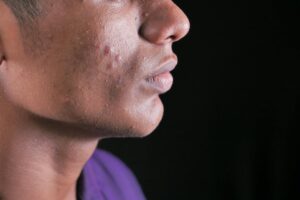
Patient-reported outcomes matter for acne research because they measure what actually matters most to patients—how treatment affects their quality of life, appearance, and psychological well-being—not just what doctors observe under a microscope. For decades, acne clinical trials focused primarily on what dermatologists could see: how many comedones remained, whether inflammation decreased, or whether scarring improved. But research now shows that acne’s psychological and social impact rivals that of serious chronic diseases like asthma and diabetes, meaning that a treatment might clear lesions while still failing to restore a patient’s confidence or quality of life. This article explores why regulatory agencies, researchers, and dermatologists are increasingly centering patient voices in acne research, how this shift is changing what treatments get approved, and what it means for anyone seeking effective acne care.
The turning point came in 2009 when the FDA issued formal guidance directing that patient-reported outcome (PRO) measures be used to support labeling claims in medical products. This wasn’t just bureaucratic language—it fundamentally changed how acne treatments are evaluated. Before this guidance, a medication might be deemed successful based on clinical assessments alone. Now, PRO data is a critical component of clinical trial evaluation, and FDA approvals for acne treatments increasingly require evidence that patients themselves report improvement in their symptoms and quality of life.
Table of Contents
- What Are Patient-Reported Outcomes and Why Do They Matter for Acne Treatment?
- The FDA’s Shift Toward Patient-Centered Clinical Trials
- Recent Research Breakthroughs in Patient-Centered Acne Science (2025)
- How Patient-Reported Outcomes Change Clinical Practice
- The Ongoing Challenge of PRO Measurement Standardization
- Validated Instruments That Matter
- The Future of Patient-Centered Acne Research and Personalized Treatment
- Conclusion
What Are Patient-Reported Outcomes and Why Do They Matter for Acne Treatment?
Patient-reported outcomes are measurements of health or disease collected directly from patients themselves, rather than inferred from lab tests, imaging, or a doctor’s examination. For acne, PROs capture what patients experience: Does the treatment reduce pain and tenderness? Has it improved their skin’s appearance in ways that matter to them? Have they regained confidence in social situations? Do they feel less distressed or anxious about their skin? These dimensions simply cannot be captured by a dermatologist counting pustules during a 15-minute office visit. Acne is unique among skin conditions in its psychological toll. Clinical research has documented that acne’s impact on health-related quality of life is comparable to chronic diseases such as asthma, arthritis, and diabetes.
A patient with mild acne might report severe social withdrawal, while another with moderate acne might adjust well—and no clinical severity scale captures that variation. This is why PROs are essential: they reveal whether a treatment is actually solving the patient’s problem. A medication that clears 80% of acne lesions but leaves patients feeling self-conscious about remaining marks may not represent the clinical success that raw lesion counts suggest. Conversely, a treatment that produces modest lesion reduction but dramatically improves a patient’s confidence and social functioning may be profoundly valuable.
The FDA’s Shift Toward Patient-Centered Clinical Trials
The 2009 FDA guidance on patient-reported outcomes was a watershed moment for acne research. Before this formal direction, patient-reported measures were largely optional add-ons to dermatology trials. A 1994-2001 review found that PROs were included in only 25% of 125 dermatology clinical trials conducted during that era. This meant the vast majority of acne studies were measuring treatment success through a purely clinical lens, ignoring the patient’s own assessment of their outcomes. Since the FDA issued its guidance, adoption has grown significantly, reflecting a broader recognition that treatments must improve patients’ actual lives, not just their skin metrics.
However, this shift has revealed a significant challenge: until recently, acne research lacked standardized, rigorously validated PRO instruments. A systematic review published in JAMA Dermatology examined 21 patient-reported outcome measures for acne and found that only 2 met recommended standards for validation and reliability—the Acne-Q and CompAQ. This means many historical trials used poorly validated measures, and researchers comparing results across studies often could not be sure they were measuring the same thing. The Dermatology Life Quality Index (DLQI) has become a standard for measuring quality-of-life impact, and it has been applied in acne research to quantify improvements in social functioning, emotional distress, and daily activities. Without standardized instruments, FDA approvals could not be reliably justified, and clinical advancement was hampered by inconsistent measurement.
Recent Research Breakthroughs in Patient-Centered Acne Science (2025)
The field experienced two major advances in 2025 that demonstrate the maturing sophistication of PRO-driven acne research. The Acne Core Outcomes Research Network Patient Global Assessment for Acne was validated and published in JAMA Dermatology, establishing a new standardized patient assessment tool specifically designed for acne clinical research. This is significant because it provides researchers with a rigorously tested instrument that directly captures patients’ global perception of their acne condition and its severity—exactly what the field had been lacking.
Simultaneously, a randomized controlled trial published in JMIR Dermatology demonstrated that machine learning-enabled personalized skincare recommendations for mild-to-moderate acne significantly improved both severity scores (the clinical measures dermatologists track) and overall quality of life as measured by the DLQI. This study is important because it showed that modern precision medicine approaches can optimize treatment outcomes not just by clinical metrics but by directly measuring what patients themselves experience. Patients receiving personalized AI-driven recommendations reported improvements in emotional well-being, social confidence, and daily functioning alongside clinical improvements. This dual measurement paradigm—combining clinical severity reduction with patient-reported quality-of-life gains—represents the new gold standard that regulatory agencies and researchers now expect.

How Patient-Reported Outcomes Change Clinical Practice
When PROs are systematically measured in clinical trials, the results can reveal unexpected treatment trade-offs. A study of 79 acne patients treated with tretinoin gel microsphere for 12 weeks documented significant improvements not just in clinical acne severity but across multiple quality-of-life measures: DLQI scores improved, self-esteem increased, GHQ-28 scores (measuring general mental health and distress) improved, and SF-36 scores (measuring overall functional status) rose. These data provided evidence not only that tretinoin worked clinically but that it meaningfully restored patients’ psychological and social functioning—information that matters enormously to patients deciding whether to tolerate the treatment’s side effects like dryness, irritation, and photosensitivity. PRO-driven trials also surface nuances that pure clinical measurement misses.
For instance, two treatments might show equivalent acne clearance, but one could result in better psychological recovery and social reintegration. In clinical practice, dermatologists increasingly discuss these PRO findings with patients when selecting treatments, moving away from a one-size-fits-all approach toward shared decision-making that acknowledges each patient’s priorities. A teenager might weight psychological recovery most heavily, while an adult in a conservative profession might prioritize residual appearance. PROs make these conversations evidence-based rather than anecdotal.
The Ongoing Challenge of PRO Measurement Standardization
Despite the progress represented by 2025 validations, a significant challenge remains: most historical acne research lacks reliable PRO data, creating a fragmented evidence base. Earlier I mentioned that only 2 of 21 acne-specific PRO measures met validation standards until very recently. This historical gap means that many older studies claiming “excellent outcomes” may not have actually measured patient satisfaction rigorously. Researchers and clinicians must be cautious about over-interpreting legacy trial data that relied on unvalidated or informal patient assessments.
Additionally, even with validated instruments like the DLQI and the new Acne Core Outcomes Research Network Patient Global Assessment, interpretation requires nuance. A significant improvement in DLQI score, for example, indicates better quality of life, but it doesn’t capture the temporal dimension—how long patients must endure side effects or waiting time before improvements appear. A treatment showing a large PRO improvement after 16 weeks but causing severe dryness weeks 1-4 might be less attractive than a slower treatment with minimal side effects, depending on the patient’s circumstances. The broader lesson is that PRO data is essential but must be interpreted contextually, considering the patient’s full experience across time.

Validated Instruments That Matter
The distinction between validated and unvalidated PRO measures has real clinical consequences. The Acne-Q and CompAQ, identified as the only two acne-specific measures meeting recommended validation standards, are now increasingly used in research because they reliably capture acne-related quality-of-life impact. The Dermatology Life Quality Index (DLQI), though broader and not acne-specific, has become an essential companion measure in acne trials because it quantifies effects on emotional well-being, social functioning, and daily activities—domains that vary widely among individual patients.
The 2025 validation of the Acne Core Outcomes Research Network Patient Global Assessment provides a new gold standard specifically for acne, moving the field closer to consistency. Researchers selecting which PRO instruments to use in future acne trials can now choose from a small but robust toolkit of validated measures, rather than improvising with informal patient questionnaires. This standardization is accelerating the pace at which findings from different trials can be compared, synthesized, and translated into clinical guidelines.
The Future of Patient-Centered Acne Research and Personalized Treatment
As PRO measurement becomes the norm rather than the exception, acne research is shifting toward precision medicine—matching specific treatments to specific patients based not just on acne severity but on each patient’s priorities and predicted response. The 2025 machine learning study illustrates this trend: by collecting robust PRO data alongside clinical data, researchers can train algorithms to predict which patients will benefit most from particular skincare approaches. This personalized, evidence-based approach promises to improve outcomes while reducing the trial-and-error cycle that has historically characterized acne treatment.
The regulatory and scientific infrastructure is now in place for this transition. The FDA’s 2009 guidance is being operationalized through validated instruments, modern technology enables systematic PRO data collection at scale, and researchers recognize that patient-reported outcomes are as essential to acne research as any laboratory measurement. For patients, this means future acne treatments will be approved based on evidence that they actually improve quality of life, not just lesion counts. For researchers and dermatologists, it means acne research is becoming more rigorous, more patient-centered, and more clinically relevant.
Conclusion
Patient-reported outcomes matter for acne research because acne is not a disease that can be understood through clinical observation alone. Its impact on psychological well-being, social functioning, and quality of life rivals that of serious chronic diseases, yet for decades, research largely ignored these patient-centered dimensions. The FDA’s 2009 guidance and recent advances—including the 2025 validation of the Acne Core Outcomes Research Network Patient Global Assessment and the demonstration of machine learning-enhanced personalized treatment—have established PROs as essential to rigorous acne research and evidence-based treatment selection.
Moving forward, acne patients should expect that treatments approved or recommended to them will be supported by evidence of improved quality of life and patient satisfaction, not just clinical severity reduction. Dermatologists increasingly ground treatment recommendations in PRO data, enabling shared decision-making that respects each patient’s unique priorities. This patient-centered paradigm represents a maturation of acne science, ensuring that research and clinical practice focus on what genuinely matters: not just clearing skin, but restoring confidence, functionality, and well-being.
You Might Also Like
- What Acne Research Funding Gaps Mean for Treatment Progress
- Why Ziana Gel Combines Tretinoin and Clindamycin for Acne
- Why Vegans Still Get Acne — What They’re Missing
Browse more: Acne | Acne Scars | Adults | Back | Blackheads