Post-inflammatory erythema and hyperpigmentation are two fundamentally different skin conditions that both appear as marks after acne or skin inflammation, but they require completely different treatments. The key difference lies in what’s causing the discoloration: post-inflammatory erythema (PIE) appears as red or pink marks caused by dilated or damaged blood vessels beneath the skin, while post-inflammatory hyperpigmentation (PIH) appears as brown, gray, or black marks caused by excess melanin production. If you apply gentle pressure with a glass to a mark and it fades temporarily before returning, you’re likely dealing with PIE.
If the mark stays the same color despite the pressure, it’s PIH. Understanding which condition you have is critical because treating PIE with retinoids or chemical exfoliants—common PIH treatments—can actually make the redness worse and prolong your healing time. This article walks you through how to identify each condition, why they develop, how they differ in their healing timeline, and most importantly, which treatments actually work for each one. We’ll also explain why your skin tone matters when it comes to which condition you’re more likely to experience, and how sun exposure plays a major role in how long both conditions stick around.
Table of Contents
- How to Tell Post-Inflammatory Erythema Apart From Hyperpigmentation
- The Root Cause: Why These Marks Appear Differently
- The Timeline: How Long Each Condition Actually Lasts
- Treatment Strategies: Why You Can’t Use the Same Approach for Both
- The Irritation Risk: When Standard Acne Treatments Backfire
- Skin Tone and Which Condition You’re More Likely to Experience
- Sun Exposure: The Factor That Determines Your Healing Timeline
- Conclusion
How to Tell Post-Inflammatory Erythema Apart From Hyperpigmentation
The most reliable way to distinguish between PIE and PIH is the glass test, which works because of the fundamental difference in what’s causing the discoloration. Take a clean glass or transparent object and press it gently against the mark for a few seconds. If the spot blanches—meaning it fades to normal skin color—and then returns to red or pink when you remove the glass, you have post-inflammatory erythema. The blanching happens because you’re temporarily displacing the blood in the dilated blood vessels beneath the skin.
In contrast, if you perform the same test on a brown or gray spot and it doesn’t change color at all, you’re dealing with post-inflammatory hyperpigmentation caused by excess melanin that won’t be pushed away by pressure. Beyond the glass test, the color itself gives you clues. PIE marks are distinctly red, pink, or sometimes purple, while PIH marks range from light brown to dark brown, gray, or even black depending on your skin tone and how much melanin was produced. The distinction matters because many people waste months using the wrong treatments—someone using hydroquinone or retinoids on red PIE marks won’t see improvement and may actually irritate their skin further. If you’re ever unsure, the glass test is your most objective method to confirm which condition you’re dealing with.

The Root Cause: Why These Marks Appear Differently
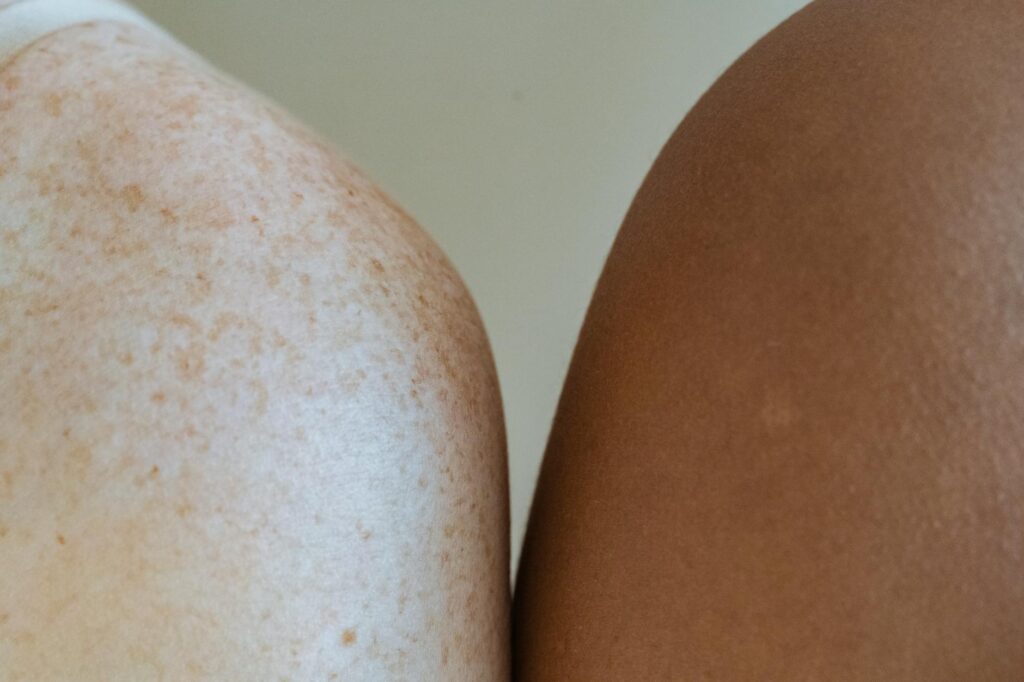
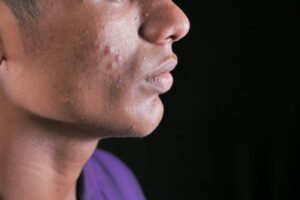
post-inflammatory erythema develops when acne or another inflammatory skin injury damages the blood vessels and capillaries in the dermis layer. When inflammation occurs, blood vessels dilate to bring immune cells and nutrients to the area. Sometimes this response damages the vessel walls, or the vessels remain dilated long after the inflammation has subsided, creating that persistent red appearance. The redness is literally dilated blood vessels showing through your skin—it’s a vascular issue, not a pigmentation issue. This is why PIE is more visible in people with lighter skin tones where red undertones are easier to see against the skin surface.
Post-inflammatory hyperpigmentation, by contrast, develops when melanocytes (the cells that produce pigment) overproduce melanin in response to inflammation. Your body sees the inflammatory injury and signals melanocytes to increase protection, but they overcompensate and create deposits of melanin that persist long after the inflammation has healed. This is why PIH is more common and more visible in people with medium to darker skin tones—melanin overproduction shows up more prominently in skin with naturally higher melanin levels. The key limitation here is that these two conditions can sometimes appear together on the same mark, especially if the original acne or injury was particularly severe. Someone might have both red PIE and brown PIH on the same spot, which complicates treatment because you can’t use the same approach for both simultaneously.
The Timeline: How Long Each Condition Actually Lasts
Post-inflammatory erythema typically resolves within a few weeks to a few months with appropriate treatment, but this timeline depends heavily on how severely the blood vessels were damaged and whether you protect your skin from sun exposure. If left untreated and repeatedly exposed to UV radiation, PIE can persist for months or even years as the damaged vessels struggle to fully heal. The inflammation perpetuates itself because sun exposure increases vasodilation and produces free radicals that prevent the blood vessels from normalizing. Someone who gets a post-acne red mark and doesn’t use sunscreen will watch that mark stay red far longer than someone who immediately starts sun protection and uses vascular treatments like IPL or PDL therapy.
Post-inflammatory hyperpigmentation typically takes longer to resolve than PIE—full resolution often requires several months to over a year depending on how much melanin was deposited and how consistently you use treatments that fade pigmentation. The timeline also varies based on your skin tone; deeper skin naturally takes longer because there’s more melanin to clear. Unlike PIE, which can improve relatively quickly with the right treatments, PIH requires patience and consistent use of fading agents. For example, someone with medium skin tone who develops PIH after moderate acne might see significant improvement in four to six months with daily retinoid use, while someone with deeper skin might need eight to twelve months or longer of the same treatment regimen.

Treatment Strategies: Why You Can’t Use the Same Approach for Both
Post-inflammatory erythema responds well to vascular treatments that directly target dilated blood vessels—specifically intense pulsed light (IPL) and pulsed dye laser (PDL) therapy, which use light wavelengths absorbed by hemoglobin in the blood vessels to reduce their visibility. Beyond professional treatments, topical ingredients like vitamin C, azelaic acid, and niacinamide can help reduce redness and strengthen vessel walls over time. Broad-spectrum sunscreen is non-negotiable for PIE because UV exposure worsens vasodilation and prolongs healing. The important caveat is that harsh treatments don’t help PIE—chemical exfoliants and retinoids, which are excellent for other skin concerns, can actually irritate PIE and make the redness worse because they increase skin sensitivity and blood flow to the area. Post-inflammatory hyperpigmentation requires a completely different approach focused on stopping melanin production and promoting the shedding of pigmented skin cells.
The most effective treatments include retinoids (like tretinoin or adapalene), chemical exfoliants (AHAs and BHAs), hydroquinone, and targeted pigment-fading treatments. These work by either inhibiting tyrosinase (the enzyme that produces melanin) or accelerating cell turnover to shed the pigmented cells faster. However, if you use these treatments on PIE marks, you risk making the redness worse through increased irritation. This is why the glass test and proper diagnosis are so critical—using the wrong treatment category can double your healing time. For example, someone with both PIE and PIH would need to use calming, vascular-focused treatments for the red portions while carefully introducing retinoids only for the hyperpigmented areas, potentially on different days or different parts of the face.
The Irritation Risk: When Standard Acne Treatments Backfire
Many people make the mistake of treating PIE with the same products they used to treat their original acne, assuming anything that helped with active breakouts will help with post-inflammatory marks. This assumption causes real problems because retinoids and chemical exfoliants, while excellent for unclogging pores and treating active acne, can intensify redness and inflammation in PIE-prone skin. When you apply a strong retinoid or AHA to PIE, you’re increasing skin sensitivity and blood flow to the area, which can trigger more vasodilation and actually deepen the red appearance. Someone with PIE who starts using nightly tretinoin might find their red marks get worse before they get better—or they might get worse and never get better if the irritation is too intense. The solution is to treat PIE with calming, anti-inflammatory ingredients and avoid aggressive exfoliation until the redness has significantly faded.
Niacinamide is particularly helpful because it reduces redness and inflammation without causing irritation. Azelaic acid is another excellent choice because it’s both calming and has some vascular-soothing properties. Only after PIE has substantially improved should you consider introducing gentler exfoliants or retinoids, and even then, you should introduce them slowly and at lower concentrations. The timeline matters too—if you’re still in the first few weeks after an inflammatory acne lesion, your focus should be on calming and protection, not treating. Jumping straight to aggressive treatments when your skin is still healing sets you back significantly.

Skin Tone and Which Condition You’re More Likely to Experience
Post-inflammatory erythema is more visible and therefore more commonly reported in people with lighter skin tones, where red and pink undertones stand out clearly against the skin surface. However, this doesn’t mean people with darker skin don’t get PIE—they do, but the redness is less visible because it doesn’t contrast as much with their natural skin color. Someone with deep skin tone might have significant PIE that barely shows as a visible mark, while someone with fair skin has a very noticeable red spot from the same level of blood vessel damage. This visibility difference has led to a misconception that PIE only affects lighter skin, when in reality it’s just that it’s harder to see.
Post-inflammatory hyperpigmentation is much more prevalent in people with medium to darker skin tones because melanin overproduction is more visible when you already have higher baseline melanin. Melanocytes in darker skin are naturally more reactive and more likely to overproduce melanin in response to inflammation, making PIH a more significant concern for this population. Someone with deep skin tone who experiences acne has a much higher likelihood of developing visible PIH marks than someone with fair skin from the same acne severity. This difference has real practical implications for treatment planning—people with darker skin may need to be more aggressive about treating PIH and more conservative about triggering additional inflammation that could worsen hyperpigmentation.
Sun Exposure: The Factor That Determines Your Healing Timeline
UV radiation is damaging for both PIE and PIH, but for different reasons and with different consequences. For post-inflammatory erythema, sun exposure increases vasodilation and generates free radicals that prevent damaged blood vessels from healing properly. Someone with PIE who spends their summer without sunscreen will watch their red marks persist or even deepen, while someone who uses daily SPF 30 or higher will see noticeable improvement in the same timeframe. The vasodilation triggered by UV heat actually perpetuates the condition, creating a cycle where sun exposure keeps vessels dilated and inflamed. This is why PIE healing timelines vary so dramatically—two people with identical post-acne redness might see completely different outcomes based purely on their sun protection habits.
For post-inflammatory hyperpigmentation, UV exposure triggers additional melanin production as your skin tries to protect itself from sun damage, essentially adding new hyperpigmentation on top of what’s already there. Someone fading PIH without sunscreen is essentially working against their skin because every sunny day adds more pigment while their treatment tries to fade what’s already there. This is why consistent broad-spectrum sunscreen use is absolutely critical for both conditions, not optional. The sunscreen needs to be applied daily, reapplied every two hours if you’re outdoors, and used year-round even on cloudy days because UV radiation penetrates clouds. Without this sun protection, even the most effective treatments for either condition work much more slowly.
Conclusion
The difference between post-inflammatory erythema and hyperpigmentation comes down to the mechanism causing the discoloration: dilated blood vessels creating redness versus excess melanin creating brown or gray marks. The glass test gives you an objective way to determine which one you have, and accurate diagnosis is essential because these conditions require opposite treatment approaches. Using retinoids or exfoliants on PIE makes it worse, while the vascular treatments that work for PIE don’t fade hyperpigmentation at all. Your skin tone influences which condition you’re more likely to experience and how visible it will be, with PIE more apparent in lighter skin and PIH more common and visible in darker skin.
The most important takeaway is that healing for either condition depends heavily on sun protection and using the right treatment category for what you’re dealing with. If you have red PIE marks, focus on vitamin C, azelaic acid, niacinamide, and daily sunscreen while considering IPL or PDL if the redness persists beyond two to three months. If you have brown PIH marks, introduce retinoids and chemical exfoliants gradually while maintaining consistent sun protection. For the fastest healing, get an accurate diagnosis using the glass test, choose treatments matched to your specific condition, and commit to daily sunscreen use regardless of which marks you’re fading.
You Might Also Like
- How to Treat Post Inflammatory Erythema After Acne and Reduce Red Marks Faster
- Why the NHS Acne Treatment Path Is Slower Than Private Care in the UK
- Why Managing Expectations Is the Hardest Part of Acne Scar Treatment
Browse more: Acne | Acne Scars | Adults | Back | Blackheads