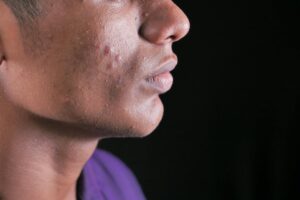
DHEA — dehydroepiandrosterone — is an adrenal hormone that your body converts into androgens like testosterone and dihydrotestosterone, and elevated levels of DHEA or its sulfated form DHEA-S are one of the most overlooked drivers of persistent acne in adult women. When DHEA-S is high, it stimulates sebaceous glands to produce excess oil, thickens the follicular lining, and creates the exact conditions that lead to deep, cystic breakouts along the jawline, chin, and lower cheeks — the classic “hormonal acne” pattern that no amount of salicylic acid face wash will fix. A 35-year-old woman who has been battling stubborn chin acne for years despite a solid skincare routine may finally get answers when bloodwork reveals her DHEA-S is sitting at 400 µg/dL, well above the typical range for her age.
The relationship between DHEA and adult female acne is not just about having “high androgens” in a general sense. DHEA occupies a specific upstream position in the hormonal cascade, meaning it feeds multiple androgenic pathways simultaneously. This article covers how DHEA differs from other androgens in its effect on skin, why standard hormone panels sometimes miss it, what conditions cause DHEA-S to spike, how to get tested properly, treatment approaches that actually target DHEA-driven acne, and when elevated DHEA-S signals something more serious than a skincare problem.
Table of Contents
- Why Does DHEA Cause Acne in Adult Women?
- How DHEA-S Levels Change with Age and Why That Matters for Breakouts
- The Adrenal Stress Connection and DHEA-Driven Breakouts
- Testing DHEA-S Properly and What to Do with the Results
- Treatment Approaches That Actually Target DHEA-Related Acne
- DHEA, Birth Control, and the Oral Contraceptive Factor
- Emerging Research on DHEA, Skin Enzymes, and Future Treatment Targets
- Conclusion
- Frequently Asked Questions
Why Does DHEA Cause Acne in Adult Women?
DHEA is produced primarily by the adrenal glands, with a smaller contribution from the ovaries. What makes it particularly relevant to acne is that skin cells themselves contain the enzymes needed to convert DHEA into more potent androgens — testosterone and DHT — right at the sebaceous gland. So even when a woman’s total testosterone level looks normal on a blood test, locally elevated DHEA conversion in the skin can still flood oil glands with androgenic stimulation. This is why some dermatologists call DHEA-S the “hidden androgen” in adult female acne cases. The mechanism works like this: DHEA-S circulates in the blood as a relatively stable sulfated form. When it reaches the skin, sulfatase enzymes strip off the sulfate group, converting it to active DHEA.
From there, 3β-hydroxysteroid dehydrogenase and 17β-hydroxysteroid dehydrogenase convert it stepwise into androstenedione, then testosterone, then DHT. DHT is roughly five to ten times more potent than testosterone at binding androgen receptors on sebocytes. A woman whose DHEA-S is elevated is essentially supplying raw material for a local androgen factory in her skin, regardless of what her ovaries are doing. Compare this to polycystic ovary syndrome, where excess androgens are often ovarian in origin. A woman with PCOS might have elevated total testosterone and DHEA-S simultaneously, while a woman with adrenal-driven acne might show normal testosterone but isolated high DHEA-S. The distinction matters because the treatment approaches differ. Spironolactone, for instance, blocks the androgen receptor and is effective in both scenarios, but if the root cause is adrenal overproduction, addressing stress and cortisol dysregulation may be equally important.
How DHEA-S Levels Change with Age and Why That Matters for Breakouts
DHEA-S peaks in a woman’s early to mid-twenties and then gradually declines throughout adulthood. By age 40, most women have roughly half the DHEA-S they had at 25, and by 60, levels may be only 10 to 20 percent of their youthful peak. This natural decline is part of what’s sometimes called “adrenopause.” Given this trajectory, you might expect acne to simply improve with age. For many women, it does. But for a significant subset, acne either persists or actually worsens in the late twenties and thirties — and that often correlates with DHEA-S levels that remain stubbornly elevated relative to age-adjusted norms. The important caveat here is that “normal range” on a lab report is not the same as “optimal for clear skin.” A DHEA-S level of 350 µg/dL might fall within the reference range for a 30-year-old woman, but if that same woman is highly sensitive to androgens at the receptor level — a genetic trait — that technically normal level can still drive significant acne.
This is a limitation of relying on lab numbers alone. Some women with DHEA-S of 200 break out terribly, while others at 400 have clear skin. Receptor sensitivity, which cannot be easily tested, plays an enormous role. However, if your DHEA-S is above the age-adjusted reference range — say, above 400 µg/dL for a woman in her thirties — that warrants further investigation regardless of skin symptoms. Markedly elevated DHEA-S can signal conditions like non-classic congenital adrenal hyperplasia, adrenal tumors, or Cushing’s syndrome. The acne, in that case, is a symptom of something that needs medical evaluation beyond a dermatology appointment.
The Adrenal Stress Connection and DHEA-Driven Breakouts
One of the most clinically relevant triggers for elevated DHEA-S in otherwise healthy adult women is chronic stress. The adrenal glands produce both cortisol and DHEA in response to ACTH stimulation from the pituitary gland. Under sustained psychological or physiological stress, the adrenals ramp up production across the board. While cortisol gets most of the attention in popular health discussions, DHEA-S rises in tandem, and the skin pays the price. Consider a woman in her early thirties working a high-pressure job with poor sleep. She notices that her acne flares predictably during stressful project deadlines, not during her menstrual period. Her breakouts cluster along the jawline and neck, not the forehead or nose.
A hormone panel reveals normal estrogen, progesterone, and testosterone, but DHEA-S is elevated at 420 µg/dL. Her doctor initially attributes the acne to “stress” in vague terms, but the specific mechanism is adrenal androgen overproduction. Addressing the acne effectively means addressing the adrenal output — through stress management, sleep optimization, and potentially targeted supplementation or medication — rather than just layering on topical retinoids. This adrenal pathway also explains why some women experience acne flares during periods of intense exercise, caloric restriction, or illness. All of these are physiological stressors that activate the hypothalamic-pituitary-adrenal axis. Marathon training, for example, is a well-documented trigger for adrenal androgen elevation. The takeaway is that DHEA-driven acne is not always a “hormone disorder” in the traditional sense — sometimes it’s a stress disorder manifesting through the skin.

Testing DHEA-S Properly and What to Do with the Results
If you suspect DHEA is contributing to your acne, the correct test is serum DHEA-S — not DHEA alone. DHEA fluctuates throughout the day and has a short half-life, making a single measurement unreliable. DHEA-S, by contrast, is the sulfated storage form. It has a much longer half-life, remains relatively stable throughout the day, and provides a more accurate picture of your adrenal androgen status. Most endocrinologists and informed dermatologists will order DHEA-S as part of a hormonal acne workup, but some practitioners skip it in favor of only checking total testosterone and free testosterone, which misses the adrenal piece entirely. A comprehensive hormonal acne panel should include DHEA-S, total testosterone, free testosterone, sex hormone-binding globulin, androstenedione, and ideally 17-hydroxyprogesterone to screen for late-onset congenital adrenal hyperplasia. Timing matters less for DHEA-S than for other hormones, but drawing the blood in the morning gives the most reproducible results.
If DHEA-S comes back elevated, the tradeoff in next steps depends on how high it is. Mildly elevated levels in the context of clear stress and acne may warrant a trial of anti-androgen therapy and lifestyle modification. Levels above 500 to 600 µg/dL, or rapidly rising DHEA-S, should prompt imaging of the adrenal glands and further endocrine workup to rule out tumors or enzymatic defects. One comparison worth noting: salivary hormone testing and dried urine tests like the DUTCH panel also measure DHEA and its metabolites. The DUTCH test, in particular, shows downstream androgen metabolites like 5α-androstanediol and androsterone, which can help clarify whether the body is converting DHEA aggressively toward DHT. This additional detail is useful but not essential for initial evaluation. Serum DHEA-S through a standard blood draw remains the most validated and widely accepted first step.
Treatment Approaches That Actually Target DHEA-Related Acne
The standard first-line pharmaceutical treatment for androgen-mediated acne in women is spironolactone, typically dosed at 50 to 200 mg daily. Spironolactone works by blocking the androgen receptor, which means it reduces the skin’s response to androgens regardless of whether those androgens originate from the ovaries or the adrenals. For DHEA-driven acne specifically, this receptor-level blockade is effective because it intercepts the endpoint of the DHEA-to-DHT conversion chain. Most women see meaningful improvement within three to six months. However, spironolactone has limitations. It does not reduce DHEA-S production itself — it only blocks the receptor. If the underlying cause of elevated DHEA-S is chronic adrenal stress, the hormone levels remain high and may contribute to other symptoms like oily hair, thinning scalp hair, or menstrual irregularity.
Women who want to address the root cause rather than just the skin symptoms may need to work on adrenal modulation: consistent sleep schedules, stress reduction techniques, blood sugar regulation, and in some cases adaptogenic supplements like phosphatidylserine, which has some evidence for blunting exaggerated cortisol and DHEA responses to stress. The evidence for adaptogens is mixed and modest, so expectations should be tempered accordingly. A significant warning: some women with acne turn to over-the-counter DHEA supplements for anti-aging or energy purposes, not realizing that supplemental DHEA will worsen their skin. DHEA supplements are widely available and aggressively marketed to women over 30 for bone health, libido, and vitality. If you are prone to hormonal acne, exogenous DHEA is essentially adding fuel to the fire. Even low doses of 10 to 25 mg daily can measurably increase DHEA-S and trigger breakouts within weeks. If you are currently taking a DHEA supplement and struggling with acne, stopping it should be the very first intervention.
DHEA, Birth Control, and the Oral Contraceptive Factor
Combined oral contraceptives are another common treatment for hormonal acne, and they work partly by increasing sex hormone-binding globulin, which binds free testosterone and reduces its availability to skin. Some formulations — particularly those containing drospirenone, norgestimate, or cyproterone acetate — have additional anti-androgenic properties. For women whose acne involves both ovarian and adrenal androgens, combining an oral contraceptive with spironolactone can be more effective than either alone.
That said, oral contraceptives have less direct impact on DHEA-S itself compared to their effect on ovarian androgens. A woman whose acne is driven almost entirely by adrenal DHEA overproduction may find that the pill helps somewhat but doesn’t fully clear her skin. This is one reason some women feel frustrated after being prescribed birth control for acne — if the adrenal component isn’t being addressed, results may plateau. For example, a woman might go from severe cystic breakouts to moderate persistent acne on the pill, then finally achieve clearance only after adding spironolactone or implementing meaningful stress reduction.
Emerging Research on DHEA, Skin Enzymes, and Future Treatment Targets
The next frontier in understanding DHEA-related acne lies in the enzymes that convert DHEA into active androgens within the skin itself. Researchers are investigating topical inhibitors of 5α-reductase type 1 — the enzyme isoform predominant in sebaceous glands — as a way to block DHT production locally without systemic anti-androgen effects. Some compounds in early-stage trials aim to inhibit 3β-hydroxysteroid dehydrogenase in the skin, which would interrupt the conversion of DHEA to androstenedione before it even reaches the testosterone stage.
There is also growing interest in the role of the skin microbiome in modulating local androgen metabolism. Certain bacterial populations on the skin appear to influence sulfatase activity, potentially affecting how much circulating DHEA-S gets converted to active DHEA at the follicular level. If confirmed, this could eventually lead to probiotic or microbiome-targeted therapies that reduce androgenic acne by changing the skin’s enzymatic environment rather than altering systemic hormone levels. For now, these approaches remain in the research phase, but they represent a promising shift toward more targeted, personalized treatment for DHEA-driven acne.
Conclusion
DHEA-S is a critical and frequently overlooked piece of the hormonal acne puzzle in adult women. Produced mainly by the adrenal glands, it serves as a precursor that the skin converts into potent androgens like DHT, driving sebum overproduction and the deep, inflammatory breakouts that characterize hormonal acne. Chronic stress, inadequate sleep, intense exercise, and certain medical conditions can all elevate DHEA-S, and the standard acne workup sometimes fails to test for it. Understanding this pathway explains why some women with “normal” testosterone levels still struggle with persistent jawline and chin acne that refuses to respond to topical treatments alone.
If you suspect DHEA is playing a role in your breakouts, request a serum DHEA-S test as part of a comprehensive hormone panel. Work with a dermatologist or endocrinologist who understands the distinction between ovarian and adrenal androgens. Treatment may include spironolactone, combined oral contraceptives, or lifestyle modifications targeting adrenal health — and if you are currently supplementing with DHEA, stopping is the most immediate and impactful step. Hormonal acne is solvable once you identify the right hormonal driver, and DHEA-S is one that deserves far more attention than it typically gets.
Frequently Asked Questions
What is a normal DHEA-S level for an adult woman?
Reference ranges vary by lab and age. Generally, for women aged 30 to 39, the typical range is roughly 45 to 270 µg/dL, though some labs extend the upper limit to around 400 µg/dL. Levels above the age-adjusted range warrant further evaluation, but even levels within the “normal” range can contribute to acne in women with high androgen receptor sensitivity.
Can DHEA-S cause acne even if my testosterone is normal?
Yes. DHEA-S is converted into testosterone and DHT locally within the skin by enzymes in the sebaceous glands. Your blood testosterone level can be completely normal while your skin is producing significant amounts of androgen from DHEA-S at the follicular level.
Will stopping a DHEA supplement clear my acne?
In many cases, yes — but it takes time. DHEA-S has a long half-life, so after discontinuing a supplement, it may take four to eight weeks for levels to normalize and several more weeks for existing acne lesions to resolve. Expect a timeline of roughly two to four months before seeing meaningful improvement.
Does spironolactone lower DHEA-S?
No. Spironolactone blocks the androgen receptor, preventing testosterone and DHT from exerting their effects on the skin. It does not reduce DHEA-S production by the adrenal glands. However, by blocking the endpoint, it effectively neutralizes the skin impact of elevated DHEA-S.
Should I see a dermatologist or an endocrinologist for DHEA-related acne?
Ideally, start with a dermatologist who has experience with hormonal acne and routinely orders hormone panels including DHEA-S. If your DHEA-S is significantly elevated or if there is suspicion of an underlying adrenal condition like congenital adrenal hyperplasia or an adrenal tumor, a referral to an endocrinologist is appropriate.
Can diet affect DHEA-S levels?
Directly, the evidence is limited. However, blood sugar instability and insulin resistance can amplify adrenal androgen production. Diets high in refined carbohydrates may contribute to elevated DHEA-S indirectly through insulin-mediated pathways. Maintaining stable blood sugar through balanced meals with adequate protein, fat, and fiber is a reasonable supportive measure but should not be considered a standalone treatment.
You Might Also Like
- What Causes Acne in People With PCOS
- Why Your Back Acne Won’t Go Away
- Why Your Acne Gets Worse in Winter
Browse more: Acne | Acne Scars | Adults | Back | Blackheads