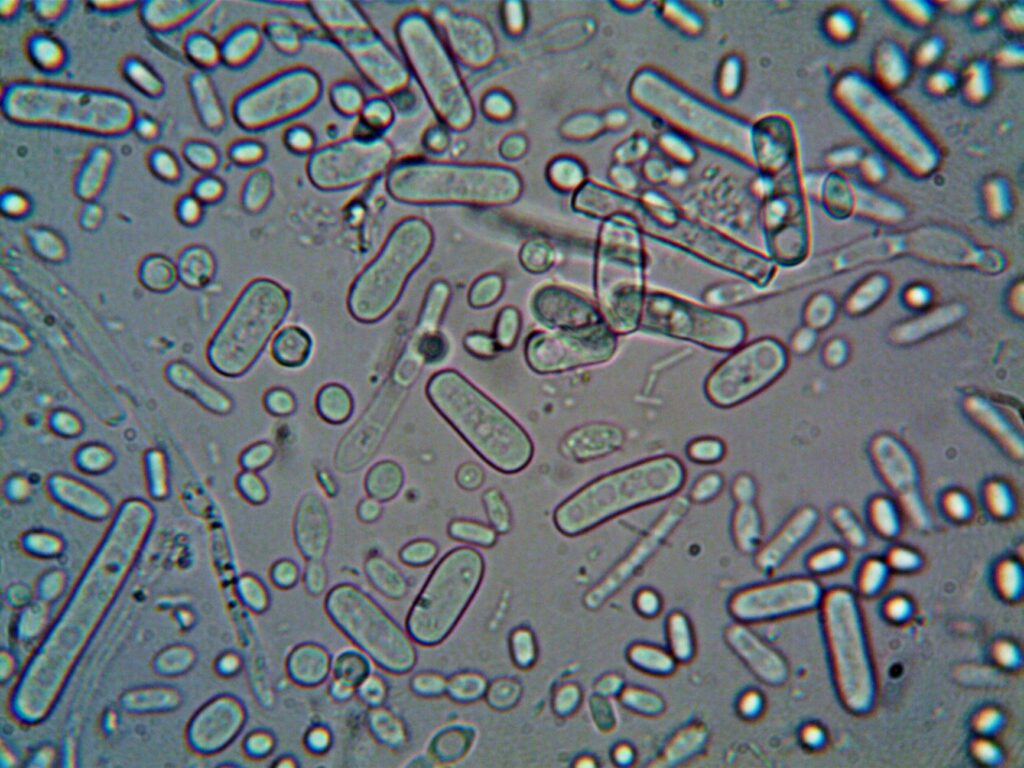
Bacterial culture testing reveals that antibiotic-resistant acne is no longer rare—it’s becoming the norm in clinical practice. When dermatologists culture bacteria from acne lesions and test sensitivity to antibiotics, they increasingly discover that *Cutibacterium acnes* (the primary acne bacterium) resists the very drugs patients have been prescribed. For example, clindamycin, once a reliable acne antibiotic, now shows resistance in roughly 31% of tested acne strains, a significant jump from the 25.5% resistance rate recorded in the early 2000s and 1980s. This shift means that a patient treated with clindamycin has a one-in-three chance their bacteria won’t respond to the medication—a sobering reality that culture testing makes impossible to ignore.
Culture testing also exposes multidrug resistance, where acne bacteria resist multiple antibiotics simultaneously. Recent research shows that nearly one-third (32.6%) of *C. acnes* strains isolated from acne patients display resistance to at least two antibiotics, and 9.3% resist multiple drug classes. These findings challenge the assumption that simply switching to a different antibiotic will solve treatment failure. This article explores what culture testing reveals about antibiotic resistance in acne, how resistance patterns vary globally, why resistance develops, and what dermatologists and patients should do about it.
Table of Contents
- How Bacterial Culture Testing Detects Antibiotic Resistance in Acne
- Rising Resistance to Clindamycin and Macrolides Over Time
- Geographic Variations Expose Antibiotic Overuse Patterns
- Multidrug Resistance Complicates Treatment Options
- How Prolonged Antibiotic Exposure Drives Resistance Development
- Requesting and Interpreting Culture Tests for Acne
- The Shift Toward Non-Antibiotic and Combination Approaches
- Conclusion
- Frequently Asked Questions
How Bacterial Culture Testing Detects Antibiotic Resistance in Acne
Bacterial culture testing for acne involves growing *Cutibacterium acnes* from a patient’s lesions under controlled laboratory conditions, then exposing the cultured bacteria to various antibiotics to determine which drugs kill the bacteria and which ones it resists. Laboratories use Mueller Hinton agar plates and incubate cultures anaerobically (without oxygen) at 37°C for 48 to 72 hours—replicating the anaerobic environment deep within acne lesions. Once bacteria are grown, sensitivity is measured using E-test strips or agar dilution methods that determine the Minimum Inhibitory Concentration (MIC), the lowest antibiotic concentration needed to stop bacterial growth.
The results guide treatment selection more accurately than empirical prescribing. Rather than starting with clindamycin “because it usually works,” culture results might reveal that a patient’s specific strain resists clindamycin but remains sensitive to doxycycline. However, culture testing is not routine in many dermatology practices because it requires specialized laboratory resources, takes several days to produce results, and isn’t covered by all insurance plans. Patients experiencing repeated treatment failure benefit most from testing, as it pinpoints which antibiotics their particular bacteria will respond to rather than wasting weeks on ineffective drugs.
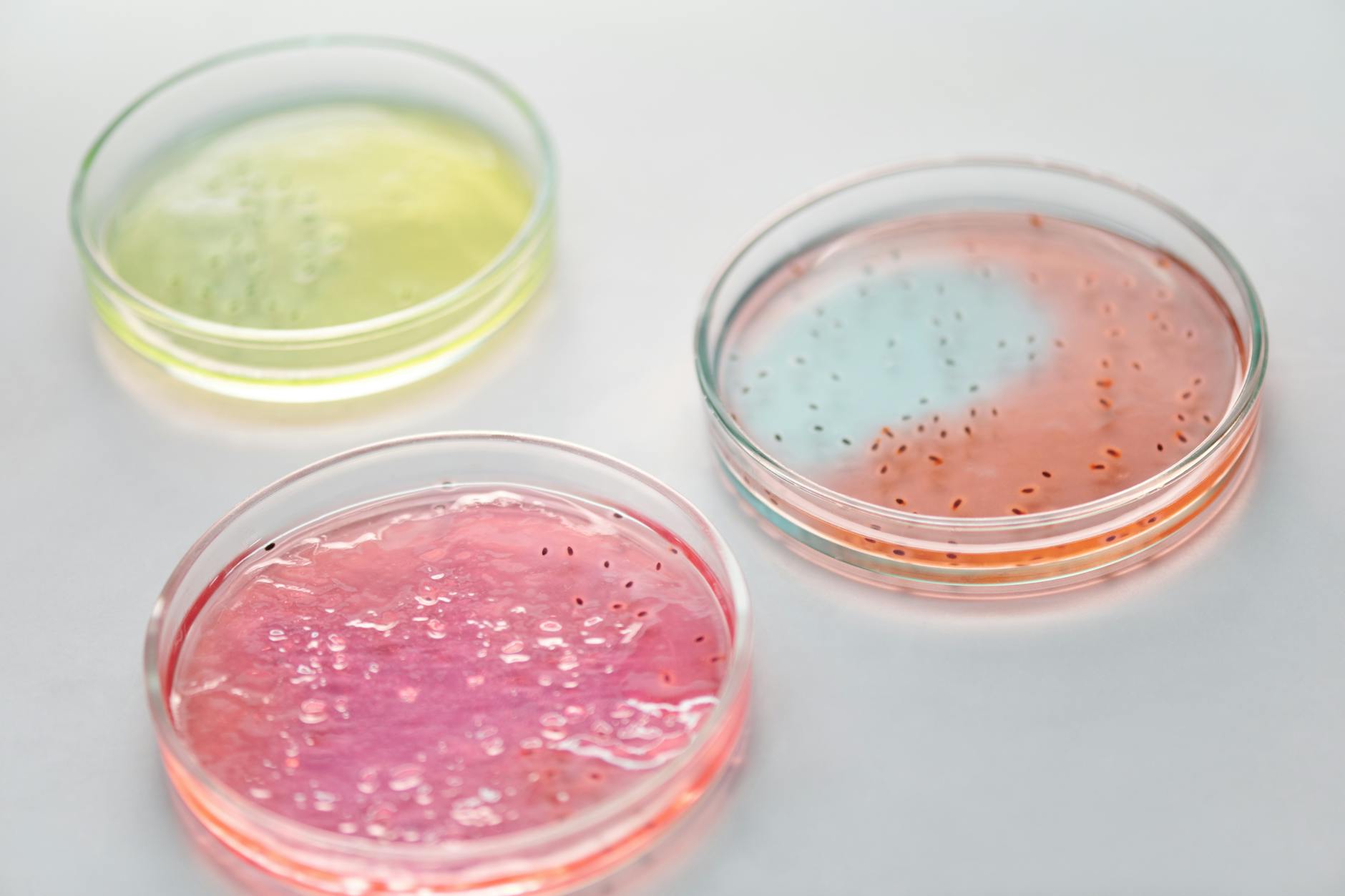
Rising Resistance to Clindamycin and Macrolides Over Time
The most striking trend revealed by culture testing is the dramatic rise in clindamycin resistance. A comprehensive 2025 systematic review analyzing 23 studies and 2,046 *C. acnes* isolates from 2005 to April 2025 found that clindamycin resistance increased from 25.5% (in studies covering 1983–2014) to 35.4% (in studies covering 2015–2023), though recent data suggest it’s stabilized around 31%. This pattern reflects decades of clindamycin overuse in acne treatment—when millions of patients take the same antibiotic, resistant bacteria multiply and spread, making the drug progressively less effective for everyone. Similarly, macrolide antibiotics like erythromycin and azithromycin show rising resistance over time, with statistically significant increases evident in the research literature (p < 0.05).
Individual studies report azithromycin resistance in roughly 18% of acne strains and clindamycin resistance ranging from 16% to 35% depending on the population sampled and time period studied. The silver lining is that tetracyclines—particularly doxycycline—remain highly effective, with resistance rates staying low at just 2.44%. This is why dermatologists increasingly recommend doxycycline as a first-line acne antibiotic rather than clindamycin, despite years of prescribing patterns favoring the latter. However, resistance can still emerge over time; data from prolonged antibiotic use shows that extended treatment beyond guideline-recommended durations correlates with higher tetracycline-resistant *C. acnes* prevalence, suggesting that even doxycycline could face resistance challenges if overused indefinitely.
Geographic Variations Expose Antibiotic Overuse Patterns
Culture testing data reveals dramatic geographic differences in antibiotic resistance, reflecting how acne is treated in different regions. In China, clarithromycin resistance reaches an alarming 77% (95% confidence interval: 62-87%), far exceeding resistance rates in North America and Europe. This disparity is directly attributed to widespread antibiotic overuse in acne treatment in China, where antibiotics have been prescribed more liberally for decades. A 2025 Bulgarian study examining 73 *C.
acnes* strains isolated from October 2017 through April 2025 (55 from acne patients and 18 from other sources) used standardized E-test strips and disk diffusion methods per EUCAST guidelines, revealing resistance patterns specific to that Eastern European population. These geographic variations are clinically important because they affect which antibiotics dermatologists can rely on in different parts of the world. A treatment regimen that works reliably in the United States may fail in regions where years of antibiotic overuse have produced resistant bacteria. For patients relocating internationally or seeking second opinions from dermatologists abroad, local resistance patterns matter. Culture testing becomes especially valuable in high-resistance regions, as empirical prescribing becomes increasingly unreliable when more than half of patient isolates resist first-line drugs.
Multidrug Resistance Complicates Treatment Options
Beyond single-antibiotic resistance, culture testing frequently detects multidrug resistance—bacteria that simultaneously resist multiple antibiotics or multiple drug classes. Recent research found that 32.6% of *C. acnes* strains from acne patients showed resistance to at least two antibiotics, while 9.3% displayed genuine multidrug resistance to representatives of different antibiotic classes. This pattern emerges because bacteria that survive exposure to one antibiotic often carry resistance genes to other drugs, either on the same genetic element or acquired over time.
Multidrug resistance narrows treatment options and sometimes forces dermatologists to use less conventional approaches, such as combining antibiotics with benzoyl peroxide (which bacteria cannot easily resist) or shifting to isotretinoin for severe cases. A patient whose culture reveals resistance to both clindamycin and azithromycin cannot simply alternate between the two drugs as a workaround; both are compromised. Culture testing is particularly valuable in these cases, as it identifies which antibiotics remain effective and which combinations might work synergistically. For patients with multidrug-resistant acne bacteria, culture results often reshape the entire treatment strategy away from antibiotics and toward alternative approaches like hormonal therapy, topical retinoids, or oral isotretinoin.
How Prolonged Antibiotic Exposure Drives Resistance Development
One of the most important findings from recent research is that prolonged antibiotic exposure directly correlates with increased antibiotic resistance in *C. acnes*. Prospective data collected from 2015 through 2026 shows that patients treated with antibiotics for longer than guideline-recommended durations (typically 3–6 months) develop higher rates of tetracycline-resistant bacteria. This occurs through a well-understood mechanism: every day a patient takes an antibiotic, susceptible bacteria die while any bacteria with even partial resistance mutations survive and multiply, gradually shifting the population toward resistance.
Current dermatologic guidelines recommend limiting antibiotic courses to the shortest effective duration and always combining antibiotics with benzoyl peroxide (which prevents resistance) and topical retinoids (which reduce bacterial colonization independently). Yet many patients and some dermatologists continue extended antibiotic courses, inadvertently accelerating resistance development. A patient prescribed doxycycline for acne with instructions to take it for 12 months is directly contributing to the creation of doxycycline-resistant bacteria—both in their own microbiome and, through transmission, in the broader population. Culture testing post-treatment sometimes reveals resistant strains that weren’t present initially, directly documenting this resistance development in real time.

Requesting and Interpreting Culture Tests for Acne
Not all acne patients need culture testing; many respond well to standard empirical treatment. However, patients with treatment-resistant acne, previous antibiotic failures, or cystic acne warrant culture testing to guide therapy. The test begins with a dermatologist collecting bacteria from an acne lesion using a sterile swab, sending it to a laboratory for culture and sensitivity determination. Results typically arrive within one week and report which antibiotics inhibit growth and which the patient’s bacteria resist.
Interpreting results requires understanding that “resistant” doesn’t mean a drug won’t help at all, but rather that standard doses are unlikely to be effective—higher doses might work but with increased side effects and toxicity risk. “Susceptible” means the drug should work at standard doses. Some laboratories also report intermediate susceptibility, meaning the drug might work but reliability is uncertain. Armed with these results, dermatologists can prescribe antibiotics their culture testing confirmed will work, or switch strategies entirely toward non-antibiotic treatments if resistance is widespread. Unfortunately, many insurance plans don’t cover culture testing unless treatment has already failed multiple times, creating a delay before patients and doctors have actionable information to guide care.
The Shift Toward Non-Antibiotic and Combination Approaches
As culture testing increasingly documents antibiotic resistance, dermatology is shifting toward regimens that minimize antibiotic dependence. Benzoyl peroxide, a topical oxidizing agent, works via a completely different mechanism—it generates reactive oxygen species that kill bacteria and is so chemically different from antibiotics that bacteria cannot easily develop resistance. When benzoyl peroxide is combined with antibiotics, resistance development slows dramatically. Similarly, topical and oral retinoids shrink sebaceous glands and reduce the microbial environment acne bacteria depend on, making them valuable partners to antibiotics or replacements when resistance is problematic.
For severe resistant acne, isotretinoin (Accutane) remains the definitive treatment, offering potential cure through permanent reduction of sebaceous gland activity and bacterial colonization. While isotretinoin carries serious side effects requiring careful monitoring, it’s increasingly positioned as the appropriate choice for patients with multidrug-resistant acne rather than cycling through ineffective antibiotics. Culture testing plays a crucial role in this decision-making: when results show widespread resistance, continuing antibiotic therapy becomes harder to justify, and dermatologists and patients can make informed decisions about escalating to more definitive treatments. The future of acne treatment likely involves culture-guided, antibiotic-sparing regimens that preserve antibiotic efficacy for acne and other infections where they’re truly essential.
Conclusion
Bacterial culture testing reveals an uncomfortable truth: antibiotic-resistant acne is widespread and growing. With clindamycin resistance now affecting roughly one in three acne strains, multidrug resistance complicating treatment options for many patients, and geographic hotspots like China seeing clarithromycin resistance above 75%, empirical prescribing is increasingly unreliable. Culture testing transforms acne treatment from guesswork into precision medicine by identifying which antibiotics each patient’s bacteria will actually respond to. The broader lesson from culture testing data is that antibiotic resistance is not a future problem—it’s present now, and it stems directly from years of overuse and prolonged courses.
Dermatologists and patients should view antibiotic prescriptions for acne as precious resources requiring careful stewardship, not first-line defaults. If you’ve experienced repeated antibiotic failures, ask your dermatologist about culture testing to guide your next treatment choice. If culture results reveal resistance or multidrug resistance, be prepared to shift strategies toward combination therapy, topical retinoids, or more definitive approaches. The data culture testing provides is too valuable to ignore.
Frequently Asked Questions
Does a positive culture test mean acne is contagious?
No. While bacterial culture identifies *Cutibacterium acnes*, this bacterium normally colonizes everyone’s skin. Positive culture only identifies what bacteria are present in your lesions; it doesn’t alter how contagious acne is (not contagious in the traditional sense).
Can culture testing identify which antibiotic will work best, or only which ones won’t?
Culture testing identifies both. Results report which antibiotics the bacteria are susceptible to (likely to respond) and which it resists. Your dermatologist can select from the susceptible options, or if all tested antibiotics show resistance, shift to non-antibiotic strategies.
How long does culture testing take, and why does it take so long?
Results typically arrive within 7 to 10 days because *Cutibacterium acnes* grows slowly, requiring 48 to 72 hours of incubation just for visible growth, followed by sensitivity testing and result reporting. This delay is why dermatologists often prescribe empirically first, then adjust if testing suggests a better option.
If my culture shows doxycycline sensitivity, does that mean I can take doxycycline indefinitely?
No. Even doxycycline can develop resistance with prolonged use, as recent data show. Guidelines recommend limiting antibiotic courses to 3 to 6 months when possible, always combining with benzoyl peroxide and topical retinoids to minimize resistance risk.
Why don’t all dermatologists order culture tests routinely?
Cost, laboratory availability, and insurance coverage are limiting factors. Culture testing isn’t routine because many patients respond to empirical treatment, and testing adds expense and delay. It’s most valuable for treatment-resistant cases or when treatment failures raise questions about resistance.
What should I do if culture testing reveals resistance to all common acne antibiotics?
Multidrug resistance warrants a shift away from antibiotics. Your dermatologist might recommend isotretinoin, hormonal therapy (for women), or aggressive combination therapy with benzoyl peroxide and topical retinoids. Culture results showing widespread resistance are actually valuable because they justify moving toward more definitive treatments.
You Might Also Like
- What UV Photography Reveals About Hidden Acne Damage
- What Mass Spectrometry of Sebum Reveals About Acne
- What Dermatoscopy Reveals About Acne Lesion Type
Browse more: Acne | Acne Scars | Adults | Back | Blackheads