unresolved questions. These products are not a proven replacement for established acne treatments but may become a useful complement as research progresses.
You Might Also Like
- Why Your Gut Health Directly Affects Your Acne
- Why Stopping Birth Control Causes an Acne Flare
- Why Rosacea Gets Mistaken for Acne
Browse more: Acne | Acne Scars | Adults | Back | Blackheads