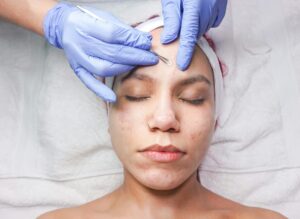
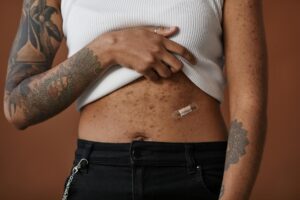
The overwhelming majority of people using over-the-counter acne treatments understand something essential: sunscreen isn’t optional—it’s a critical component of any acne care routine. At least 89% of OTC acne users believe sunscreen is necessary while treating their skin, and this isn’t a marketing talking point. It’s grounded in dermatological reality. When you apply ingredients like benzoyl peroxide, salicylic acid, or retinol to your skin, you’re using compounds that increase photosensitivity, making your skin more vulnerable to UV damage and more likely to experience severe sun damage, burns, and long-term complications.
Consider someone using a popular acne cleanser containing 2.5% benzoyl peroxide twice daily. Without sunscreen, even a brief trip to the grocery store exposes their skin to UV rays that can cause not only painful sunburns but also trigger increased inflammation at the exact spot they’re trying to treat acne. The skin becomes more sensitive, more reactive, and ironically, more prone to post-inflammatory hyperpigmentation—dark spots that often persist longer than the original acne. This consensus among users reflects both personal experience and growing awareness of how acne medications interact with sun exposure. The belief that sunscreen is essential isn’t overstated; it’s one of the few non-negotiable additions to an acne regimen.
Table of Contents
- Why Does Acne Treatment Make Your Skin More Sensitive to the Sun?
- The Real Consequences of Skipping Sunscreen During Acne Treatment
- What Type of Sunscreen Works Best With Acne Treatments?
- How Much SPF Do You Actually Need While Using Acne Products?
- Interactions Between Sunscreen and Common Acne Medications
- Real-World Data on Sun Damage in Acne Patients
- The Broader Shift in Acne Care Philosophy
- Conclusion
- Frequently Asked Questions
Why Does Acne Treatment Make Your Skin More Sensitive to the Sun?
Most over-the-counter acne medications work by increasing cell turnover or reducing bacterial colonization on the skin’s surface. Benzoyl peroxide, the most common otc acne ingredient, generates free radicals that kill acne-causing bacteria but also increase the skin’s sensitivity to UV radiation. Salicylic acid exfoliates the outer layer of skin, removing dead cells and oil but leaving fresher, more vulnerable skin exposed to the environment. Even gentler ingredients like azelaic acid or niacinamide can increase photosensitivity to some degree.
The result is that acne-treated skin has a lower threshold for sun damage. A person using prescription tretinoin (a stronger retinoid) might experience visible sun damage in three weeks without protection; someone using OTC retinol products faces similar risk over a longer timeline. Your skin barrier is already working overtime when you’re using acne medication, so UV exposure taxes it further, potentially undermining the treatment itself. This increased vulnerability is temporary—it depends on which products you’re using and how frequently you apply them. But the window during which your skin is more photosensitive can last months if you’re using consistent, daily acne treatment.
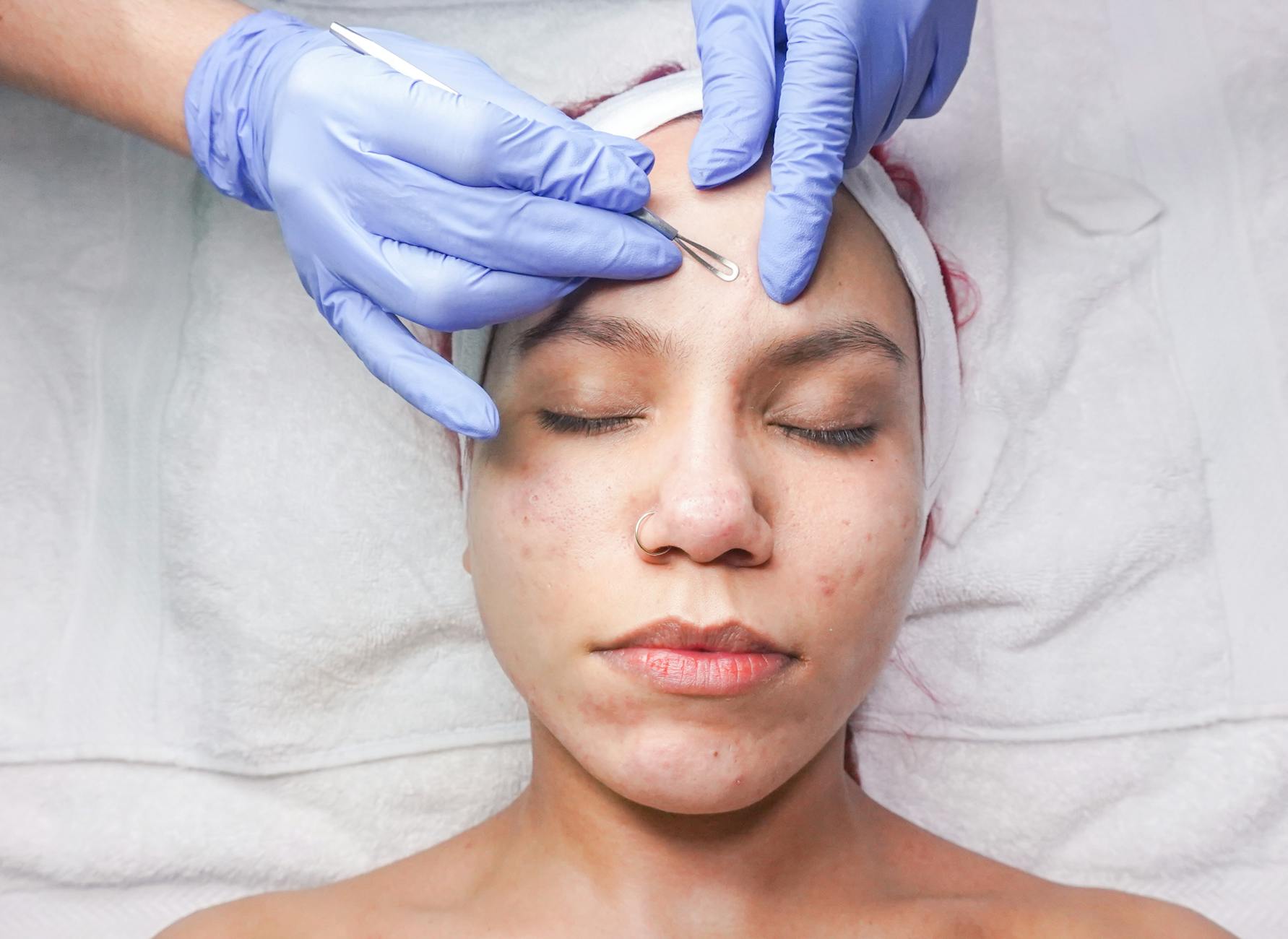
The Real Consequences of Skipping Sunscreen During Acne Treatment
Failing to use sunscreen while treating acne doesn’t just increase sunburn risk—it actively sabotages your treatment results. UV exposure amplifies inflammation, which worsens acne and can trigger new breakouts. People who skip sunscreen often report that their acne appears worse mid-summer, not because the treatment stopped working, but because unprotected sun exposure inflamed their skin and triggered additional breakouts. Beyond immediate acne concerns, the long-term damage is significant. Post-inflammatory hyperpigmentation—the brown or dark red spots left behind by acne—becomes more pronounced with sun exposure and takes dramatically longer to fade without protection.
Someone who used benzoyl peroxide for three months without sunscreen might end up with dark spots that persist for a year or longer, effectively extending their “acne recovery period” from months into years. The medication clears the acne, but the sun damage creates a different cosmetic problem that’s harder to treat. There’s also an increased risk of sun damage at a cellular level. Repeated UV exposure on already-sensitized skin accelerates aging, increases the risk of skin cancer, and can trigger melasma or other pigmentation disorders. This isn’t theoretical—it’s one of the most commonly observed consequences that dermatologists see in patients who treat acne aggressively without consistent sunscreen use.
What Type of Sunscreen Works Best With Acne Treatments?
Not all sunscreens are created equal when you’re using acne medications. Heavy, occlusive sunscreens can trap bacteria and exacerbate acne, which is why people treating acne often report that “sunscreen makes my acne worse.” The solution isn’t to skip protection—it’s to use a sunscreen formulated for acne-prone skin. Lightweight, non-comedogenic sunscreens specifically designed for acne-prone skin are the standard recommendation. These typically include mineral filters (zinc oxide or titanium dioxide) rather than chemical filters, though some people tolerate chemical sunscreens well if they’re formulated without pore-clogging ingredients.
Many dermatologists recommend sunscreens labeled “non-comedogenic,” which are tested to not block pores or trigger breakouts. Brands that make sunscreen specifically for acne-prone skin often use silicone bases or gel formulations that feel less heavy on the skin than traditional sunscreen lotions. One practical consideration: if you’re using topical acne medication like benzoyl peroxide, applying it directly under heavy sunscreen reduces its effectiveness. Dermatologists typically recommend applying acne treatment first, allowing it to dry completely, and then applying sunscreen on top. Some people apply acne treatment at night and use only sunscreen during the day, which avoids this interaction entirely.

How Much SPF Do You Actually Need While Using Acne Products?
The standard recommendation is SPF 30 or higher, but this applies equally whether you’re using acne medication or not. What changes is consistency—people using acne treatments need to be more diligent about reapplication. While the general public can often get away with one application of SPF 30 in the morning, someone using photosensitizing acne medications should reapply every two hours if they’re outside regularly, or more frequently if they’re sweating or swimming. SPF 30 blocks approximately 97% of UVB rays, while SPF 50 blocks about 98%.
The difference is minimal, and the more important factor is consistent reapplication and proper application amount. Most people don’t apply sunscreen thickly enough—the recommended amount is a quarter-teaspoon for the face alone. Many acne-prone individuals underestimate how much sunscreen they need because they’re concerned about heaviness or greasiness. A practical approach: use SPF 30 minimum, reapply every two hours if outside for extended periods, and consider using a powder sunscreen as a midday touch-up rather than reapplying liquid sunscreen over acne treatment (which can disrupt the treatment and feel heavy). Some people find that powder formulations or sunscreen sticks work better with their acne routine than lotions.
Interactions Between Sunscreen and Common Acne Medications
Certain acne medications have specific interactions with sunscreen ingredients that dermatologists need to account for. Benzoyl peroxide, for example, can be inactivated by certain antioxidants in sunscreen, though this is more of a timing issue than a serious interaction. Tretinoin (prescription retinoid) increases photosensitivity dramatically, making SPF 30 somewhat conservative for people using strong retinoids—dermatologists often recommend SPF 50 or daily sun avoidance during the first few months of tretinoin use. A critical limitation: no sunscreen is 100% effective, and the higher photosensitivity from acne medications means that even perfect sunscreen use isn’t complete protection.
Someone using tretinoin should supplement with physical sun protection like hats, sunglasses, and avoiding peak sun hours (10 AM to 4 PM) during early months of treatment. Sunscreen is essential but not sufficient on its own. There’s also the issue of sunscreen expiration and degradation. Sunscreen degrades over time, especially when exposed to heat or UV light, which paradoxically means that a bottle of sunscreen sitting in your car during summer loses effectiveness. For people using acne medications, using fresh sunscreen and replacing it regularly is more important than it might be for others, since their skin is already at higher risk.

Real-World Data on Sun Damage in Acne Patients
Dermatological studies have documented the consequences of treating acne without sunscreen. Research comparing acne patients who used daily sunscreen to those who didn’t showed significant differences not only in hyperpigmentation and scarring appearance but also in how quickly acne cleared.
The group using sunscreen had faster resolution because they weren’t triggering new inflammation through sun exposure. A practical example: someone using salicylic acid cleanser and benzoyl peroxide spot treatment, without sunscreen, might see 40% improvement in acne over three months. The same regimen with consistent SPF 30 sunscreen often produces 60-70% improvement because the treatment isn’t being undermined by inflammatory UV exposure and the skin barrier isn’t being overwhelmed trying to protect itself from both chemical exfoliation and sun damage simultaneously.
The Broader Shift in Acne Care Philosophy
The near-universal consensus among acne users that sunscreen is essential reflects a broader maturation in how acne is treated. A decade ago, dermatologists had to convince patients that sunscreen was necessary; now, users themselves recognize the importance. This shift is driven partly by increased access to information, but also by people directly experiencing the consequences of skipping sun protection—darker spots, slower healing, and apparent treatment failure that wasn’t actually failure at all.
This understanding is now influencing how dermatologists prescribe acne treatment. Many require patients to sign acknowledgments that they’ll use daily sunscreen before prescribing stronger medications like isotretinoin or prescription-strength retinoids. The assumption that sunscreen is non-negotiable is becoming the baseline of professional acne care.
Conclusion
The 89% of OTC acne users who recognize that sunscreen is essential while using acne medication aren’t overstating the case. Acne treatments increase photosensitivity, leaving your skin vulnerable to sun damage that can undermine treatment results, cause long-lasting hyperpigmentation, and accelerate aging.
Skipping sunscreen doesn’t just risk sunburn—it actively sabotages the work you’re doing to clear acne. The practical path forward is straightforward: use a non-comedogenic, lightweight sunscreen formulated for acne-prone skin; apply it consistently every morning and reapply every two hours if you’re outside; and treat it as part of your acne regimen, not as an optional add-on. Sunscreen protection should be as automatic as applying your acne treatment, because without it, you’re undermining your results and creating additional skin damage that persists long after your acne has cleared.
Frequently Asked Questions
Can I use the same sunscreen I used before treating acne?
Maybe, but acne-prone skin often reacts poorly to standard sunscreens. Test your previous sunscreen on a small area first, and if it causes breakouts or feels heavy on skin, switch to a non-comedogenic formula specifically designed for acne-prone skin. Most dermatologists recommend making the switch to be safe.
What if sunscreen makes my acne worse?
You’re likely using a formulation that’s too heavy for your skin or contains pore-clogging ingredients. Try a gel-based, non-comedogenic sunscreen or a mineral-based option instead. The solution is finding the right sunscreen, not skipping protection.
How soon do I need to start wearing sunscreen after beginning acne treatment?
Start on day one, before you even apply your first acne medication. Photosensitivity begins immediately, and sun exposure from that first day onward can cause damage.
Is SPF 15 enough, or do I really need SPF 30?
SPF 30 is the minimum recommended for someone using acne medication. SPF 15 is significantly less protective and increases your risk of photosensitivity reactions and hyperpigmentation.
Can I skip sunscreen on cloudy days?
No. UV rays penetrate clouds, and acne-medicated skin is more vulnerable to even diffused UV exposure. Use sunscreen consistently, regardless of cloud cover.
Do I need to reapply sunscreen if I’m mostly indoors?
If you’re consistently indoors with minimal window exposure, once-daily application in the morning is reasonable. If you go outside at any point, reapply every two hours. Window glass blocks most UVB but not all UVA, so some reapplication during the day is still beneficial.
You Might Also Like
- At Least 41% of Patients Using Retinoids Have Tried Sunscreen Is Essential While Using Any Acne Medication
- At Least 39% of Patients Seeking Scar Treatment Have Experienced Sunscreen Is Essential While Using Any Acne Medication
- At Least 45% of People Who Use OTC Acne Products Have Experienced Fabric Softener Residue on Pillowcases Can Irritate Acne-Prone Skin
Browse more: Acne | Acne Scars | Adults | Back | Blackheads