Dermatology residency programs shape acne treatment norms by embedding the American Academy of Dermatology’s evidence-based guidelines directly into standardized curricula that all residents complete. Every dermatology trainee in an ACGME-accredited program learns the same core acne therapies—benzoyl peroxide, topical retinoids, topical antibiotics, oral doxycycline, and isotretinoin—along with the latest FDA-approved treatments and emerging laser technologies. This ensures that whether a patient sees a dermatologist in Seattle or Miami, they receive care grounded in the same clinical evidence. The result is that residency training doesn’t just educate individual physicians; it codifies which treatments become standard practice nationwide.
This article explores how residency programs establish these norms, the guidelines they teach from, the therapies residents master, and how those training pathways directly influence the acne treatments available and recommended in your dermatologist’s office. The power of residency education lies in its scope and mandate. ACGME accreditation requires that all dermatology programs teach pharmacologic therapeutics covering every acne treatment modality—from topical agents to systemic therapies to cutting-edge lasers. Residents also attend periodic Acne and Rosacea Symposia as part of their structured curriculum, exposing them to the latest research and clinical innovations. Because residency training is the gateway to becoming a licensed dermatologist, the treatments emphasized in these programs become the treatments that dominate clinical practice.
Table of Contents
- How Do Residency Programs Establish Treatment Standards for Acne?
- The Role of Evidence-Based Guidelines in Residency Curricula
- Training in Conventional and Emerging Acne Therapies
- The Impact of Standardized Training on Clinical Practice
- Advanced and Laser Therapies in Modern Acne Residency
- Ensuring Equitable Care: Skin of Color in Dermatology Education
- The Future of Acne Treatment Norms and Residency Education
- Conclusion
How Do Residency Programs Establish Treatment Standards for Acne?
Dermatology residency training is not left to chance or individual faculty preferences. The ACGME establishes Program Requirements that all accredited residencies must follow, including core competencies in patient care, medical knowledge, practice-based learning, communication, and professionalism. within this framework, acne management is a required curriculum component. Every resident must develop competency in diagnosing acne across skin types, understanding the pathophysiology of acne (follicular obstruction, sebaceous gland dysfunction, bacterial colonization, and inflammation), and selecting appropriate treatments for mild, moderate, and severe cases. What makes residency training powerful is that it creates a common language and shared evidence base.
A dermatologist trained in New York and one trained in Arizona both learned from the same ACGME guidelines and the same AAD recommendations. They were taught to assess acne severity in the same way, to recognize contraindications to the same medications, and to escalate to systemic therapy or isotretinoin using the same criteria. This standardization doesn’t happen by accident—it’s the direct result of how residency programs structure their educational requirements and how they train the next generation of specialists. The comparison here is instructive: dermatology differs markedly from general practice, where many family medicine physicians and nurse practitioners treat acne without the same depth of training. A family medicine resident might spend a few weeks on dermatology total; a dermatology resident spends three years with acne management woven throughout their training. That difference in exposure directly translates to differences in clinical practice patterns.

The Role of Evidence-Based Guidelines in Residency Curricula
The 2024 American Academy of Dermatology Clinical Guidelines for acne management form the backbone of what residents learn. These guidelines include 18 evidence-based recommendations and 5 good practice statements covering everything from initial assessment to maintenance therapy to treatment of severe cases. Residency programs don’t create their own treatment protocols from scratch; they teach residents how to implement AAD-endorsed approaches. Strong recommendations in the current guidelines favor benzoyl peroxide, topical retinoids, topical antibiotics, and oral doxycycline for mild to moderate acne, while isotretinoin is strongly recommended for severe acne, cases causing psychosocial burden, therapy-resistant cases, or cases likely to cause scarring. One theme that has strengthened in recent years is antibiotic stewardship.
The AAD guidelines now emphasize limiting oral antibiotic use to reduce antibiotic resistance development—a major public health concern. Residents are trained that antibiotics should not be monotherapy and should not be used long-term without additional acne medications. This represents a shift in acne treatment norms over the past decade. However, this guideline emphasis only applies to bacterial acne (inflammatory lesions with possible bacterial involvement); purely comedonal acne, where bacteria play a lesser role, may be treated differently with retinoids and other non-antibiotic agents. The limitation here is that some patients and even some providers still over-prescribe antibiotics for types of acne where they’re less effective, a practice residency training aims to correct.
Training in Conventional and Emerging Acne Therapies
Residency curricula cover the full spectrum of acne treatments, from foundational therapies to the newest FDA approvals. Residents master the mechanism of action, efficacy data, side effects, and appropriate patient selection for benzoyl peroxide (antibacterial and comedolytic), topical retinoids like adapalene and tretinoin (normalize keratinization), and topical antibiotics like clindamycin (bacteriostatic effect). They learn when to escalate to oral doxycycline (anti-inflammatory and antibiotic properties), when isotretinoin is indicated (the only treatment targeting all four pillars of acne pathogenesis: sebum production, follicular plugging, bacterial colonization, and inflammation), and how to manage isotretinoin’s serious side effects through the iPLEDGE program. In recent years, residency programs have updated their curricula to include newly FDA-approved medications.
Winlevi (clascoterone), approved in 2020, is the first and only topical therapy specifically targeting excessive sebum production—a fundamental driver of acne. A 2024 fixed-dose combination therapy combining clindamycin, adapalene, and benzoyl peroxide was noted as the most efficacious single-agent topical treatment currently available, reflecting advances in understanding how combination therapy works better than monotherapy. Residents now learn not just the old standby combinations but these newer approaches as they’re adopted into practice guidelines. A concrete example: a resident in 2024 learning acne management will be taught Winlevi as a topical option for patients with oily skin and comedonal or mild inflammatory acne, whereas a dermatologist trained in 2015 might not have learned about it at all. This difference in training directly leads to differences in what treatments get offered to patients.

The Impact of Standardized Training on Clinical Practice
Because dermatology residency training is standardized nationwide, it creates conformity in acne treatment norms across different regions and practice settings. A patient visiting a private practice dermatologist in California should encounter similar first-line treatment recommendations as a patient visiting a university dermatology clinic in North Carolina, simply because both physicians completed comparable residency training. This standardization has significant advantages: it means evidence-based, proven treatments are consistently accessible rather than dependent on a particular provider’s idiosyncratic preferences. The tradeoff is that standardization can sometimes lag behind innovation.
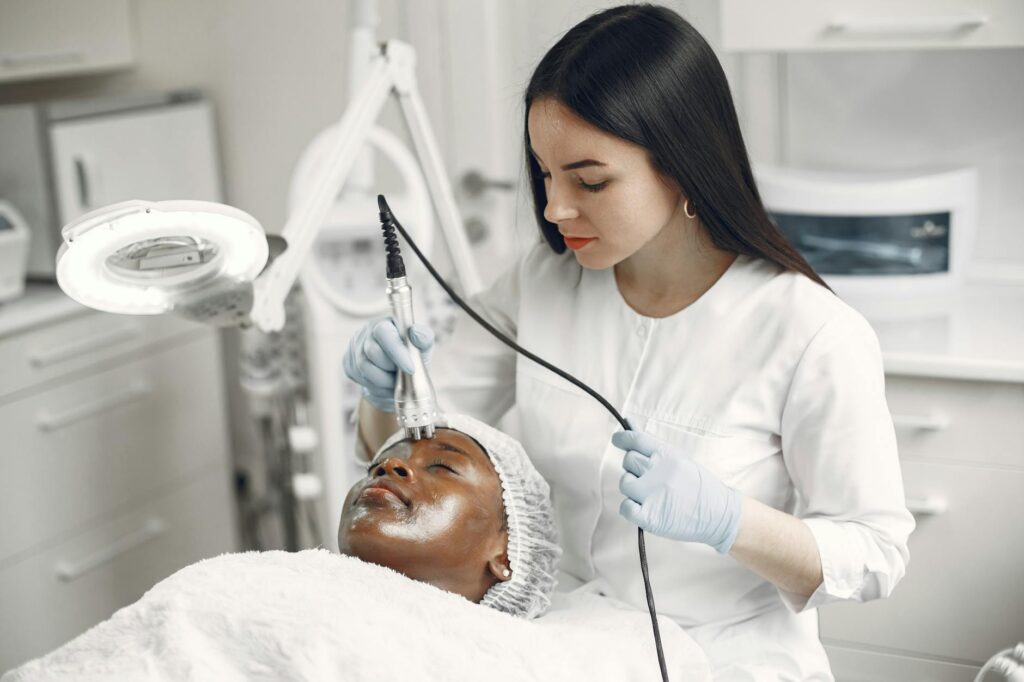
Newer treatments or emerging data take time to filter into residency curricula and then into widespread practice. For instance, if a breakthrough acne treatment were published today, it might be 2–3 years before it becomes standard residency curriculum material and longer still before it’s adopted into AAD guidelines. During that gap, early adopters or practices near academic medical centers might have access to the new treatment, while other regions lag behind. A practical example: the rise of laser therapy for acne represents a case where residency training has had to evolve. Older residency programs may have taught lasers as a niche therapy; current programs are integrating newer 1726-nanometer laser technology (available through devices like AviClear and Accure) that directly targets sebaceous glands as part of the standard curriculum.
Advanced and Laser Therapies in Modern Acne Residency
Modern dermatology residency programs now include training in advanced acne therapies, particularly laser and light-based treatments. The 1726-nanometer lasers that selectively target sebaceous glands represent a significant addition to the armamentarium, with clinical outcomes showing that approximately 40% of moderate to severe acne patients achieve clear or almost clear skin for up to 6 months post-treatment. Residents learn when laser therapy is appropriate (typically for patients who have failed conventional treatments or prefer a non-pharmacologic approach) and its limitations (results are not permanent; maintenance treatments may be needed).
However, laser therapy has important constraints that residents must understand. The 6-month durability of results means patients need to consider ongoing costs and time commitment for maintenance. Additionally, laser therapy works best for certain acne phenotypes and may be less effective in patients with active severe inflammatory acne or certain darker skin types where the technology is less developed. The emphasis in modern residency training is that lasers complement conventional therapy rather than replace it for most patients.

Ensuring Equitable Care: Skin of Color in Dermatology Education
A significant evolution in dermatology residency training is the increasing emphasis on skin of color presentations and addressing diagnostic and treatment disparities. Historically, acne guidelines and residency curricula were developed with limited diversity in the patient populations studied, leading to underdiagnosis and undertreatment of acne in patients with darker skin tones, particularly patients with skin types IV–VI. Current residency programs now actively teach how acne presents differently across skin tones—post-inflammatory hyperpigmentation is more common and can be distressing, certain inflammatory morphologies are more prevalent, and some treatments have different efficacy or side effect profiles depending on skin type.
The 2024 DERM Conference, which offered 20+ hours of CME credit covering acne management, reflects this evolution. Programs increasingly dedicate curriculum time to ensuring residents understand how to diagnose and treat acne equitably. This shift directly impacts patient outcomes: residents trained with this knowledge are more likely to offer the same evidence-based treatments to all patients, rather than potentially underrecognizing or under-treating acne in patients of color.
The Future of Acne Treatment Norms and Residency Education
As new acne therapies continue to emerge and resistance to antibiotics remains a public health priority, dermatology residency programs will continue evolving their curricula. The emphasis on antibiotic stewardship is expected to grow, meaning future residents will likely be trained with even more restrictive guidelines around when oral antibiotics are appropriate. Simultaneously, as laser and other device-based therapies improve, residency programs will likely expand training in these modalities.
The trajectory suggests that acne treatment norms will become increasingly personalized and multimodal. Residents will be trained to select from a wider toolkit—conventional topical and systemic therapies, newer medications targeting specific pathophysiologic drivers, and advanced laser treatments—based on individual patient factors including acne severity, skin type, treatment preferences, and prior treatment response. This evolution in residency training will shape how acne care is delivered for decades to come.
Conclusion
Dermatology residency programs shape acne treatment norms through standardized ACGME-accredited curricula that embed the latest evidence-based guidelines into training for every resident. By requiring competency in the full range of acne therapies—from benzoyl peroxide and retinoids to isotretinoin to cutting-edge lasers—residency programs ensure that the treatments that dominate clinical practice are grounded in clinical evidence rather than individual whim.
The 2024 AAD guidelines with their 18 recommendations, the emphasis on antibiotic stewardship, and the growing focus on equitable care across skin tones all flow directly from decisions made in residency training. If you’re seeking acne treatment, understanding that your dermatologist’s recommendations are informed by standardized residency training and evidence-based guidelines may provide confidence that you’re receiving care grounded in rigorous clinical evidence. If you’re considering dermatology as a career, know that the field’s commitment to residency training ensures that acne management—one of dermatology’s most common clinical tasks—continues to improve through systematic education and continuous guideline updates.
You Might Also Like
- What Acne Research Funding Gaps Mean for Treatment Progress
- Why Iron Supplements Cause Acne in Some People
- Why Curcumin Supplements Help Inflammatory Acne
Browse more: Acne | Acne Scars | Adults | Back | Blackheads