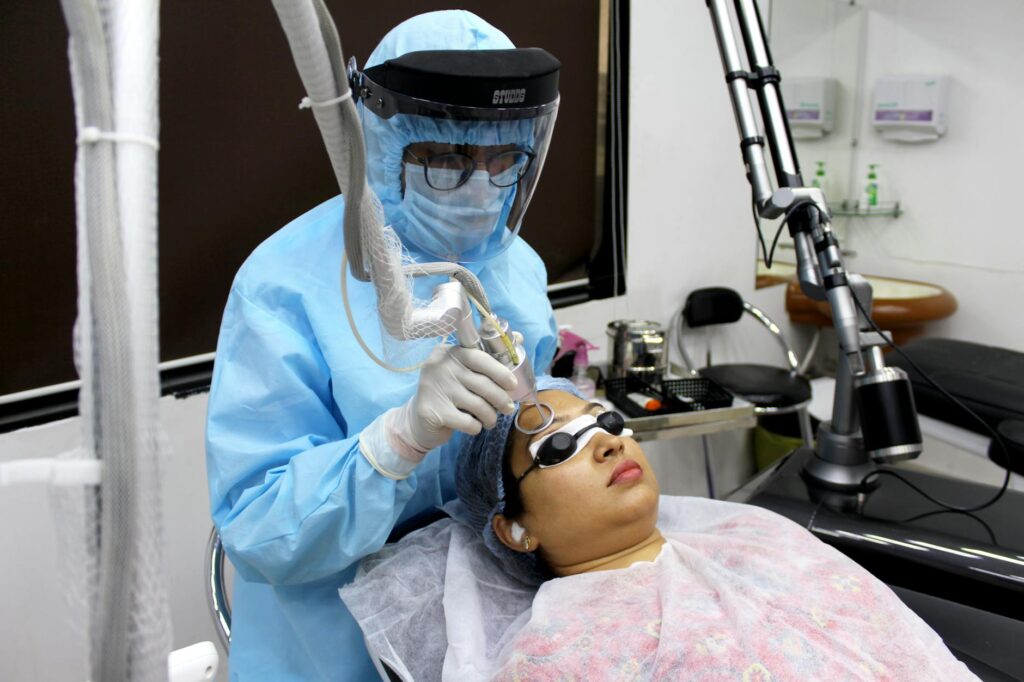
Laser treatments are used for persistent redness because they directly target and destroy the dilated blood vessels near your skin’s surface that cause the visible flushing. When light energy from the laser hits hemoglobin in red blood cells, it converts to heat that permanently damages the problematic capillaries responsible for the redness. This is why dermatologists increasingly recommend lasers for conditions like rosacea, post-inflammatory erythema, and general facial flushing—the treatments address the root cause rather than just masking symptoms. For example, someone with persistent redness across their cheeks and nose from rosacea can see dramatic improvements where topical creams have failed, with most patients achieving 50-75% reduction in visible blood vessels after just 1-3 treatments.
The mechanics behind laser redness treatment are elegant in their precision. Different laser wavelengths penetrate to different depths in your skin, allowing dermatologists to customize treatment based on vessel size and location. Longer wavelengths reach deeper blood vessels, while shorter wavelengths target superficial vessels near the epidermis. This article covers how these treatments work at a biological level, compares the different laser types currently available, explains what results you can realistically expect, and walks through important considerations like recovery time and durability of results.
Table of Contents
- How Do Lasers Target and Eliminate Redness-Causing Blood Vessels?
- What Are the Most Effective Laser Types for Treating Persistent Redness?
- What Results Can You Realistically Expect After Treatment?
- How Do Different Laser Types Compare in Terms of Comfort, Recovery, and Downtime?
- What Are the Risks, Limitations, and Who Should Avoid Laser Treatment for Redness?
- What Does the Recent 2025 Research Tell Us About Laser Effectiveness and Innovation?
- The Future of Laser and Light Therapy for Persistent Redness
- Conclusion
How Do Lasers Target and Eliminate Redness-Causing Blood Vessels?
The process begins with selective photothermolysis—a scientific principle where laser light is absorbed by a specific target (in this case, hemoglobin) while leaving surrounding tissue relatively unharmed. When the laser beam passes through your skin, the hemoglobin in red blood cells absorbs the light energy and converts it to thermal energy. This heat damages the blood vessel walls, causing them to collapse and eventually be reabsorbed by your body. The surrounding healthy skin tissue remains largely unaffected because it doesn’t absorb the specific wavelength being used, which is why lasers are so much more targeted than older treatments like chemical peels. The depth at which a laser works depends entirely on its wavelength. Think of it like adjusting how deep a stone sinks into water—the right angle and force determine the depth. Longer wavelengths (like those in neodymium lasers) penetrate deeper into the dermis to reach larger, deeper blood vessels.
Shorter wavelengths (like those in pulsed dye lasers) stay closer to the surface and are ideal for superficial capillaries and telangiectasia. This is why a dermatologist won’t use the same laser for everyone; they’ll select the wavelength and settings based on your specific redness pattern, skin type, and vessel depth. For someone with deep facial flushing from rosacea, a longer-wavelength laser might be the better choice, whereas someone with surface-level broken capillaries might benefit more from a shorter-wavelength option. Importantly, the lasers used for redness treatment are selective—they damage the blood vessels but don’t destroy the surrounding skin structure. The vessel walls are stripped of their endothelial cells and collagen, causing them to collapse. Once collapsed, your body’s lymphatic system gradually removes the damaged vessel debris over weeks to months. The treated blood vessels do not reappear once destroyed, which is why results can last 3-5 years. However, if you remain exposed to the same triggers (sun damage, rosacea flare factors, heat), new blood vessels can form over time, which is why some patients need maintenance treatments years later.

What Are the Most Effective Laser Types for Treating Persistent Redness?
Several laser and light technologies have proven track records for treating facial redness, each with slightly different strengths and tradeoffs. The Pulsed Dye Laser (PDL) remains the gold standard for many dermatologists, offering a balanced therapeutic profile with strong efficacy and fewer adverse events compared to older alternatives. PDL is particularly effective for rosacea and post-inflammatory erythema, with clinical studies showing consistent improvement rates. The KTP laser (potassium-titanyl-phosphate) is another excellent option, and some recent analyses suggest patients report higher satisfaction with KTP compared to PDL, along with faster recovery times and better treatment comfort. If you’re considering these two, the choice often comes down to your skin type, pain tolerance during treatment, and how quickly you need to return to normal activities. For deeper redness and larger vessel involvement, the Long-Pulsed Alexandrite Laser (LPAL) shows favorable results, and a 2025 prospective clinical trial specifically examined its effectiveness on facial redness and skin microbiota. The latest comparison data also highlights IPL (Intense Pulsed Light), which technically isn’t a true laser but functions similarly—most patients achieve excellent or satisfactory improvement with IPL for rosacea and general redness.
More recently, radiofrequency microneedling has emerged as a compelling option, with 2025-2026 analysis showing it may actually be superior to traditional lasers for rosacea erythema, delivering excellent patient satisfaction scores. The trade-off is that RF microneedling often requires more sessions and may have slightly longer recovery, but patients who’ve struggled with traditional lasers sometimes see better results with this approach. When choosing between these options, understand that effectiveness varies by redness type. For erythematotelangiectatic rosacea (the form with prominent redness and visible vessels), neodymium laser studies showed a 79.5% mean reduction in lesion severity—these are dramatic results. For papulopustular rosacea (with bumps and pustules alongside redness), the mean reduction was 63.0%—still significant but slightly lower. For general facial redness without an underlying rosacea diagnosis, you’re looking at approximately 20% reduction on average, though individual results vary widely. The takeaway: if you have rosacea with obvious blood vessels, you’ll likely see more dramatic improvement than someone with diffuse, vague redness. Your dermatologist should discuss which laser type and expected improvement percentage applies to your specific situation.
What Results Can You Realistically Expect After Treatment?
Most patients experience noticeable improvement within 2-4 weeks as the treated blood vessels are gradually reabsorbed and inflammation subsides. However, the full results unfold over 2-3 months. In clinical practice, 50-75% reduction in visible blood vessels is typical after 1-3 laser sessions, though some patients require additional treatments to reach their desired outcome. This means if you walk in with significantly flushed cheeks, you’ll likely see your skin tone return much closer to your baseline—red patches fade, broken capillaries disappear, and the overall ruddy appearance lessens considerably. It’s not always a complete eradication of redness, but the change is substantial enough to transform how people feel about their appearance. Duration of results is one of the major selling points of laser treatment: results typically last 3-5 years. This longevity occurs because the damaged blood vessels are genuinely destroyed and removed—they don’t come back. Compare this to topical treatments (which work only while you use them) or oral medications (which require continuous use), and you understand why so many dermatologists and patients favor lasers for persistent redness.
A single treatment or series can give you years of clearer skin, which often justifies the cost and downtime. However, this doesn’t mean your redness will never return. New blood vessels can form over time if you’re exposed to the same triggers—sun exposure, temperature extremes, spicy foods, alcohol, or stress if you have rosacea. A 2020 study found significant improvement in facial redness with reduced symptom recurrence over a 2-year period, suggesting the benefits are durable even as some underlying triggers persist. One important caveat: not everyone responds equally to laser treatment. Skin type, vessel characteristics, and the specific cause of your redness all influence outcomes. Someone with pale skin, superficial telangiectasia, and mild rosacea might see 80%+ improvement with a single treatment. Someone with deeper redness, larger vessel involvement, or darker skin tone might need more sessions and achieve a more modest improvement percentage. This is why a thorough consultation with a dermatologist is essential—they can assess your specific situation and give you honest expectations rather than promising universal, dramatic results for everyone.

How Do Different Laser Types Compare in Terms of Comfort, Recovery, and Downtime?
Treatment comfort and recovery time are practical considerations that often influence which laser a patient chooses. The Pulsed Dye Laser feels like rapid snapping sensations against your skin—uncomfortable but usually tolerable without anesthesia, though topical numbing cream can help. Most PDL treatments take 15-30 minutes depending on treatment area size. Recovery involves mild redness and possible bruising (purpura) that typically fades within 7-14 days. KTP lasers generally produce less bruising than PDL and have a similar or slightly shorter recovery window, which is one reason some patients prefer them—you can return to normal activities and makeup use faster. IPL treatments feel similar to PDL and have comparable recovery times. The Long-Pulsed Alexandrite Laser tends to be well-tolerated with minimal bruising and faster healing, making it attractive for patients who can’t afford significant downtime.
However, it may require more sessions for complete results. Radiofrequency microneedling involves tiny needles combined with RF energy, which sounds intimidating but many patients report it’s actually less uncomfortable than laser during treatment—the real trade-off is that downtime can be longer (1-2 weeks of visible redness and possibly peeling) and you typically need more sessions (4-6 spaced 4 weeks apart) compared to 1-3 laser sessions. This explains why RF microneedling appeals to patient satisfaction ratings even though it requires more commitment—some people prefer one uncomfortable laser treatment with weeks of recovery to multiple gentler treatments. A practical example: someone with a wedding in four weeks should probably avoid PDL in week one because of potential bruising visibility. They might choose KTP or Alexandrite for faster healing, or even opt for radiofrequency microneedling if they have time for multiple sessions before the event. Conversely, someone willing to invest time upfront for potentially superior results might choose the treatment requiring most sessions. These aren’t medical trade-offs—they’re lifestyle trade-offs, which is why discussing your schedule and preferences with your dermatologist matters as much as the clinical effectiveness data.
What Are the Risks, Limitations, and Who Should Avoid Laser Treatment for Redness?
While laser treatment for redness is generally safe, certain complications can occur, and some patients aren’t good candidates. The most common side effects are temporary redness, swelling, and bruising at the treatment site—these resolve within days to weeks. More serious but rare complications include blistering, infection, scarring, or paradoxical worsening of rosacea (though this is uncommon and usually resolves with proper post-treatment care). Patients taking isotretinoin (Accutane) for severe acne, those with active infections or cold sores, or people with very dark skin tones (where the laser may not effectively target blood vessels and carries higher risk of pigmentation changes) should avoid laser redness treatment or discuss extensively with a dermatologist first. Sun exposure is a critical limitation both before and after treatment. If you’re planning laser treatment, you must commit to strict sun avoidance for at least 2-4 weeks before and after—sun exposure can increase bruising risk, impair healing, and reduce treatment effectiveness. Sunscreen alone isn’t enough during this period; you need physical barriers like hats and staying indoors. If you live a lifestyle involving frequent sun exposure and won’t protect your skin adequately, the results won’t be as good and the risk of complications rises.
Similarly, if your redness is caused by something lasers can’t address—like severe dehydration, internal heat, or emotional flushing—the treatment might show minimal benefit. A dermatologist should rule out underlying conditions and ensure you’re a good candidate before proceeding. Another limitation to acknowledge: persistence of redness. Some patients experience recurrence of rosacea symptoms or redness even after successful initial treatment. This isn’t because the treatment failed; it’s because the underlying triggers (genetic predisposition to rosacea, sun damage, environmental factors) remain active. The laser addresses the visible blood vessels, but it doesn’t cure rosacea at a systemic level. You might still need to manage triggers, use gentle skincare, and possibly take oral or topical medications alongside laser treatment for optimal, sustained results. Laser works best as part of a comprehensive rosacea management plan, not as a standalone cure.

What Does the Recent 2025 Research Tell Us About Laser Effectiveness and Innovation?
Recent clinical research continues to refine our understanding of which lasers work best and under what conditions. A 2025 prospective, multicentre clinical trial specifically examined long-pulsed alexandrite laser therapy for facial redness and its effects on skin microbiota—the bacterial communities living on your skin. This research suggests that laser treatment doesn’t just eliminate blood vessels; it may also modulate the skin microbiota in ways that reduce rosacea flares, which could explain why some patients experience sustained improvement beyond simple vessel destruction.
A comprehensive 2025 review published by MDPI analyzed the application of PDL, KTP, IPL, and Nd:YAG lasers for rosacea management, synthesizing evidence from multiple clinical trials to provide updated recommendations. The emerging picture from 2025-2026 research is that no single laser is universally superior—rather, the best choice depends on your specific redness type, skin characteristics, and practical constraints. Radiofrequency microneedling’s rise in the literature reflects its strong clinical outcomes, but PDL and KTP remain highly effective and faster for patients seeking quick results. The field is also moving toward combination therapies, where laser treatment is paired with skincare modifications, avoidance of triggers, and sometimes oral medications, creating better overall outcomes than laser alone.
The Future of Laser and Light Therapy for Persistent Redness
As technology evolves, we’re seeing refinements in laser systems that offer better precision, faster treatment times, and reduced complications. Newer laser systems have improved cooling mechanisms to protect surrounding tissue, variable pulse widths to customize treatment to different vessel sizes, and real-time feedback systems to adjust energy delivery.
The growing evidence supporting radiofrequency microneedling and combination therapies suggests that future treatment protocols will likely move away from “one laser fits all” toward personalized approaches based on your specific redness etiology and skin type. Looking forward, research into the relationship between skin microbiota and rosacea-related redness might lead to lasers combined with targeted probiotic or microbiota-modulating treatments. For now, if you’re considering laser treatment for persistent redness, the evidence strongly supports its effectiveness, safety, and durability—with the caveat that results vary by individual and the best outcomes come from choosing the right laser type with a qualified dermatologist and committing to proper pre- and post-treatment care.
Conclusion
Laser treatments effectively address persistent redness by selectively destroying the dilated blood vessels responsible for facial flushing through selective photothermolysis—the conversion of light energy into targeted heat. Most patients achieve 50-75% reduction in visible blood vessels after 1-3 treatments, with results lasting 3-5 years because the treated vessels are permanently removed. Multiple laser types (PDL, KTP, LPAL, IPL) and emerging technologies like radiofrequency microneedling each offer different advantages in terms of comfort, recovery time, and results, making it essential to discuss your specific goals and constraints with a dermatologist.
The decision to pursue laser treatment should be made in consultation with a qualified dermatologist who can assess your redness type, skin characteristics, and candidacy. While laser is highly effective, it works best as part of comprehensive rosacea management that includes trigger avoidance, sun protection, and potentially skincare modifications or medications. Recent 2025 research continues to refine our understanding of which lasers work best and hints at future personalized approaches, but for persistent redness today, evidence supports laser therapy as one of the most durable and effective options available.
You Might Also Like
- What Happens When You Combine Too Many Treatments for Redness
- Why Gel Cleansers Are Often Recommended for Acne Prone Skin
- What Happens When You Treat Redness With Harsh Ingredients
Browse more: Acne | Acne Scars | Adults | Back | Blackheads