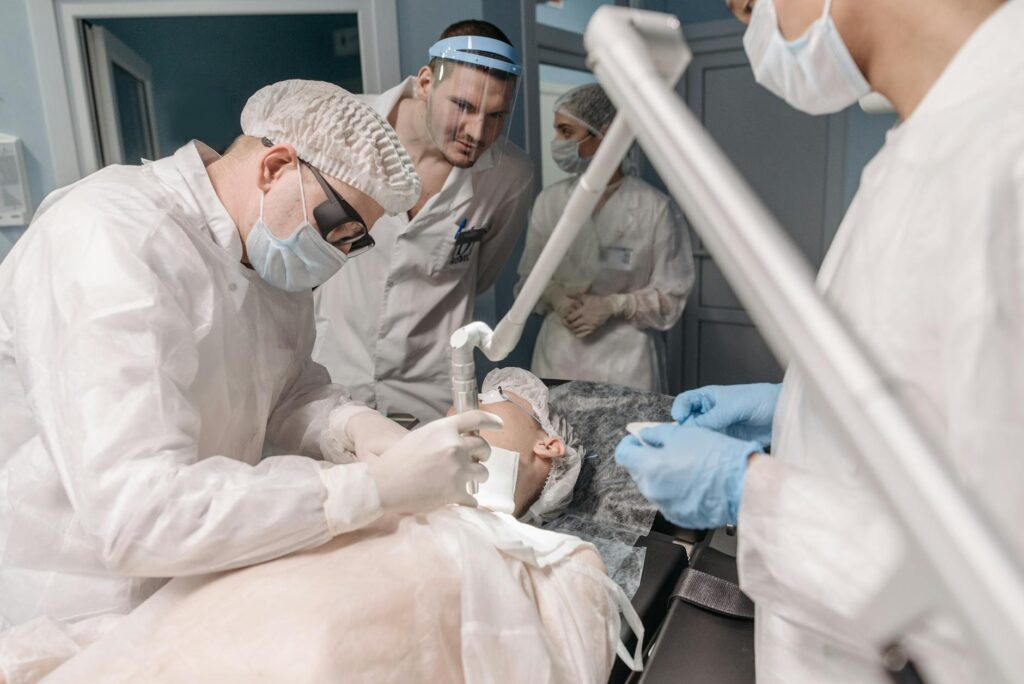
Smoothbeam operates through a process called phototermolysis, where the laser energy converts to heat at a precise depth in the skin. Because the 1450-nanometer wavelength absorbs preferentially into water (which is abundant in gland tissue), the laser can reliably reach and heat sebaceous glands located 1-2 millimeters below the skin surface. A patient with moderate acne who produces excess oil may see significant reduction in breakouts after 2-4 treatment sessions, though results vary based on skin type, acne severity, and whether the sebaceous glands are genuinely overactive or if other factors are driving the acne.
Table of Contents
- How Does Smoothbeam Laser Specifically Target Sebaceous Glands?
- The Mechanism—How Thermal Damage to Sebaceous Glands Reduces Acne
- What Results Do Patients Experience After Smoothbeam Treatment?
- Smoothbeam Treatment Compared to Topical and Oral Alternatives
- Limitations and Potential Side Effects of Smoothbeam Laser
- How Smoothbeam Compares to Other Laser and Light Therapies for Acne
- Long-Term Outlook and Maintenance Strategy After Smoothbeam Treatment
- Conclusion
How Does Smoothbeam Laser Specifically Target Sebaceous Glands?
Sebaceous glands are oil-producing structures attached to hair follicles throughout the skin, and they’re essential for skin health—but when overactive, they contribute directly to acne formation. Smoothbeam’s 1450-nanometer wavelength is absorbed efficiently by water molecules in the dermis, causing the laser energy to convert to heat concentrated around the sebaceous glands. This is different from surface-level treatments because the laser heat reaches the gland structure itself, not just the pore opening on the skin surface. The cooling system built into the Smoothbeam handpiece protects the outer epidermis from burn damage while allowing deeper tissue to heat to around 40-45 degrees Celsius—high enough to disrupt the gland’s function but low enough to avoid scarring.
The specificity matters clinically. A patient using topical retinoids or oral antibiotics may improve their acne, but these medications don’t permanently reduce sebaceous gland activity. Smoothbeam laser actually causes sebaceous gland atrophy—a reduction in gland size and oil-producing capacity that can last for extended periods. Studies show that patients experience decreased sebum production for 6-12 months after a single series of treatments, and some see sustained improvements for 2+ years. However, the sebaceous glands are not destroyed permanently; over time, some regrowth and return of oil production can occur, which is why touch-up treatments are sometimes needed.
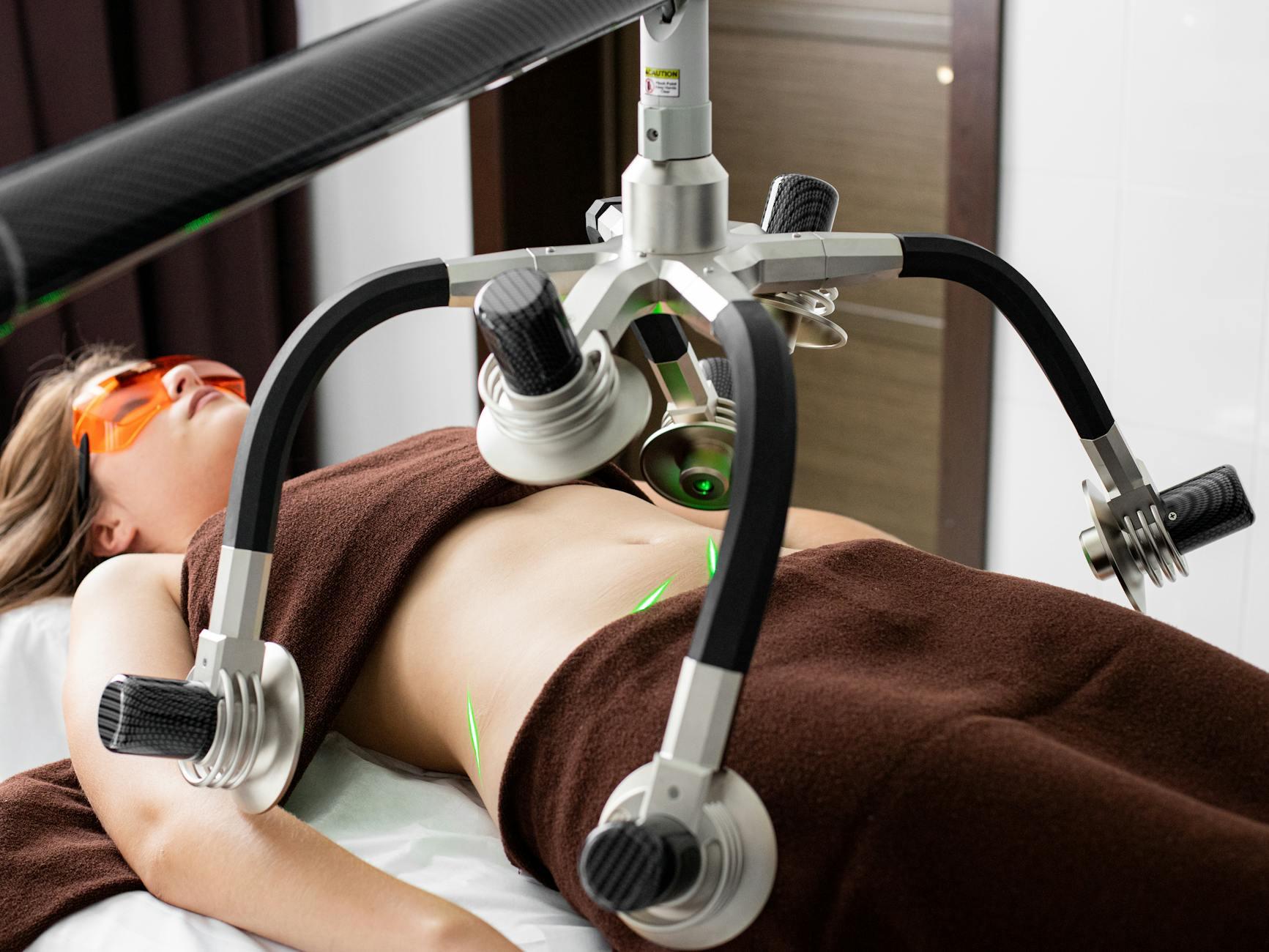
The Mechanism—How Thermal Damage to Sebaceous Glands Reduces Acne
The mechanism of action involves selective photothermolysis—the laser energy creates heat selectively in one target (sebaceous glands) while sparing surrounding skin. When sebaceous gland cells are heated to a sufficient temperature, proteins denature and cell membranes rupture, leading to programmed cell death. The body then gradually removes these damaged cells through normal tissue remodeling. This causes the gland to shrink and, crucially, to produce less oil going forward.
A patient with hormonal acne driven by excess oil production may experience dramatic improvement because the root cause—sebaceous gland overactivity—is being addressed, not just the surface symptoms. However, if a patient’s acne is driven primarily by bacterial colonization (Cutibacterium acnes), inflammation, or follicular keratinization rather than excess oil, Smoothbeam results will be more modest. A 25-year-old woman with oily skin and comedones will likely see excellent results; a 35-year-old with rosacea-type inflamed acne might see minimal change if oil production isn’t the primary driver. Additionally, Smoothbeam works best on active sebaceous glands in actively oil-producing skin. patients with naturally dry skin or those already on isotretinoin (Accutane) will not be good candidates because the laser has less target tissue to affect—there’s insufficient gland activity to modify.
What Results Do Patients Experience After Smoothbeam Treatment?
Most patients undergoing a series of 3-4 Smoothbeam treatments spaced 2-4 weeks apart report noticeable reductions in oiliness within 1-2 weeks after the first treatment. Pores appear smaller because they’re less engorged with sebum. Acne breakout frequency typically decreases by 40-70% over the 2-3 month treatment course, with maximum improvement visible 2-3 months after the final session. A typical patient might go from experiencing 5-8 breakouts per week to 1-2 per week. Some patients achieve near-complete clearance of acne if oil overproduction was the primary cause; others see a 50% improvement and need to maintain it with complementary treatments like retinoids or oral contraceptives.
The improvement is not instantaneous like some medications. Unlike oral antibiotics, which can show results within 4 weeks, Smoothbeam requires multiple sessions and the results build gradually as sebaceous gland tissue remodels. Patients should expect to wait at least 2-3 months to judge the full effectiveness. It’s also important to note that not all improvement is permanent—studies tracking patients 12-24 months post-treatment show that approximately 30-50% of patients experience some return of oiliness and acne as sebaceous glands partially regenerate, though it’s usually less severe than the baseline. This is why maintenance treatments every 12-18 months are sometimes recommended for long-term oil control.

Smoothbeam Treatment Compared to Topical and Oral Alternatives
When comparing Smoothbeam to standard acne treatments, the key difference is durability and target mechanism. Topical retinoids (tretinoin, adapalene) reduce sebum production by about 20-30% but require ongoing daily use; discontinuation leads to oil production rebounding within weeks. Oral isotretinoin (Accutane) can achieve 70-90% permanent sebum reduction, but it carries serious systemic risks including birth defects, liver toxicity, and severe dry skin side effects. Smoothbeam occupies a middle ground—it achieves 50-70% sebum reduction without systemic medication and maintains benefits for 6-12 months without daily application, but it’s not permanent like Accutane and results may gradually decline.
The practical tradeoff is cost and commitment. A typical Smoothbeam series costs $3,000-$6,000 out of pocket (rarely covered by insurance) and requires 4 office visits. A 3-month course of tretinoin costs $30-$100 and can be used indefinitely. For patients who are tretinoin-intolerant or fatigued by daily skincare, Smoothbeam makes sense; for budget-conscious patients, topical retinoids offer better cost-effectiveness. Combination therapy—using Smoothbeam to reduce oil production followed by maintenance with topical retinoids or azelaic acid—is increasingly common because it addresses sebaceous gland overactivity while managing bacterial colonization simultaneously.
Limitations and Potential Side Effects of Smoothbeam Laser
Smoothbeam is not suitable for all acne patients or all skin types. The laser light is absorbed into the skin, so darker skin types (Fitzpatrick IV-VI) are at higher risk for post-inflammatory hyperpigmentation or hypopigmentation. Additionally, patients taking photosensitizing medications (certain antibiotics, NSAIDs, retinoids) or with a history of keloid scarring should undergo careful evaluation before treatment. The procedure also causes temporary inflammation; most patients experience redness, swelling, and mild crusting for 3-7 days post-treatment. In rare cases (estimated <2%), patients develop post-inflammatory hyperpigmentation or, very rarely, atrophic scarring if the laser setting is too aggressive.
A critical limitation is that Smoothbeam does not treat acne caused by factors other than sebaceous gland overactivity. Patients with follicular hyperkeratinization, C. acnes bacterial overgrowth, or hormone-driven inflammation may see minimal results. There’s also a real possibility of patient disappointment if expectations aren’t properly set—some patients expect Smoothbeam to work like Accutane (permanent clearance) when the reality is a temporary reduction in oil production. Furthermore, the effects are not instantaneous; some patients discontinue treatment after 1-2 sessions thinking it’s not working, when in fact they need 3-4 sessions to see meaningful change. If a patient is pregnant, planning pregnancy, or currently nursing, Smoothbeam is contraindicated because its long-term effects on sebaceous gland recovery in these populations aren’t well-studied.

How Smoothbeam Compares to Other Laser and Light Therapies for Acne
The laser treatment landscape includes several competing technologies. Blue light (415-nanometer wavelength) kills C. acnes bacteria but does not address sebaceous gland activity—patients with oil-driven acne won’t see lasting improvement. Red light and near-infrared wavelengths reduce inflammation but again don’t target the gland itself.
Fractional CO2 lasers can ablate skin and disrupt follicles but cause more visible downtime (10-14 days of healing) and are typically reserved for severe scarred acne rather than active breakouts. Smoothbeam’s 1450-nanometer wavelength is unique because it reliably reaches sebaceous glands without the extensive downtime of ablative lasers. Diode lasers at 1320 nanometers are similar to Smoothbeam in wavelength and mechanism and show comparable results in clinical studies. The choice between Smoothbeam and 1320-nanometer diode treatment often comes down to equipment availability and provider experience rather than efficacy differences. For patients comparing options, the key question is: does your acne primarily involve oil overproduction, or are bacteria, inflammation, and follicular clogging the main drivers? If oil production is the driver, Smoothbeam or comparable 1320-1450-nanometer lasers are more effective than light-based therapies.
Long-Term Outlook and Maintenance Strategy After Smoothbeam Treatment
After completing an initial series of Smoothbeam treatments, the long-term outcome depends on individual biology and whether the underlying cause of acne (excess oil production) was addressed successfully. Patients who experience significant improvement face a choice: accept that some return of oil and occasional breakouts may occur as the gland recovers, or plan for maintenance treatments. Clinical data suggests that touch-up treatments every 12-18 months help sustain the benefits, with each successive treatment showing similar or slightly diminishing returns.
A patient treated with Smoothbeam at age 25 might choose to repeat treatments every 18 months through age 40, realizing cumulative benefit over many years, though the cost compounds over a decade. The future of sebaceous gland-targeted treatment likely includes combination approaches and refined laser parameters. Emerging research explores whether combining Smoothbeam with topical medications that further inhibit sebaceous gland function (such as novel retinoids or hormonal therapies) could extend results beyond 12 months. For now, realistic long-term expectations are that Smoothbeam provides significant temporary improvement in sebaceous gland activity and acne severity, but not a permanent cure—more of a “reset” that buys patients several months to a year of clearer skin, during which they can establish sustainable skincare routines or transition to maintenance medication if needed.
Conclusion
Smoothbeam laser targets sebaceous glands by delivering 1450-nanometer laser energy that converts to controlled heat in the dermis, damaging oil-producing gland tissue and reducing sebum production by 50-70% for 6-12 months. This approach addresses acne at the sebaceous gland level rather than treating surface symptoms, making it effective for patients whose acne is driven by oil overproduction. Results require a series of multiple sessions, are not instantaneous, and are not permanent—but they offer a meaningful middle ground between daily topical treatments and permanent systemic medication like Accutane.
The decision to pursue Smoothbeam should account for realistic expectations, skin type compatibility, cost ($3,000-$6,000), and whether oil production is genuinely the primary acne driver or a secondary factor. For appropriate candidates—those with oily, acne-prone skin resistant to topical treatments—Smoothbeam can significantly improve skin clarity and reduce reliance on daily medications. Discussing treatment goals, timeline, and maintenance expectations with a dermatologist experienced in Smoothbeam therapy is essential to determine whether this technology is the right choice for your specific acne pattern and skin type.
You Might Also Like
- What Ruby Laser Does for Superficial Acne Pigmentation
- What Enlighten III Picosecond Laser Does for Acne
- What Alexandrite Laser Does Versus Nd:YAG for Acne Pigmentation
Browse more: Acne | Acne Scars | Adults | Back | Blackheads