The future of hormonal acne treatment is moving toward more targeted, effective options that reduce the systemic side effects associated with traditional therapies. The next generation includes topical antiandrogens like clascoterone that work directly on skin without affecting reproductive hormones, laser technologies that selectively disable sebaceous glands, and oral medications in development that approach the problem through new biochemical pathways.
If you’ve struggled with hormonal acne or worry about the side effects of birth control pills and spironolactone, the treatment landscape over the next 2-3 years will offer meaningful alternatives that address the underlying hormonal drivers without the trade-offs of current options. This article covers the most promising innovations reaching patients soon, how current hormonal therapies are being refined based on new clinical evidence, the emerging role of microbiome-targeted treatments, and personalized approaches that combine inside-and-out strategies. Whether you’re considering hormonal acne treatment for the first time or looking for alternatives to what you’re using now, understanding these developments will help you have more informed conversations with your dermatologist.
Table of Contents
- What New Topical Antiandrogens Mean for Hormonal Acne Treatment
- How Laser Technology Is Changing the Approach to Sebum Control
- Oral Treatments Reshaping How Dermatologists Approach Severe Acne
- How Current Hormonal Therapies Are Being Refined with New Evidence
- Microbiome-Directed Therapies and Postbiotics Enter the Treatment Arsenal
- AI-Personalized Skincare and Individualized Treatment Planning
- What the Convergence of These Advances Means for Future Acne Patients
- Conclusion
What New Topical Antiandrogens Mean for Hormonal Acne Treatment
For decades, treating hormonal acne meant choosing between oral medications that affect your whole body or topical treatments that didn’t target the hormone-driven root cause. Clascoterone 1% cream breaks that pattern. It’s the first FDA-approved topical antiandrogen specifically for acne, and it works by blocking androgen receptors directly on skin cells without significant systemic absorption. This matters because traditional hormonal therapies like spironolactone and birth control pills suppress hormones throughout your body, which can affect menstrual cycles, mood, and breast tenderness in some users. Clascoterone delivers targeted hormone blocking where acne actually forms.
Another breakthrough is DMT310 (marketed as Xyngari), which recently completed Phase 3 trials and represents a different innovation: it’s the first once-weekly topical acne treatment to demonstrate clinical benefit in Phase 3 testing. The convenience of once-weekly application compared to daily creams changes the treatment experience significantly. Both medications represent a shift toward acne therapies that work like precision tools rather than systemic interventions, though neither has the decade-long safety data that retinoids and birth control pills carry at this point. The limitation worth understanding: topical antiandrogens excel for moderate hormonal acne driven by local androgen sensitivity, but they won’t help patients whose acne stems from high circulating testosterone levels or significant sebum overproduction. For severe hormonal acne with widespread cystic lesions, a dermatologist may still recommend pairing a topical antiandrogen with an oral option to address both the local skin environment and systemic hormone levels.

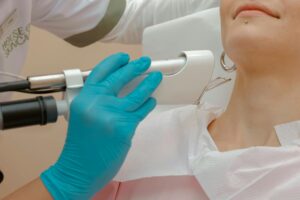
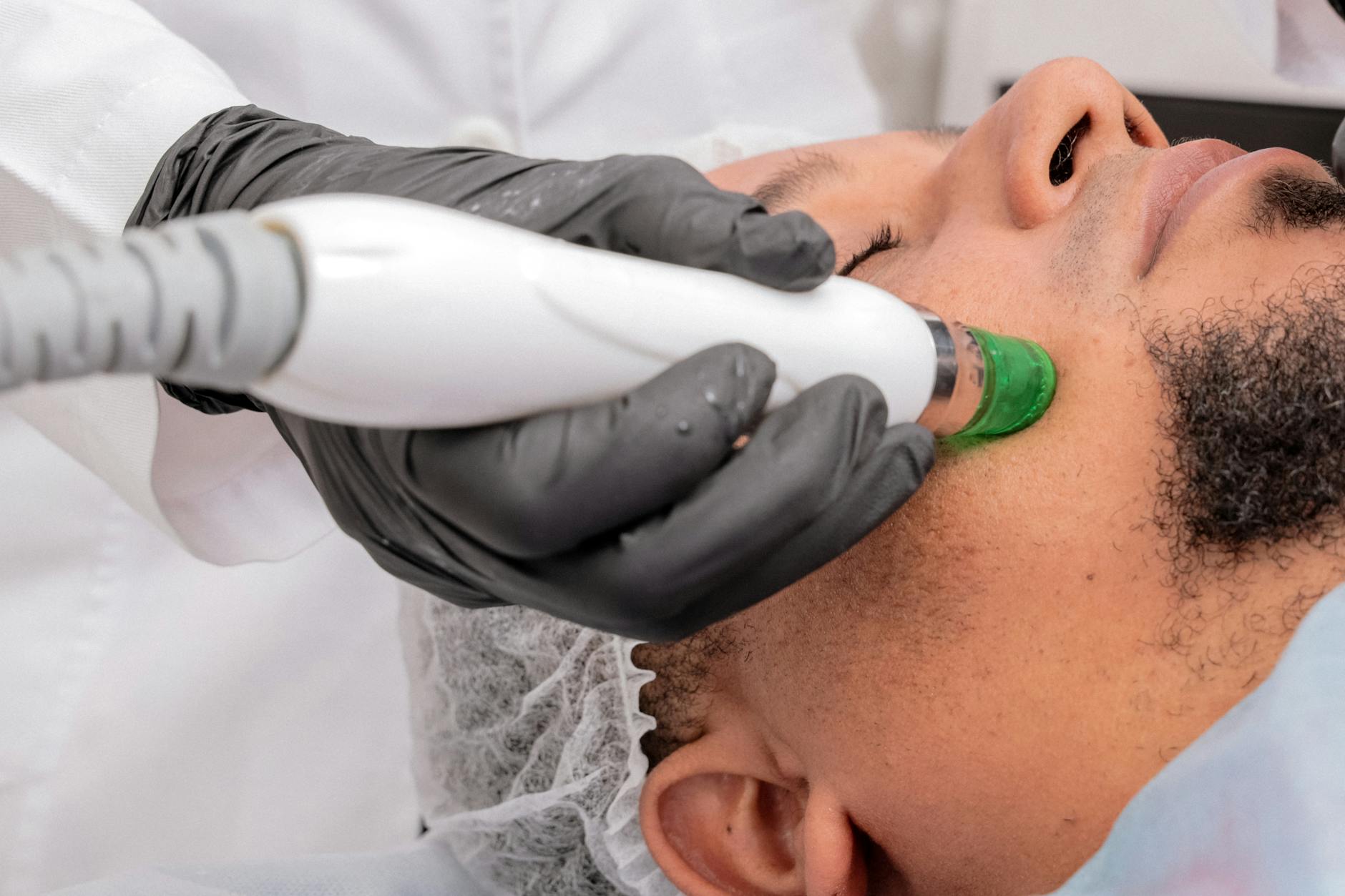
How Laser Technology Is Changing the Approach to Sebum Control
One of the most significant shifts in acne treatment is the rise of 1726 nm laser technology, represented by devices like AviClear and Accure. These lasers work on a fundamentally different principle than topical or oral treatments. Instead of modulating hormones or bacteria, they directly target the sebaceous glands themselves, using selective heating to reduce sebum production without damaging surrounding skin tissue. Because excess sebum production is a hallmark of hormone-driven acne, this technology bypasses the hormonal system entirely and addresses the mechanical problem that fuels acne formation. The clinical significance is substantial: sebaceous glands are the source, bacteria are the problem, and hormones drive the glands.
By reducing gland activity through laser treatment, you reduce the fuel supply for acne bacteria while keeping hormones unchanged. This appeals to patients who want to avoid hormonal medication altogether or who have contraindications to spironolactone or oral contraceptives. Multiple laser treatments are typically required (usually 3 sessions spaced weeks apart), and results take several weeks to fully manifest as sebum production gradually decreases. However, laser treatment is a longer-term investment than starting a topical or oral medication, and it’s not covered by most insurance plans, making it significantly more expensive than prescriptions. Additionally, for hormonal acne patients with irregular cycles, hormonal sensitivity in other body areas, or other signs of elevated androgens, laser treatment addresses only one piece of the puzzle. Someone with hormonal acne rooted in underlying PCOS or hormonal imbalance would likely benefit from combining laser treatment with hormonal management rather than relying solely on the laser.
Oral Treatments Reshaping How Dermatologists Approach Severe Acne
While birth control pills and spironolactone have dominated hormonal acne treatment, a new class of oral medications is in advanced development. Denifanstat (ASC40), developed by Ascletis Pharma, recently completed Phase III trials for moderate to severe acne vulgaris. It works as a farnesyltransferase inhibitor, a mechanism that reduces sebum production and inflammation simultaneously by blocking a specific cellular pathway involved in both processes. This is notably different from the androgen-blocking approach of spironolactone or the estrogen-dominance strategy of birth control, offering a distinct biological target for patients who haven’t responded adequately to hormonal therapies. More experimental but potentially transformative is the mRNA acne vaccine in development by Sanofi, which takes a completely different approach by training the immune system to modulate the inflammatory response to acne bacteria.
Clinical trials are expected to yield results by 2029, so this remains years away from potential availability. If successful, it represents a paradigm shift from managing acne symptoms to preventing the inflammatory cascade that turns bacterial colonization into visible breakouts. The reality check: denifanstat and the mRNA vaccine are not yet available to patients, and the earlier drugs reach the market doesn’t guarantee they’ll work for your acne. Acne is heterogeneous—hormonal acne in one person is driven by excess androgens, in another by androgen sensitivity, and in a third by inflammatory response patterns. A new oral medication that works brilliantly for some patients may be ineffective for others, and dermatologists will need time and clinical experience to predict who benefits from each option.
How Current Hormonal Therapies Are Being Refined with New Evidence
While new treatments get attention, current hormonal therapies are being sharpened by recent clinical research. Spironolactone, a diuretic that blocks androgen receptors, remains effective at 50-100 mg daily for acne in women. Recent prospective cohort research showed that 74% of women with severe acne achieved at least 75% reduction in lesions when spironolactone was combined with a drospirenone/ethinyl estradiol oral contraceptive. Importantly, none of the participants developed hyperkalemia (dangerously high potassium), which is the primary safety concern driving caution around spironolactone use. Updated 2024 American Academy of Dermatology guidelines reflect this safety data: potassium monitoring is no longer considered necessary for healthy patients starting spironolactone, though it should be considered for individuals with risk factors for hyperkalemia (like kidney disease or certain medications).
This represents a meaningful shift that makes spironolactone more straightforward to access for appropriate patients. The three FDA-approved oral contraceptives specifically for acne—Ortho-Tri-Cyclen, Estrostep FE, and Yaz—continue to be refined formulations with better tolerability, and combination therapy pairing one of these with spironolactone represents a proven, well-understood option that works for many patients. The tradeoff to understand: spironolactone and oral contraceptives are effective and have decades of safety data, which makes them less risky than new medications still in trials. But they do alter systemic hormones and carry side effects some women find unacceptable—breakthrough bleeding, mood changes, or changes in breast tenderness. Someone seeking to avoid hormonal medication entirely would need to choose a laser-based approach or wait for the topical antiandrogens and oral medications currently in development to offer sufficient evidence of their own long-term safety profile.
Microbiome-Directed Therapies and Postbiotics Enter the Treatment Arsenal
Beyond hormones and sebaceous glands, the microbiome emerging as an acne driver has opened a third avenue for treatment innovation. Microbiome-directed therapies—including probiotics, postbiotics, and even bacteriophages—are being explored to restore bacterial balance and reduce acne-promoting strains on skin. This acknowledges that hormonal imbalance creates an environment where problematic bacteria proliferate, but that reducing the bacterial load is still essential to preventing breakouts. Postbiotics, which are metabolites produced by beneficial bacteria, are receiving attention as a less unstable alternative to live probiotics. These compounds can modulate skin inflammation and support the skin barrier without the storage and viability challenges of probiotic products.
By 2026, dermatologists increasingly recommend combining inside-out approaches—oral probiotics or supplements that support the skin microbiome—with topical treatments that directly manage hormonal drivers and bacterial load. One emerging supplement gaining traction is DIM (diindolylmethane), derived from cruciferous vegetables like broccoli and cabbage. DIM supports healthy estrogen metabolism, helping the body process and eliminate estrogen more efficiently and favor metabolites associated with clearer skin. When used alongside other hormonal acne treatments, DIM may offer modest additional benefit, though the evidence is not yet as robust as it is for spironolactone or birth control. However, for patients who want to try a natural intervention before moving to prescription medications, DIM is a lower-risk starting point worth discussing with a dermatologist.

AI-Personalized Skincare and Individualized Treatment Planning
One of the 2026 acne treatment trends that few people discuss is the role of AI in personalizing skincare regimens and predicting treatment response. Rather than a one-size-fits-all recommendation to use a benzoyl peroxide wash and a retinol serum, dermatologists are increasingly using AI tools to analyze skin microbiome profiles, hormonal labs, and individual response patterns to predict which combination of treatments will work best for that specific patient.
This trend reflects a broader shift toward inside-out acne treatment that combines dermatological therapy with targeted supplements and skincare ingredients chosen for individual microbiome and inflammatory profiles. Retinol systems with reduced irritation—microencapsulated and time-release formulations—are being designed to work alongside hormonal treatments without the excessive dryness that previously made combining retinoids with spironolactone challenging. This represents a maturation of acne treatment from prescribing the same combination to everyone toward truly personalized regimens.
What the Convergence of These Advances Means for Future Acne Patients
Looking ahead to 2027 and beyond, hormonal acne treatment is moving toward a menu of options rather than a one-standard choice. Patients with mild hormonal acne might start with topical antiandrogens and microbiome-supportive products. Those with moderate to severe acne would have choices: combination oral therapy with spironolactone and birth control, or laser-based sebaceous gland reduction, or clinical trial access to denifanstat.
Those unable or unwilling to use systemic hormonal therapy have new topical and laser alternatives that were unavailable five years ago. The bigger picture is that understanding the root mechanism of your acne—whether it’s driven by androgens, androgen sensitivity, excess sebum, inflammatory response, or microbiome imbalance—will become increasingly central to treatment decisions. This requires better diagnostic tools and dermatologist assessment, but it means your treatment can be chosen strategically rather than prescribed by default. The future of hormonal acne treatment is not a single breakthrough drug but a expanding toolkit matched to individual biology.
Conclusion
The next wave of hormonal acne treatment brings real advances: topical antiandrogens that work without systemic effects, lasers that reduce sebaceous gland activity, oral medications with new mechanisms of action, and refined combinations of proven therapies with better safety data. For patients frustrated with current options, this expansion means more pathways to clear skin without unacceptable side effects.
If you’re considering hormonal acne treatment, the practical path forward is understanding your own acne drivers through a dermatologist’s assessment, then choosing from the growing menu of options—traditional hormonal therapy, new topical options, laser approaches, or emerging microbiome-directed strategies. The future of treating hormonal acne lies not in waiting for a perfect cure but in having real choices tailored to your body, your preferences, and your underlying acne mechanism.
You Might Also Like
- Why Acne Scar Treatment Will Look Very Different in 2035
- What i-PRF vs L-PRF Means for Acne Scar Treatment Protocols
- Why NAD+ Supplements Are Being Marketed for Acne — What We Know
Browse more: Acne | Acne Scars | Adults | Back | Blackheads