Skin thickness directly determines how deep a treatment can safely reach, what type of acne scars form on your face, and which therapeutic approach will actually work for you. A dermatologist treating scars on your cheeks must use completely different needle depths and treatment intensities than one addressing forehead scars—and that’s not just a preference, it’s a requirement rooted in anatomy.
For example, the cheeks contain significantly thicker skin than the temples, which means they can tolerate deeper microneedling (around 1.5 to 2.5mm) while forehead and temple areas max out at 0.5mm to avoid damage. This fundamental difference means that two people with seemingly identical acne scars can have completely different treatment experiences and timelines based purely on where those scars live on their face. This article explores exactly how skin thickness shapes scar formation, determines which treatments will succeed or fail, and what realistic timelines you should expect.
Table of Contents
- How Skin Thickness Varies Across Your Face and the Scars It Creates
- Why Thinner Skin Requires Completely Different Treatment Depth Protocols
- The Collagen Remodeling Timeline: Why Skin Thickness Affects How Fast You’ll See Results
- Matching Treatment Type to Your Skin Thickness and Scar Depth
- Injectable Fillers and the Practicality of Skin Thickness
- Emerging 2026 Therapies That Bypass Traditional Skin Thickness Limitations
- Planning Your Treatment Strategy Around Your Unique Skin Anatomy
- Conclusion
How Skin Thickness Varies Across Your Face and the Scars It Creates
Your skin is not uniformly thick. The deepest, most resilient skin sits on your lower cheeks and jaw—this is where you’ll find thickened collagen and elastin fibers that can withstand stronger treatments. The thinnest, most delicate skin wraps around your temples, forehead, and upper cheekbones. This thickness variation isn’t random; it reflects where your face experiences the most movement and stress over a lifetime.
This anatomical reality directly shapes the scars that form in the first place. Rolling scars—those gentle, wavelike indentations—tend to appear on the thicker skin of the lower cheeks and jaw, where the dermis has more structure to distort. Ice pick scars, which look like narrow puncture wounds, are more common on the thinner forehead and upper cheeks, where deep enough trauma can create sharp, defined pits. Boxcar scars, with their squared-off edges, appear across the face but are particularly stubborn on thinner-skinned areas because there’s less surrounding tissue to remodel. Understanding which scar type dominates your problem areas already tells you something important: the underlying skin thickness has already determined part of your treatment challenge.

Why Thinner Skin Requires Completely Different Treatment Depth Protocols
When a dermatologist performs microneedling, they’re not using the same depth everywhere. The 1.5 to 2.5mm needle depth used on cheeks would cause serious injury on your forehead or temples, where the entire dermal layer is barely 0.5mm deep. Going too deep in thin-skinned areas risks breaching into subcutaneous fat, triggering inflammation, scarring, or permanent damage.
This is why a competent provider must map out your face before treatment and adjust settings region by region. However, if your scars are concentrated on thin-skinned areas, this presents a real limitation: the treatment depth that would most aggressively remodel scar tissue can’t be safely used. Instead, providers compensate by increasing treatment frequency (more sessions with gentler parameters), combining modalities (microneedling plus topical retinoids, for instance), or pivoting to entirely different approaches like laser therapy or injectable fillers that don’t rely on deep needle penetration. This tradeoff is important to understand going in—thin-skinned areas may require more patience and creativity to treat effectively.
The Collagen Remodeling Timeline: Why Skin Thickness Affects How Fast You’ll See Results
When treatment works correctly, something remarkable happens beneath the skin’s surface. Histological studies show a dramatic increase in new collagen and elastin fibers—the skin literally thickens and strengthens in response to the controlled injury of treatment. However, this rebuilding doesn’t happen overnight. Visible improvement appears around the six-week mark, but the full, mature results don’t stabilize for at least three months.
In thicker-skinned areas like the cheeks, collagen remodeling can continue producing improvements for up to six months after treatment. Thinner-skinned areas sometimes show faster initial results because the treatment stimulus reaches the dermis more directly, but the total magnitude of improvement may plateau sooner due to the smaller volume of tissue available to thicken. This is why comparing your forehead healing to your cheek healing during the same treatment course can be confusing—they’re operating on different timelines and responding with different intensities. Patience is essential; declaring a treatment failed before the three-month mark is premature, regardless of skin thickness.

Matching Treatment Type to Your Skin Thickness and Scar Depth
Different treatment modalities interact with skin thickness in distinctly different ways. Laser therapy, particularly CO2 and Er:YAG lasers, achieves up to 90% efficacy for atrophic (depressed) acne scars through aggressive collagen remodeling and thermal contraction. These lasers work effectively across varying skin thicknesses because the provider controls energy delivery and can adjust wavelength and pulse duration. The thicker your skin, the deeper the laser penetrates and the more tissue it remodels; thinner skin responds with more superficial but still meaningful improvement.
Retinoids take a different approach entirely. A recent 2025 study found that the prescription retinoid trifarotene reduced atrophic scar count by 55.2% at week 24, with statistical significance visible as early as week 2. This makes retinoids particularly valuable for thin-skinned areas—they work through sustained cellular signaling and collagen production rather than controlled trauma, so there’s no safety ceiling based on skin thickness. The tradeoff is slower visible results and the requirement for daily application over months, compared to a laser’s dramatic single-session improvement. For many patients, combining retinoids with another modality offers the best outcome.
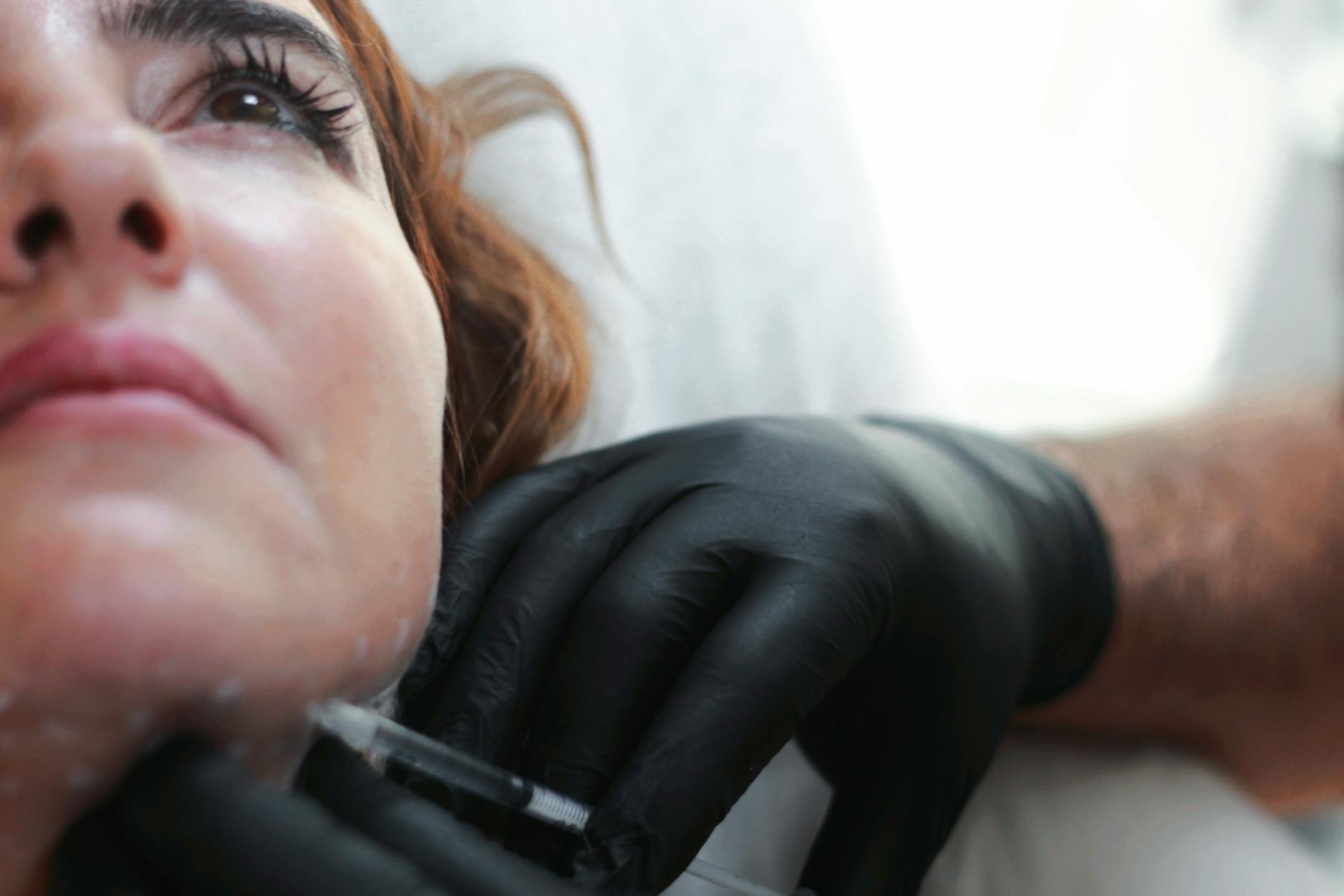
Injectable Fillers and the Practicality of Skin Thickness
Injectable hyaluronic acid fillers operate on a different principle altogether—they physically elevate depressed scars by adding volume beneath them. Cross-linked hyaluronic acid produces more than 50% improvement in boxcar scars after a single injection, with results lasting six to twelve months. The beauty of this approach is that it bypasses the skin thickness question entirely; a filler works the same whether your skin is thin or thick because it’s working below the surface rather than trying to remodel existing tissue.
However, fillers are not a permanent solution. They’re reabsorbed gradually over time, requiring repeat treatments every six to twelve months indefinitely if you want to maintain results. This makes them ideal for someone with a few isolated deep scars who wants immediate improvement, but less practical for extensive scar fields or as a long-term solution. On thin-skinned areas where other treatments carry more risk, fillers can be a sensible first step or interim option while you pursue more definitive approaches like laser therapy or retinoid therapy.
Emerging 2026 Therapies That Bypass Traditional Skin Thickness Limitations
The frontier of acne scar treatment is moving toward biologics and regenerative approaches that work with your body’s own healing machinery. Emerging therapies now include peptides, growth factors, and exosome-derived molecules designed to trigger healing-phase prevention—essentially coaching your skin to repair scars more aggressively from within. These approaches don’t rely on creating controlled trauma, so they sidestep many of the limitations imposed by skin thickness variation.
Autologous fibroblast transfer (cells harvested from your own skin and injected into scars) and PMMA microspheres in bovine collagen represent newer approved options that deliver longer-lasting results than temporary fillers. These interventions represent a shift toward stimulating or replacing the cellular machinery responsible for scar formation rather than just mechanically removing the scar tissue. For someone with extensive scarring across areas of varying thickness, these emerging options may offer more flexibility than earlier-generation treatments.
Planning Your Treatment Strategy Around Your Unique Skin Anatomy
The most successful scar treatment plans acknowledge skin thickness variation from the start. If your scars are concentrated on thick-skinned areas like the lower cheeks and jaw, aggressive laser therapy or deep microneedling can be your primary weapon, with retinoids as supporting therapy. If they’re spread across your entire face including thin-skinned areas, a staged approach using gentler modalities in sensitive zones and stronger treatment in resilient areas makes more sense. Your dermatologist should be mapping your face and explicitly discussing which areas get which depth settings—if they’re not, you’re likely not receiving optimal care.
This anatomical reality also explains why online before-and-afters can be misleading. Someone with thick cheek skin might achieve dramatic results with laser therapy, while someone with predominantly thin-skinned forehead scars might see the exact same laser produce underwhelming results. You’re not failing the treatment; the skin thickness is simply imposing different constraints. Understanding your own face’s topography of thickness is the first step toward realistic expectations and choosing the right treatment plan.
Conclusion
Skin thickness is not a minor variable in acne scar treatment—it’s a fundamental determinant of which scars form where, how deep treatments can safely reach, how quickly you’ll see results, and which modalities will work best for you. Cheeks and jaw allow more aggressive intervention and often show dramatic results; foreheads and temples require gentler approaches and sometimes longer timelines. Modern dermatology offers multiple effective pathways: lasers achieve up to 90% efficacy through collagen remodeling, retinoids produce 55% scar reduction with consistent application, fillers provide immediate but temporary elevation, and emerging biologics open new possibilities for extensive scarring across varied skin types.
Your next step is a consultation with a dermatologist who understands these thickness-based variations and will customize treatment parameters to your specific anatomy rather than applying a one-size-fits-all protocol. Bring photos of your scars and ask explicitly how treatment depth will change across your face. With a plan that respects your skin’s natural thickness variation, realistic timelines (visible improvement at six weeks, full results by three months), and potentially combined modalities, meaningful scar improvement is achievable for virtually any scar pattern.
You Might Also Like
- What Skin Laxity Has to Do with Acne Scar Appearance
- Why TotalFX Combines Both for Comprehensive Acne Scar Treatment
- Why Fluence and Energy Density Affect Acne Scar Treatment Results
Browse more: Acne | Acne Scars | Adults | Back | Blackheads





