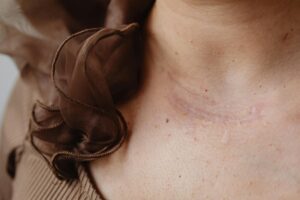
The short answer is that most insurance companies classify a significant portion of acne treatments as “cosmetic” rather than “medically necessary,” which gives them grounds to deny coverage outright. This distinction is often arbitrary. A teenager with severe cystic acne that causes deep scarring and clinical depression faces the same insurance bureaucracy as someone requesting an elective cosmetic procedure. The result is that acne, which affects up to 50 million Americans annually and is the single most common skin condition in the country, gets treated by the healthcare system as something closer to a vanity concern than the legitimate medical condition it is. The financial fallout is real.
A full course of isotretinoin, the most effective treatment for severe acne, can run $3,000 to $5,000 or more out of pocket when you factor in monthly dermatologist visits, lab work, and the medication itself. Brand-name Accutane alone costs $200 to $700 per month without insurance. And yet only about 10 percent of acne sufferers ever consult a dermatologist, with the majority relying on over-the-counter products that may not address their condition. Over $6 billion is spent annually on acne treatments in the U.S., and a disproportionate share of that burden falls on patients and families rather than insurers. This article breaks down the specific reasons insurance companies deny acne claims, the real costs patients face without coverage, and the concrete steps you can take to fight back. If you have been denied coverage for acne treatment, you should know that roughly 40 percent of all insurance appeals succeed, and that number climbs much higher with the right documentation and strategy.
Table of Contents
- Why Does Insurance Classify Acne Treatment as Cosmetic Instead of Medical?
- The True Cost of Acne Treatment Without Insurance Coverage
- How Mental Health Impact Strengthens the Case for Medical Necessity
- How to Appeal an Insurance Denial for Acne Treatment
- Step Therapy and Prior Authorization — The Hidden Barriers
- Discount Programs and Alternative Payment Strategies
- Where Acne Coverage Is Headed
- Conclusion
- Frequently Asked Questions
Why Does Insurance Classify Acne Treatment as Cosmetic Instead of Medical?
The core problem is how insurance companies draw the line between “cosmetic” and “medically necessary.” In practice, this line is blurry and inconsistently applied. Prescription retinoids and oral antibiotics for active acne are more likely to be covered because they treat an active condition. But treatments for acne scarring, including laser therapy, chemical peels, and dermal fillers, are almost universally classified as cosmetic, regardless of how severe the scarring is or what psychological impact it carries. A patient with deep ice-pick scars across their face from years of untreated cystic acne will typically receive the same denial letter as someone seeking a purely elective procedure. Research published in PMC confirms that acne scarring treatments incur significant out-of-pocket costs precisely because of this blanket cosmetic classification. The classification problem extends beyond scar treatment. Even for active acne, insurers use mechanisms like step therapy and prior authorization to limit what they will pay for.
Step therapy forces patients to try cheaper treatments first, even when those treatments are inappropriate for their specific condition. The American Academy of Dermatology has called this practice “illogical and inappropriate,” citing cases where insurers require patients to fail on oral antibiotics before approving a topical retinoid, which is a backwards approach to acne management. Prior authorization for topical tretinoin, one of the most commonly prescribed acne medications, has been shown in research to provide no meaningful cost benefit to insurers while creating significant treatment delays and lowering patient adherence. Off-label prescriptions face an even steeper climb. Spironolactone, widely used by dermatologists to treat hormonal acne in women, is technically prescribed off-label for this purpose. Because the FDA approved it as a blood pressure medication, not an acne treatment, insurance companies are far less likely to cover it. This is despite the fact that spironolactone is one of the most effective options for adult women dealing with hormonal breakouts along the jawline and chin, a demographic that standard acne treatments often fail.

The True Cost of Acne Treatment Without Insurance Coverage
When insurance does not cover acne treatment, the numbers add up fast. Generic isotretinoin carries an average retail price of around $445, though patients who use discount programs like goodrx can sometimes bring that down to roughly $40 per month. But the medication is only part of the cost. Isotretinoin requires monthly dermatologist visits, typically $100 to $300 each, plus monthly blood work at $50 to $150 per draw. Over a standard four-to-six-month course, the total easily exceeds $3,000 and can push past $5,000 depending on the provider and region. The average cost of a single acne treatment episode across all ages is $689, according to research published in the Journal of the American Academy of Dermatology.
For adolescents aged 15 to 17, that average rises to $869 per episode. These figures represent averages, which means many patients pay considerably more, especially those with severe or treatment-resistant acne who cycle through multiple medications before finding something that works. Each failed treatment is another round of office visits, prescriptions, and lab work. However, it is worth noting that not all acne requires expensive intervention. Mild to moderate acne often responds well to over-the-counter benzoyl peroxide and adapalene, which is now available without a prescription. If your acne is limited to occasional breakouts without cystic lesions or scarring, you may not need to navigate insurance battles at all. The real financial pain hits patients with moderate-to-severe acne who need prescription-strength treatments, and those patients are precisely the ones most likely to encounter coverage denials.
How Mental Health Impact Strengthens the Case for Medical Necessity
One of the strongest arguments against the cosmetic classification of acne treatment comes from mental health research. Clinical studies have found that the psychological distress caused by severe acne is comparable to that experienced by patients with life-threatening or physically disabling diseases. That is not hyperbole. Researchers have documented rates of depression, anxiety, social withdrawal, and suicidal ideation among severe acne patients that rival those seen in conditions like epilepsy, diabetes, and chronic back pain. When an insurer labels acne treatment as cosmetic, they are ignoring a body of evidence that says otherwise. Consider the case of a college student with severe nodulocystic acne who avoids classes, drops out of social activities, and develops clinical depression.
Their dermatologist prescribes isotretinoin, but the insurance company demands they first try two rounds of oral antibiotics and a topical retinoid, a process that could take six months or more. During that time, the scarring worsens, becoming permanent, and the psychological damage deepens. This is not a hypothetical. It is the lived experience of thousands of patients caught in step therapy and prior authorization loops. The good news is that growing awareness of acne’s mental health toll is beginning to shift the conversation. The American Journal of Managed Care has highlighted research on how acne scars affect patients’ quality of life, and there is increasing pressure on insurers to reclassify severe acne treatment as medically necessary. If you are building an appeal, documenting the mental health impact through a therapist’s letter or psychiatric evaluation can significantly strengthen your case.

How to Appeal an Insurance Denial for Acne Treatment
The single most important thing to know about insurance denials is that appealing works far more often than most people assume. Patients who appeal win roughly 40 percent of the time across all claim types. For dermatology specifically, the numbers are even more encouraging: two-thirds of denied claims are recoverable with proper documentation, and success rates can reach 89 percent when specialty-specific appeal strategies are used. Most people never appeal because they assume the denial is final. It is not. Start by reading your denial letter carefully. It will include a reason for the denial and information about your appeal deadline, which typically falls between 30 and 180 days from the date of the letter. Missing this window forfeits your right to appeal entirely, so mark the date immediately.
Then gather your documentation: a letter of medical necessity from your dermatologist, your medical records showing the severity and history of your condition, clinical guidelines from the American Academy of Dermatology, peer-reviewed studies supporting your treatment, and the insurer’s own clinical policy bulletin. The AAD has published updated acne management guidelines with 18 evidence-based recommendations, and these can be directly cited to support medical necessity arguments. There is a tradeoff to consider in how aggressively you pursue an appeal. A simple written appeal with supporting documentation costs you time but no money. Escalating to an external review after an internal appeal is denied adds complexity but is often free to the patient. Hiring a health insurance attorney for a potential bad faith claim can recover significant costs but introduces legal fees and a longer timeline. For most patients, the written appeal with strong dermatologist documentation is the highest-value first step. Save the attorney for cases where you believe the insurer is acting in demonstrable bad faith.
Step Therapy and Prior Authorization — The Hidden Barriers
Even when your insurance plan technically covers acne treatment, step therapy and prior authorization requirements can delay or effectively block access to appropriate care. Step therapy, sometimes called “fail first,” requires patients to try and fail on cheaper medications before the insurer will approve the treatment their dermatologist actually recommended. In acne treatment, this often means being forced onto oral antibiotics, which carry their own risks including antibiotic resistance and gut health disruption, before you can access a retinoid or isotretinoin. The AAD has been vocal in its opposition to these practices, actively advocating for prior authorization reform at the state and federal level. Their position is supported by research: a study on prior authorization for topical tretinoin found that the process created meaningful treatment delays and reduced patient adherence without producing any cost savings for the insurer.
In other words, prior authorization for common acne medications costs everyone more while helping no one. Some states have begun passing legislation to limit step therapy in dermatology, but progress is uneven. A critical warning: if your insurer requires step therapy, document every step meticulously. Save pharmacy receipts, note the dates you started and stopped each medication, photograph your skin throughout, and have your dermatologist record the clinical rationale for moving to the next treatment. If you later need to appeal, this documentation trail is what separates a successful appeal from a denied one. Do not rely on memory or assume your medical records will capture everything.

Discount Programs and Alternative Payment Strategies
While you fight the insurance battle, there are ways to reduce your immediate out-of-pocket costs. Prescription discount programs like GoodRx can bring the cost of generic isotretinoin from its retail price of roughly $445 down to approximately $40 per month, a significant reduction that makes treatment accessible even without insurance cooperation. Manufacturer copay cards are sometimes available for brand-name medications, and some dermatology practices offer payment plans or sliding-scale fees based on income.
Telehealth dermatology has also expanded access and reduced visit costs for patients managing acne. While isotretinoin still requires in-person monitoring due to its mandatory iPLEDGE program requirements, many other prescription acne treatments can be prescribed and managed through virtual visits at a lower cost than traditional office appointments. If cost is the primary barrier, ask your dermatologist’s office directly about their most affordable options before assuming you cannot afford treatment.
Where Acne Coverage Is Headed
The landscape is shifting, slowly. Acne prevalence has risen 14.5 percent over the past decade, with over 8.6 million prevalent cases recorded in 2021, and the condition now affects a broader demographic than the stereotypical teenager. Over 50 percent of adults experience acne at some point, and the combination of rising prevalence, growing mental health awareness, and active AAD advocacy is putting sustained pressure on insurers to modernize their coverage policies.
The most likely near-term changes will come through state-level prior authorization reform and expanded mental health parity arguments that force insurers to account for the documented psychological impact of severe acne. For patients dealing with denials today, the practical takeaway is that the system can be navigated. Appeals succeed more often than not when properly documented, discount programs dramatically reduce medication costs, and the medical establishment is increasingly aligned with patients in pushing back against arbitrary cosmetic classifications.
Conclusion
Insurance companies deny acne treatment coverage primarily by classifying it as cosmetic, imposing step therapy requirements, and erecting prior authorization barriers that delay and discourage treatment. These practices persist despite acne being the most common skin condition in the country, despite documented psychological impacts comparable to serious chronic diseases, and despite evidence that prior authorization produces no cost savings.
The system is not designed with patients in mind, and navigating it requires active effort. The most important steps you can take are to appeal every denial with thorough documentation, work with your dermatologist to build a medical necessity case, use discount programs to manage costs during the process, and document every stage of your treatment history. With appeal success rates reaching as high as 89 percent in dermatology when the right strategies are used, accepting a denial at face value is the most expensive mistake you can make.
Frequently Asked Questions
Does insurance cover dermatologist visits for acne?
Most insurance plans cover dermatologist visits when acne is diagnosed as a medical condition. The coverage disputes typically arise around specific treatments, medications, and procedures rather than the office visit itself. However, your copay and whether the dermatologist is in-network will significantly affect your out-of-pocket cost.
Is Accutane covered by insurance?
Generic isotretinoin is covered by many insurance plans, but often only after prior authorization and step therapy requirements are met. You may need to demonstrate that you have tried and failed on other treatments first. Brand-name Accutane is less commonly covered. Without insurance, generic isotretinoin averages around $445 retail but can be found for approximately $40 per month through discount programs.
How long do I have to appeal an insurance denial for acne treatment?
Appeal deadlines typically range from 30 to 180 days from the date on your denial letter. The exact timeframe depends on your specific plan and state regulations. Missing this deadline forfeits your right to appeal, so check your denial letter immediately and mark the deadline.
Can I get acne scar treatment covered by insurance?
Acne scar treatments including laser therapy, chemical peels, and dermal fillers are almost universally classified as cosmetic by insurance companies. Coverage is extremely rare. Your strongest argument is documenting the psychological impact and obtaining a letter of medical necessity, but expectations should be realistic about the likelihood of approval.
What is step therapy and can I avoid it?
Step therapy requires you to try cheaper treatments before your insurer will approve the medication your doctor recommended. Some states have laws allowing exceptions, and your dermatologist can sometimes request an override by demonstrating medical necessity. The AAD actively advocates against step therapy in acne treatment, calling it “illogical and inappropriate.”
Should I hire a lawyer if my acne treatment claim is denied?
For most patients, a well-documented written appeal is the best first step, and it costs nothing beyond your time. If your internal appeal and external review both fail and you believe the insurer is acting in bad faith, consulting a health insurance attorney may be worthwhile. Legal action introduces costs and a longer timeline, so it is generally reserved for cases involving significant denied claims or systemic bad faith behavior.
You Might Also Like
- Why Ro Derm Is a Strong Option for Online Acne Treatment
- What Nurx Offers for Acne Treatment
- What Hormonal Panels to Run Before Starting Acne Treatment
Browse more: Acne | Acne Scars | Adults | Back | Blackheads