Yes, acne can develop after stopping antidepressants, and it catches many people off guard. The connection is rooted in hormonal rebalancing, shifts in serotonin availability, and changes in sebaceous gland activity that occur when your body adjusts to functioning without medication it has relied on for weeks, months, or even years. While no large-scale clinical trial has specifically studied post-SSRI acne as a primary endpoint, evidence from case reports, dermatological reviews, and patient-reported experiences confirms that this is a real phenomenon affecting a meaningful subset of people who discontinue these medications. The frustrating part is that the relationship between antidepressants and acne runs in both directions.
Some people develop acneiform eruptions while taking SSRIs, while others experience clear skin on medication only to break out after stopping. A published case in The Journal of Neuropsychiatry and Clinical Neurosciences documented sertraline-induced acne that disappeared within five days of discontinuation, illustrating just how directly these drugs can influence skin. But the reverse scenario, where skin worsens after stopping, is equally documented in clinical literature and patient forums. This article breaks down why post-antidepressant acne happens, which medications are most commonly implicated, what the science says about the gut-skin-brain axis and hormonal shifts during discontinuation, and what practical steps you can take to manage breakouts during the transition period.
Table of Contents
- Why Does Acne Flare Up After Stopping Antidepressants?
- The Hormonal Rebalancing Window and What It Means for Your Skin
- The Gut-Skin-Brain Axis and Post-SSRI Breakouts
- Which Antidepressants Are Most Likely to Cause Post-Discontinuation Acne?
- Why Gradual Tapering Matters for Your Skin
- Managing Post-Discontinuation Breakouts Without Overcorrecting
- What We Still Do Not Know and Where the Research Is Headed
- Conclusion
- Frequently Asked Questions
Why Does Acne Flare Up After Stopping Antidepressants?
The short answer involves hormones, inflammation, and your body’s serotonin system recalibrating in real time. SSRIs can alter androgen and cortisol levels during use, and when you stop taking them, the body’s hormonal equilibrium shifts as it works to restore baseline function. Androgens stimulate sebaceous gland activity and increase sebum production, which is one of the primary drivers of acne. During the readjustment period after discontinuation, androgen levels may temporarily spike or fluctuate unpredictably, triggering breakouts that seem to come out of nowhere. There is also a serotonin component that operates at the skin level. Lowered serotonin availability after stopping SSRIs can weaken the skin barrier by affecting cortisol regulation and upregulating pro-inflammatory cytokines.
This creates a one-two punch: more oil production from hormonal shifts combined with a compromised skin barrier that is less able to manage bacteria and inflammation. Stress-induced androgen surges, which are common during the emotionally turbulent discontinuation period, further stimulate sebaceous gland activity. It is worth noting that approximately 15 percent of patients, roughly one in six or seven, experience antidepressant discontinuation symptoms after stopping medication taken for at least six weeks, according to a 2024 Lancet Psychiatry meta-analysis covering 21,002 patients across 79 studies. About one in 35 patients suffers severe discontinuation symptoms. The commonly catalogued symptoms include flu-like feelings, insomnia, nausea, dizziness, and sensory disturbances like brain zaps. Skin-specific symptoms are less commonly tracked in the literature, which means post-discontinuation acne may be underreported.
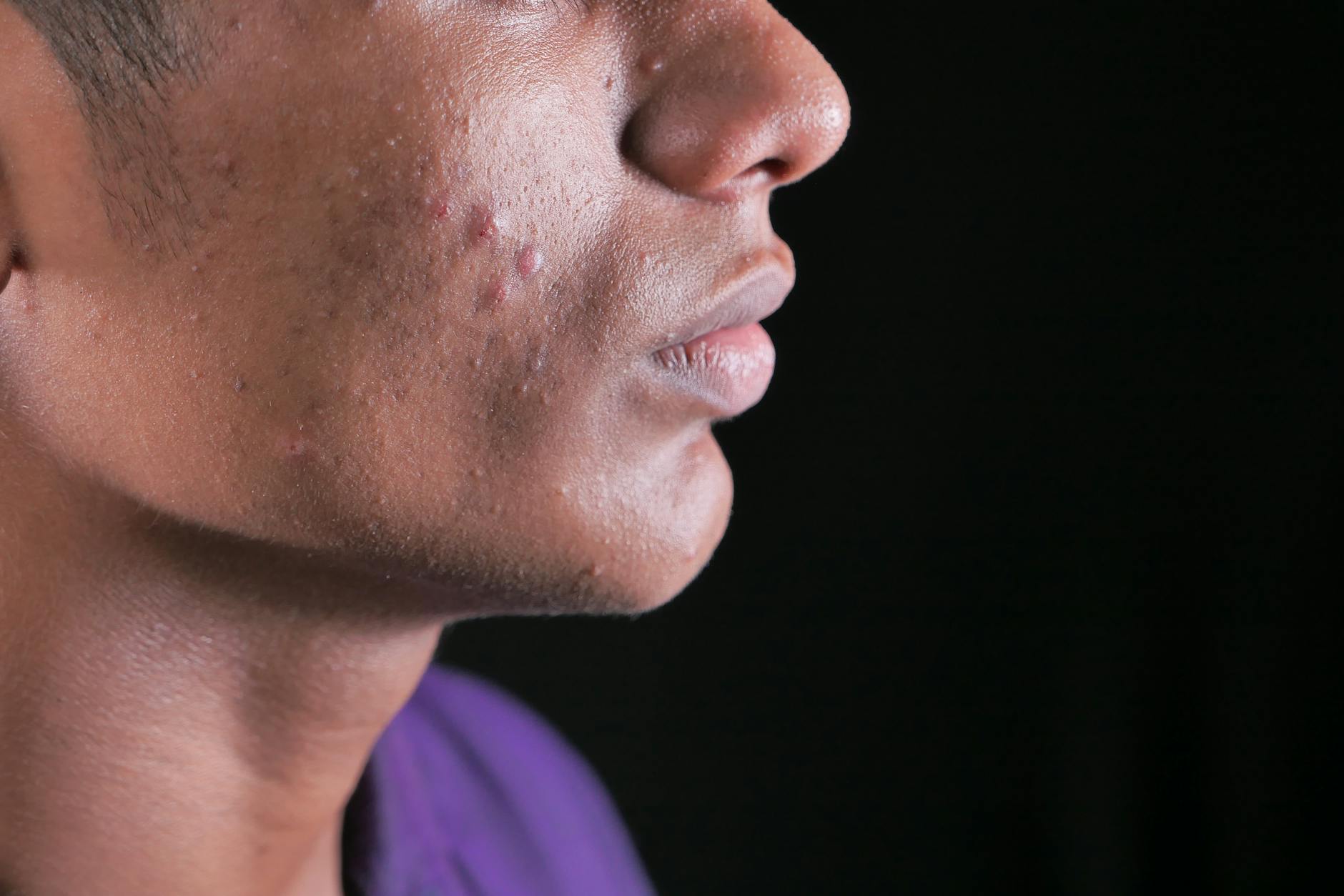
The Hormonal Rebalancing Window and What It Means for Your Skin
When you stop an SSRI, your body does not snap back to its pre-medication state overnight. The hormonal rebalancing process can take weeks to months, and during this window, your skin may behave in ways it never has before. People who never had acne-prone skin might suddenly develop cystic breakouts along the jawline and chin, areas heavily influenced by hormonal fluctuations. Others might notice increased oiliness across the T-zone before any visible breakouts appear. The timeline varies significantly from person to person. Some individuals report breakouts starting within the first week of discontinuation, while others do not see skin changes until several weeks later.
This variability makes it difficult to draw a straight line between stopping medication and the onset of acne, which is one reason the connection is underrecognized in clinical settings. If your dermatologist is not aware that you recently stopped an antidepressant, they may treat the acne as a standalone condition without addressing the underlying hormonal trigger. However, if you were already acne-prone before starting antidepressants, the picture gets more complicated. Some SSRIs may have been incidentally suppressing breakouts through their effects on hormones and inflammation, and stopping them essentially removes that unintentional benefit. In this case, what feels like new acne may actually be a return to your pre-medication baseline. This distinction matters because the treatment approach differs: temporary post-discontinuation acne may resolve on its own, while a return to chronic acne likely requires a longer-term skincare strategy.
The Gut-Skin-Brain Axis and Post-SSRI Breakouts
One of the more compelling explanations for post-antidepressant acne involves a system that most people do not think about when they look in the mirror: the gut. Approximately 95 percent of the body’s serotonin is produced in the gut, not the brain. When SSRIs are discontinued and serotonin availability changes, it can disrupt gut microbiome balance. This disruption is linked to inflammatory skin conditions including acne through what researchers call the gut-skin-brain axis. The mechanism works something like this. SSRIs increase serotonin availability throughout the body, including the gut. When you stop taking them, the sudden reduction in serotonin signaling can alter gut motility, change the composition of gut bacteria, and increase intestinal permeability.
These gut changes trigger systemic inflammation that manifests, among other places, on the skin. It is the same pathway that explains why people under extreme psychological stress often break out: the brain, gut, and skin are in constant communication. A specific example illustrates this connection. Consider someone who has been on escitalopram for two years with clear skin throughout. Within three weeks of tapering off, they develop inflammatory papules across the cheeks and forehead. Their diet has not changed, their skincare routine is the same, and they have not introduced any new products. The variable is the medication change, and the pathway likely runs through disrupted serotonin signaling in the gut triggering an inflammatory cascade that reaches the skin.

Which Antidepressants Are Most Likely to Cause Post-Discontinuation Acne?
Not all antidepressants carry equal risk for skin-related side effects, either during use or after stopping. SSRIs as a class are documented to produce a variety of cutaneous reactions including pruritus, urticaria, bruising, erythema multiforme, alopecia, and acneiform eruptions. But within the SSRI class, certain medications appear more frequently in case reports and patient forums. Sertraline, sold as Zoloft, has documented case reports of acneiform eruptions during use, and acne is recognized as an uncommon side effect.
The fact that sertraline-induced acne has been shown to resolve within days of stopping the drug suggests a direct pharmacological link rather than a coincidental association. Escitalopram, marketed as Lexapro, shows up in both clinical and patient-reported accounts of acne during use and acne after withdrawal, with responses varying considerably between individuals. The tradeoff is worth considering: if you developed acne while on sertraline, stopping may clear your skin, but if your skin was clear on escitalopram, discontinuation might trigger new breakouts. SNRIs, tricyclics, and other antidepressant classes have their own skin-related side effect profiles, but the evidence base for post-discontinuation acne is most developed for SSRIs. If you are planning to switch medications rather than stop entirely, discussing the dermatological side effect profiles of different options with your prescriber could help you make a more informed choice.
Why Gradual Tapering Matters for Your Skin
Abruptly stopping antidepressants is generally discouraged for a list of reasons that includes the potential for skin reactions. Gradual tapering, rather than sudden cessation, is the recommended approach to minimize all discontinuation symptoms, including potential skin effects. The American Academy of Family Physicians recommends a structured tapering schedule to reduce the severity of withdrawal symptoms across all body systems. The logic is straightforward. A slow taper gives your hormonal system, serotonin pathways, and gut microbiome time to adjust incrementally rather than being forced into a sudden recalibration.
Think of it as the difference between easing into cold water versus jumping in: the physiological shock is less severe when the change is gradual. For skin specifically, this means the hormonal fluctuations that drive sebum overproduction and inflammation are dampened, reducing the likelihood of a dramatic breakout. A limitation of this advice is that tapering does not guarantee you will avoid skin changes entirely. Some people taper perfectly over months and still develop acne once they reach zero. The taper reduces the severity and abruptness of hormonal shifts but cannot eliminate them altogether. If you are someone whose skin is particularly sensitive to hormonal fluctuations, as many people with a history of hormonal acne are, you may need to pair your tapering schedule with proactive skincare adjustments.

Managing Post-Discontinuation Breakouts Without Overcorrecting
The temptation when acne suddenly appears after stopping antidepressants is to throw everything at it: new cleansers, acids, retinoids, spot treatments, and complete routine overhauls. This is almost always counterproductive. Your skin barrier is already under stress from internal hormonal shifts, and layering on aggressive actives can worsen inflammation and prolong the breakout period.
A more measured approach involves keeping your existing routine stable, adding one targeted active ingredient at a time, and giving your skin four to six weeks to adjust before evaluating results. Ingredients that address the specific drivers of post-discontinuation acne, namely excess sebum, inflammation, and barrier compromise, include niacinamide for oil regulation, salicylic acid for pore clearance, and ceramides for barrier repair. If breakouts persist beyond three months or are severe and cystic, that is the point to see a dermatologist who can evaluate whether prescription intervention is warranted.
What We Still Do Not Know and Where the Research Is Headed
The honest reality is that post-antidepressant acne remains an understudied phenomenon. The evidence we have comes from case reports, dermatological reviews, and patient-reported experiences rather than controlled clinical trials designed to measure this specific outcome. Individual variation is significant, and there is no way to predict with certainty who will develop skin issues after stopping medication and who will not.
What seems increasingly clear is that the relationship between psychiatric medication and skin health deserves more formal investigation. As the gut-skin-brain axis gains traction as a research framework, future studies may be better equipped to map the specific pathways through which SSRI discontinuation affects the skin. Until then, the best approach is informed awareness: knowing that this can happen, understanding the likely mechanisms, and having a plan in place before you begin tapering.
Conclusion
Acne after stopping antidepressants is a legitimate, if underrecognized, consequence of the hormonal and neurochemical shifts that occur during discontinuation. The mechanisms are multifaceted, involving androgen fluctuations, serotonin-mediated changes in skin barrier function, and gut microbiome disruption through the gut-skin-brain axis. SSRIs like sertraline and escitalopram appear most frequently in reports, though individual responses vary widely.
The practical takeaways are to taper gradually under medical supervision, resist the urge to overhaul your skincare routine all at once, and give your body time to recalibrate. If breakouts are severe or persist beyond a few months, consult a dermatologist who understands the medication context. Post-discontinuation acne is usually temporary, but managing it well requires patience and a targeted approach rather than panic-driven product shopping.
Frequently Asked Questions
How long does acne last after stopping antidepressants?
There is no single timeline. Some people see breakouts resolve within a few weeks as hormones stabilize, while others experience skin changes for several months. If acne persists beyond three months, it may reflect a return to a pre-medication baseline rather than a temporary discontinuation effect, and professional evaluation is warranted.
Can I prevent acne when tapering off SSRIs?
Gradual tapering reduces the severity of all discontinuation symptoms, including potential skin effects, but it cannot guarantee breakout-free skin. Pairing a slow taper with a consistent, gentle skincare routine that includes oil-regulating and anti-inflammatory ingredients gives you the best chance.
Does everyone get acne after stopping antidepressants?
No. Individual variation is significant. Some people develop acne while on SSRIs, others develop it after stopping, and many experience no skin changes at all in either direction. There is no universal response, and predicting your outcome in advance is not currently possible.
Should I tell my dermatologist that I recently stopped an antidepressant?
Absolutely. Medication changes are relevant medical history for any dermatological evaluation. Knowing that you recently discontinued an SSRI can help your dermatologist distinguish between temporary hormonal acne and other conditions that require different treatment approaches.
Is post-antidepressant acne different from regular hormonal acne?
The underlying drivers overlap, particularly the role of androgens and sebum production, but the trigger is different. Post-discontinuation acne is specifically precipitated by the withdrawal of a medication that was influencing your hormonal and serotonin systems. The breakout pattern may resemble hormonal acne, often concentrated along the jawline and chin, but the treatment timeline may differ because the trigger is time-limited.
You Might Also Like
- Acne After Stopping Anticonvulsants
- Acne After Stopping Antibiotics
- Acne After Stopping ADHD Medication
Browse more: Acne | Acne Scars | Adults | Back | Blackheads





