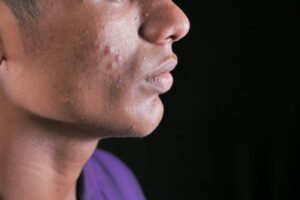
The biggest skincare mistakes people with oily, acne-prone skin make center on one paradox: they treat their skin more aggressively in hopes of fixing it, which actually makes breakouts worse. The most common culprits are over-cleansing and over-exfoliating, which strip the skin barrier and trigger your sebaceous glands to produce even more oil in compensation. Other major mistakes include skipping moisturizer, using comedogenic ingredients, changing treatments too frequently, applying acne medications only to visible blemishes, squeezing pimples, and avoiding sunscreen.
This article covers each of these mistakes in detail and explains why dermatologists say that “trying to do too much” has become the number one skincare error in 2026. If you’re dealing with oily, acne-prone skin, understanding these mistakes is critical because the stakes are high. Acne affects 85% of people aged 12-24, and for adults, the problem persists: up to 15% of adult women experience acne, with 50% of women in their 20s, 33% in their 30s, and 25% in their 40s struggling with breakouts. The good news is that most of these mistakes are completely reversible once you understand what’s happening beneath the surface.
Table of Contents
- Why Over-Cleansing Worsens Oily, Acne-Prone Skin
- The Moisturizer Mistake That Fuels Breakouts
- Comedogenic Ingredients Hiding in Your Products
- The Trap of Changing Treatments Too Frequently
- Applying Treatment Only to Visible Blemishes and Squeezing Pimples
- Avoiding Sunscreen Due to Clogging Concerns
- The 2026 Skincare Reality: Simplicity Beats Complexity
- Conclusion
Why Over-Cleansing Worsens Oily, Acne-Prone Skin
Over-cleansing and over-exfoliating is the fastest way to trap yourself in a vicious cycle. When you strip your skin barrier with harsh cleansers or excessive scrubbing, your sebaceous glands perceive this damage as a sign to produce more protective oil. You’ll feel like your skin is greasier than ever, so you cleanse again—harder and more frequently—which only amplifies the problem. Dermatologists recommend cleansing your face only twice daily with a gentle cleanser, yet many people struggling with acne cleanse three, four, or even five times daily. The damage happens at a microscopic level.
Your skin barrier consists of lipids and proteins that protect underlying layers. When you over-cleanse, you’re essentially removing this protective layer, leaving your skin vulnerable to irritation and bacteria. Your sebaceous glands don’t know you’re trying to fix acne; they only know the barrier is compromised, so they compensate by producing excess sebum. This creates more oiliness, not less—and more food for acne-causing bacteria like *Cutibacterium acnes*. Here’s the counterintuitive part: if you dial back to just two gentle cleansings per day, your skin will likely produce less oil within two to three weeks as your barrier repairs itself. This feels wrong when you’re accustomed to aggressive cleansing, but it’s the dermatologist-recommended standard for good reason.

The Moisturizer Mistake That Fuels Breakouts
Many people with oily skin skip moisturizer entirely, believing it will make breakouts worse. This is one of the most damaging misconceptions. When you don’t moisturize, your skin perceives itself as dehydrated—regardless of how oily the surface appears. In response, your sebaceous glands produce even more oil to compensate, worsening the acne cycle. Conversely, using a proper lightweight, non-comedogenic moisturizer signals to your skin that hydration is being met, reducing the need for excessive oil production. The key distinction is that oily skin and hydrated skin are not the same thing.
You can have oily skin that is actually dehydrated beneath the surface—a condition called “dehydrated oily skin.” When this happens, your skin produces excess sebum while simultaneously feeling tight and uncomfortable. Adding a hydrating moisturizer paradoxically decreases oil production because your sebaceous glands no longer feel the urgency to overproduce. look for moisturizers labeled “non-comedogenic” and formulated for oily or acne-prone skin; these are designed to hydrate without clogging pores. However, if you’ve never used moisturizer and your skin is actively inflamed from active breakouts, you may want to wait until inflammation subsides before introducing a new product. Adding too many new products simultaneously makes it impossible to identify what helps and what triggers breakouts. Start with a single, lightweight moisturizer and give it at least two weeks before evaluating results.
Comedogenic Ingredients Hiding in Your Products
Comedogenic ingredients are substances that are likely to clog pores and trigger breakouts. The most notorious offenders are coconut oil and beef tallow—both are extremely popular in natural and “clean” skincare products but highly comedogenic, meaning they’ll almost certainly make acne worse. If you’re using products marketed as natural or organic without checking the ingredient list, you may unknowingly be applying pore-clogging substances directly to your acne-prone skin. Other common comedogenic ingredients include certain silicones, mineral oil, and lanolin. While some people tolerate these without issue, those with acne-prone skin often experience flare-ups within 48 to 72 hours of using them.
The challenge is that comedogenicity can be individual—what clogs one person’s pores might not affect another. However, for oily, acne-prone skin, it’s safer to avoid known high-risk ingredients altogether rather than experiment and risk triggering a breakout. Reading ingredient labels becomes essential. If you see coconut oil, coconut butter, or beef tallow near the top of the ingredient list, that product is not suitable for acne-prone skin, regardless of marketing claims about naturalness or purity. Instead, prioritize products formulated with non-comedogenic alternatives like jojoba oil, squalane, or glycerin, which hydrate without clogging pores.

The Trap of Changing Treatments Too Frequently
One of the most common mistakes people make is trying a new acne treatment every week or two, hoping to find a quick fix. This constant switching irritates your skin, triggers breakouts, and prevents you from knowing whether a product actually works. Most acne treatments—including benzoyl peroxide, salicylic acid, and prescription retinoids—require at least four to six weeks to show meaningful improvement. Changing treatments weekly means you never give anything time to work, and your skin stays in a constant state of irritation and inflammation. The dermatologist recommendation is straightforward: pick one or two treatments, introduce them gradually into your routine, and commit to them for at least four to six weeks before evaluating results.
For example, if you decide to use a benzoyl peroxide wash, start with it twice daily for two weeks, monitor how your skin responds, then stick with it. If after six weeks you see no improvement, that’s when you consider switching. But jumping between treatments every few days guarantees failure because you’re not allowing your skin’s barrier time to adjust or for the active ingredients to work. Viral skincare trends often encourage people to layer multiple actives—retinoids, vitamin C, benzoyl peroxide, salicylic acid, and more—all at once. This is a recipe for severe irritation, a compromised skin barrier, and paradoxically, worse acne. Dermatologists increasingly warn that “doing too much” has become the biggest skincare mistake in 2026, with people abandoning simple, evidence-based routines in favor of complicated regimens inspired by social media.
Applying Treatment Only to Visible Blemishes and Squeezing Pimples
A critical mistake is applying acne treatments only to visible pimples rather than to all acne-prone areas. Acne isn’t just the inflamed bump you see; it’s a condition affecting your entire face or wherever breakouts occur. When you apply benzoyl peroxide or salicylic acid only to existing blemishes, you’re treating the symptom but missing the prevention opportunity. New pimples form because acne bacteria and clogged pores are already developing beneath the skin surface where you can’t see them. For best results, apply acne treatment to your entire acne-prone area—usually the T-zone for oily skin—not just individual pimples. Squeezing or picking at pimples is another mistake that feels satisfying in the moment but causes serious damage. When you squeeze a pimple, you’re pushing bacteria deeper into the skin, increasing infection risk and triggering a stronger inflammatory response.
You’re also creating tiny wounds that can scar, and for acne-prone skin, scarring is often the lasting consequence of picking. The urge to squeeze is understandable, but dermatologists strongly recommend resisting it. If a pimple has come to a whitehead and you feel you must extract it, only do so after applying a warm compress to soften the area, and use clean tools or a professional extraction at a dermatology office. The psychological component of pimple-squeezing is often overlooked. Many people find it stress-relieving, almost compulsive. If you struggle with this, keep your hands busy with a stress ball or fidget toy, and avoid looking in the mirror under bright lighting where the temptation is strongest. Some people find that covering a pimple with a hydrocolloid bandage (pimple patch) reduces the urge to pick while simultaneously helping the blemish heal faster.

Avoiding Sunscreen Due to Clogging Concerns
Many people with oily, acne-prone skin avoid sunscreen because they believe it will clog pores and worsen breakouts. This is a costly mistake. Without sunscreen protection, the UV damage you accumulate worsens acne scars, makes post-inflammatory hyperpigmentation darker and more visible, and can trigger more inflammation in acne-prone skin. Additionally, some acne treatments—particularly retinoids and chemical exfoliants—increase photosensitivity, making sun protection even more critical. The solution is finding the right sunscreen formulated specifically for oily or acne-prone skin.
Mineral sunscreens (zinc oxide and titanium dioxide) are often better tolerated than chemical sunscreens for acne-prone skin, though mineral sunscreens can feel heavier. Chemical sunscreens absorb into the skin and tend to feel lighter, making them more comfortable for oily skin. Look for “non-comedogenic” labels and consider sunscreens designed for acne-prone skin. Apply sunscreen daily, even on cloudy days, and reapply every two hours if you’re outdoors. The difference this makes in preventing dark scars and minimizing post-acne hyperpigmentation is substantial—often more visible than any acne treatment itself.
The 2026 Skincare Reality: Simplicity Beats Complexity
Dermatologists have identified a troubling 2026 trend: people are attempting increasingly complicated skincare routines inspired by viral content, and this over-complication is driving acne worse rather than better. The allure is understandable—if one active ingredient helps, surely five will work better, right? In reality, layering multiple active ingredients simultaneously irritates the skin barrier, triggers sensitivity, and often leads to a frustrating rebound effect where acne temporarily worsens before any improvement occurs.
The most effective skincare routines for oily, acne-prone skin are paradoxically simple: a gentle cleanser, a non-comedogenic moisturizer, and one or two targeted treatments (such as benzoyl peroxide or a retinoid). This streamlined approach allows your skin barrier to remain intact, prevents irritation, and gives you clear data about what’s working. If you’re tempted by the latest viral skincare hack or trend, ask yourself: has a dermatologist validated this for acne-prone skin, or is this marketing? The answer usually matters more than the hype.
Conclusion
The biggest skincare mistakes for oily, acne-prone skin all stem from the desire to do more to solve the problem faster. Over-cleansing, skipping moisturizer, using comedogenic products, changing treatments too frequently, applying treatments only to visible blemishes, squeezing pimples, and avoiding sunscreen are all mistakes that seem logical but backfire in reality.
The counterintuitive truth is that less intervention—a gentle, consistent routine with two daily cleansings, a lightweight moisturizer, and one or two evidence-based treatments—produces better results than aggressive or complicated regimens. Start by assessing your current routine: how many times daily are you cleansing? Are you using a moisturizer? What ingredients are in your products? Are you changing treatments frequently? Are you squeezing pimples? Once you identify your mistakes, focus on making one change at a time and giving it at least four to six weeks before evaluating results. Your skin barrier will thank you, your acne will likely improve, and you’ll finally break the cycle of over-treating your way to worse breakouts.
You Might Also Like
- Best Skincare Routine for Acne Prone Oily Skin That Actually Controls Breakouts
- The Most Common Cleanser Mistakes People With Combination Acne Skin Make
- How to Build a Simple Routine for Acne Prone Oily Skin Without Overloading Products
Browse more: Acne | Acne Scars | Adults | Back | Blackheads