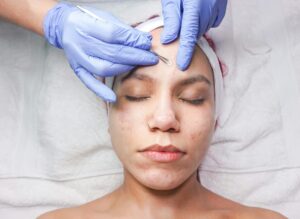
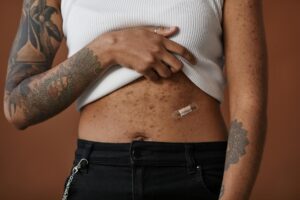
Petroleum jelly, commonly known as Vaseline, is a staple in many skincare routines for its occlusive properties that lock in moisture and protect the skin barrier. However, for some individuals prone to fungal acne, this seemingly innocent product can trigger or exacerbate breakouts.
Fungal acne, medically termed pityrosporum folliculitis or Malassezia folliculitis, arises from an overgrowth of Malassezia yeast in hair follicles, leading to uniform small pimples that mimic bacterial acne but resist standard treatments. This article explores why petroleum jelly poses a risk for fungal acne in susceptible people, drawing from dermatological insights on yeast behavior and skincare interactions. Readers will learn the science behind the issue, how to identify if they are affected, safe alternatives, and practical steps to prevent flare-ups while maintaining healthy skin.
Table of Contents
- What Exactly Is Fungal Acne and How Does It Differ from Regular Acne?
- Why Does Petroleum Jelly Feed Fungal Growth in Some People?
- Who Is Most at Risk for Fungal Acne from Occlusives Like Petroleum Jelly?
- Ingredients in Skincare That Mimic Petroleum Jelly's Fungal Risks
- Diagnosing and Treating Fungal Acne Triggered by Petroleum Jelly
- How to Apply This
- Expert Tips
- Conclusion
- Frequently Asked Questions
What Exactly Is Fungal Acne and How Does It Differ from Regular Acne?
Fungal acne stems from an overgrowth of Malassezia yeast, a naturally occurring fungus on human skin that thrives in hair follicles when conditions favor its proliferation. Unlike regular acne vulgaris, which involves blocked pores from dead skin, excess oil, and Propionibacterium acnes bacteria, fungal acne specifically infects follicles due to yeast, often presenting as itchy, uniform whiteheads without blackheads.
The confusion arises because both conditions produce pimple-like bumps, leading many to apply antibacterial acne treatments that worsen fungal overgrowth by killing competing bacteria without addressing the yeast. Factors like humidity, sweat, and occlusive products create a warm, moist environment ideal for Malassezia, distinguishing it from bacterial acne's reliance on sebum and inflammation.
- Itchy, uniform small bumps on the forehead, chest, back, or arms, often in clusters
- Lack of blackheads or cysts, unlike bacterial acne
- Resistance to benzoyl peroxide or salicylic acid, but improvement with antifungal treatments
Why Does Petroleum Jelly Feed Fungal Growth in Some People?
Petroleum jelly acts as a heavy occlusive, forming a thick barrier that traps moisture and oils on the skin, creating the warm, anaerobic environment Malassezia yeast craves for unchecked growth. While it suffocates some surface yeasts in anecdotal reports, its inability to penetrate follicles allows deeper Malassezia to proliferate by preventing natural shedding and airflow.
Yeast like Malassezia is lipid-dependent, metabolizing skin oils and fatty acids; petroleum jelly, though not oily itself, enhances sebum retention, providing nutrients that fuel fungal colonies without balancing bacterial competition. People in humid climates or with high sebum production are particularly vulnerable, as the jelly exacerbates oil buildup in follicles.
- Creates a sealed, humid microenvironment ideal for yeast overgrowth
- Traps natural skin oils that nourish Malassezia
- Commonly used post-cleansing or on damp skin, amplifying moisture retention
Who Is Most at Risk for Fungal Acne from Occlusives Like Petroleum Jelly?
Certain individuals have skin microbiomes or lifestyles that predispose them to Malassezia overgrowth when using heavy occlusives. Those in hot, humid environments or with excessive sweating experience amplified risk, as sweat combined with petroleum jelly's barrier fosters yeast-friendly conditions.
Recent antibiotic use, immunosuppression, or steroid treatments disrupt microbial balance, allowing yeast dominance, while teenagers and those with oily skin produce more sebum that pairs dangerously with occlusives. Genetic factors influencing sebum composition may also play a role, making some skins more hospitable to lipid-loving fungi.
- Living in humid climates or frequent heavy sweating
- History of antibiotics or immunosuppressive medications
- Oily skin types or high sebum production

Ingredients in Skincare That Mimic Petroleum Jelly's Fungal Risks
Beyond petroleum jelly, many emollients share its pore-clogging, occlusive nature, feeding Malassezia by delivering or trapping fatty acids it metabolizes. Oils rich in lauric, oleic, or palmitic acids, like coconut oil, directly nourish yeast while blocking follicles, much like petroleum jelly's indirect support through sebum occlusion.
Fermented ingredients and certain emulsifiers such as polysorbates further promote fungal growth by introducing yeast-friendly compounds or preventing evaporation. Fatty alcohols from plant sources add to the problem by comedogenicity, creating a cumulative effect in multi-ingredient products.
Diagnosing and Treating Fungal Acne Triggered by Petroleum Jelly
Suspect fungal acne if petroleum jelly use coincides with persistent, itchy uniform bumps unresponsive to acne topicals; a dermatologist can confirm via skin scraping or clinical exam. Treatment involves antifungal agents like ketoconazole shampoo or oral fluconazole to target Malassezia directly, alongside discontinuing occlusives.
Clearance often occurs within weeks of removing triggers and incorporating sulfur-based washes or tea tree oil, which disrupt yeast without harsh drying. Post-treatment, rebuilding the barrier with non-comedogenic, breathable moisturizers prevents recurrence while maintaining hydration.
How to Apply This
- Patch test new products on your inner arm for 48 hours to check for fungal triggers before full-face use.
- Discontinue petroleum jelly immediately if bumps appear, and cleanse gently twice daily with an antifungal shampoo like ketoconazole as a face wash.
- Switch to lightweight, non-occlusive moisturizers such as squalane or hyaluronic acid serums that hydrate without trapping oils.
- Monitor skin in a journal, noting humidity, sweat, and product changes to identify personal triggers early.
Expert Tips
- Opt for "fungal acne safe" lists from dermatologists, avoiding esters, fatty acids, and polysorbates in ingredient checks
- Shower immediately after sweating and wear breathable fabrics to reduce moisture buildup
- Use oil-free, mattifying sunscreens to prevent occlusive layering on humid days
- Incorporate probiotics or prebiotic skincare sparingly to support microbial balance post-treatment
Conclusion
Understanding petroleum jelly's role in fungal acne empowers skincare enthusiasts to choose products that protect rather than provoke.
By recognizing occlusive risks and prioritizing antifungal strategies, you can achieve clearer skin without compromising hydration. Ultimately, personalized routines tailored to your skin's microbial needs offer the best defense, turning potential pitfalls like Vaseline into informed choices for lasting acne control.
Frequently Asked Questions
Can everyone get fungal acne from petroleum jelly?
No, only those with predisposing factors like oily skin, humidity exposure, or microbial imbalance; many tolerate it well.
How long does it take for fungal acne to clear after stopping petroleum jelly?
Typically 1-4 weeks with antifungal treatment, though full resolution may take longer if deeply entrenched.
Are there safe occlusive alternatives for dry skin prone to fungal acne?
Yes, dimethicone-based silicones or lightweight lanolin derivatives provide barrier protection without feeding yeast.
Does fungal acne leave scars like regular acne?
Rarely, as it primarily causes superficial inflammation without deep cyst formation.