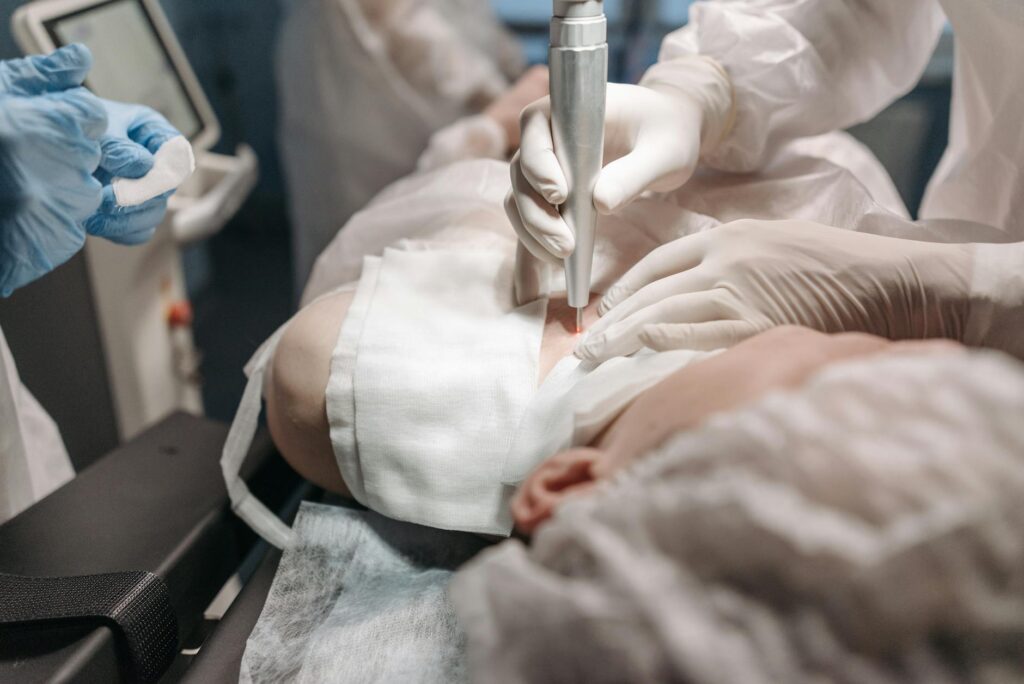
The order in which you undergo acne scar treatments directly determines how much improvement you’ll see and how quickly you’ll achieve it. Performing procedures in the wrong sequence can waste time and money, leave you with incomplete results, or even create temporary setbacks that set your overall timeline back months. For example, starting with aggressive laser resurfacing before addressing depressed scars with subcision or fillers means the laser treats skin that still has structural deficits underneath—the scars may appear lighter, but the indentation remains. In contrast, a practitioner who first releases the scar tissue with subcision, then follows with filler if needed, and finally refines the appearance with laser or chemical peels will deliver results that address the scars at multiple levels, creating lasting improvement that’s visible in every type of light.
The reason order matters comes down to both biology and physics. Your skin’s capacity to remodel is limited in any given treatment window—it can only handle so much inflammation and stimulation before you hit the point of diminishing returns or risk complications. Some procedures damage skin intentionally to trigger healing, meaning doing them simultaneously or in rapid succession overwhelms your skin’s repair response. Other procedures only work effectively on skin that’s already been prepared by an earlier treatment. This article covers the science behind treatment sequencing, how to assess your scar type to determine the right order, common mistakes that dermatologists see in patients jumping between providers, and a practical roadmap for planning your acne scar treatment journey.
Table of Contents
- How Skin Type and Scar Morphology Dictate the Procedure Order
- Why Layered Damage Control Prevents Burnout and Complications
- Combination Treatments and Strategic Pairing
- Building Your Custom Treatment Timeline Based on Scar Severity
- Common Ordering Mistakes That Dermatologists See Repeatedly
- Recovery Windows and Why Timing Between Sessions Matters More Than You Think
- Reassessing and Adjusting Your Plan as Your Skin Changes
- Conclusion
- Frequently Asked Questions
How Skin Type and Scar Morphology Dictate the Procedure Order
Your starting point—the specific type and depth of scars you have—is the foundation that determines everything else. acne scars aren’t monolithic; they come in distinct categories: atrophic (depressed) scars including icepick scars (very narrow and deep), boxcar scars (wider and angular), and rolling scars (shallow and wave-like), plus hypertrophic or keloid scars that are raised. Each responds best to different first-line treatments, and the order cascades from there. Rolling scars often respond well to subcision or radiofrequency as a first step because the main problem is fibrous tethering pulling the skin down; releasing that tethering immediately improves appearance.
Icepick scars, by contrast, are often too narrow for subcision to work effectively, so many practitioners start with laser or chemical peels to gradually soften their appearance, or skip straight to filler if depth is severe. Skin tone and texture complicate the sequencing further. Patients with darker skin tones have a higher risk of post-inflammatory hyperpigmentation (darkening) after aggressive treatments, which means the order must account for a longer recovery window between procedures and often prioritizes gentler techniques first. Someone with baseline sensitive or rosacea-prone skin needs to avoid consecutive inflammatory procedures, whereas someone with resilient, thick skin can often tolerate a tighter sequence. A dermatologist assessing your scars will also consider whether you have pitted scars isolated to specific zones (like the cheeks) or diffuse scarring across the entire face—localized scarring sometimes benefits from more aggressive single procedures in sequence, while diffuse scarring often calls for multiple gentler passes spaced weeks apart to avoid overwhelming the skin.

Why Layered Damage Control Prevents Burnout and Complications
The most dangerous mistake patients make is assuming that back-to-back aggressive procedures will deliver faster results. In reality, your skin has a limited capacity for inflammation and remodeling within a specific timeframe—usually 6 to 12 weeks after a major procedure is when collagen remodeling peaks. If you perform multiple ablative procedures (those that remove or severely damage skin) close together, you don’t compound the benefit; instead, you trigger excessive inflammation that leads to post-inflammatory hyperpigmentation, prolonged redness, temporary worsening of rolling scars as swelling masks any improvement, and in worst cases, skin barrier breakdown that results in infection or permanent texture changes. Consider the scenario of someone receiving a deep chemical peel (aggressive resurfacing) followed by fractional CO2 laser two weeks later.
The skin is still healing from the chemical peel, its barrier is compromised, and it’s in a heightened inflammatory state. The laser then triggers another wave of inflammation while the skin is already stressed, increasing the likelihood of hypertrophic scarring during healing and extending the recovery window dramatically—what might have been two weeks of visible peeling from the laser alone now turns into a month of inflammation, redness, and sensitivity. However, if that same sequence is spaced 8 to 12 weeks apart, allowing the skin to fully remodel and barrier function to restore between treatments, the second procedure actually works more effectively because the skin is stable and can tolerate the treatment without complications. The key principle is staggering ablative procedures (laser, deep peels, aggressive microneedling) and reserving back-to-back treatments for gentler modalities like light chemical peels or conservative radiofrequency.
Combination Treatments and Strategic Pairing
Certain procedure combinations are so synergistic that practitioners intentionally pair them in the same session or within a few days, while others must be strictly separated. Subcision paired with microneedling in the same session, for instance, is a recognized safe combination—the subcision releases tethered scar tissue, and the microneedling in the weeks following stimulates collagen in the released area. By contrast, performing subcision and then immediately doing laser resurfacing creates competing inflammation signals and risks excessive post-inflammatory changes.
Another high-value pairing is starting with radiofrequency or microneedling to build foundational collagen, then adding a chemical peel or light laser 4 to 6 weeks later once that collagen has strengthened the skin. The initial treatment creates a “strengthened” base layer, and the second treatment refines surface texture without risking the complications you’d see if you did both simultaneously. Dermal fillers complicate sequencing differently because they’re non-ablative and can technically be done alongside almost anything, but the strategic order matters: many practitioners inject filler after finishing ablative treatments (once swelling resolves) rather than before, because the ablative procedures already improve the appearance and sometimes reduce the filler volume needed. Injecting filler first, then doing laser, can mean over-filling areas that will improve on their own, wasting product and creating overstuffed-looking results.
Building Your Custom Treatment Timeline Based on Scar Severity
A practical starting framework depends on scar depth and type. For someone with mild rolling scars and light boxcar scarring, a reasonable order is: start with 2 to 3 sessions of fractional laser or radiofrequency spaced 4 to 6 weeks apart, assess results, and add light chemical peels or microneedling in months 2 to 4 if additional refinement is needed. This sequence works because the initial radiofrequency or laser improves collagen in the dermis without excessive surface damage, so tolerability is high and results are visible. For moderate icepick or deeper boxcar scars, many experienced practitioners start with a single session of subcision or trichloroacetic acid (TCA) cross (spot treatment on icepick scars) to address structural deficits, follow with radiofrequency or fractional laser 6 to 8 weeks later, and then layer in gentler resurfacing like light chemical peels or additional radiofrequency rounds.
The tradeoff in this approach is that TCA cross and aggressive subcision carry temporary risks—visible peeling, scabbing, and if TCA is applied incorrectly, permanent depigmentation—which means you need a practitioner experienced enough to apply them safely and you need realistic expectations about a 1 to 2 week visible recovery period. Severe pitted scarring with deep icepick scars and extensive boxcar involvement sometimes requires a longer timeline: starting with TCA cross or punch techniques, allowing 8 to 12 weeks for remodeling, then adding radiofrequency, and potentially including filler or additional procedures in months 3 to 6. The benefit of a longer timeline is that each procedure works on skin that’s been improved by the previous one, creating compounding results rather than fighting against unhealed inflammation. The downside is patience—you won’t see the final result for 6 months or longer, whereas a faster protocol might show improvement in 2 to 3 months even if it’s less comprehensive.
Common Ordering Mistakes That Dermatologists See Repeatedly
One frequent error is patients seeking filler first, before any resurfacing treatment. While filler can temporarily improve scars, injecting it into untreated depressed scars sometimes makes them look better in the short term but creates dependency on repeated filler and misses the opportunity to use more effective structural treatments. A scar that could be released with subcision and then remodeled with laser instead gets filled every 6 months indefinitely. Another mistake is jumping between providers and repeating similar procedures without adequate spacing: a patient might get laser at one clinic, then see a different provider who recommends laser again just 4 weeks later, not realizing the first procedure is still actively remodeling.
The most consequential mistake involves patients with post-inflammatory hyperpigmentation (darkened scars or post-treatment darkening) continuing with aggressive treatments instead of pausing. If you’ve experienced hyperpigmentation after a procedure, the correct next step is usually to wait 3 to 6 months for the pigmentation to naturally fade, use topical hydroquinone or tretinoin to speed fading, and then resume gentler treatments once the skin is stable. Instead, many patients see the darkening and immediately book more aggressive laser, assuming it will “burn off” the pigmentation—this almost always worsens it and extends the total recovery timeline. A related error is underestimating recovery time between procedures; practitioners sometimes tell patients they can do another treatment in 3 weeks, and patients comply, only to find their skin is still red or sensitive enough that the second procedure causes complications.

Recovery Windows and Why Timing Between Sessions Matters More Than You Think
The standard guidance is 4 to 6 weeks between most laser and radiofrequency treatments, but this is a minimum, not an ideal. What actually matters is skin barrier restoration and resolution of post-procedure inflammation. Under the microscope, your skin is still remodeling collagen up to 12 weeks after a procedure, which means doing another inflammatory treatment at 4 weeks is happening while the previous treatment is still actively working—you’re not adding to the benefit, you’re interrupting it and creating confused inflammatory signals.
In contrast, waiting a full 8 to 12 weeks allows the first procedure’s results to stabilize, and the second procedure then acts on improved skin. For gentler procedures like light chemical peels or conservative microneedling, spacing can be closer—some protocols do these weekly or every other week because they’re not triggering enough damage to monopolize the skin’s healing resources. However, even with gentle treatments, doing more than one inflammatory procedure per week is counterproductive; most skin can handle one inflammatory stimulus per week, maximum, without beginning to show signs of irritation or barrier compromise. Practical advice: if your skin shows any residual redness, sensitivity, or peeling when you return for your next procedure, that procedure should be deferred or made significantly gentler, because adding stress to already-stressed skin increases complication risk without improving results.
Reassessing and Adjusting Your Plan as Your Skin Changes
Acne scars don’t respond uniformly to treatment, which means your treatment order might need adjustment mid-course. It’s not uncommon to complete the first 2 sessions of laser or radiofrequency, reassess with your dermatologist, and realize that rolling scars have improved significantly but icepick scars remain unchanged. At that point, rather than continuing with the same modality, you might pivot to subcision or TCA cross to address the remaining icepick damage, then resume radiofrequency or laser afterward.
This kind of adaptive planning requires a practitioner who’s willing to modify the plan based on results rather than robotically following a preset protocol. Looking forward, combination therapies and newer technologies (like combination radiofrequency with microneedling, or plasma devices) are allowing practitioners to deliver better results with shorter timelines, but the fundamental principle remains unchanged: the order matters because each procedure primes your skin’s collagen system for the next one. As technologies improve and become less aggressive, the strict spacing requirements of older techniques (like deep chemical peels) are loosening, allowing faster overall treatment timelines. However, this doesn’t mean you should rush; a thoughtful, sequential approach tailored to your specific scars will always outperform a hurried regimen aimed at finishing fast.
Conclusion
The order of acne scar procedures is not arbitrary—it’s a carefully sequenced strategy that determines whether your treatments compound toward dramatic improvement or work against each other and waste your time and money. Starting with the right foundation (whether that’s subcision, radiofrequency, laser, or chemical peels) ensures that each subsequent procedure works on primed, improving skin rather than against unhealed inflammation or structural deficits. Understanding your scar type, accepting realistic spacing between treatments, and being willing to adjust your plan as results emerge are the three pillars of successful acne scar treatment.
The path forward is to consult with a dermatologist who will assess your specific scar morphology and create a custom sequence rather than offering a one-size-fits-all protocol. Ask about the reasoning behind the proposed order—why they recommend starting with a specific treatment, how long between procedures, and what the decision tree looks like if results come in slower than expected. A practitioner who can explain the sequence and adjust it based on your individual response is far more likely to deliver the comprehensive improvement you’re seeking.
Frequently Asked Questions
Can I do laser and microneedling in the same session to speed up results?
This depends on intensity. Light microneedling followed by light laser on the same day is generally safe, but aggressive laser combined with deep microneedling creates excessive inflammation. Most practitioners prefer spacing them 4 to 6 weeks apart to allow each procedure’s effects to compound safely.
How much time should pass between subcision and filler injections?
Subcision can be done with filler injected the same day or within a few days; however, many practitioners wait 1 to 2 weeks to see how much the skin improved on its own from subcision before deciding whether filler is even needed, often reducing the filler volume required.
If I get a chemical peel, when can I do laser?
Light chemical peels allow laser in 4 to 6 weeks; deep chemical peels require 8 to 12 weeks before any additional ablative treatment. The darker and more sensitive your skin, the longer you should wait to avoid post-inflammatory hyperpigmentation.
Can I do two laser treatments in one month if they target different depths?
No. The skin doesn’t distinguish between different types of laser inflammation—it sees cumulative damage. Two laser treatments one month apart, even if different wavelengths, significantly increases risk of prolonged redness, hyperpigmentation, and scarring during healing.
Is it better to do many gentle treatments or fewer aggressive ones?
Fewer aggressive treatments spaced properly (8 to 12 weeks apart) typically deliver better results and faster visible improvement than many gentle treatments. However, this assumes expert technique and appropriate candidate selection; many patients benefit from a hybrid approach of a few moderate treatments rather than either extreme.
What’s the ideal total timeline for treating moderate acne scars?
Expect 6 to 12 months from start to final result. This includes 2 to 4 major procedures spaced 6 to 8 weeks apart, plus potential maintenance treatments or fine-tuning. Results continue improving for up to a year as collagen remodeling concludes.
You Might Also Like
- New Acne Skincare Line Focuses on Results
- Why Under-Eye Hollowing Worsens After Laser for Acne Scars
- New Study Suggests Hormones Can Trigger Rapid Acne Response
Browse more: Acne | Acne Scars | Adults | Back | Blackheads