Ultrasound imaging reveals the internal architecture of acne cysts that’s invisible to the naked eye—specifically, whether they’re fluid-filled or solid, how deep they extend into the skin, the degree of surrounding inflammation, and whether they’ve damaged underlying tissue. For dermatologists, this information determines whether a cyst needs extraction versus topical treatment and signals whether scarring is likely to occur. For example, a superficial fluid-filled cyst measuring 5mm shows different treatment urgency than a deep, solid lesion at 15mm with inflammation extending into the dermis. This article covers what ultrasound technology actually shows dermatologists when evaluating cystic acne, how those findings translate into treatment decisions, and what imaging limitations mean for clinical practice.
Table of Contents
- How Does Ultrasound Differentiate True Cysts from Other Severe Acne Lesions?
- What Precise Depth and Size Measurements Does Ultrasound Provide?
- How Does Ultrasound Reveal Inflammation and Surrounding Tissue Changes?
- How Do Ultrasound Findings Guide Extraction versus Conservative Treatment Decisions?
- What Ultrasound Limitations Mean for Clinical Decisions?
- What Ultrasound Findings Signal Risk of Post-Extraction Scarring?
- What Does the Future Hold for Imaging in Acne Management?
- Conclusion
- Frequently Asked Questions
How Does Ultrasound Differentiate True Cysts from Other Severe Acne Lesions?
Ultrasound distinguishes true sebaceous cysts from inflamed nodules, papules, and pseudocysts through characteristic echogenicity patterns and internal fluid content. A genuine cyst appears as a well-defined, round or oval structure with an anechoic (black, fluid-filled) center on the screen, bordered by a distinct hyperechoic capsule wall.
In contrast, an inflamed nodule shows diffuse internal echoes without clear fluid demarcation, appearing more heterogeneous throughout. This distinction matters clinically because true cysts containing sebum or fluid require extraction or injection therapy to resolve, while inflamed nodules often respond to oral antibiotics and retinoids alone. A dermatologist evaluating a patient with persistent facial acne lumps can use ultrasound to confirm the lesion is actually a cyst rather than residual scarring or scar tissue, which can appear similar to the eye but shows completely different echo patterns on imaging.
What Precise Depth and Size Measurements Does Ultrasound Provide?
Ultrasound provides real-time depth measurements showing exactly how far acne cysts extend into the skin layers, from the epidermis through the dermis and sometimes into subcutaneous fat. A superficial cyst measuring 3-4mm deep in the upper dermis has a fundamentally different prognosis than a subcutaneous cyst extending 10-15mm below the skin surface.
The depth determines whether needle extraction is sufficient or if larger incisions and formal removal become necessary, and deeper cysts carry higher risk of recurrence if not fully extracted. However, ultrasound can sometimes overestimate size compared to clinical examination, especially in very inflamed cysts where surrounding edema creates an echo-dark halo that appears larger than the actual lesion. Additionally, ultrasound measures the cyst at a single cross-section; cysts are three-dimensional structures that may be larger or smaller than the single plane the ultrasound captured, so dermatologists typically obtain images from multiple angles.
How Does Ultrasound Reveal Inflammation and Surrounding Tissue Changes?
Ultrasound images show not just the cyst itself but the inflammatory response in surrounding dermis through increased echogenicity (brightness) and thickened skin texture around the lesion. A calm cyst with minimal surrounding inflammation appears as a discrete structure with normal-echo tissue around it, suggesting the cyst is asymptomatic and infection risk is low.
By contrast, a cyst surrounded by significant inflammation shows hazy, echogenic tissue extending outward, indicating active inflammation that may be causing pain, redness, or warmth. This inflammatory pattern matters because heavily inflamed cysts often require initial antibiotic therapy or corticosteroid injection before extraction, whereas minimally inflamed cysts can go directly to drainage or incision-and-removal. Dermatologists also use ultrasound to identify whether inflammatory changes suggest developing infection or are simply the body’s response to the cyst’s contents, which changes antibiotic recommendations.

How Do Ultrasound Findings Guide Extraction versus Conservative Treatment Decisions?
The ultrasound findings create a clinical decision tree: small, superficial, fluid-filled cysts under 5mm often respond to topical retinoids and benzoyl peroxide without intervention, while larger cysts or those extending deep into the dermis typically require extraction or injection therapy. If ultrasound confirms the lesion is a true cyst with distinct borders and fluid content, dermatologists can confidently recommend extraction, knowing the patient will see a real improvement rather than hoping a cyst might resolve on its own.
In contrast, if ultrasound shows a solid nodular lesion without fluid, the treatment shifts toward oral isotretinoin or long-term antibiotics because extraction of a solid lesion often leaves significant scarring and recurs easily. A practical example: a patient with a painful 12mm cyst on the cheek shows ultrasound evidence of fluid content and clear demarcation, making that patient an ideal candidate for incision-and-drainage with minimal downtime. The same-sized solid nodule might be better managed medically first, with extraction only if it persists after several months of treatment.
What Ultrasound Limitations Mean for Clinical Decisions?
Ultrasound cannot reliably distinguish between cyst contents (sterile sebum versus infected material), which means a dermatologist seeing ultrasound evidence of fluid still needs clinical assessment for signs of infection before choosing between simple drainage and more aggressive treatment. Additionally, very superficial cysts in the upper epidermis sometimes generate ultrasound artifacts or reflections that obscure their true size, potentially leading to overestimation; these lesions are often better assessed clinically.
Ultrasound also struggles with cysts under 2mm in diameter, where the resolution becomes insufficient for accurate measurement. Most significantly, ultrasound availability varies widely—many general dermatology practices lack in-office ultrasound capability, so these diagnostic benefits remain limited to specialized centers, academic practices, or dermatologists with equipment investment. This means most acne patients receive cyst treatment decisions based on clinical examination alone, not imaging confirmation.
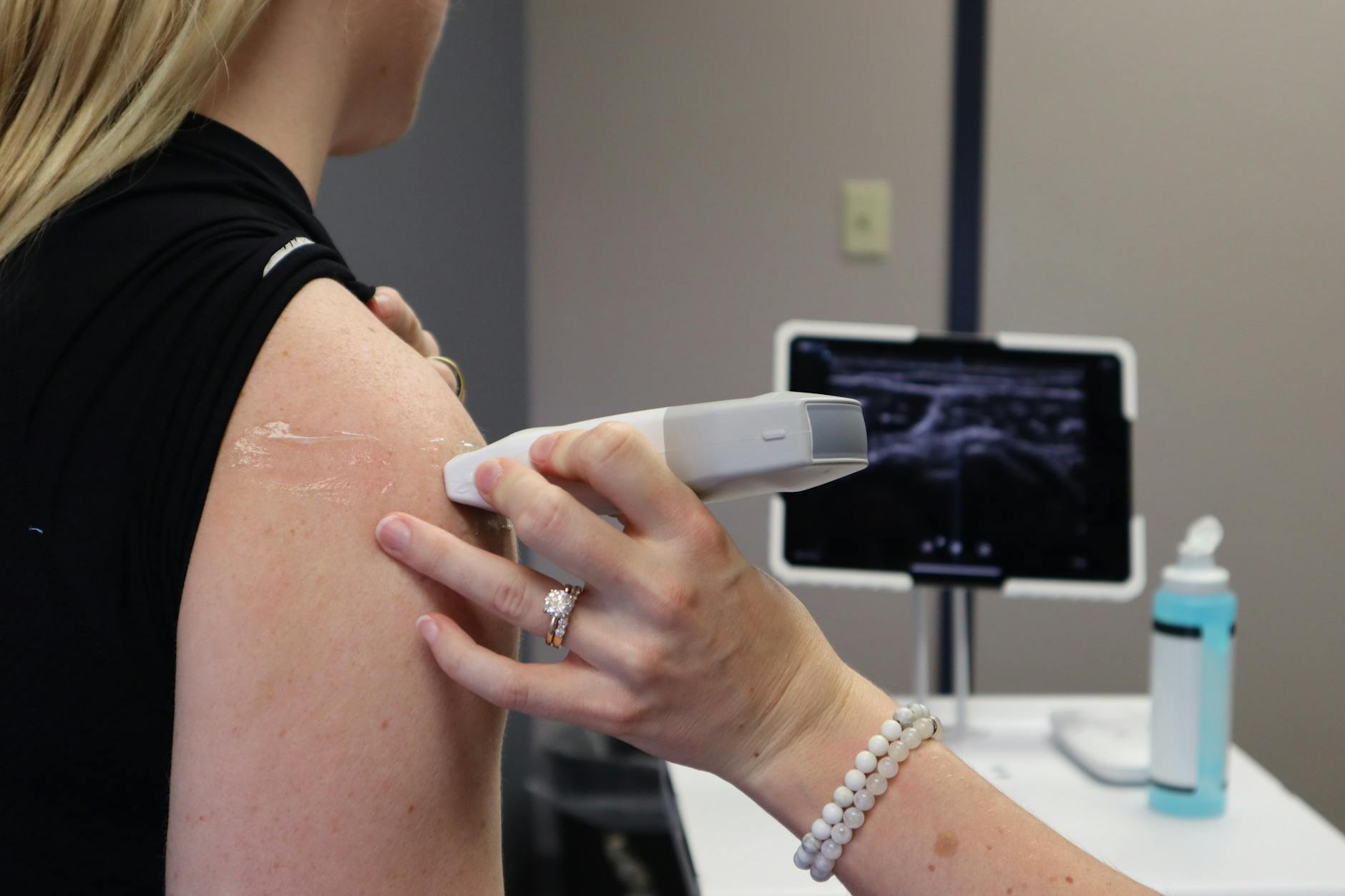
What Ultrasound Findings Signal Risk of Post-Extraction Scarring?
Dermatologists correlate specific ultrasound patterns with scarring likelihood: cysts with large diameter (>10mm), deep location in the dermis, thick inflammatory halo, or evidence of prior rupture on imaging carry higher scarring risk. If ultrasound shows a cyst has partially ruptured internally, spilling contents into surrounding tissue rather than maintaining an intact wall, that patient faces more inflammation and greater scarring potential regardless of treatment method chosen.
A 14mm cyst at 8mm depth with significant surrounding echogenic inflammation has a measurably different scarring outlook than a 6mm superficial cyst with minimal inflammation, and this objective distinction allows dermatologists to counsel patients more honestly about what to expect. Ultrasound findings combined with skin type and patient age create a risk stratification—a deep cyst in a patient with darker skin tone or history of keloids requires more cautious, conservative treatment planning.
What Does the Future Hold for Imaging in Acne Management?
Newer high-frequency ultrasound systems (15-20 MHz) provide improved resolution for shallow lesions compared to traditional 10-12 MHz machines, expanding the range of cysts that can be accurately imaged. Some dermatology research centers are exploring harmonic imaging and contrast-enhanced ultrasound to visualize inflammatory perfusion in active acne cysts, potentially enabling even earlier identification of infection risk.
As the technology becomes more accessible and standardized, ultrasound may shift from a specialized tool to routine equipment in dermatology offices, similar to how dermatoscopy for melanoma became standard practice. This democratization of imaging would allow dermatologists to move beyond clinical guesswork for cyst assessment and base treatment decisions on objective measurements of cyst size, depth, structure, and inflammatory burden.
Conclusion
Ultrasound imaging of acne cysts shows dermatologists critical information invisible to examination alone: whether a lesion is a true fluid-filled cyst or something else, its exact depth and size, the degree of surrounding inflammation, and warning signs of prior rupture or infection. This information transforms cyst management from guesswork to evidence-based decision-making, allowing dermatologists to confidently recommend extraction for appropriate candidates while steering others toward medical therapy or observation.
While ultrasound remains unavailable at most practices and has genuine technical limitations, its ability to visualize cyst structure, measure depth, and assess inflammation offers a significant advantage whenever accessible. If you have problematic acne cysts, ask your dermatologist whether in-office ultrasound is available at their practice—if it is, requesting imaging can provide concrete information about your specific lesions and the most appropriate treatment path forward.
Frequently Asked Questions
Can dermatologists see acne cysts on ultrasound that they can’t see during a regular exam?
Not usually for visible cysts, but ultrasound reveals internal structure and depth of lesions you can already see, which determines appropriate treatment. Ultrasound is more valuable for distinguishing true cysts from other lesions and measuring depth than for finding completely hidden cysts.
Does ultrasound imaging hurt or have any side effects?
No—ultrasound uses only sound waves and produces no pain, radiation, or tissue damage. It’s completely non-invasive, so it can be repeated as many times as needed without risk.
If my dermatologist doesn’t have ultrasound, can I get one at an urgent care or imaging center?
Technically yes, but most urgent care centers and imaging facilities don’t regularly perform ultrasound specifically for acne cysts—they’re set up for different applications. You’d need a dermatologist’s referral to a facility equipped for dermatologic ultrasound.
How much does ultrasound imaging of acne cysts cost?
Pricing varies widely depending on location and whether the ultrasound is performed at a dermatology office, imaging center, or medical facility. If your dermatologist offers it in-office, it’s often included in the visit fee or charged as a small add-on ($50-150).
Will ultrasound help me avoid scarring from my acne cysts?
Ultrasound won’t prevent scarring itself, but it helps your dermatologist identify cysts at high scarring risk, allowing more aggressive early treatment (like extraction) rather than waiting and hoping they resolve on their own, which sometimes leads to worse scarring.
You Might Also Like
- Why 3D Vectra Imaging Helps Track Acne Scar Improvement
- What Reflectance Confocal Microscopy Shows in Acne Skin
- What Metagenomics Shows About Acne Skin Bacteria
Browse more: Acne | Acne Scars | Adults | Back | Blackheads