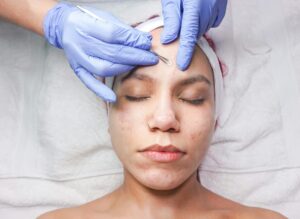
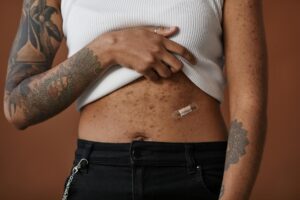
Stress and acne are deeply intertwined, though the exact percentage of adults who identify stress as their primary breakout trigger varies across research populations. What we do know from rigorous medical studies is that stress is a consistent and significant factor in acne development. A comprehensive study of acne patients across 17 Korean hospitals found that 82% reported psychological stress as the main triggering factor for their breakouts. Similarly, research among medical students—a notably stressed population—showed that 67-74% identified stress and anxiety as significant exacerbating factors.
These numbers tell us that while the specific 53% figure may not appear in peer-reviewed literature, the core truth is undeniable: stress is one of the most commonly reported acne triggers among adults. The connection between stress and breakouts isn’t purely psychological or anecdotal. When you experience stress, your body releases cortisol and corticotropin-releasing hormone (CRH), which increases oil production at the skin level and can trigger or worsen acne. Consider a common scenario: a person faces a major work deadline or personal crisis, experiences several days of heightened stress, and within days or a week, new breakouts appear on their chin, jawline, or forehead. This pattern repeats so consistently that dermatologists now recognize stress-induced acne as a distinct clinical phenomenon worthy of targeted treatment.
Table of Contents
- Why Is Stress One of the Most Commonly Cited Acne Triggers?
- How Stress Affects Acne Development and Severity
- Real-World Examples of Stress-Triggered Acne Patterns
- Managing Stress-Related Acne: A Multi-Pronged Approach
- Common Misconceptions and Advanced Considerations
- The Psychological Impact of Stress-Induced Acne
- The Future of Stress-Acne Research and Treatment
- Conclusion
- Frequently Asked Questions
Why Is Stress One of the Most Commonly Cited Acne Triggers?
When you’re under stress, your body enters a state of heightened alert. The adrenal glands pump out cortisol and adrenaline, preparing you for the “fight or flight” response. At the skin level, this hormonal cascade has specific consequences: sebaceous glands (which produce oil, or sebum) become more active, your skin barrier may weaken, and inflammatory pathways become more reactive. The 82% figure from the Korean study suggests that stress-related hormonal changes affect the majority of acne sufferers, making it as relevant as bacteria and genetics in the acne equation. The reason stress ranks so highly as a trigger is partly physiological and partly practical.
Unlike genetic predisposition, which you cannot change, or bacterial colonization, which requires specific treatments, stress is something many people recognize they can influence. A person might not know their acne is partly hereditary, but they absolutely notice that their skin flares when they’re anxious or overwhelmed. This lived experience—what dermatologists call “patient-reported triggers”—places stress consistently at the top of the list in surveys. However, it’s important to note that the severity of stress-induced acne varies dramatically between individuals. Some people experience minor breakouts during stressful periods, while others develop severe inflammatory acne that can last weeks.

How Stress Affects Acne Development and Severity
The biochemical pathway from stress to acne is well-documented. Cortisol increases sebum production, particularly in oil-prone zones like the T-zone. Simultaneously, stress impairs the skin’s barrier function and alters the balance of beneficial microbes on your skin’s surface. This creates an ideal environment for Cutibacterium acnes (formerly called Propionibacterium acnes) to proliferate. The result is not just excess oil, but also increased bacterial colonization and inflammation—the perfect storm for breakouts.
One important limitation to recognize is that stress doesn’t trigger acne uniformly across the population. A 2023 Nature Scientific Reports study examining the stress-acne correlation found moderate statistical associations (r=0.23-0.758, p<0.01), meaning that while the relationship is statistically significant, stress alone does not predict acne breakouts with complete accuracy. Some people under intense stress have clear skin, while others with minor life stressors experience severe acne. This variation depends on genetics, baseline sebum production, skin microbiome composition, and existing acne-prone conditions like polycystic ovary syndrome (PCOS) or hormonal imbalances. Additionally, the time delay between a stressful event and a visible breakout is not instantaneous—it typically takes 24-72 hours for stress hormones to trigger noticeable skin changes, which can make the cause-and-effect relationship seem unclear.
Real-World Examples of Stress-Triggered Acne Patterns
Consider the medical student who clears their skin during summer break, then within a week of returning to classes, develops a cluster of inflammatory papules on their cheeks and forehead. This pattern repeats every semester. The 67-74% of medical students in JAMA Dermatology research who reported stress as a significant acne factor experienced exactly this phenomenon. The stress is quantifiable—exams, long hours, sleep deprivation—and the skin response is visible and reproducible.
Another common scenario involves professionals during high-pressure work periods. A manager faces a major project launch, works 12-hour days, sleeps poorly, and skips their usual skincare routine. Within days, they notice new breakouts clustered around the jawline and chin—areas rich in sebaceous glands and sensitive to hormonal fluctuations. The stress itself triggers the acne, and the psychological impact compounds the problem: seeing new blemishes increases anxiety, which further elevates cortisol, creating a vicious cycle. A 2024 Cutera survey found that 90% of acne sufferers experience daily insecurities related to their acne, meaning that stress-triggered breakouts don’t just affect the skin—they amplify emotional distress, which then worsens the acne further.

Managing Stress-Related Acne: A Multi-Pronged Approach
The most effective strategy for stress-related acne addresses both the stress and the skin simultaneously. Stress-reduction techniques like meditation, exercise, or therapy can help lower cortisol levels, but results vary widely. A person who practices yoga three times per week may see skin improvement, while someone who meditates daily might see no change if their acne is driven primarily by genetics or bacterial overgrowth. The key is consistency and patience—most skin changes take 4-8 weeks to become visible after a behavioral change.
Concurrently, topical acne treatments become more important when stress is a known trigger. Retinoids, benzoyl peroxide, and salicylic acid work regardless of cortisol levels, while stress reduction works only if stress is actually driving the breakouts. This is the practical tradeoff: you can address stress through lifestyle changes, but you often need pharmaceutical support to clear existing acne while you’re managing stress. For some people, combining a stress-management strategy with a dermatologist-prescribed treatment (such as prescription retinoids or even oral antibiotics for severe stress-triggered acne) produces the fastest and most reliable results.
Common Misconceptions and Advanced Considerations
One widespread misconception is that stress-related acne only affects people with an already acne-prone skin type. In reality, stress can trigger breakouts in people who otherwise have clear skin, particularly if they experience sudden, severe stress. However, there’s a caveat: the acne triggered by stress tends to be milder in people with naturally resilient skin and more severe in those with genetic predisposition to acne. A person with no family history of acne might develop a few breakouts during a stressful month and then clear up once the stress resolves. Someone with a family history might develop persistent, severe acne from the same stressor.
Another advanced consideration involves the interaction between stress, hormones, and gender. People who menstruate often notice that stress exacerbates pre-menstrual acne flares. During the luteal phase of the menstrual cycle, cortisol levels are already elevated, and additional psychological stress compounds this hormonal imbalance. Women and people with female-typical hormones may find that stress management becomes particularly important during the week before their period. Additionally, those with PCOS or other hormonal conditions should be aware that stress-triggered oil production can significantly worsen their acne during high-stress periods.

The Psychological Impact of Stress-Induced Acne
The relationship between stress and acne is bidirectional: stress causes acne, and acne causes stress. The visible nature of acne means that stress-triggered breakouts often generate shame, anxiety, and social withdrawal—emotions that further elevate cortisol and perpetuate the cycle. An adult experiencing stress-related breakouts might avoid social situations or work meetings, which increases isolation and mental stress, which worsens the acne.
This psychological component is significant enough that some dermatologists now recommend counseling or therapy alongside acne treatment when stress is a clear trigger. A person who learns coping strategies for stress may see skin improvement without any topical medication, while someone who only treats the skin topically without addressing stress may experience repeated breakouts. The most successful outcomes typically involve both the physical treatment of acne and the psychological management of stress.
The Future of Stress-Acne Research and Treatment
Emerging research is moving beyond simply confirming the stress-acne link to understanding individual variation in stress sensitivity. Future treatments may include biomarkers that predict who will experience severe stress-triggered acne, allowing for preventive treatment during foreseeable high-stress periods. Some researchers are also exploring whether certain types of stress management (meditation vs.
exercise vs. therapy) work better for stress-triggered acne than others—a question that current research hasn’t definitively answered. As our understanding of the skin microbiome advances, treatments may become more precise, targeting the specific bacterial and fungal changes that stress induces rather than broadly reducing oil production. This precision medicine approach could mean fewer side effects and faster acne resolution for stress-sensitive individuals.
Conclusion
While the exact percentage of adults who identify stress as their number one acne trigger may vary depending on the population studied, the evidence is clear: stress is a major and consistent trigger for acne in a substantial portion of the adult population. The 82% rate observed in a Korean hospital study and the 67-74% rate among medical students suggest that stress is at least as important as bacteria and possibly more important than many other controllable factors in acne development.
If you’ve noticed that your acne worsens during stressful periods, you’re not alone—and you have options. Work with a dermatologist to develop a treatment plan that addresses both the skin condition and your stress levels. Whether through topical treatments, stress management, lifestyle changes, or a combination of approaches, managing stress-related acne is achievable and worth the effort.
Frequently Asked Questions
How long does it take for stress-related acne to appear after a stressful event?
Most stress-triggered breakouts appear 24-72 hours after the stressful event, though some may take up to a week. This delay can make the connection between stress and acne less obvious than it actually is.
Does stress reduction alone clear stress-related acne?
Not always. While stress management can prevent new stress-triggered breakouts, existing acne often requires topical or oral treatment to resolve. A combination approach typically works best.
Is stress-related acne different from other types of acne?
Stress-related acne involves the same bacteria and inflammation as other acne, but the trigger is hormonal rather than genetic or bacterial. This distinction matters for treatment strategy.
Why does stress-triggered acne often appear on the chin and jawline?
These areas have a high concentration of sebaceous glands and are particularly sensitive to hormonal fluctuations triggered by cortisol and other stress hormones.
Can acne from stress be prevented?
Preventive treatment during foreseeable high-stress periods—such as increasing your skincare routine or starting a topical retinoid before exams or a major work project—can reduce the severity of stress-triggered breakouts, though complete prevention is difficult.
If I manage my stress, will my acne automatically clear?
Not necessarily. While stress management prevents new stress-triggered breakouts, existing acne may require additional treatment to fully resolve, particularly if genetics or bacterial overgrowth are also contributing factors.
You Might Also Like
- At Least 35% of People With Acne Scars Report That Scarring Has Affected Their Career Advancement
- At Least 78% of Adults Over 25 Are Surprised to Learn That Adult Acne Is More Common Than Teenage Acne in Women
- At Least 68% of Young Adults Admit to Picking at Their Acne Despite Knowing It Causes Scarring
Browse more: Acne | Acne Scars | Adults | Back | Blackheads