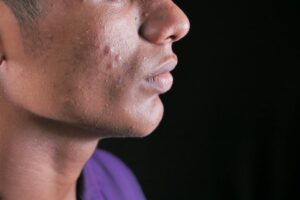
Tretinoin is the stronger, more potent retinoid—it’s the only FDA-approved retinoid for treating photoaging and wrinkles, backed by over 50 years of research supporting long-term safety and efficacy. But adapalene, while technically less powerful, is significantly better tolerated by most people’s skin. If you’re deciding between these two prescription-strength retinoids, the answer depends on your skin’s tolerance threshold and your primary goal: adapalene wins for gentler treatment with comparable acne results, while tretinoin wins for maximum anti-aging power and wrinkle reversal.
Both medications are effective retinoids that produce complete clearance or marked improvement in over 70% of acne patients after just eight weeks of treatment. The key difference isn’t whether they work—it’s how much irritation you’ll endure getting there. A patient starting tretinoin 0.025% might experience weeks of burning, peeling, and redness that forces them to stop, while someone on adapalene 0.1% achieves nearly identical acne results with minimal discomfort. For many people, the retinoid you’ll actually use consistently beats the theoretically stronger one you abandon after two weeks.
Table of Contents
- Which Retinoid Is Truly Stronger—Tretinoin or Adapalene?
- Why Adapalene Is Better Tolerated—The Clinical Evidence
- Side Effects and Safety—What to Actually Expect
- Which Retinoid Should You Choose—A Practical Comparison
- Managing Retinization and Irritation—Common Mistakes
- Timeline and Expected Results—When to Expect Improvement
- The Future of Retinoid Therapy—Beyond Tretinoin and Adapalene
- Conclusion
Which Retinoid Is Truly Stronger—Tretinoin or Adapalene?
Tretinoin is objectively the more potent retinoid. It’s a first-generation retinoid that binds directly to retinoic acid receptors in your skin with greater affinity than adapalene, which is a third-generation retinoid that requires metabolic conversion. This molecular difference translates to tretinoin being particularly effective for photoaging damage—sun damage, deep wrinkles, and loss of skin elasticity—making it the gold standard dermatologists reach for when patients need serious anti-aging results. Adapalene, by comparison, excels at acne and mild photoaging but isn’t the first choice for deep wrinkles or severe sun damage. When researchers compared adapalene 0.1% gel directly against tretinoin 0.025% gel in clinical trials, adapalene demonstrated comparable efficacy with actually faster onset of action on both inflammatory lesions and total lesion reduction.
This means that while tretinoin is theoretically stronger, adapalene achieves acne results equally well and sometimes more quickly. For someone treating acne—the most common use case—the difference in raw strength doesn’t matter much; what matters is what your skin can tolerate. The strength advantage becomes meaningful only for specific concerns. If your goal is reversing significant photoaging or deep wrinkles accumulated from decades of sun exposure, tretinoin’s superior potency justifies its harsher side effects. If your goal is clearing acne, adapalene’s comparable efficacy makes it the sensible choice because you’ll have fewer barriers to consistent use.

Why Adapalene Is Better Tolerated—The Clinical Evidence
Adapalene’s tolerability advantage is substantial and well-documented. In head-to-head clinical trials, adapalene gel produced significantly fewer adverse reactions overall: only 5.1% of patients (15 out of 296) experienced adverse events, compared to 9.1% of tretinoin patients (27 out of 295). That’s nearly a 40% lower rate of problems. Discontinuation rates due to side effects tell the same story: approximately 1.3% of adapalene users stopped treatment because of adverse reactions, versus 2.4% for tretinoin—roughly twice as likely to quit tretinoin. The difference comes down to irritation severity. Clinical studies consistently found that redness, dryness, and burning were more common and more severe in tretinoin groups compared to adapalene groups.
Tretinoin’s mechanism—its direct activation of retinoic acid receptors—produces a more aggressive inflammatory response initially, while adapalene’s gentler pathway allows most skin to acclimate without intense discomfort. For someone with sensitive skin or a history of irritation from other actives, adapalene is substantially less likely to trigger the kind of persistent redness that makes daily life uncomfortable. However, better tolerance doesn’t mean no irritation. Both medications cause dryness, peeling, and temporary sensitivity. The real-world implication: adapalene might cause mild dryness and occasional flaking, while tretinoin might cause severe peeling, burning sensations, and weeks of pronounced redness. That difference determines whether treatment is sustainable.
Side Effects and Safety—What to Actually Expect
Both tretinoin and adapalene share the same constellation of side effects because they’re both retinoids: dryness, redness, peeling, burning, and irritation are common to both. The difference is frequency and severity. With adapalene, you might experience manageable dryness that responds well to a good moisturizer. With tretinoin, that dryness might be severe enough to cause visible flaking and require prescription-strength moisturizers or occlusive treatments. Both medications increase sun sensitivity significantly, making SPF 30+ sunscreen non-negotiable year-round. This isn’t a minor precaution—retinoids thin the outer layer of skin slightly and increase photosensitivity, meaning your skin burns more easily and ages faster if exposed to UV without protection. Someone using tretinoin for anti-aging who skips sunscreen is essentially undermining their treatment.
The same applies to adapalene; both retinoids require the same sun protection discipline. One underappreciated side effect: retinization. Both drugs cause an initial “retinization period” where irritation and dryness peak before improving. With adapalene, this might last 2-4 weeks. With tretinoin, it can extend 6-8 weeks or longer. Patients often interpret this as the medication not working or their skin rejecting it, when actually it’s just the normal adjustment period. Understanding this prevents premature discontinuation.

Which Retinoid Should You Choose—A Practical Comparison
Your choice between tretinoin and adapalene should hinge on three factors: your skin’s sensitivity, your primary treatment goal, and whether you can commit to consistent use. Choose adapalene if: you have sensitive skin, you’re treating acne as your primary concern, you want the fastest path to results with minimal discomfort, or you prefer starting with an over-the-counter option. Adapalene (Differin brand) is available without a prescription, making it the more accessible entry point to prescription-strength retinoid treatment. You’ll achieve excellent acne results in 8-12 weeks with less irritation and a much lower risk of abandoning treatment.
Choose tretinoin if: your primary goal is treating photoaging and wrinkles, you have relatively resilient skin with a history of tolerating strong actives well, or you’re willing to manage intense initial irritation for maximum long-term anti-aging benefits. Tretinoin requires a prescription and should be obtained through a dermatologist or legitimate telehealth service, but it’s your best option if you’re serious about reversing sun damage. The practical reality: most people starting retinoid treatment will have better outcomes with adapalene because they’ll actually stick with it. Better to use adapalene consistently for a year than to try tretinoin for three weeks, experience unbearable irritation, and quit entirely.
Managing Retinization and Irritation—Common Mistakes
The biggest mistake people make with both medications is using too much, too soon. Tretinoin and adapalene should both start at the lowest available concentration (tretinoin 0.025%, adapalene 0.1%) and be used just 2-3 times per week initially. Many patients apply nightly from day one expecting faster results and instead trigger such severe irritation that they stop treatment. Slow introduction—gradually increasing frequency from twice weekly to every other night to nightly over 4-8 weeks—produces better long-term outcomes. Another common error is inadequate moisturization. Both retinoids require a robust moisturizing routine.
Use a good moisturizer immediately after applying the retinoid (apply tretinoin or adapalene to clean, dry skin, wait 20 minutes, then moisturize). Some people also benefit from the “sandwich method”: apply moisturizer first, then retinoid, then moisturizer again. This reduces irritation without significantly compromising efficacy. If you’re experiencing persistent burning or severe dryness, your moisturizer probably isn’t adequate—upgrade to a heavier cream. The final warning: never use tretinoin or adapalene while pregnant or trying to become pregnant. Tretinoin is a Category X medication (contraindicated in pregnancy), and adapalene is Category C (avoid unless benefits clearly outweigh risks). Both are only safe for non-pregnant skin.

Timeline and Expected Results—When to Expect Improvement
For acne, both medications follow similar timelines. You’ll likely notice initial irritation within the first week—redness, dryness, mild burning. By week 2-3, retinization peaks, and irritation is at its worst. By week 4-6, most people see their skin starting to adjust, irritation declining, and early signs of improvement (fewer new breakouts, existing lesions healing faster).
Complete results typically appear by week 8-12, at which point you’ll see that 70%+ clearance or marked improvement the clinical data promises. For wrinkles and photoaging, tretinoin has a longer timeline. Fine lines might improve slightly after 8-12 weeks, but significant improvements in deep wrinkles and skin texture take 3-6 months of consistent use. This is why tretinoin is a long-term commitment—you’re not treating an acute problem like acne; you’re slowly remodeling photodamaged skin over months. Adapalene produces mild improvements in mild photoaging but isn’t the right tool for severe sun damage.
The Future of Retinoid Therapy—Beyond Tretinoin and Adapalene
While tretinoin remains the gold standard for anti-aging and adapalene leads in tolerability, newer retinoids continue to emerge. Tazarotene is more potent than tretinoin but also more irritating. Retinol and retinyl palmitate are weaker options available over-the-counter.
For most people, the choice remains between tretinoin and adapalene because they occupy the optimal balance of efficacy, safety, and accessibility. The trend in dermatology is moving toward combination therapy—pairing retinoids with other actives like vitamin C, niacinamide, or azelaic acid to enhance results and manage irritation. Someone on tretinoin might benefit from niacinamide to reduce irritation, while someone on adapalene might add azelaic acid for enhanced anti-inflammatory acne results. The future isn’t one retinoid ruling all; it’s strategic combinations tailored to your specific skin needs.
Conclusion
Tretinoin is the stronger, more powerful retinoid with superior anti-aging credentials and five decades of research backing its long-term safety. Adapalene is the better-tolerated alternative that achieves comparable acne results with significantly fewer adverse effects and a lower discontinuation rate. Neither is objectively “better”—the right choice depends on your goals, your skin’s sensitivity, and your ability to tolerate the retinization process.
If you’re starting retinoid treatment, consider adapalene first. It’s accessible (available over-the-counter), effective (70%+ clearance in 8 weeks), and manageable for most skin types. If you’re treating significant photoaging or deep wrinkles and your skin can handle it, tretinoin is worth the irritation. Either way, the most important factor isn’t which retinoid you choose—it’s that you start low, go slow, protect yourself from the sun religiously, and commit to consistent use for at least 12 weeks before evaluating results.
You Might Also Like
- Medspa Microneedling Costs $800/Session…Dermatologist RF Microneedling Costs $1,200 but More Effective
- Spa Facial With Extractions Costs $250…Dermatologist Extraction Session Costs $150 With Better Results
- Insurance Denied Coverage for Photodynamic Therapy Costing $700 Per Month…FDA-Approved for Acne but Insurance Rarely Covers It
Browse more: Acne | Acne Scars | Adults | Back | Blackheads