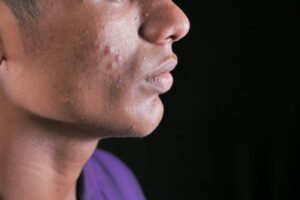
Your skin feels slick with oil, yet it’s simultaneously parched and breaking out. This isn’t a contradiction—it’s a skin barrier problem. Oil (sebum) and water play entirely different roles in maintaining healthy skin. You can produce excess sebum on the surface while your skin is severely dehydrated at the cellular level, a condition that’s clinically measurable and surprisingly common in acne-prone skin.
When your barrier is compromised, your skin loses water faster than it should, triggering a compensatory mechanism: your body ramps up oil production to try to seal in the remaining moisture. Meanwhile, the dehydration itself causes dead cells to accumulate, pores to become dysfunctional, and inflammation to spike—creating the perfect storm for breakouts. This article breaks down exactly why this happens, how a damaged barrier creates this oily-yet-dehydrated cycle, and what actually stops it. You’ll learn why your usual acne routine might be making it worse, how to identify true dehydration versus simple dryness, and the specific barrier-repair steps that address root cause instead of just treating surface symptoms.
Table of Contents
- How Can Skin Be Oily and Dehydrated at the Same Time?
- Why Does Dehydration Trigger Excess Oil Production?
- The Barrier Dysfunction Behind Trapped Pores and Breakouts
- Why Standard Acne Treatments Often Backfire
- Inflammation as the Hidden Driver of Persistent Breakouts
- The Role of Sebum Composition in Acne Development
- Recognizing Oily-Dehydrated Skin and Moving Forward
- Conclusion
How Can Skin Be Oily and Dehydrated at the Same Time?
The confusion starts with terminology. When dermatologists talk about dehydration, they’re measuring water content deep within your skin layers using biophysical parameters like transepidermal water loss (TEWL) and moisture levels—not whether your skin feels dry to the touch. Sebum production and hydration exist on completely separate tracks. You can have excessive oil on the surface while your stratum corneum (the outermost barrier layer) is losing water rapidly to the environment. In fact, acne patients show significantly elevated TEWL compared to non-acne skin, meaning water is escaping through a compromised barrier even as oil production remains high or even increases.
Think of it like a leaky roof covered in waterproofing sealer. The sealer is there (the excess oil), but the structure underneath is water-damaged (dehydrated). Your skin interprets this moisture loss as an emergency and responds by producing even more sebum, trying to compensate for the water that‘s escaping. This is why people with acne-prone skin often feel trapped: they’re oily enough that moisturizers seem unnecessary, yet their skin acts like it’s desperately thirsty. The barrier dysfunction means their skin is actually both—oily on the surface and parched underneath, because the lipid barrier isn’t functioning properly.
Why Does Dehydration Trigger Excess Oil Production?
your skin’s sebaceous glands are designed to produce oil that helps seal in moisture. When your barrier becomes compromised, moisture escapes through something called transepidermal water loss. Your skin detects this water loss and interprets it as a threat. In response, your sebaceous glands upregulate sebum production as a defensive mechanism—an attempt to create a thicker lipid seal to prevent further water loss. This is an involuntary response; you can’t willpower your way out of it.
The problem is that this compensatory sebum production doesn’t actually solve the underlying dehydration because the barrier damage remains. You end up in a cycle where excess oil production coexists with dehydration, and both drive acne. However, if you strip away that oil too aggressively with harsh cleansers or over-exfoliation, you’ll actually accelerate barrier damage and make the compensatory sebum response even stronger. This is why people who scrub their oily skin relentlessly often end up oilier and more breakout-prone after a few weeks. The barrier damage worsens, water loss increases, and sebum production goes into overdrive. Understanding this distinction changes everything about how you should treat the condition—you’re not trying to eliminate all the oil; you’re trying to repair the barrier so your skin stops desperately overproducing it.
The Barrier Dysfunction Behind Trapped Pores and Breakouts
A compromised skin barrier doesn’t just cause water loss—it also causes pores to become dysfunctional. When your barrier lacks the proper lipid composition, pores collapse and don’t lubricate properly. Oil becomes trapped alongside dead skin cells, forming comedones and trapped bacteria that lead to acne. Your skin naturally sheds about 30,000 to 40,000 dead cells per minute, but when your skin is dehydrated, that cell turnover slows significantly. Dead cells pile up inside pores instead of sloughing off cleanly.
Combined with trapped sebum, this creates an ideal environment for acne-causing bacteria to proliferate. Additionally, acne-prone skin produces sebum with abnormal lipid composition—it contains lower levels of linoleic acid and ceramide deficiencies. These are critical lipids that maintain barrier integrity and skin flexibility. Without them, your barrier becomes even more fragile, accelerating water loss and pore dysfunction. The inflammation that follows from this cascade of barrier impairment makes skin more sensitive and more prone to breakouts. Many people don’t realize they’re dealing with an inflammatory barrier problem; they think they just have “acne-prone skin,” when really they have a specific pattern of lipid insufficiency that needs targeted repair.

Why Standard Acne Treatments Often Backfire
Most traditional acne treatment approaches focus on drying out oil and killing bacteria—salicylic acid, benzoyl peroxide, isotretinoin. These work for some skin types, but for oily, dehydrated, barrier-compromised skin, they often worsen the underlying problem. When you strip away surface oil aggressively, your skin perceives even greater water loss and responds with even more sebum overproduction. You create a vicious cycle where the treatment itself is perpetuating the condition.
The trade-off is real: you can reduce acne temporarily with aggressive treatments, but you’ll likely deepen the barrier damage in the process. Within weeks or months, you’ll deal with rebound oiliness, increased sensitivity, and potentially worse breakouts. A barrier-repair approach—focusing on hydration, ceramides, and lipid restoration—takes longer to see results (typically 4-8 weeks), but it addresses root cause. The downside is that barrier repair requires patience and consistency, and some people get frustrated because active acne doesn’t clear as quickly as it might on harsher treatments. However, the breakouts that do emerge on a barrier-repair regimen are typically less severe and less frequent than the rebound acne from over-treated skin.
Inflammation as the Hidden Driver of Persistent Breakouts
A compromised skin barrier inherently triggers increased inflammation. When your barrier is damaged, inflammatory cytokines are released, your skin becomes more reactive, and pathogenic bacteria find easier access to deeper layers. This inflammation doesn’t just cause acne—it perpetuates it. Inflamed skin produces more sebum, heals more slowly, and is more likely to scar. If you have oily, dehydrated, breakout-prone skin, you’re almost certainly dealing with systemic barrier inflammation, not just localized acne.
A critical warning: if you’re using anti-inflammatory treatments like corticosteroids or strong retinoids on top of an already-damaged barrier, you might get short-term redness reduction but long-term barrier weakening. Retinoids especially can initially worsen dehydration and inflammation before they improve it, which is why the “retinization” period exists. During that window, your barrier is even more compromised. If you’re already oily and dehydrated, introducing a retinoid without proper barrier support is likely to create a temporary crisis before improvement. Time the introduction carefully and prioritize barrier repair first.

The Role of Sebum Composition in Acne Development
Not all sebum is created equal. Sebum from acne-prone skin has a distinctly different lipid profile than sebum from clear skin. Research shows acne sebum contains lower levels of linoleic acid, which is essential for barrier function, and deficient ceramides, which are the “mortar” between skin cells. This abnormal sebum composition means that even though you’re producing plenty of oil on the surface, the oil itself isn’t effective at maintaining barrier integrity.
It’s like having a waterproofing sealer that doesn’t actually waterproof. This explains why simply controlling oil production through diet, hormones, or topical treatments doesn’t always solve the problem. You can reduce sebum volume but still have a compromised barrier because the sebum that’s being produced is fundamentally altered. Someone with oily, acne-prone skin often needs to focus on lipid replacement (ceramides, cholesterol, free fatty acids) rather than pure oil reduction. A ceramide-rich moisturizer will do far more to improve their skin than another acne cleanser will.
Recognizing Oily-Dehydrated Skin and Moving Forward
True oily, dehydrated, barrier-compromised skin has specific signs beyond just feeling oily and breaking out. Your skin may feel tight or uncomfortable even when it looks shiny. Moisturizers may feel heavy or cause congestion because your barrier can’t properly absorb hydrating ingredients. You might notice increased sensitivity to products you used to tolerate. These signs confirm that you’re dealing with barrier dysfunction, not just typical acne or typical oiliness.
Understanding this distinction is crucial because it completely changes your treatment strategy. The path forward involves barrier repair as the primary goal, with acne management as a secondary benefit. This means prioritizing ceramide-rich hydration, gentle cleansing that doesn’t strip, avoiding over-exfoliation, and patience with a longer timeline for visible improvement. The good news is that once you repair your barrier and normalize sebum production, you’ll often see acne improve significantly without ever using aggressive acne medications. Your skin has a remarkable capacity to heal itself when you stop actively damaging it.
Conclusion
Oily skin that feels dehydrated and breaks out is a clinically measurable condition rooted in barrier dysfunction and abnormal sebum composition, not a character flaw or a reason to wage war on your skin. The solution isn’t stronger products or more aggressive treatment—it’s barrier repair. When you stop stripping your skin and start rebuilding its lipid foundation, excess oil production normalizes, dead cell accumulation decreases, pores function properly, and breakouts resolve. This approach takes patience and consistency, but it addresses the actual problem rather than creating a temporary improvement followed by a deeper crash.
Start by identifying barrier-damaging products in your routine and replacing them with gentle cleansing and ceramide-rich hydration. Give your barrier 6-8 weeks to repair before judging results. If you’re currently using active acne treatments, don’t necessarily stop them immediately—transition slowly while building barrier support underneath. Your skin is responding logically to damage; repair the damage, and the breakouts and excess oil will follow.
You Might Also Like
- Why Some Skin Types Are More Prone to Hyperpigmentation
- Why Skin Cycling Can Help Acne Prone Skin Types
- What Order to Apply Skincare Products for Acne Prone Skin
Browse more: Acne | Acne Scars | Adults | Back | Blackheads