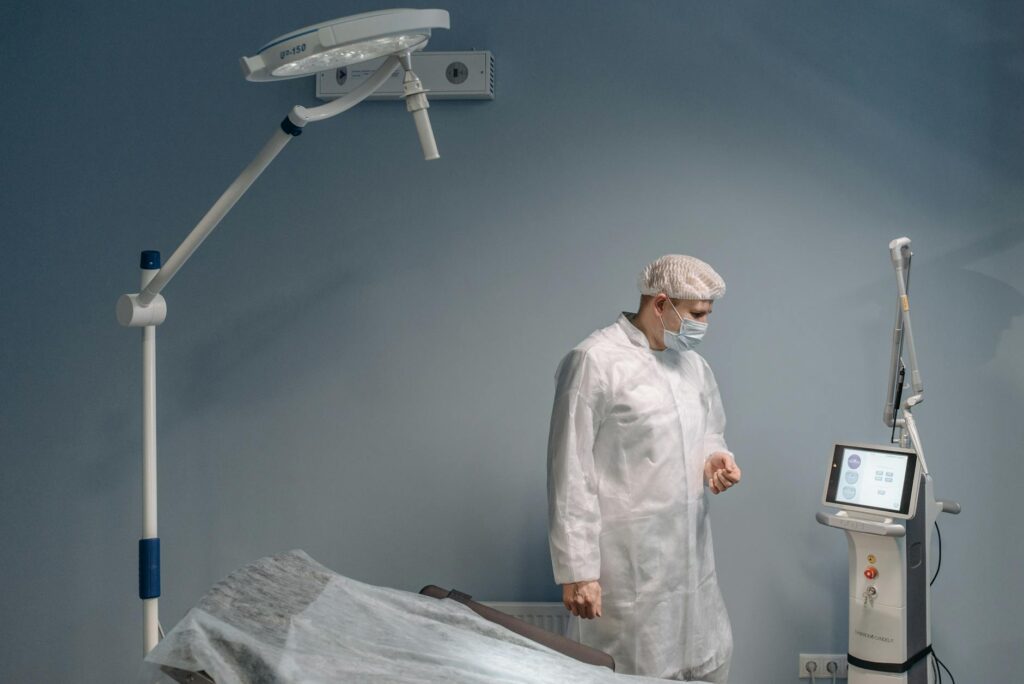
Academic medical center acne clinics remain significantly underutilized despite offering some of the most comprehensive and evidence-based acne treatment available. The primary reasons are straightforward: patients often don’t know these clinics exist, face bureaucratic hurdles with insurance requirements and referrals, encounter long wait times that can stretch months, and assume they’re only for severe nodular acne—when in reality they treat everything from mild adolescent breakouts to complex cystic forms.
Meanwhile, private dermatology practices have invested heavily in patient acquisition and convenience, while telehealth platforms have made easy-access treatment seem just a click away. Consider a 19-year-old with moderate inflammatory acne who could benefit from professional supervision while on isotretinoin, a powerful medication that requires monthly lab monitoring—yet they may never think to contact their local university medical center’s dermatology department, opting instead for a $99 telemedicine visit that offers no follow-up care. This article explores the systemic, practical, and perceptual barriers that keep academic medical centers from serving the acne patients who could benefit most from their expertise and resources.
Table of Contents
- Why Patients Don’t Find or Access Academic Acne Clinics
- The Insurance and Referral Barrier
- Competition from Private Practice and Telehealth Alternatives
- Misperceptions About Who Should Use Academic Acne Clinics
- Limited Hours, Long Wait Times, and Systemic Constraints
- What Academic Acne Clinics Actually Offer
- The Shift Toward Patient Autonomy and What It Means for Academic Centers
- Conclusion
- Frequently Asked Questions
Why Patients Don’t Find or Access Academic Acne Clinics
Most patients seeking acne treatment never discover that academic medical centers offer specialized dermatology services, let alone dedicated acne clinics. Unlike chain dermatology practices or direct-to-consumer skincare brands, academic medical centers typically allocate minimal resources to marketing, relying instead on referrals from primary care physicians or word-of-mouth—channels that have largely eroded as patients increasingly self-direct their healthcare searches. When someone with acne searches online, they encounter targeted ads from Curology, Ro, and boutique dermatology practices; they do not encounter ads from the university medical center across town.
Additionally, the patient experience requires navigation through appointment systems designed for complex medical needs rather than straightforward cosmetic or dermatological concerns. For example, calling a university dermatology clinic often routes patients through a centralized appointment line that asks why they’re calling, screens for insurance, and may tell them there’s a six-month wait. By that point, a patient who simply wants help with their breakouts has already booked a telemedicine appointment instead.

The Insurance and Referral Barrier
A significant structural barrier involves insurance requirements and the gatekeeper model that academic medical centers often maintain. Many academic centers require a referral from a primary care physician before scheduling a dermatology appointment, a requirement that private practices have abandoned. While insurance may ultimately cover the visit more comprehensively than a cash-pay telehealth option, the added step of contacting a primary care doctor, requesting a referral, waiting for it to be sent, and then scheduling with dermatology creates friction.
Additionally, some insurance plans classify acne treatment as “cosmetic” unless the patient meets specific severity thresholds—meaning a university dermatology clinic may refuse to schedule a patient without a referral documenting that acne is causing significant scarring or psychological distress. However, if the patient’s acne does qualify, academic centers typically offer superior treatment options, including compounded topical medications, oral antibiotics under dermatologist supervision, and access to newer agents. The catch is that navigating this insurance labyrinth requires persistence, knowledge of how to advocate for oneself within the medical system, and time—resources not all patients possess.
Competition from Private Practice and Telehealth Alternatives
The dermatology landscape has fragmented over the past decade in ways that directly disadvantage academic centers. Dermatologists increasingly leave academic medicine to open private practices where they can control patient volume, set fees, and operate without the constraints of a teaching institution. These private practices invest in convenient locations, efficient scheduling systems, and targeted marketing that academic centers cannot match. Simultaneously, telehealth platforms have made low-friction acne consultation available at midnight on a Sunday, sometimes without an insurance card, which appeals to younger patients accustomed to on-demand services.
A 16-year-old with moderate acne can book a Ro appointment in minutes and receive a prescription for topical tretinoin or oral doxycycline without ever explaining their situation to a dermatologist in person. An academic medical center appointment requires planning weeks in advance and traveling to a hospital or medical campus. From the patient’s perspective—and from many insurance companies’ perspectives—the outcome is similar enough that the frictionless option wins. Academic centers lose volume not necessarily because they’re worse at treating acne, but because they’re harder to access.

Misperceptions About Who Should Use Academic Acne Clinics
Many patients believe that academic medical center dermatology is appropriate only for severe, complicated cases—treatment-resistant acne, acne rosacea, cystic nodular disease, or patients requiring isotretinoin monitoring. This perception serves as a self-selecting barrier: patients with mild to moderate acne don’t even attempt to schedule because they assume academic centers won’t see them or will deprioritize their cases.
In reality, academic clinics manage the full spectrum of acne severity and routinely provide initial assessments and ongoing care for patients with straightforward inflammatory or comedonal acne. Moreover, if you begin treatment at an academic center, you gain access to dermatologists who are current on the latest evidence and are often teaching faculty—people who stay at the cutting edge of treatment protocols. The tradeoff, however, is that academic teaching clinics may involve seeing a resident or fellow under faculty supervision, which some patients find less personable than a private practice appointment, and there is a higher likelihood of structured follow-up versus the convenience of telemedicine-as-needed.
Limited Hours, Long Wait Times, and Systemic Constraints
Academic medical centers operate according to institutional policies, teaching schedules, and budget constraints that limit their ability to serve on-demand. Many academic dermatology clinics operate only three or four days per week, have restricted evening or weekend hours, and require appointments to be scheduled during standard business hours—creating obvious friction for working patients or students.
Wait times of three to six months for an initial dermatology appointment are not unusual at large university systems, which means a patient’s acne may significantly improve or worsen before they’re even evaluated. Furthermore, academic centers often cannot accommodate urgent appointments for acute flares or reactions to treatment, instead directing patients to urgent care or referring them back to primary care. This is a critical limitation for patients considering medications like isotretinoin, which genuinely require robust, reliable follow-up—yet many academic clinics’ bureaucratic structures make providing that follow-up more difficult than a private dermatology practice accustomed to serial patient management.

What Academic Acne Clinics Actually Offer
Despite the barriers, academic medical centers provide distinct advantages that private practice and telehealth cannot replicate. Most academic dermatology clinics have access to compounded topical medications, combination therapies, and specialized formulations not available through standard pharmacy channels. They can prescribe oral antibiotics with dermatologic expertise, manage complex drug interactions, and monitor for side effects of medications like doxycycline or minocycline.
Many academic centers have dermatologists with specific expertise in acne—some even have dedicated acne specialists—whereas a random private dermatologist may see acne as one small part of their general practice. Additionally, academic clinics often participate in clinical trials for emerging acne treatments, offering patients access to new therapies not yet widely available. For example, a university dermatology clinic might offer enrollment in a trial evaluating a novel 5-alpha reductase inhibitor for acne-prone skin, whereas a telehealth platform offers only the standard rotation of doxycycline, tretinoin, and topical benzoyl peroxide.
The Shift Toward Patient Autonomy and What It Means for Academic Centers
The future of academic medical center acne clinics depends partly on whether these institutions can adapt to patient expectations for convenience and direct access. Some progressive academic centers are implementing online scheduling, reducing or eliminating referral requirements, and creating separate acne-focused clinic tracks with faster appointment availability.
However, the fundamental constraint remains: academic centers serve educational missions and research functions alongside clinical care, which necessarily limits their capacity to operate as high-volume, patient-focused practices. Younger patients increasingly expect to initiate their own healthcare without physician gatekeepers, which further erodes the referral-based patient flow that academic dermatology has historically relied on. As acne treatment becomes increasingly professionalized at the retail level—with aestheticians prescribing topical retinoids, dermatologists operating private practices optimized for acne patients, and telehealth platforms offering convenient access—academic centers will likely continue to serve primarily as secondary or tertiary referral destinations rather than first-line sources of acne care.
Conclusion
Academic medical center acne clinics are underutilized not because they lack expertise or resources, but because systemic barriers—limited visibility, insurance gatekeeping, long wait times, and the convenience of private practice and telehealth alternatives—have made them inaccessible to patients who might benefit from their care.
These institutions offer depth of dermatologic knowledge, access to specialized medications and compounded formulations, and the potential for robust, long-term management that matters particularly for patients on challenging medications like isotretinoin. If you have moderate to severe acne, are beginning isotretinoin, experience treatment-resistant breakouts, or want dermatologic expertise rather than a transactional prescription, contacting your local academic medical center’s dermatology department is worthwhile—even if it means navigating a referral requirement and waiting weeks for an appointment.
Frequently Asked Questions
Do I need a referral to see an acne doctor at an academic medical center?
It depends on the institution and your insurance. Many academic medical centers still require a referral from your primary care physician, though some have moved to open-access scheduling. Call the dermatology clinic directly to ask; if you need a referral and your primary care doctor is reluctant, explain that you have acne requiring specialist evaluation, and your doctor should provide one.
How long is a typical wait time for an acne appointment at a university dermatology clinic?
Expect four to twelve weeks for an initial appointment, depending on the institution. Some academic centers have expedited tracks for patients on isotretinoin or with severe cystic acne. Call ahead to ask if there are faster options available.
Will I see the same dermatologist each time?
In academic teaching clinics, no—you may see a resident, fellow, or attending dermatologist depending on the clinic structure. However, residents and fellows are supervised by faculty, and the quality of care is typically high. If continuity with the same provider is important to you, a private dermatology practice is more likely to offer it.
Are academic medical center acne treatments more expensive than private dermatology?
Not necessarily. Academic centers often have negotiated insurance rates similar to private practices and may offer financial assistance programs for uninsured patients. However, the true cost depends on your insurance and what medications are prescribed.
Can I get isotretinoin treatment at an academic medical center?
Yes, many academic dermatology clinics manage isotretinoin patients and often have excellent infrastructure for the required monthly lab monitoring, pregnancy tests, and iPLEDGE enrollment. This is one area where academic centers have a significant advantage over telemedicine.
What should I do if my acne is mild but I still want specialist evaluation?
Call the academic dermatology clinic and ask directly whether they see patients with mild acne, or check their website for clinic descriptions. Some academic centers prioritize severe cases; others see the full spectrum. Some patients with mild but persistent acne benefit from early intervention with a dermatologist rather than months of trial-and-error with over-the-counter products.
You Might Also Like
- What Acne Center of Excellence Clinics Offer
- Why Zinc Acetate IV Is Studied for Severe Inflammatory Acne
- Why Stem Cell Conditioned Media Works for Acne Healing
Browse more: Acne | Acne Scars | Adults | Back | Blackheads