Anticoagulants increase bruising during acne scar subcision because they thin your blood and prevent it from clotting normally, leading to prolonged bleeding and larger bruises at the treatment site. During subcision—a procedure where a dermatologist uses a needle to deliberately break apart scar tissue beneath the skin’s surface—any medication that reduces clotting will allow blood to accumulate longer in the small tissue pockets created by the technique. If you’re taking warfarin, apixaban, rivaroxaban, or even aspirin regularly, your bruising response will be notably more severe and take longer to fade compared to patients not on anticoagulants. This article explains the mechanism behind this effect, how different anticoagulants impact bruising severity, what you should do before your procedure, and how to manage recovery expectations.
Table of Contents
- How Anticoagulants Prevent Normal Clotting During Acne Scar Treatment
- Direct Anticoagulants Versus Antiplatelet Agents: Different Effects on Bruising Severity
- Common Anticoagulant Medications and Their Bruising Profiles During Cosmetic Procedures
- Pre-Procedure Medication Management and Risk Reduction Strategies
- Bruising Severity and Managing Expectations During Recovery
- Baseline Bleeding Disorder Complications and When Anticoagulants Create Additional Risk
- Alternative Procedures and Future Directions in Anticoagulant-Friendly Scar Treatment
- Conclusion
- Frequently Asked Questions
How Anticoagulants Prevent Normal Clotting During Acne Scar Treatment
Anticoagulants work by inhibiting one or more steps in your body’s blood clotting cascade—either by blocking vitamin K-dependent clotting factors (warfarin), directly inhibiting factor Xa (apixaban, rivaroxaban), or inhibiting thrombin (dabigatran). When your dermatologist performs subcision, they intentionally create multiple small puncture wounds and separate the scar tissue from underlying tissue planes. Without anticoagulants, a blood clot forms within minutes to seal these micro-injuries.
With anticoagulants active in your bloodstream, this clotting process is delayed or incomplete, allowing blood to continue seeping into the tissue space and the dermis, creating larger and more visible bruises. The difference is measurable: patients on anticoagulants typically experience bruising that extends further from the treatment site and persists for 2-3 weeks, compared to 1-2 weeks for non-anticoagulated patients. For example, a patient on apixaban may develop a bruise covering 3-4 square inches after subcision, while the same procedure on someone not taking anticoagulants might result in a bruise covering 1-2 square inches. This isn’t a failure of the procedure—it’s a predictable pharmacological consequence.
Direct Anticoagulants Versus Antiplatelet Agents: Different Effects on Bruising Severity
It’s important to distinguish between anticoagulants (which affect clotting factors) and antiplatelet agents like aspirin (which affect platelet function). Anticoagulants like warfarin and DOACs (direct oral anticoagulants: apixaban, rivaroxaban, dabigatran, edoxaban) have a more dramatic effect on bruising than aspirin because they target the coagulation cascade itself rather than just platelet aggregation. However, this doesn’t mean aspirin has no effect—patients on aspirin still experience measurably worse bruising than unmedicated controls, just not as severely as those on full anticoagulants.
A limitation here is that bruising severity varies significantly based on individual factors: age, skin thickness, the specific dermatologist’s technique, the depth and number of subcision passes, and baseline bleeding tendency. A 65-year-old on warfarin may bruise more heavily than a 35-year-old on apixaban, even though warfarin is the “stronger” anticoagulant. Additionally, if you’ve been on an anticoagulant for months, your body may show less bruising than if you’ve just started the medication, suggesting some degree of physiological adaptation, though this is not well-studied in cosmetic dermatology literature.
Common Anticoagulant Medications and Their Bruising Profiles During Cosmetic Procedures
Warfarin (Coumadin) produces the most severe bruising because it blocks multiple vitamin K-dependent clotting factors and has a longer half-life. DOACs like apixaban (Eliquat) and rivaroxaban (Xarelto) produce slightly less dramatic bruising than warfarin but still significantly more than aspirin. Dabigatran (Pradaxa) is a direct thrombin inhibitor and may cause slightly different bruising patterns, though clinical data comparing DOACs head-to-head for cosmetic procedures is limited.
Real-world example: A patient on warfarin with an INR of 2.5-3.0 (therapeutic range) undergoing subcision will typically have bruising that takes 4-6 weeks to fully resolve, with residual purple and yellow discoloration visible for 3 weeks. The same patient on apixaban might see full resolution in 3-4 weeks. For comparison, a patient on aspirin alone may only need 2-3 weeks. If you’re on multiple medications—for instance, aspirin plus clopidogrel (Plavix) for heart disease—your bruising response becomes cumulative and can rival that of warfarin patients.
Pre-Procedure Medication Management and Risk Reduction Strategies
The standard recommendation from dermatologists is to discontinue anticoagulants 5-7 days before subcision if medically safe to do so. For warfarin, this means stopping 5 days before and checking your INR to confirm it has normalized (typically dropping to 1.0-1.2). For DOACs, which have shorter half-lives (12-26 hours depending on the agent), stopping 2-3 days before is usually sufficient. However, if you take anticoagulants for atrial fibrillation, mechanical heart valves, or recent thromboembolism, your cardiologist or primary care physician must approve any interruption—the stroke risk of stopping may outweigh the cosmetic benefit of reduced bruising.
One important caveat: discontinuing anticoagulants carries real medical risk and is not appropriate for everyone. If your anticoagulant cannot be safely stopped, you should proceed with subcision understanding that bruising will be more pronounced. In these cases, discussing alternative procedures with less bleeding risk—like chemical peels, laser resurfacing, or dermal filler augmentation—may be worth considering. Some dermatologists also use topical hemostatic agents like thrombin or tranexamic acid during the procedure to offset anticoagulant effects, though evidence for their effectiveness in this specific application is anecdotal rather than robust.
Bruising Severity and Managing Expectations During Recovery
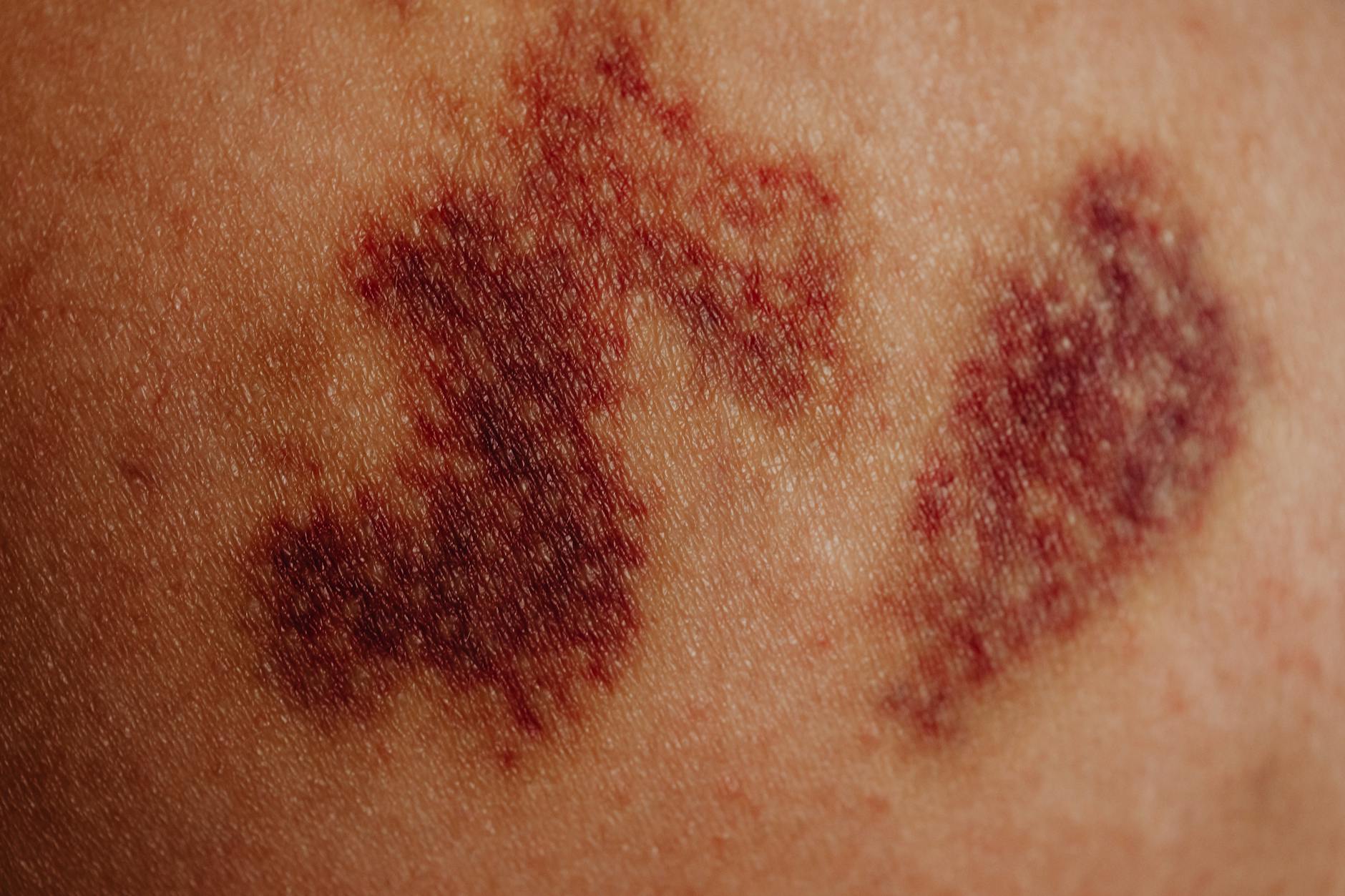
Even with optimized preparation, patients with recent anticoagulant use can expect more extensive bruising than textbook predictions suggest. The bruises typically progress through standard color changes—red to purple within hours, transitioning to blue-purple by day 3, then yellow-green by day 10-14. However, in anticoagulated patients, these stages stretch out longer, and the yellow-green phase may persist into week 4. Some patients also experience more swelling alongside bruising, though swelling typically resolves faster than the discoloration.
A critical limitation is that topical treatments—arnica, vitamin K creams, laser bruise removal—show minimal evidence for accelerating bruise fading in anticoagulated patients. While a non-anticoagulated patient might see meaningful improvement with diligent bruise treatment, someone on warfarin should expect these interventions to provide modest benefit at best. Your best strategy is cold therapy for the first 48 hours (reduces inflammation and may limit initial bruise expansion), compression if tolerated, elevation, and sun avoidance once the acute bruising phase ends. Makeup and corrective concealers become particularly important for coverage during weeks 2-4.
Baseline Bleeding Disorder Complications and When Anticoagulants Create Additional Risk
Patients with hereditary bleeding disorders (hemophilia, von Willebrand disease) who are also on anticoagulants face compounded bruising and bleeding risk. In these rare cases, subcision may not be appropriate without hematology clearance and careful planning.
Similarly, patients taking anticoagulants for thrombophilia (inherited clotting disorders) represent a subset where bleeding risk is particularly high. These patients should undergo hematology consultation before any cosmetic procedure and may be candidates for locoregional anesthesia with epinephrine, which can help minimize bleeding through vasoconstriction.
Alternative Procedures and Future Directions in Anticoagulant-Friendly Scar Treatment
If you cannot safely discontinue anticoagulants and cannot tolerate extensive bruising, several alternatives exist. Laser-based scar revision, particularly fractional CO2 or erbium lasers, causes minimal bleeding compared to subcision and can be effective for shallow atrophic scars. Microneedling with radiofrequency produces collagen remodeling with less bruising than subcision, though results are typically more gradual. Dermal fillers can camouflage scars temporarily.
Combination approaches—such as mild laser resurfacing followed by filler—can sometimes achieve comparable scar improvement with less procedural trauma. Future developments include topical or injectable hemostatic agents specifically designed for cosmetic procedures on anticoagulated patients, though none are yet standard of care. Platelet-rich plasma (PRP) is sometimes added to subcision to theoretically promote faster healing, but its effect on anticoagulant-related bruising remains unclear. As cosmetic dermatology evolves, more anticoagulation-aware procedural protocols will likely emerge.
Conclusion
Anticoagulants increase bruising during acne scar subcision because they impair your body’s ability to form stable blood clots, allowing blood to accumulate longer in the tissue planes created by the procedure. The severity depends on the specific anticoagulant (warfarin typically causes the most bruising, followed by DOACs, then aspirin), your individual physiology, and whether your medication can be safely discontinued before treatment. Planning ahead with your dermatologist and primary care physician—ideally stopping anticoagulants 3-7 days before the procedure if medically safe—significantly reduces bruising severity.
If you cannot or should not stop anticoagulants, you should schedule subcision with realistic expectations: assume 4-6 weeks for full bruise resolution instead of 1-2 weeks, plan for coverage during weeks 2-4, and discuss alternative scar treatments with your dermatologist. The procedure itself remains safe and effective for scar improvement, but the cosmetic recovery timeline lengthens considerably. Always confirm anticoagulant management with your prescribing physician before scheduling any procedure—your medical safety outweighs cosmetic convenience.
Frequently Asked Questions
Can I stay on my anticoagulant and still get subcision?
Yes, but expect significantly more bruising that lasts 4-6 weeks instead of 1-2 weeks. If your anticoagulant is essential for your health (atrial fibrillation, heart valve replacement), do not stop it for a cosmetic procedure. Discuss risk tolerance with your dermatologist.
How long before subcision should I stop aspirin?
Aspirin causes less bruising impact than warfarin or DOACs but still increases it. Stop 5-7 days before if medically safe. If aspirin is for cardiovascular protection, ask your cardiologist before stopping.
Will my bruises fade faster if I use arnica or vitamin K cream?
Evidence suggests minimal benefit, especially in anticoagulated patients. Focus on cold therapy, compression, elevation, and sun protection instead. Makeup is your most reliable coverage tool.
Is subcision safe if I take both aspirin and clopidogrel?
Yes, but dual antiplatelet therapy significantly increases bruising. Plan for extended recovery and discuss with both your cardiologist and dermatologist before proceeding.
Should I use a laser or filler instead of subcision if I’m on anticoagulants?
Fractional laser and filler-based approaches cause minimal bleeding and may be preferable if you cannot stop anticoagulants. However, subcision often produces better long-term scar improvement. Weigh cosmetic goals against recovery tolerance with your dermatologist.
When should I resume anticoagulants after subcision?
Resume the day after the procedure or as directed by your physician. Most dermatologists recommend waiting at least 24 hours to allow initial clot formation and minimize extended oozing, though the procedure itself poses minimal clotting risk.
You Might Also Like
- Why Fluence and Energy Density Affect Acne Scar Treatment Results
- Why TotalFX Combines Both for Comprehensive Acne Scar Treatment
- Why Starlux Fractional Laser Was an Early Acne Scar Option
Browse more: Acne | Acne Scars | Adults | Back | Blackheads





