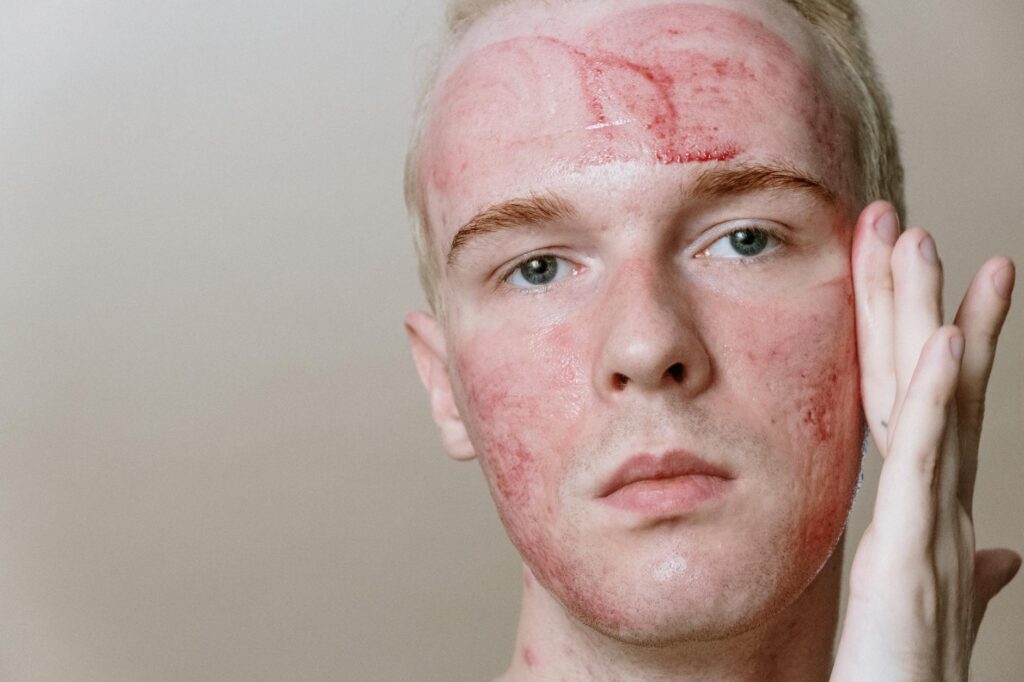
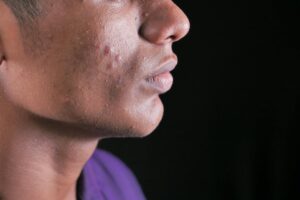
Probiotics help acne-prone skin by reducing systemic inflammation, strengthening the skin barrier, and rebalancing the gut-skin axis that often drives persistent breakouts. Oral probiotic strains like Lactobacillus rhamnosus and Lactobacillus acidophilus have shown measurable reductions in acne lesion counts in clinical trials, while topical probiotics can calm redness and prevent the overgrowth of Cutibacterium acnes, the bacterium most associated with inflammatory pimples. A 2010 Italian study found that participants taking a Lactobacillus and Bifidobacterium supplement alongside standard acne treatment had significantly better outcomes than those using standard treatment alone, with clearer skin and fewer relapses over a 12-week period.
This article breaks down the specific mechanisms behind how probiotics influence acne, which strains have the strongest evidence, and what the realistic limitations are. We will also cover the difference between oral and topical probiotics, how long they take to show results, common mistakes people make when choosing probiotic products, and who should be cautious about adding them to a skincare routine. If you have been cycling through benzoyl peroxide and salicylic acid without lasting improvement, understanding the microbial component of acne may fill in a missing piece.
Table of Contents
- How Do Probiotics Actually Affect Acne-Prone Skin?
- Which Probiotic Strains Have the Strongest Evidence for Acne?
- Oral vs. Topical Probiotics — What Works Better for Breakouts?
- How to Choose and Use Probiotics for Acne Results
- When Probiotics Do Not Work — and When They Make Things Worse
- The Role of Prebiotics and Diet in Supporting Probiotic Benefits
- Where Probiotic Acne Research Is Heading
- Conclusion
- Frequently Asked Questions
How Do Probiotics Actually Affect Acne-Prone Skin?
The connection between probiotics and acne runs through two main pathways: the gut and the skin surface itself. In the gut, probiotics influence the composition of your intestinal microbiome, which directly affects systemic inflammation levels. When your gut flora is imbalanced — a state called dysbiosis — the intestinal lining becomes more permeable, allowing inflammatory molecules like lipopolysaccharides to leak into the bloodstream. This chronic low-grade inflammation shows up in the skin as increased sebum production, heightened sensitivity to androgens, and a more aggressive inflammatory response to clogged pores. Probiotics help seal that leaky gut lining and reduce the overall inflammatory load your skin has to deal with. On the skin’s surface, topical probiotics work differently. They produce antimicrobial peptides called bacteriocins that can inhibit the growth of pathogenic bacteria without wiping out beneficial microbes the way antibiotics do.
Think of it as introducing a competitor species rather than carpet-bombing the entire ecosystem. Some probiotic strains also produce short-chain fatty acids that lower the skin’s pH, creating an environment less hospitable to acne-causing bacteria. A practical comparison: oral antibiotics like doxycycline reduce acne bacteria systemically but also destroy gut flora, often causing rebound breakouts once you stop. Probiotics attempt to achieve bacterial balance without that destructive tradeoff. The concept dermatologists now reference is the “gut-skin axis,” first proposed by John Stokes and Donald Pillsbury back in 1930. They hypothesized that emotional states alter gut flora, increase intestinal permeability, and contribute to skin inflammation. Modern research has largely vindicated this theory, though the mechanisms turned out to be more complex than they imagined.

Which Probiotic Strains Have the Strongest Evidence for Acne?
Not all probiotics are interchangeable, and this is where many people waste money on products that are unlikely to help their skin. The strains with the most clinical support for acne specifically include Lactobacillus rhamnosus SP1, which was tested in a 2016 randomized controlled trial published in Beneficial Microbes. Participants taking this strain for 12 weeks experienced a significant reduction in adult acne compared to placebo, particularly in the expression of genes related to insulin signaling — a known driver of sebum production and pore-clogging. Lactobacillus acidophilus and Bifidobacterium bifidum have also shown positive results when combined, especially in the Italian study mentioned earlier where they complemented antibiotic therapy. For topical use, Streptococcus thermophilus has demonstrated an ability to increase ceramide production in the skin, which strengthens the barrier and reduces the transepidermal water loss that often accompanies acne treatments like retinoids. Lactobacillus plantarum has shown anti-inflammatory effects in topical formulations tested on acne lesions.
However, if you have a compromised immune system, including anyone on immunosuppressive medications or undergoing chemotherapy, introducing live bacteria topically carries real risk. Even generally safe strains can cause infections in immunocompromised individuals, and this is a scenario where you absolutely need to consult a physician first. The colony forming unit count matters too. Most studies showing acne improvement used products delivering at least one billion CFUs daily. Many commercial probiotic supplements contain this amount, but cheaper options sometimes overstate their CFU counts or fail to keep cultures alive through manufacturing and shelf life. Third-party tested brands are worth the premium here.
Oral vs. Topical Probiotics — What Works Better for Breakouts?
The honest answer is that oral and topical probiotics address different aspects of acne, and for moderate to severe cases, using both may be more effective than either alone. Oral probiotics tackle the systemic inflammation and gut permeability issues that set the stage for breakouts across your entire face and body. If your acne appears in multiple zones — jawline, forehead, chest, and back — gut-level intervention makes more sense because no topical product can cover that much territory efficiently. A person dealing with hormonal cystic acne along the chin and jawline, for example, would likely benefit more from oral Lactobacillus rhamnosus addressing insulin and androgen signaling pathways than from applying a probiotic cream to individual cysts. Topical probiotics shine for localized concerns: calming a specific inflamed area, reducing post-inflammatory redness, or maintaining the skin’s acid mantle after aggressive treatments like chemical peels or prescription retinoids.
Some newer formulations use “postbiotics” — the metabolic byproducts of probiotic bacteria — rather than live cultures. These are more shelf-stable and less likely to cause reactions, though they lack the colonization benefits of live strains. Products from brands like La Roche-Posay and Mother Dirt have incorporated this postbiotic approach with varying degrees of clinical backing. One important caveat: topical probiotics can initially cause a brief purging period where skin appears to worsen for one to two weeks as the microbial balance shifts. This is not the same as an allergic reaction, which would involve hives, itching, or swelling. If you experience the latter, discontinue immediately.

How to Choose and Use Probiotics for Acne Results
Start by identifying whether your acne pattern suggests a gut-driven component. Signs include concurrent digestive issues like bloating, irregular bowel movements, or food sensitivities alongside breakouts. A history of antibiotic use for acne — which disrupts gut flora — is another strong indicator. If these apply, begin with an oral probiotic containing Lactobacillus and Bifidobacterium strains at a minimum of one billion CFUs. Take it with food to improve survival through stomach acid. Refrigerated probiotics generally maintain potency better than shelf-stable ones, though spore-based formulations like Bacillus coagulans are a notable exception since they survive heat and stomach acid more reliably. The tradeoff with oral probiotics is patience versus immediacy. You will not see skin changes in a week.
Most clinical trials run 8 to 12 weeks before measuring outcomes, and anecdotal reports from dermatology forums suggest noticeable improvement often starts around week four to six. Compare this to benzoyl peroxide, which can reduce surface bacteria within days, or a retinoid, which accelerates cell turnover within two to four weeks. Probiotics are slower because they work upstream — fixing the environment that produces acne rather than treating individual pimples. This means they pair well with conventional treatments rather than replacing them. The combination of a standard topical regimen plus an oral probiotic has more support than probiotics used as a sole treatment. For topical probiotic products, apply them after cleansing but before heavier treatments like retinoids or moisturizers. Check that the product specifies which strains it contains and at what concentration. “Probiotic-infused” on a label without strain names or CFU counts is a marketing term, not a clinical claim.
When Probiotics Do Not Work — and When They Make Things Worse
Probiotics are not a universal fix for acne, and setting realistic expectations matters. They tend to be least effective for purely comedonal acne — blackheads and whiteheads without significant inflammation — because their primary mechanism is anti-inflammatory. If your acne is mainly non-inflamed clogged pores, a retinoid or salicylic acid will outperform probiotics. Similarly, probiotics will not override acne driven by high-androgen conditions like polycystic ovary syndrome unless those hormonal drivers are also being managed. There are also situations where probiotics can actively worsen skin.
People with small intestinal bacterial overgrowth, known as SIBO, sometimes experience increased bloating, gas, and paradoxically more skin inflammation when taking Lactobacillus-based probiotics, because they are adding more bacteria to an already overpopulated small intestine. A 2018 study in Clinical and Translational Gastroenterology found that some probiotic users developed brain fog and significant bloating due to D-lactic acidosis from bacterial overgrowth. If you notice digestive symptoms getting worse rather than better after starting a probiotic, stop taking it and get evaluated for SIBO before continuing. Another limitation is strain-specificity. The probiotic yogurt you eat at breakfast almost certainly does not contain the strains tested in acne research, and the doses are far lower than what clinical trials use. Fermented foods like kimchi and kefir support general gut diversity, which is beneficial, but they should not be confused with targeted probiotic supplementation.

The Role of Prebiotics and Diet in Supporting Probiotic Benefits
Probiotics do not operate in isolation — they need fuel. Prebiotics are the non-digestible fibers that feed beneficial gut bacteria, and without adequate prebiotic intake, supplemented probiotic strains may not colonize effectively. Foods high in prebiotic fiber include garlic, onions, leeks, asparagus, and oats.
A person taking a Lactobacillus supplement while eating a low-fiber, high-sugar diet is essentially planting seeds in poor soil. High-glycemic diets have independently been linked to increased acne severity through insulin and IGF-1 pathways, so dietary changes that support probiotic efficacy also happen to reduce acne triggers directly. Some supplement manufacturers now combine probiotics with prebiotic fiber in a single capsule, often marketed as “synbiotics.” These can be convenient, though you will typically get more prebiotic fiber from food than from a capsule. The practical takeaway: address diet alongside supplementation, or the probiotic is working against a headwind.
Where Probiotic Acne Research Is Heading
The next frontier in probiotic acne treatment is personalization. Researchers at the University of California San Diego and other institutions are mapping individual skin microbiomes to identify which specific bacterial imbalances correlate with each person’s breakouts. The goal is to move beyond one-size-fits-all Lactobacillus capsules toward custom probiotic blends tailored to your unique microbial fingerprint.
Early-stage companies are already offering skin microbiome testing kits, though the science connecting those test results to effective treatment recommendations is still maturing. Bacteriophage therapy — using viruses that selectively target Cutibacterium acnes without harming other skin bacteria — is another promising avenue being studied alongside probiotic approaches. If these targeted therapies reach clinical use, they could replace broad-spectrum antibiotics for acne entirely. For now, probiotics represent the most accessible way to work with your body’s microbial ecosystem rather than against it, and the evidence base, while still developing, is strong enough to warrant serious consideration as part of a comprehensive acne management plan.
Conclusion
Probiotics offer acne-prone skin a fundamentally different approach than conventional treatments. Rather than killing bacteria or forcing skin cells to turn over faster, they address the inflammatory and microbial imbalances that make skin vulnerable to breakouts in the first place. The strongest evidence supports oral Lactobacillus rhamnosus and Lactobacillus acidophilus strains taken at adequate doses for at least 8 to 12 weeks, ideally alongside standard topical treatments and a diet that supports gut health.
The practical next step is straightforward: if your acne involves persistent inflammation and has not fully responded to topical treatments alone, add a clinically supported oral probiotic and give it a genuine trial period. Pair it with prebiotic-rich foods and keep your existing skincare routine in place. Track your skin weekly with photos so you can assess changes objectively rather than relying on daily mirror checks, which are notoriously unreliable for evaluating gradual improvement. Probiotics are not a miracle cure, but for the right person with the right strain, they can be the missing variable in a stubborn acne equation.
Frequently Asked Questions
How long do probiotics take to improve acne?
Most clinical studies measure outcomes at 8 to 12 weeks. Some people notice reduced inflammation as early as four weeks, but meaningful improvement in lesion count and overall skin clarity typically requires at least two months of consistent daily use.
Can I just eat yogurt instead of taking a probiotic supplement?
Yogurt contains some beneficial bacteria, but the strains and doses rarely match what has been tested in acne research. A single serving of yogurt might deliver 100 million CFUs of non-specific strains, while acne studies typically use 1 billion or more CFUs of targeted strains like Lactobacillus rhamnosus SP1.
Do probiotics cause purging or initial breakouts?
Some people report a brief worsening in the first one to two weeks, particularly with topical probiotics, as the skin microbiome adjusts. This should be mild and temporary. Severe or prolonged worsening is not normal purging and warrants stopping the product.
Should I take probiotics if I am already on antibiotics for acne?
Yes, and this may be one of the most beneficial times to take them. Antibiotics disrupt gut flora, which can lead to rebound breakouts after discontinuation. Taking probiotics during and after an antibiotic course helps maintain microbial balance. Space them at least two hours apart so the antibiotic does not immediately kill the probiotic bacteria.
Are topical probiotics safe to use with retinoids or benzoyl peroxide?
Topical probiotics can generally be layered with retinoids, though apply the probiotic first and allow it to absorb before applying the retinoid. Benzoyl peroxide is antimicrobial by nature and will likely kill the live probiotic organisms on contact, so use them at different times of day if combining both.
Do probiotics help with acne scars or just active breakouts?
Probiotics primarily address active inflammation and new breakout prevention. There is limited evidence that the anti-inflammatory effects may modestly improve post-inflammatory erythema — the red or pink marks left after pimples heal — but they will not meaningfully improve depressed or raised scars, which require procedures like microneedling or laser treatment.
You Might Also Like
- Why Your Gut Health Directly Affects Your Acne
- Why Your Acne Gets Worse in Winter
- Why Stopping Birth Control Causes an Acne Flare
Browse more: Acne | Acne Scars | Adults | Back | Blackheads