Dermatologists specialize exclusively in acne treatment for three fundamental reasons: the disease’s staggering prevalence, the considerable complexity of treatment protocols, and the permanent scarring that can result from mismanaged cases. Acne affects 9.4% of the global population and ranks as the 8th most prevalent disease worldwide. In the United States alone, approximately 50 million Americans struggle with acne annually, with 85% of all people experiencing at least some form of it during their lifetime. This isn’t a rare condition that only occasionally walks through the clinic door—it’s the reason roughly one-fifth of all dermatology office visits happen. For dermatologists looking to build a sustainable, high-demand practice, specializing in acne makes straightforward business sense.
Beyond prevalence, acne presents a genuinely complex clinical challenge. The condition involves understanding sebum production, bacterial colonization, inflammation, hormonal influences, scarring mechanisms, and the pharmacology of multiple drug classes. A dermatologist who focuses only on acne can develop surgical precision with extractions, laser ablation, chemical peeling protocols, and systemic medication management that a generalist simply cannot match. When a patient has been to five other dermatologists without improvement, the acne specialist has the depth of knowledge to identify what previous doctors missed. This article examines why acne specialization has become a viable full-time career path, the training required to do it well, the market forces supporting it, and how acne specialists approach treatment differently than generalists.
Table of Contents
- Why Acne Creates a Self-Sustaining Specialization Niche
- The Clinical Complexity That Demands Specialization
- Demographic-Specific Acne Expertise
- The Extensive Training Acne Specialization Requires
- The Prevention of Permanent Damage Drives Specialization
- Minimally Invasive and Emerging Procedure Expertise
- The Future of Acne Specialization—Personalized and Technology-Driven
- Conclusion
Why Acne Creates a Self-Sustaining Specialization Niche
The acne market is substantially larger than most people realize. U.S. consumers spend over $6 billion annually on acne treatments—yet only 10% of those people actually consult a dermatologist. This creates an enormous gap between demand and professional supply. The global acne treatment market was valued at $11.6 billion in 2025 and is projected to reach $18.4 billion by 2034, growing at a compound annual rate of 5.3%.
Dermatology clinics specifically hold 59.8% of this market share and are expected to continue dominating in specialized acne management. For individual dermatologists, this means acne specialization can support a fully booked practice. A general dermatologist might see acne patients mixed among skin cancer screenings, eczema cases, and cosmetic consultations. But an acne specialist can maintain consistent patient volume simply by becoming the local expert that primary care doctors and other specialists refer their difficult cases to. In major metropolitan areas, average wait times to see a dermatologist range from 28 to 32 days, yet specialized acne clinics often book appointments weeks in advance. The economics are straightforward: high demand, limited supply, and the willingness of patients to wait or travel for expertise creates the conditions where someone can spend their entire career treating one condition.

The Clinical Complexity That Demands Specialization
Acne is not one disease—it’s a spectrum of diseases with different underlying drivers and treatment pathways. The same acne treatment that works for a 16-year-old with hormonally driven comedonal acne will fail completely for a 35-year-old woman with perioral dermatitis masquerading as acne, or for someone whose breakouts are being triggered by their skincare routine’s silicone content. A general dermatologist might recognize acne at a glance, but an acne specialist can identify these distinctions and adjust accordingly.
However, not every breakout requires an acne specialist. Mild acne that responds to over-the-counter benzoyl peroxide or salicylic acid rarely needs professional evaluation at all. The specialization becomes valuable when patients have inflammatory cystic acne, acne that has resisted multiple topical treatments, or acne occurring in contexts where common treatments are contraindicated (pregnancy, for example). This is why dermatologists who specialize in acne often see a high proportion of moderate-to-severe cases, and why their expertise translates into measurably better outcomes than generalists.
Demographic-Specific Acne Expertise
Acne prevalence varies dramatically by age and sex, creating natural specialization opportunities. Females experience nearly double the acne incidence of males. More strikingly, 50% of women in their 20s continue to struggle with acne, declining to 33% in their 30s and 25% in their 40s. This pattern is nearly invisible to most healthcare providers, but acne specialists see it constantly. A woman in her late thirties with sudden inflammatory breakouts often has hormonal acne triggered by menstrual cycle shifts, androgen sensitivity, or spironolactone deficiency—conditions that a dermatologist who primarily treats skin cancer will miss.
Among adolescents aged 12 to 24, acne prevalence reaches 85%, making this the highest-risk demographic. But acne specialization in this age group requires understanding how to manage systemic medications in teenagers whose organs are still developing, how to address the psychological impact of facial scarring during formative social years, and how to navigate parental involvement in treatment decisions. An acne specialist treating teenagers develops expertise that a dermatologist seeing teenagers only occasionally will never acquire. Young adults represent another distinct cohort. Male-pattern hormonal acne, post-inflammatory hyperpigmentation in darker skin types, and the occupational acne triggered by protective equipment all have specific prevalence patterns in this age group that specialists learn to recognize and manage.
The Extensive Training Acne Specialization Requires
Becoming an acne-focused dermatologist requires a commitment that extends far beyond medical school. The baseline training to become any dermatologist involves 4 years of college, 4 years of medical school, 1 year of internship, and 3 years of dermatology residency—a total of 12 years of formal education and training. After residency, dermatologists who want to specialize in acne typically pursue additional fellowship training, attend acne-focused conferences and workshops, and maintain their knowledge as new treatments emerge. This depth of training matters because acne management has evolved considerably.
Twenty years ago, oral antibiotics were first-line treatment for most moderate acne. Today, acne specialists recognize that long-term antibiotic use drives resistance and that isotretinoin (formerly Accutane) now has clearer clinical guidelines, making it appropriate for cases that would previously have been managed with years of antibiotics. Retinoid therapy is experiencing rapid growth due to underutilization and proven anti-inflammatory benefits—but prescribing retinoids requires understanding pregnancy risk, photosensitivity, and patient tolerance of the initial “retinization” phase that discourages many patients. An acne specialist has this knowledge; a generalist may not.
The Prevention of Permanent Damage Drives Specialization
This is perhaps the most compelling reason dermatologists specialize in acne: the stakes of poor management are genuinely high. Acne can cause permanent scarring and dark spots that persist for years or indefinitely. A patient with inflammatory cystic acne who receives only topical treatments and sympathy has a high probability of developing atrophic or hypertrophic scars. These scars cannot be completely erased—they can only be improved through expensive procedures like laser resurfacing, subcision, or filler injections. However, if that same patient had seen an acne specialist who recognized the need for systemic treatment within the first six months of breakouts, many of those scars would never have formed in the first place. Prevention is vastly cheaper and more effective than treatment after the fact.
This preventive power is what justifies the higher fees acne specialists often charge and why patients will wait weeks to see them. A parent watching their teenager’s face become permanently scarred will pay whatever it costs to see the specialist they should have consulted two years earlier. Post-inflammatory hyperpigmentation—the dark marks left behind after acne clears—is another area where specialization matters. In patients with darker skin types, these marks can be more pronounced and longer-lasting than in fair-skinned patients. Acne specialists understand that some treatments that work well in fair skin (like certain laser types) can worsen hyperpigmentation in darker skin. They have alternative protocols, experience with different laser wavelengths, and knowledge of how vitamin C serums and hydroquinone interact with acne treatment regimens.

Minimally Invasive and Emerging Procedure Expertise
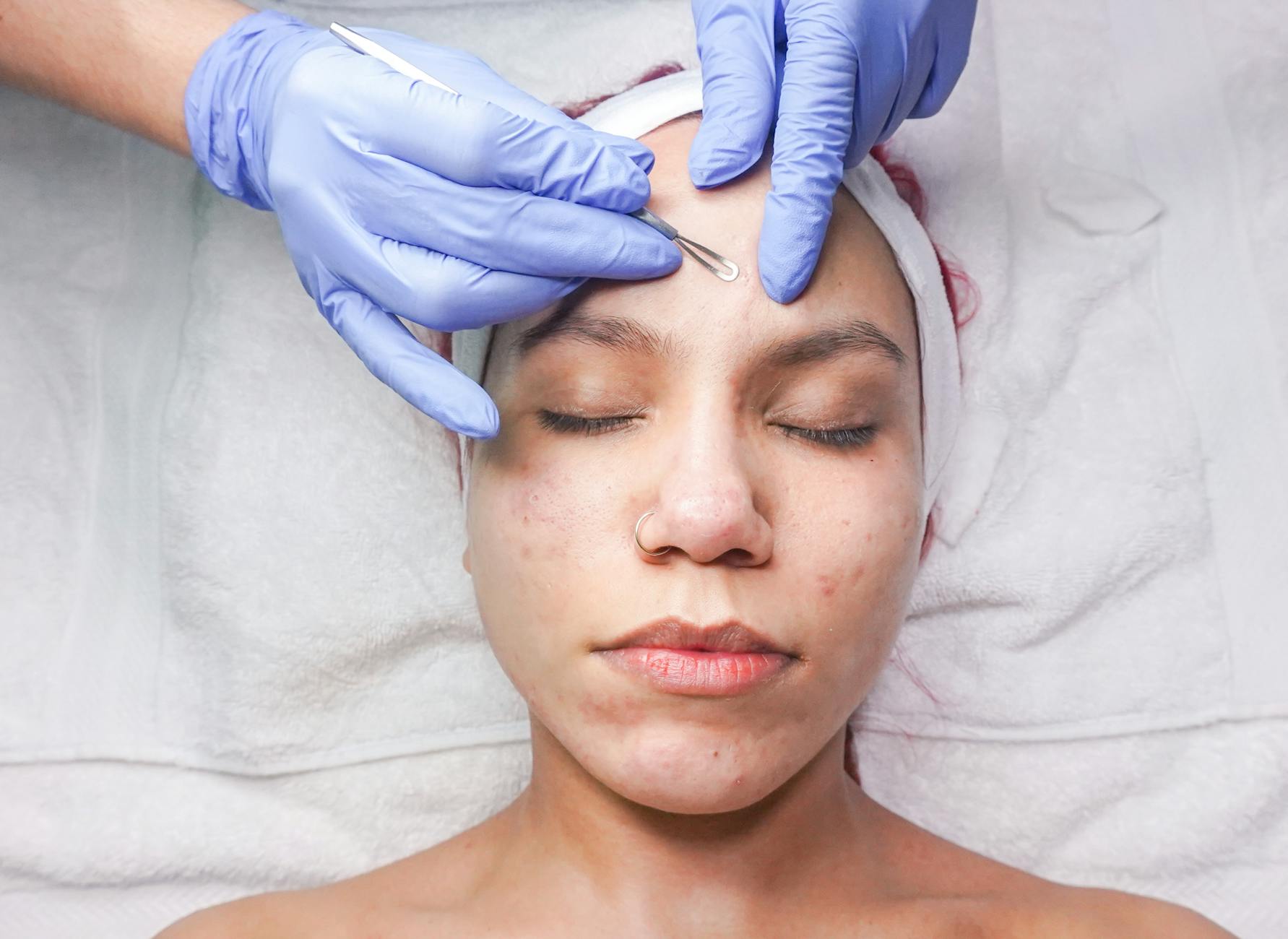
The acne treatment landscape has expanded dramatically beyond prescriptions. Minimally invasive procedures—steroid injections for cystic acne, chemical peels, laser therapy, and extraction techniques—are projected to grow at approximately 5% annually during 2024-2029. These procedures require substantial skill to perform safely and effectively.
Consider intralesional steroid injection: an acne specialist performs this on cystic lesions to flatten them within 24 to 48 hours, preventing permanent scar formation. This is a quick, elegant intervention that a general dermatologist might perform occasionally, but an acne specialist performs dozens of times per month and has refined the technique to minimize side effects. Similarly, chemical peels for post-inflammatory hyperpigmentation require understanding how peeling strength, frequency, and timing interact with acne treatment medications like isotretinoin and retinoids. An acne specialist has this integration of knowledge; others have pieces of it.
The Future of Acne Specialization—Personalized and Technology-Driven
The acne market is increasingly driven by personalized treatment approaches, artificial intelligence, telemedicine, and wearable monitoring technologies. These emerging tools are not replacing specialist dermatologists—they’re expanding what specialists can do. AI algorithms that analyze photographs to predict which acne patients will respond to certain medications are already being tested in research settings. Acne specialists who integrate these tools into their practice will likely capture more market share and achieve better patient outcomes.
Telemedicine has already transformed acne specialization by removing geographic constraints. A patient in a rural area can now consult with an acne specialist who practices in a major city, send photographs, receive a treatment plan, and follow up remotely. This technology is expanding the reach of specialized acne care while simultaneously increasing demand for specialists who know how to conduct acne assessments via telehealth. The future likely involves hybrid practices where dermatologists spend part of their week seeing patients in-clinic for procedures and direct visualization, and the other part conducting virtual consultations.
Conclusion
Dermatologists specialize exclusively in acne because the condition’s prevalence, clinical complexity, and consequences justify deep expertise. With 85% of Americans experiencing acne at some point, and dermatology clinics holding nearly 60% of a $11.6-billion-and-growing global treatment market, specialization represents both a sound clinical and business decision.
The training required is substantial—12 years of formal education followed by ongoing specialization—but the reward is the ability to prevent permanent scarring, manage complex cases that other doctors have failed, and build a sustainable practice based on expertise rather than patient volume alone. If you struggle with acne that hasn’t improved with over-the-counter treatments or has left scarring, consulting an acne specialist is worth the wait. The time you invest now can prevent years of treatment and regret later.
You Might Also Like
- Why Some Acne Patients Never Respond to Any Treatment
- Why Zinc Acetate IV Is Studied for Severe Inflammatory Acne
- Why Stem Cell Conditioned Media Works for Acne Healing
Browse more: Acne | Acne Scars | Adults | Back | Blackheads