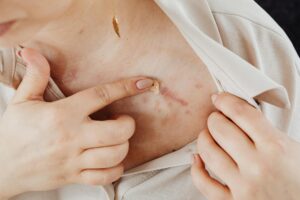
Compound pharmacies offer custom acne formulas because they can combine multiple active ingredients—like tretinoin, benzoyl peroxide, clindamycin, and others—in precise concentrations tailored to your specific skin type and acne severity. Instead of juggling three or four separate medications from your dermatologist, you pick up a single personalized cream or gel that addresses multiple causes of acne at once. With up to 50 million Americans affected by acne annually, this customization approach fills a critical gap: off-the-shelf products use fixed doses that don’t work for everyone, while compounded formulations allow dermatologists and pharmacists to fine-tune treatment plans to match individual skin chemistry and acne patterns. This article explores why compound pharmacies have become essential partners in acne treatment, how they build these custom formulas, what benefits patients actually experience, and what to know before you ask your dermatologist for a compounded prescription.
Table of Contents
- What Can Compound Pharmacies Actually Combine?
- How Customization Improves Patient Outcomes and Compliance
- The Economics: Why Compounded Formulas Cost Less Than Multiple Medications
- New and Emerging Compound Formulations
- The Regulatory Reality: What “Not FDA-Approved” Actually Means
- Working with Your Dermatologist and Pharmacist to Design Your Formula
- The Future of Compound Acne Treatment
- Conclusion
What Can Compound Pharmacies Actually Combine?
Compounding pharmacists have access to a much broader ingredient palette than commercial acne products. They can combine tretinoin (a retinoid that reduces sebum production and accelerates skin turnover), benzoyl peroxide (which kills acne-causing bacteria), clindamycin (an antibiotic that reduces bacterial colonies on skin), salicylic acid (an exfoliant that prevents pore clogging), hydroquinone (for post-inflammatory hyperpigmentation), kojic acid (another skin-lightening agent), niacinamide (which reduces sebum production and inflammation), and tranexamic acid (which addresses redness and may help with hormonal acne). A dermatologist might prescribe a formula containing tretinoin 0.05%, benzoyl peroxide 3%, and niacinamide 4%, for example—a combination that addresses bacterial growth, cell turnover, and inflammation in a single application. This flexibility matters because acne doesn’t have a one-size-fits-all cause.
Someone with oily, bacterial acne benefits from higher benzoyl peroxide. Someone with sensitive skin prone to redness needs gentler concentrations and added anti-inflammatory agents like niacinamide. Someone dealing with hormonal acne might benefit from spironolactone in topical form. However, not all combinations work well together—some ingredients can interact or destabilize in formulation—so dermatologists and pharmacists collaborate to design stable, effective blends.

How Customization Improves Patient Outcomes and Compliance
When a dermatologist prescribes multiple separate products, patients often struggle with how to apply them, in what order, and at what strength. Using tretinoin at night, then benzoyl peroxide in the morning, plus a separate niacinamide serum, creates confusion and reduces the likelihood that patients actually follow the regimen as prescribed. Research shows that compounded acne medications that combine multiple agents into a single formula significantly improve patient compliance, which directly translates to better clinical outcomes and faster acne clearance.
The single-formula approach also reduces irritation and side effects. Instead of layering multiple actives that might over-dry the skin or cause irritation when combined, a compounding pharmacist can formulate a stable product where ingredients work synergistically. One medication fights bacterial growth, another accelerates cell turnover, a third reduces inflammation—all from one application. This targeted multi-mechanism approach means patients achieve results faster and experience fewer side effects from over-application or accidental interactions between separate products.
The Economics: Why Compounded Formulas Cost Less Than Multiple Medications
Buying commercial tretinoin cream, benzoyl peroxide wash, clindamycin lotion, and a separate niacinamide serum easily adds up to $100–$200 monthly, especially with insurance gaps or brand-name premiums. A single compounded formula combining multiple active ingredients typically costs $30–$60 per month—sometimes less if your pharmacy sources ingredients in bulk or your dermatologist is mindful of cost. Patients pay for one compounded medication rather than buying multiple commercial products separately, making custom formulations significantly more affordable for long-term acne management.
Clinical research confirms that compounded formulations deliver equivalent efficacy to brand-name alternatives while remaining cost-effective. Studies show that generic and compounded formulas—including fixed-dose combinations like generic adapalene–benzoyl peroxide and clindamycin-benzoyl peroxide—are highly cost-effective for mild-to-moderate acne without sacrificing results. For severe or treatment-resistant acne, the ability to customize and adjust concentrations without switching between multiple medications often means fewer dermatology visits and faster resolution, offsetting any minor cost difference compared to off-the-shelf options.

New and Emerging Compound Formulations
Compounding pharmacies don’t simply mix old ingredients in new ways—they’re developing newer formulations that represent advances in acne treatment. One example is Acne DNS Gel, a fast-drying formulation combining dapsone 6%, niacinamide 2%, and spironolactone 5%. This triple-action formula targets bacterial infection (dapsone), inflammation and sebum production (niacinamide), and hormonal contributors to acne (spironolactone).
It’s designed for once- or twice-daily application without the drying effects of older tretinoin-benzoyl peroxide combos, making it cosmetically elegant enough for professional or social settings. These newer formulations reflect dermatology’s evolving understanding of acne pathophysiology. Rather than relying solely on tried-and-true ingredients like benzoyl peroxide, modern compounds incorporate gentler actives like tranexamic acid (which appears to help with post-inflammatory erythema) and adjust niacinamide ratios to maximize anti-sebum effects without irritation. Compounding allows pharmacists to test and refine these combinations quickly, adapting to new clinical evidence as it emerges—something commercial manufacturers with fixed production lines cannot easily do.
The Regulatory Reality: What “Not FDA-Approved” Actually Means
Compounded medications exist in a unique regulatory space: they are not reviewed by the FDA for safety or efficacy the way commercial products are. This doesn’t mean they’re unsafe or ineffective—it means they bypass the FDA approval pathway. The FDA recognizes and permits compounding under the Pharmacy Compounding Accreditation Board (PCAB) standards and state pharmacy board oversight. However, you should know that there’s no third-party verification that your compounded formula is what the label says it is, or that it’s been stability-tested like commercial products.
This limitation is meaningful if you have severe allergies, take immunosuppressant medications, or have conditions that make pharmaceutical purity critical. Most people tolerate compounded acne treatments without issue, and compounding pharmacies accredited through PCAB follow strict quality standards. However, if you develop an unexpected reaction, you won’t have the same FDA-backed safety reporting infrastructure as you would with a brand-name product. Always inform your dermatologist and pharmacist about all medications and supplements you’re taking, especially if you’re pregnant or nursing—compounded medications carry the same pregnancy warnings as their individual active ingredients.

Working with Your Dermatologist and Pharmacist to Design Your Formula
A good compounded acne formula starts with a detailed conversation between you, your dermatologist, and the compounding pharmacist. Your dermatologist reviews your acne type (bacterial, inflammatory, hormonal, cystic), skin sensitivity, and any previous treatments that worked or failed. They may prescribe a specific combination—for example, tretinoin 0.05%, benzoyl peroxide 3%, and hydroquinone 2%—leaving the exact formulation to the pharmacist’s judgment. The pharmacist then decides on the base (cream, gel, or lotion), adjusts concentrations if needed for stability, and may suggest tweaks for better tolerability.
If you’re prone to dryness, they might recommend a more emollient base. If you have oily skin, a lighter gel base works better. This collaboration is where compounding shines—it’s personalized medicine in dermatology. Don’t hesitate to loop back after 4–6 weeks if the formula isn’t working as hoped; pharmacists can often adjust concentrations or swap an ingredient without requiring a new prescription.
The Future of Compound Acne Treatment
As dermatologists grow more comfortable prescribing custom formulations, and as clinical evidence accumulates around multi-ingredient combinations, compounding will likely become a first-line option for moderate acne rather than a last resort. Newer ingredients—like azelaic acid, sulfur-based compounds, and even botanical extracts—are being tested in compounding labs.
The ability to rapidly prototype and adjust formulations gives compounding an advantage in acne research and innovation that centralized pharmaceutical manufacturers cannot match. The trend also reflects a broader shift toward precision medicine in dermatology. Instead of prescribing the same tretinoin cream to every patient, dermatologists can now say, “Based on your skin type and acne triggers, here’s your specific formula.” As more insurance plans recognize the cost-effectiveness of compounded acne treatments, and as pharmacy networks expand access to accredited compounding facilities, this personalized approach becomes increasingly practical for anyone dealing with treatment-resistant acne.
Conclusion
Compound pharmacies offer custom acne formulas because they can combine multiple active ingredients—tretinoin, benzoyl peroxide, clindamycin, niacinamide, and others—in precise ratios tailored to your unique skin chemistry and acne type. This flexibility delivers clinical benefits that off-the-shelf products cannot match: improved compliance through single-formula convenience, simultaneous targeting of multiple acne causes, and significantly lower costs than buying multiple separate medications.
For the 50 million Americans affected by acne annually, customized compounding represents a practical bridge between generic commercial products and prescription-only pharmaceuticals. If your acne isn’t responding to standard treatments, or if you’re managing multiple medications without good results, ask your dermatologist about compounding. Be transparent about your skin sensitivity, any allergies, and your lifestyle—does your job require minimal visible irritation?—so your dermatologist and pharmacist can design a formula that works for your life, not just your acne.
You Might Also Like
- Why Tretinoin Microsphere Is Better for Sensitive Acne Skin
- Why Tactupump Is Popular in Canada for Acne Treatment
- Why Skin1004 Madagascar Centella Ampoule Helps Acne
Browse more: Acne | Acne Scars | Adults | Back | Blackheads