Mechanical tension on acne wounds directly leads to worse scarring because of how your skin’s healing process responds to physical stress. When a wound is under tension—whether from skin stretching, repeated picking, or inflammation pulling the edges apart—your body deposits collagen fibers in a more haphazard, disorganized pattern to bridge that gap. This creates thicker, wider, more visible scars.
In contrast, wounds that heal under minimal tension develop tighter collagen networks that sit flush with the surrounding skin, making the scar barely noticeable. A practical example: if you pick at an acne lesion and keep the wound edges separated through scratching or touching, the resulting scar will typically be much more prominent than if you had left it undisturbed. This article explores exactly how mechanical tension influences scar formation during acne healing, which types of scars are most affected by tension, and most importantly, what practical steps you can take to minimize tension on your acne wounds to prevent severe scarring down the line.
Table of Contents
- How Does Mechanical Tension Actually Cause Wider Acne Scars?
- The Tension-Scarring Connection Across Wound-Healing Phases
- Which Acne Scar Types Are Most Worsened by Mechanical Tension?
- Practical Methods to Minimize Mechanical Tension During Acne Healing
- Common Mistakes That Increase Mechanical Tension on Acne Wounds
- Comparison: Treated vs. Untreated Acne Scars from Tension Damage
- The Future of Tension-Guided Scar Prevention
- Conclusion
- Frequently Asked Questions
How Does Mechanical Tension Actually Cause Wider Acne Scars?
Your skin doesn’t heal in a vacuum—it responds directly to the physical forces acting on the wound during the critical 2-4 week healing window. When a wound experiences tension (pulling forces from inflammation, stretching, or repeated reopening), cells called fibroblasts are mechanically stimulated to produce more collagen and lay it down in thicker bundles. This is a protective response: your body tries to create a stronger, more resilient bridge across the gap.
However, the trade-off is that this extra collagen is deposited less neatly, creating a wider area of scarring rather than a thin, linear closure. The depth and width of the final scar correlate directly with how much tension existed during weeks 1-3 of healing, when collagen is being actively laid down. A study examining surgical wound closure found that wounds sutured under low tension healed with scars one-third the width of wounds under high tension, even with identical initial wound size. This principle applies equally to acne scars: the moment you pick at a pimple and expose the dermis, if you then keep the wound under mechanical stress (touching it, squeezing nearby skin, or inflammatory swelling that pulls the edges open), you’re essentially programming your skin to create a broader scar.

The Tension-Scarring Connection Across Wound-Healing Phases
Understanding the three phases of wound healing—inflammation, proliferation, and remodeling—reveals why tension’s damage is so permanent. During the first week, inflammation causes swelling and redness; the wound edges are being held apart by fluid accumulation and inflammatory cytokines. If you then squeeze or pick at the inflamed acne lesion, you’re adding external mechanical stress on top of that inflammatory tension, which signals fibroblasts to work overtime. By week 2-3 (the proliferation phase), collagen deposition is in full swing. Any tension still present causes fibroblasts to align collagen fibers along the direction of that tension, creating a scar aligned with force lines rather than perpendicular to the skin surface.
The remodeling phase lasts months to years, but by then the scar pattern is already set. However, if you manage to keep the wound under minimal tension from day one—by avoiding picking, not stretching the skin, and using occlusive bandages or silicone to reduce inflammatory swelling—the collagen laid down during proliferation is more organized and narrower. The key limitation here: tension reduction is most effective in the first 2-4 weeks. Once the scar has matured (after 12+ weeks), tension-management strategies can still improve appearance slightly through scar tissue remodeling, but they won’t reverse an already-widened scar. Prevention is far more powerful than late-stage correction.
Which Acne Scar Types Are Most Worsened by Mechanical Tension?
Not all acne scars respond equally to tension. Atrophic scars (indented, depressed scars that look like pits or valleys) are primarily caused by loss of dermis during the infection or extraction process—tension doesn’t directly create these, but it does worsen them by creating wider pits. Hypertrophic and keloid scars, by contrast, are directly driven by excessive collagen deposition under tension. If you pick at an acne lesion and keep the wound edges separated by repeatedly touching or squeezing it, you create the perfect condition for a raised, thickened scar.
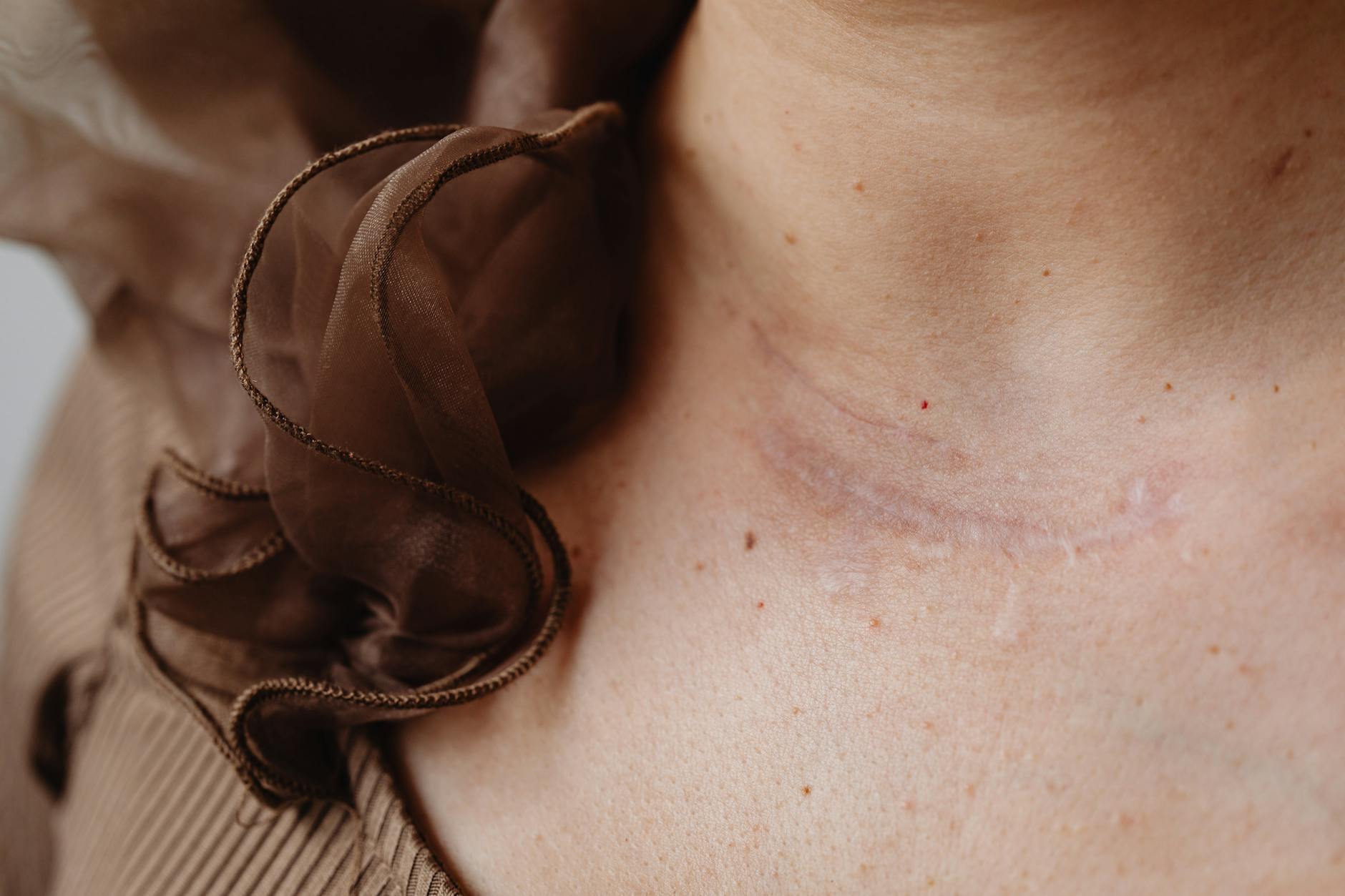
Icepick scars (narrow, deep pits) are less affected by tension than rolling scars (wider, undulating depressions), because tension tends to widen the scar opening, which exacerbates rolling scars more than it does narrow icepick scars. A common example: someone develops a cystic acne lesion and, unable to resist, repeatedly squeezes it over several days to “drain it.” Each squeeze creates new mechanical trauma and keeps the wound edges under tension. The result is typically a broader, more obvious scar than if they’d applied a warm compress instead and let the cyst drain naturally or resolve through oral antibiotics. This is especially true on the chest and shoulders, where skin is naturally looser and experiences more stretch during normal movement—these areas already have baseline mechanical tension, so acne scars there tend to be wider and more visible than identical lesions on the face, where skin is tighter.
Practical Methods to Minimize Mechanical Tension During Acne Healing
The most effective tension-reduction strategy is to stop introducing external mechanical trauma: don’t pick, squeeze, or repeatedly touch healing acne lesions. Use occlusive bandages or silicone patches (like pimple patches) to keep the wound moist and protected from touching, which reduces both inflammation-related swelling and the temptation to manipulate it. These barriers also flatten the area slightly, creating passive tension reduction. For more severe cystic acne, topical retinoids or azelaic acid can speed epithelialization, reducing the window during which the wound is vulnerable to tension damage.
Some dermatologists recommend taping the area with medical tape or scar tape after initial healing (weeks 2-4) to apply gentle, consistent low tension that encourages organized collagen alignment. Silicone gel sheeting is particularly effective because it reduces inflammation-driven swelling without adding external tension, allowing collagen to deposit in a tighter pattern. The downside is that it requires 12+ hours of daily contact for several weeks to see benefit, and it’s less practical on facial acne than on body acne. A comparison: occlusive pimple patches are more convenient for active acne (they can be worn under makeup), while silicone sheeting works better for early-stage scars (first 2-4 weeks post-healing). Avoiding certain movements also helps—if you have acne on your shoulders or chest, limiting upper-body stretching and wearing looser clothing during healing reduces baseline skin tension, which has been shown to narrow scars by 10-20% in some cases.
Common Mistakes That Increase Mechanical Tension on Acne Wounds
The biggest mistake is treating acne as a cosmetic problem to be “solved now” through aggressive extraction or squeezing. Each manipulation reopens the wound and resets the healing clock, meaning you might have a 6-week healing window that gets extended to 12 weeks because of repeated trauma. By then, collagen deposition has been stimulated multiple times under high-tension conditions, creating a much worse scar. Another mistake is using scrubs or exfoliants on healing acne.
Mechanical exfoliation tears at the delicate new skin forming over the lesion, keeping the wound open and under tension longer than it needs to be. A warning about this: if you have certain skin conditions like rosacea or eczema, your baseline inflammatory response is already elevated, which means your acne wounds are already under inflammatory tension even without picking. In these cases, tension-minimization strategies are even more critical. Additionally, some oral medications (like certain anticonvulsants or corticosteroids) slow collagen remodeling, which means scars are more permanent and more sensitive to initial tension conditions. If you’re on these medications and get acne, treating it conservatively to avoid wound trauma is especially important.

Comparison: Treated vs. Untreated Acne Scars from Tension Damage
A practical comparison illustrates the stakes. Someone with a severe pimple who aggressively squeezes it over one week, creating high mechanical trauma and keeping the wound open, typically develops a scar approximately 4-6mm wide with visible indentation. The same acne lesion on another person who resists picking, applies an occlusive patch, and waits for natural healing develops a scar 1-2mm wide with minimal visible depth.
Both started with identical acne severity, but the difference in final scar appearance is dramatic—the untreated (tension-minimized) scar is often barely noticeable, while the aggressively treated one remains visible for years. This difference is most obvious on the face, where you see your reflection regularly and where even small scars are visible. On the back or chest, where people are less likely to repeatedly examine the area and where healing happens with more baseline tension anyway, the difference is still significant but somewhat less dramatic because the final scars are broader regardless of management.
The Future of Tension-Guided Scar Prevention
Emerging research is exploring whether wearable devices or smart patches that monitor and apply precisely calibrated low tension to healing wounds could further reduce scarring. Some preliminary studies suggest that applying 5-10mmHg of continuous, gentle tension in specific directions can guide collagen alignment even better than current passive methods.
This is still experimental for acne scars specifically, but it’s being tested in surgical wound management with promising results. The practical takeaway: as dermatological technology improves, tension management will likely become an even more central part of scar prevention strategies. For now, the evidence is clear that minimizing mechanical stress on acne lesions during the first 4 weeks of healing produces measurably better scarring outcomes than aggressive extraction or repeated manipulation.
Conclusion
Mechanical tension on acne wounds directly drives worse scarring because of how your body’s collagen deposition responds to physical stress. Wounds under tension develop broader, more disorganized scar tissue, while wounds healing under minimal tension create tighter, nearly invisible scars.
The window to prevent this damage is narrow—primarily the first 2-4 weeks of healing—which is why resisting the urge to pick, squeeze, or repeatedly manipulate acne lesions is so important. Your most effective tools are simple: occlusive patches to protect from touching, avoidance of physical trauma, and allowing lesions to heal undisturbed. If you’ve already developed acne scars from tension damage, professional treatments like subcision, microneedling, or laser resurfacing can help, but prevention through tension minimization is far more effective and less costly than correction.
Frequently Asked Questions
If I already have acne scars from past picking, can tension-reduction strategies still help?
To a limited degree. Once a scar has fully matured (after 12+ weeks), tension management won’t significantly narrow it. However, applying silicone or occlusive products during the first few months after a scar forms may slightly improve texture and redness. Professional treatments are more effective at that stage.
How long do I need to avoid picking or manipulating a pimple to prevent tension scarring?
The critical window is the first 2-4 weeks. Avoid any picking or squeezing during this period. After 4 weeks, the scar pattern is largely set, though continued avoidance and sun protection still help with pigmentation and visibility.
Does acne location matter for tension-related scarring?
Yes. Areas with naturally looser skin (chest, shoulders, back) experience more baseline mechanical tension during movement, so acne scars there tend to be wider and more obvious even with minimal picking. Face and neck areas, where skin is tighter, show less scarring from identical acne under the same tension conditions.
Can silicone patches really prevent acne scars?
They can significantly reduce the risk if used from the moment a lesion opens or pus drains. They work by reducing inflammation-driven swelling and preventing external mechanical trauma. They’re most effective during the first 2-4 weeks of healing.
If I have cystic acne, what’s the tension-minimizing alternative to squeezing?
See a dermatologist for extractions under sterile conditions (which minimizes wound trauma), or use oral antibiotics and retinoids to resolve the cyst internally. Applying warm compresses may help drainage without picking, though professional intervention is often necessary for large cysts.
Does picking at a scab after acne healing restart the scarring process?
Yes, it resets the healing clock and reintroduces mechanical trauma to an area that was already under inflammatory tension. Avoid picking scabs; if a scab is uncomfortable, apply occlusive patches or moisturizer rather than removing it manually.
You Might Also Like
- Why Dehydration Makes Acne Scars Look Worse
- Why Pulse Duration Matters in Laser Selection for Acne Scars
- Why Histology of Acne Scars Guides Treatment Planning
Browse more: Acne | Acne Scars | Adults | Back | Blackheads





