Selective electrothermolysis is a targeted dermatological procedure that destroys hyperactive sebaceous glands—the root cause of acne—using high-frequency electrical current delivered through minimally invasive microneedle radiofrequency devices. Unlike topical creams that address surface symptoms or oral medications that work systemically, selective electrothermolysis works directly on the glands producing excess sebum, offering one of the most direct approaches to treating acne at its source.
A patient with severe inflammatory acne resistant to conventional treatments might see 98% reduction in inflammatory lesions within one month after completing a course of treatments, with visible improvement appearing in as little as 2-3 days. This article explores how selective electrothermolysis works, what clinical data shows about its effectiveness, what patients can expect during recovery, and whether it’s an appropriate option for your specific type of acne. Understanding this technology requires knowing both the science behind the procedure and the realistic outcomes based on peer-reviewed research.
Table of Contents
- How Does Selective Electrothermolysis Target Acne at the Source?
- What Do Clinical Results Actually Show About Effectiveness?
- Why Does Targeting Sebaceous Glands Work Better Than Surface Treatments?
- What Is the Actual Treatment Procedure and What Should You Expect?
- What Are the Side Effects and How Durable Are the Results?
- Combination Approaches and Emerging Research
- Who Is the Right Candidate, and What Does This Mean for Acne Treatment’s Future?
- Conclusion
How Does Selective Electrothermolysis Target Acne at the Source?
selective electrothermolysis works by inserting a specialized 1.5-mm needle with 0.45-mm of base insulation directly into acne pores, then applying high-frequency electrical current for 0.25-0.50 seconds at 40 W output. This creates a controlled thermal zone that selectively destroys the sebaceous gland tissue without damaging the surrounding epidermis. The procedure is “selective” because the radiofrequency energy targets only the gland itself, not the broader skin structure, minimizing collateral damage compared to older ablative approaches. The fundamental difference between this technology and other acne treatments is location and mechanism. Retinoids regulate cell turnover, antibiotics kill bacteria, and hormonal treatments reduce sebum production—but they don’t destroy the glands themselves.
Selective electrothermolysis permanently removes or significantly reduces the capacity of the sebaceous gland to produce excess sebum. For someone with chronic acne caused by overactive oil production, this represents a fundamentally different treatment category: not symptom management, but structural alteration of the tissue causing the problem. The procedure’s precision is what makes it effective for difficult cases. Someone with acne scarring and active inflammatory lesions cannot always be treated with lasers or chemical peels while they still have active breakouts. Selective electrothermolysis can be performed on active acne without waiting for lesions to heal first, since the treatment targets the gland, not the inflamed surface.

What Do Clinical Results Actually Show About Effectiveness?
The clinical data for selective electrothermolysis is remarkably strong. Peer-reviewed studies show a mean reduction of 98.14% in inflammatory acne lesions at one month after the final treatment session. For noninflammatory lesions (blackheads and whiteheads), the mean reduction is 83.09% at one month. Most patients achieved clinical success after 2-3 treatment sessions, spaced weeks apart. This level of improvement is unusual in dermatology—few treatments achieve near-total lesion reduction rates. The timeline of improvement is one of the most patient-relevant findings.
While conventional acne treatments require 6-12 weeks to show visible results, patients undergoing selective electrothermolysis saw improvement and lesion reduction visible within 2-3 days after treatment. At the 12-week follow-up point, improvements were statistically significant compared to control groups, with substantially reduced lesion counts maintained. However, the caveat is important: not all treatment benefits are permanent. One year after final treatment, clinically evident relapse occurred in 16.7% of patients (2 of 12 in the studied cohort), meaning some patients experienced return of acne lesions, though typically less severe than before treatment. For this reason, selective electrothermolysis is best understood as providing long-term remission for the majority of patients rather than a guaranteed permanent cure. The 83-98% effectiveness rates refer to lesion reduction immediately after treatment completion, not the percentage of patients remaining completely clear indefinitely. Someone who relapses may require touch-up treatments to return to clear skin.
Why Does Targeting Sebaceous Glands Work Better Than Surface Treatments?
Acne is fundamentally a disease of the sebaceous gland—excess sebum production, combined with bacterial colonization and inflammatory response, creates the comedones and cysts that characterize the condition. Topical treatments can reduce surface bacteria or increase skin cell turnover, but they cannot permanently reduce the gland’s capacity to produce oil. Systemic antibiotics work similarly, killing bacteria without addressing the overproduction that allows bacteria to thrive in the first place. Even isotretinoin, the most powerful oral acne medication, works by shrinking sebaceous glands but requires continuous use and carries significant risks. Selective electrothermolysis bypasses these limitations by directly removing or permanently disabling the tissue responsible for excess sebum production.
For someone with polycystic ovary syndrome (PCOS) or other hormonal drivers of acne, the gland is still overresponsive because the underlying endocrine system remains unchanged—however, the destruction of the gland means the overresponsive tissue is no longer present. One documented case involved a patient with severe acne and nephrotic syndrome (a serious kidney disease), where systemic treatments were contraindicated; selective electrothermolysis successfully treated the acne without requiring medication that could worsen kidney function. The limitation here is that this approach only works for acne caused by sebaceous gland activity. Someone with acne primarily driven by bacterial infections or follicular plugging without excess sebum may see less dramatic improvement. Similarly, if new acne is forming from comedone formation rather than sebaceous gland overflow, the treatment addresses one pathway but not all possible acne mechanisms. This is why proper diagnosis matters—confirming that excess sebum production is indeed a major component of your acne improves the likelihood of success.
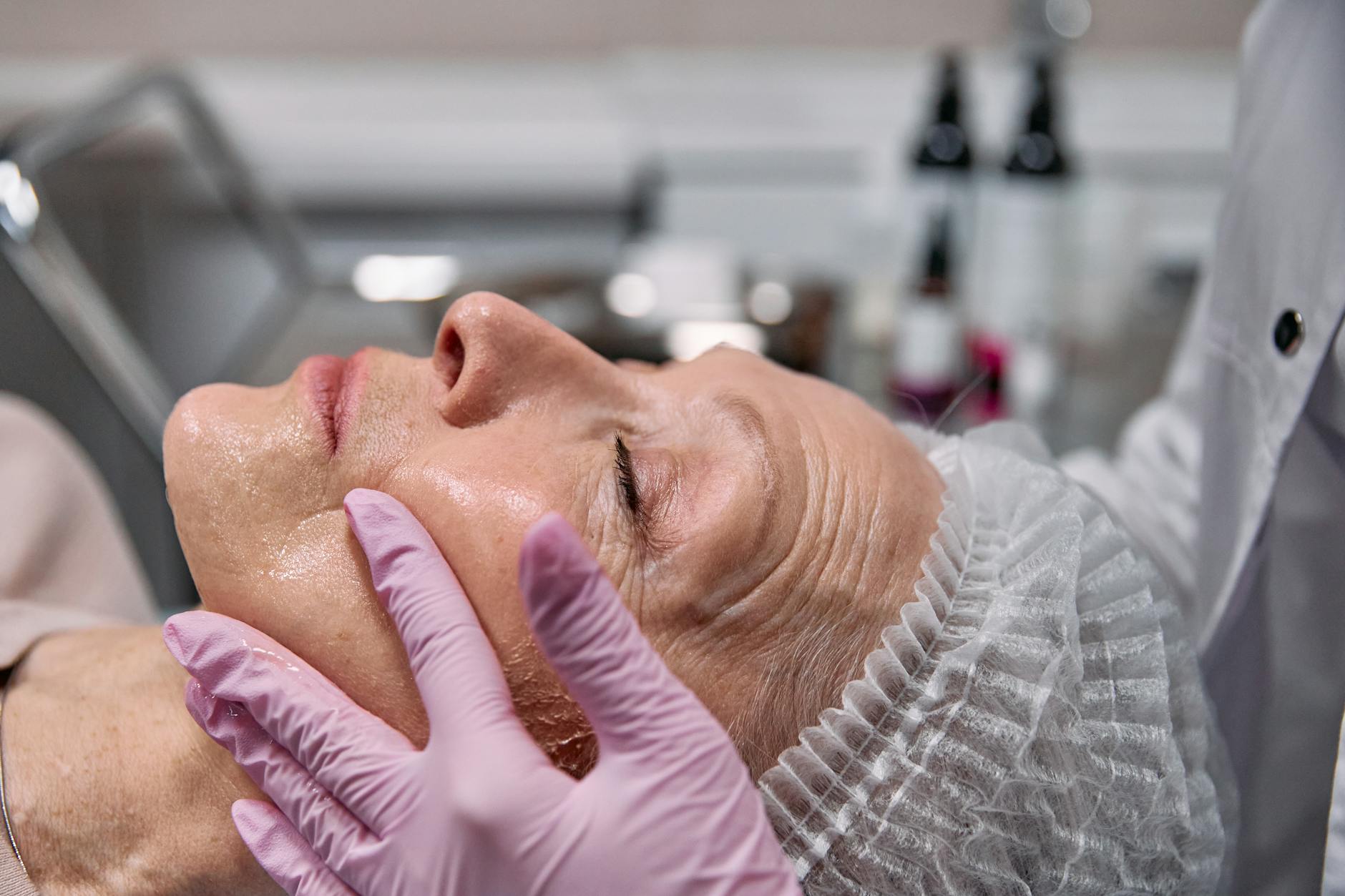
What Is the Actual Treatment Procedure and What Should You Expect?
A selective electrothermolysis treatment session involves numbing the skin with topical anesthetic, then using the specialized radiofrequency device to treat acne-affected areas. The 1.5-mm needle is inserted into individual pores or lesion sites, the current is applied for a fraction of a second, and the needle is withdrawn. Multiple lesions are treated in a single session. The entire procedure typically takes 20-45 minutes depending on the extent of acne being treated. Immediately after treatment, all patients experience transient post-treatment erythema—redness that fades within a few days.
Unlike ablative laser treatments that create visible wounds requiring longer healing, the radiofrequency approach produces erythema without significant visible damage. Most patients can return to normal activities within 1-2 days, making this more compatible with work and social schedules than more invasive procedures. The trade-off is that healing is faster but the procedure must be repeated 2-3 times to achieve maximum benefit; each session destroys additional sebaceous gland tissue, and multiple sessions provide cumulative effect. Most dermatologists space treatments 4-6 weeks apart, allowing skin to heal between sessions and sebaceous gland effects to fully develop. Someone comparing this to alternatives like oral isotretinoin (which requires months of continuous medication and monthly lab monitoring) would find the procedural approach less demanding overall, even though it requires multiple office visits. However, isotretinoin provides permanent total sebaceous gland shrinkage for 70-80% of patients, whereas selective electrothermolysis achieves this for a smaller subset but with fewer systemic side effects.
What Are the Side Effects and How Durable Are the Results?
The safety profile of selective electrothermolysis is excellent for a surgical-level treatment. The only consistent side effect observed in clinical trials was transient erythema (redness) that resolved within a few days. There were no cases of scarring, permanent pigmentation changes, or nerve damage in the published studies. The minimal epidermal damage is what allows this—the radiofrequency energy creates thermal zones focused on the sebaceous gland at depth, not the skin surface. The durability question is more complex. Relapse at one-year follow-up was 16.7%, meaning most patients maintained clear skin, but one in six experienced return of lesions.
This differs from isotretinoin, which achieves permanent remission in 70-80% but carries risks including teratogenicity (severe birth defects if used during pregnancy) and potential psychiatric effects. Selective electrothermolysis has no systemic risks, but patients should understand that relapse is possible and touch-up treatments may be needed. Someone who relapses typically sees a much milder form of acne than their baseline, suggesting partial gland regrowth rather than complete restoration. The long-term data comes from relatively small patient cohorts followed for one year. Larger, longer-term studies would clarify whether relapse rates change at 2-3 years post-treatment. For now, the realistic expectation is 12-18 months of clear skin for the majority of patients, with a minority requiring maintenance treatments.

Combination Approaches and Emerging Research
Recent research from 2022 examined combining selective sebaceous gland electrothermolysis with non-thermal plasma (NTP) treatment. This combination showed promise as a safe and effective option for refractory acne—acne resistant to conventional treatments. The rationale is that electrothermolysis destroys the gland while non-thermal plasma reduces inflammation and bacterial colonization, providing complementary effects.
This represents an emerging approach for patients whose acne hasn’t responded to other treatments. A patient who has failed multiple rounds of antibiotics, topical retinoids, and perhaps oral medications might be considered for this combination therapy. The data is preliminary, but the combination may allow lower energy settings for electrothermolysis while still achieving gland destruction, potentially reducing side effects. As with most emerging treatments, this would likely only be available at specialized dermatology centers rather than routine practices.
Who Is the Right Candidate, and What Does This Mean for Acne Treatment’s Future?
Selective electrothermolysis appears most appropriate for patients with moderate-to-severe inflammatory acne, particularly those with excess sebum production and lesions resistant to conventional treatments. Someone with mild acne might find topical retinoids and benzoyl peroxide sufficient. Someone with severe cystic acne might still choose isotretinoin as a definitive option, accepting its risks for guaranteed long-term remission.
The middle ground—patients with significant breakouts and documented sebaceous gland overactivity who want to avoid systemic medications—fits best with selective electrothermolysis. The future of acne treatment will likely involve more targeted approaches like this: instead of broad-spectrum antibiotics or hormonal changes, treatments that specifically address the tissue and mechanisms driving acne in individual patients. The combination of electrothermolysis with other modalities (plasma, laser, or topical adjuncts) may become standard for severe cases. For now, selective electrothermolysis represents a significant option between conventional topical/oral treatments and isotretinoin, filling a gap for patients seeking structural improvement rather than symptom suppression.
Conclusion
Selective electrothermolysis directly addresses acne’s root cause by destroying hyperactive sebaceous glands using focused radiofrequency energy delivered through microneedles. Clinical data shows dramatic lesion reduction—98% for inflammatory acne and 83% for noninflammatory lesions—often visible within days rather than weeks. The procedure carries minimal side effects beyond temporary redness and requires 2-3 sessions spaced weeks apart, making it less burdensome than many systemic alternatives.
The key consideration is durability: while most patients maintain clear skin for one year post-treatment, 16.7% experience relapse requiring touch-up treatments. For someone with treatment-resistant, sebaceous-gland-driven acne, selective electrothermolysis offers a middle path between conventional management and systemic medications. Consulting with a dermatologist experienced in radiofrequency treatments can determine whether your specific acne presentation would benefit from this targeted approach.
You Might Also Like
- What Agnes RF Selective Sebaceous Gland Treatment Does for Acne
- Why Sebacia Microparticle Treatment Works for Acne
- What PicoSure Pro Does for Acne Pigmentation and Texture
Browse more: Acne | Acne Scars | Adults | Back | Blackheads





