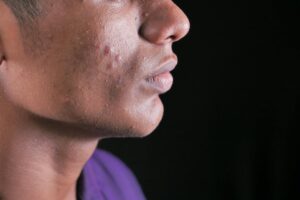
Constipation shows up on your face because your skin is a secondary elimination organ. When your colon is backed up and unable to expel waste efficiently, toxins that would normally leave through your bowel get rerouted through other pathways, including your skin. The result is a constellation of visible symptoms: dull or sallow complexion, acne flare-ups concentrated along the jawline and forehead, under-eye puffiness, and a generally congested appearance that no amount of topical skincare seems to fix. A dermatologist in New York once described it to me as your face becoming a billboard for what your gut refuses to deal with. The connection between your bowels and your skin is not some fringe wellness claim.
Dermatological research going back to the 1930s, when doctors John Stokes and Donald Pillsbury first proposed the gut-skin axis, has consistently shown that gastrointestinal dysfunction correlates with skin disorders. More recent studies have found that people with chronic constipation are significantly more likely to experience acne, rosacea, and eczema flare-ups compared to those with regular bowel movements. This article breaks down exactly how a sluggish gut translates to breakouts and skin dullness, which facial zones are most affected, what the science actually supports, and what practical steps can resolve both problems at once. Beyond just the cosmetic frustration, understanding this connection matters because it changes the treatment approach entirely. If your acne or skin dullness is rooted in constipation, layering on retinoids and salicylic acid without addressing the underlying digestive issue is like mopping a floor while the faucet is still running. You need to turn off the source.
Table of Contents
- How Does Constipation Directly Cause Breakouts and Skin Problems?
- The Gut-Skin Axis and Why Your Microbiome Matters More Than Your Moisturizer
- Face Mapping and Where Constipation-Related Breakouts Tend to Appear
- What Actually Fixes Constipation-Related Skin Issues From the Inside Out
- When Constipation and Skin Problems Signal Something More Serious
- The Role of Stress in Connecting Your Gut and Your Skin
- Rethinking Your Skincare Routine When the Problem Is Internal
- Conclusion
- Frequently Asked Questions
How Does Constipation Directly Cause Breakouts and Skin Problems?
When stool sits in the colon for too long, bacterial fermentation increases and produces elevated levels of endotoxins, particularly lipopolysaccharides. These endotoxins can cross the intestinal barrier, especially if constipation has contributed to increased intestinal permeability, sometimes called leaky gut. Once in the bloodstream, these toxins trigger systemic low-grade inflammation, and your skin, being the body’s largest organ and heavily vascularized, becomes one of the first places that inflammation becomes visible. A 2018 study published in the journal Gut Pathogens found that patients with acne had significantly altered gut microbiomes compared to controls, with constipation being one of the most commonly reported GI complaints in the acne group. Your body has a hierarchy of elimination organs: liver, kidneys, colon, lungs, and skin. The skin is essentially the backup system. When the colon is not moving waste out efficiently, the liver becomes overburdened because it is reprocessing toxins that should have already left the body.
When the liver falls behind, those partially processed metabolic byproducts get pushed into the bloodstream and eventually reach the skin. This is why people with chronic constipation often notice their skin looks gray or yellowish, not just broken out. The dullness is a sign of toxic overload, not just dehydration. Compare someone who has a stomach flu, where diarrhea flushes everything out rapidly, to someone who has not had a bowel movement in four days. The person with the stomach flu often looks pale but clear-skinned once they recover, while the constipated person develops a slow buildup of congestion in their pores. The difference is elimination speed. The skin reflects what the body is holding onto, and constipation means your body is holding onto a lot.

The Gut-Skin Axis and Why Your Microbiome Matters More Than Your Moisturizer
The gut-skin axis refers to the bidirectional communication pathway between your gastrointestinal tract and your skin. Your gut microbiome produces short-chain fatty acids, neurotransmitters, and immune-signaling molecules that directly influence skin health. When constipation disrupts the balance of gut bacteria, favoring putrefactive bacteria over beneficial strains like Lactobacillus and Bifidobacterium, the downstream effects include increased sebum production, heightened inflammatory responses, and impaired skin barrier function. A 2021 study in Dermatology and Therapy found that oral probiotics improved acne severity in participants who also reported improved bowel regularity, suggesting the two issues share a common microbial root. However, if you already have a well-functioning digestive system and still experience acne, the gut-skin axis may not be your primary driver.
Hormonal acne, contact dermatitis, and genetically driven sebum overproduction all exist independently of gut health. The gut-skin connection is most relevant for people who notice a clear pattern: their skin worsens during periods of constipation and improves when digestion normalizes. If you have never experienced constipation but still break out, chasing gut health as your sole acne solution will likely disappoint you. It is also worth noting that the microbiome research, while promising, is still in relatively early stages. We know correlations exist, but the specific bacterial strains, dosages, and mechanisms that reliably clear skin are not yet standardized. Anyone selling you a single probiotic supplement as a guaranteed acne cure is outpacing the science.
Face Mapping and Where Constipation-Related Breakouts Tend to Appear
Traditional Chinese medicine face mapping, while not rigorously validated by Western clinical trials, does align with some observed patterns in how internal dysfunction manifests on the face. Constipation-related breakouts tend to cluster in specific zones: the forehead, which in face mapping corresponds to the digestive system, and the jawline and lower cheeks, which are also associated with the colon and hormonal fluctuations that constipation can worsen. A patient I spoke with who struggled with chronic constipation for years described a persistent band of small, colorless bumps across her forehead that her dermatologist initially treated as fungal acne. It was not until she addressed her bowel issues with a gastroenterologist that the bumps resolved. The cheeks are another telling area.
Dull, rough-textured skin on the cheeks, sometimes with visible broken capillaries, can indicate that the body is working overtime to expel waste through the skin. This differs from typical hormonal acne, which presents as deep, cystic lesions along the jawline. Constipation-related skin issues tend to be more diffuse: widespread congestion, small bumps, uneven texture, and a lack of radiance rather than a few isolated deep pimples. Under-eye circles and puffiness also correlate with constipation, though the mechanism is slightly different. Fluid retention increases when the lymphatic system is sluggish, and the lymphatic system often becomes sluggish when the gut is not moving. The thin skin under the eyes shows this fluid accumulation more obviously than anywhere else on the face, creating dark circles that no eye cream can fully address because the problem is not topical.

What Actually Fixes Constipation-Related Skin Issues From the Inside Out
The most effective approach addresses both the constipation and the skin simultaneously, but the priority should be resolving the constipation first. Increasing dietary fiber to 25 to 30 grams per day from whole food sources like vegetables, legumes, and ground flaxseed tends to produce noticeable skin improvements within two to four weeks. Magnesium citrate, taken at 200 to 400 milligrams before bed, serves double duty as both an osmotic laxative and a mineral that supports skin barrier function. Hydration matters, but the often-repeated advice to drink eight glasses of water per day is somewhat arbitrary. A better gauge is urine color: pale yellow means adequate hydration. The tradeoff with fiber is that increasing it too quickly can temporarily worsen both bloating and skin breakouts.
When you suddenly feed gut bacteria a large amount of fiber they are not accustomed to, fermentation increases before the microbiome adapts, producing gas, discomfort, and sometimes a brief purge of toxins through the skin. This is why some people try a high-fiber diet, break out worse in week one, and abandon the approach before it has time to work. Increasing fiber by about 5 grams per week and pairing it with adequate water minimizes this transition period. Probiotics can help, but the strain matters. Lactobacillus rhamnosus GG and Bifidobacterium longum have the most evidence supporting both gut motility and skin health benefits. Generic store-brand probiotics that do not specify strains or colony-forming unit counts are largely a gamble. Fermented foods like sauerkraut, kimchi, and plain kefir provide a broader spectrum of beneficial bacteria and tend to be more cost-effective than supplements, though they will not help if you have a histamine sensitivity, which can itself cause skin flushing and hives.
When Constipation and Skin Problems Signal Something More Serious
Chronic constipation that does not respond to dietary changes, adequate hydration, and movement may indicate an underlying condition that needs medical evaluation. Hypothyroidism is one of the most common culprits: it slows gut motility and simultaneously causes dry, dull, acne-prone skin. If you are constipated, breaking out, losing hair, and feeling fatigued, ask your doctor for a full thyroid panel, not just TSH but also free T3, free T4, and thyroid antibodies. Small intestinal bacterial overgrowth, known as SIBO, is another condition where constipation and skin issues overlap significantly. The methane-dominant form of SIBO specifically slows transit time in the colon, and the bacterial overgrowth produces endotoxins that fuel skin inflammation.
SIBO requires a breath test for diagnosis and targeted antimicrobial treatment, not just probiotics. In fact, taking probiotics when you have SIBO can sometimes make symptoms worse, which is a limitation that the wellness industry rarely mentions. Hormonal imbalances, particularly elevated androgens in conditions like polycystic ovary syndrome, can cause both sluggish digestion and cystic acne. The relationship becomes circular: constipation impairs estrogen metabolism through the estrobolome, the collection of gut bacteria that process estrogen, leading to further hormonal imbalance, which worsens both the constipation and the acne. Breaking this cycle often requires addressing the hormonal component medically rather than relying solely on lifestyle changes.

The Role of Stress in Connecting Your Gut and Your Skin
Stress deserves its own discussion because it acts as a bridge between constipation and skin problems. Cortisol, the primary stress hormone, simultaneously slows gut motility, increases intestinal permeability, stimulates sebaceous glands, and triggers inflammatory pathways in the skin. A graduate student I spoke with described a pattern where every exam period brought constipation, followed by a predictable breakout along her forehead and chin about five days later.
Once exams ended and her stress dropped, her bowels normalized and her skin cleared within a week, without any change in diet or skincare routine. This is why stress management is not a throwaway recommendation. Practices that activate the parasympathetic nervous system, such as diaphragmatic breathing, regular moderate exercise, and consistent sleep schedules, directly improve gut motility through the vagus nerve while simultaneously reducing cortisol-driven skin inflammation. It is one intervention that treats both ends of the gut-skin axis at once.
Rethinking Your Skincare Routine When the Problem Is Internal
The skincare industry is built on the premise that skin problems have topical solutions. That framework works for many conditions, but when constipation is a contributing factor, the most expensive serums in the world will only partially mask the issue. The future of dermatology is increasingly moving toward integrative approaches that consider GI health as part of skin treatment.
Several dermatology practices now routinely screen for digestive complaints during acne consultations, and research into postbiotics, metabolites produced by beneficial gut bacteria applied topically, is showing early promise for treating inflammatory skin conditions from the outside in while the gut is addressed from the inside out. If you have been cycling through skincare products without lasting improvement in your skin clarity, it may be time to look further down. Not at the next serum launch, but at what is happening in your gut. The face often reveals what the body cannot hide, and constipation is one of those things your skin will announce long before you connect the dots.
Conclusion
Constipation affects your face through multiple overlapping mechanisms: endotoxin recirculation, liver burden, microbiome disruption, hormonal imbalance, and chronic low-grade inflammation. The visible signs include dull complexion, forehead and jawline breakouts, under-eye puffiness, and rough skin texture that does not respond well to topical treatments alone. Understanding these connections reframes acne and skin dullness not just as surface-level problems but as potential signals from your digestive system.
The practical path forward starts with the basics: adequate fiber from whole foods, sufficient hydration, magnesium supplementation, strain-specific probiotics or fermented foods, stress management, and regular movement. If those interventions do not resolve both the constipation and the skin issues within six to eight weeks, seek evaluation for thyroid dysfunction, SIBO, or hormonal imbalances. Your skin is not lying to you. It is telling you what your gut already knows.
Frequently Asked Questions
How quickly will my skin clear up after I resolve constipation?
Most people notice reduced dullness and fewer new breakouts within two to four weeks of regular bowel movements. However, existing acne lesions and post-inflammatory hyperpigmentation can take six to twelve weeks to fully resolve, so patience is necessary even after digestion normalizes.
Can laxatives help clear my skin?
Stimulant laxatives like senna or bisacodyl may temporarily relieve constipation but do not address the underlying microbiome or motility issues, and chronic use can actually damage the enteric nervous system, worsening constipation long-term. Osmotic options like magnesium citrate are gentler and more sustainable, but laxatives should not be your sole strategy.
Is there a specific diet that helps both constipation and acne?
A diet rich in vegetables, legumes, whole grains, and fermented foods while low in processed sugar and dairy tends to benefit both conditions. That said, dairy sensitivity varies by individual, and whole grains can be problematic for people with SIBO, so there is no universal diet that works for everyone.
Does drinking more water alone fix constipation-related skin issues?
Increasing water intake helps if you are genuinely dehydrated, but if you are already drinking adequate fluids, adding more water without increasing fiber will not meaningfully change stool transit time or skin appearance. Fiber and water work together, and one without the other is insufficient.
Can topical probiotics help with gut-related acne?
Topical probiotics and postbiotics show some promise for calming surface-level inflammation and supporting the skin barrier, but they do not address the root cause if your acne is driven by internal gut dysfunction. Think of them as a helpful complement, not a replacement, for fixing the digestive issue itself.
You Might Also Like
- What SIBO Has to Do with Skin Breakouts
- Why Your Gut Health Directly Affects Your Acne
- What Is the Gut-Skin Axis and Why It Matters for Acne
Browse more: Acne | Acne Scars | Adults | Back | Blackheads