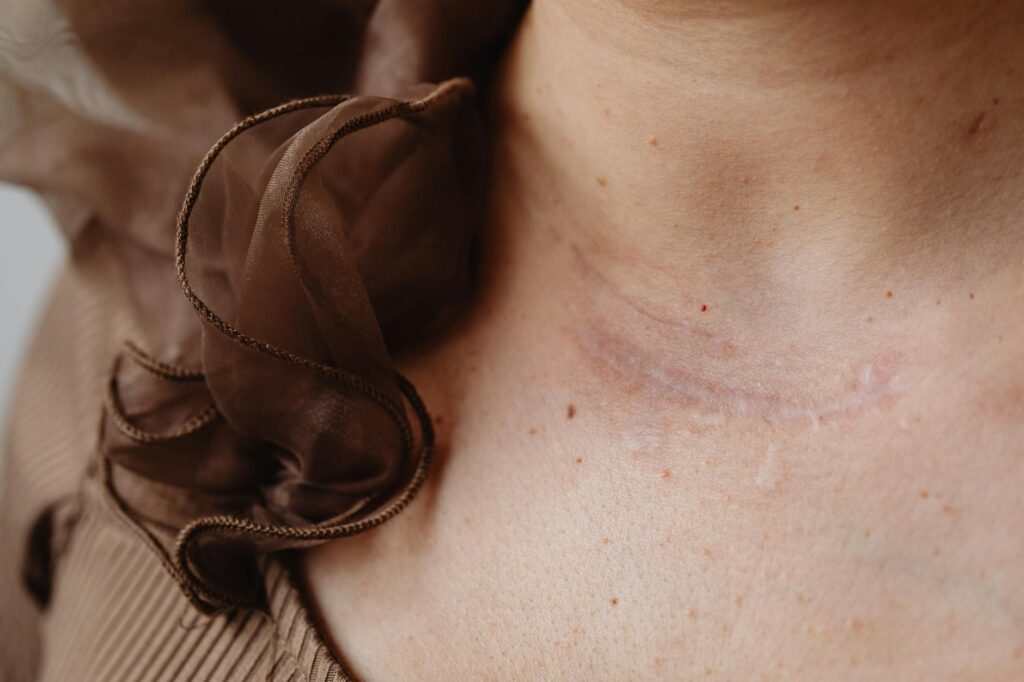
PMMA in Bellafill provides permanent scar correction through a two-phase mechanism: the surrounding collagen gel fills depressed acne scars immediately, while the 20% PMMA microspheres remain in place permanently to stimulate your body’s own collagen production. This dual approach makes Bellafill unique—unlike traditional fillers that dissolve completely, the PMMA creates a lasting scaffold beneath the skin that can maintain scar improvement for years.
If you’ve struggled with boxcar or rolling acne scars that don’t respond to topical treatments or laser therapy, Bellafill offers a genuinely different option because it’s not just filling a hole—it’s triggering your skin to rebuild itself. This article explains exactly how PMMA microspheres work within Bellafill, what the clinical data shows about results, who should consider this treatment, potential side effects, and how it compares to other scar correction options. We’ll cover the mechanism that makes Bellafill permanent, real efficacy numbers from FDA clinical trials, the timeline for seeing results, and practical considerations before treatment.
Table of Contents
- How PMMA Microspheres Create Permanent Scar Elevation
- Duration of Results and What Studies Actually Show
- What the Clinical Data Says About Improvement Rates
- Bellafill Compared to Other Scar Correction Options
- Safety Profile and What Adverse Events Actually Occurred
- Timeline for Results and the Collagen Maturation Phase
- The Evolving Role of PMMA in Scar Treatment
- Conclusion
How PMMA Microspheres Create Permanent Scar Elevation
bellafill‘s formulation contains 20% PMMA (polymethylmethacrylate) microspheres suspended in 80% bovine collagen gel, plus lidocaine for comfort during injection. The PMMA spheres are precisely engineered—sized at 30-42 microns in diameter, uniform and smooth—with approximately 6 million microspheres packed into each syringe. When injected into a depressed scar, these microscopic beads don’t dissolve; instead, they become encapsulated by your body’s fibrous tissue and act as a permanent scaffold. The mechanism unfolds in two distinct phases. In the immediate phase (days to weeks), the collagen gel provides instant filling that elevates the scar.
Over the next one to four months, your body naturally absorbs the collagen gel, but the PMMA microspheres remain exactly where they were placed. During this absorption period, the PMMA scaffold stimulates neocollagenesis—your skin’s own collagen production—which builds new connective tissue around and over the beads. This is why Bellafill can deliver results that last far longer than traditional fillers: you’re not relying on the filler itself to stay; you’re relying on your skin to rebuild itself using the PMMA as a framework. Unlike hyaluronic acid fillers that your body breaks down completely within 6-12 months, Bellafill’s permanence means you’re making a long-term commitment. However, this permanence is also an advantage if the scar correction works well—you don’t need annual touch-ups to maintain the result, which compounds savings over time.

Duration of Results and What Studies Actually Show
The FDA approved Bellafill for acne scar treatment with a minimum duration claim of 1 year, though durability data extends much further. Clinical studies followed patients for up to 12 months, with 71% of subjects maintaining efficacy at the one-year mark. A larger 5-year safety and efficacy study involving 1,008 patients across 23 U.S. centers was completed, providing longer-term insight into how Bellafill performs over extended periods.
Here’s the important caveat: the FDA’s 1-year minimum claim reflects what was proven in controlled clinical trials, but many patients report results lasting longer—potentially 5 years or more. However, beyond the FDA-approved claims and the 5-year study data, long-term durability isn’t confirmed in rigorous controlled studies for acne scars specifically. Some patients may see gradual fading of results over 3-5 years as the skin’s metabolism changes, or the scar may begin returning if significant trauma or sun damage occurs in that area. If you’re expecting permanent scar correction to mean “never think about this scar again,” it’s more accurate to say “significantly improved results that last years, with possible maintenance treatments down the line if needed.” The permanence of PMMA is real, but results depend on individual healing and how your body produces collagen around the microspheres. Someone with excellent collagen-building capacity may see more durable results than someone with limited fibroblast activity.
What the Clinical Data Says About Improvement Rates
The clinical evidence for Bellafill’s effectiveness in acne scars is substantial. In the FDA-reviewed trial with 147 subjects, Bellafill achieved a 64% response rate (improvement on the Acne Scar Assessment Scale) compared to 33% for saline control at 6 months—a statistically significant difference (p=0.0005). At 4 months, 92% of subjects showed at least 1-point improvement on the scar assessment scale, and by 7 months, that number rose to 95%, with 97% classified overall as “improved or better.” These aren’t marginal improvements. A 1-point improvement on the Acne Scar Assessment Scale represents visible, measurable elevation of depressed scars.
When 95% of patients show improvement, that’s a substantially higher success rate than many alternative scar treatments. However, important context: these trials enrolled patients with moderate to severe atrophic scars (rolling or boxcar types), not all acne scar morphologies. If you have raised or keloid-type scars, Bellafill is not suitable and won’t produce the same results. The 12-month follow-up data showing 71% efficacy maintains the improvement, though the slight decline from 7-month data suggests some patients experience modest softening of results over time. Individual variation is significant—some patients maintain near-identical results for years, while others notice gradual fading.
Bellafill Compared to Other Scar Correction Options
Bellafill operates in a distinct category compared to other scar treatments. Laser resurfacing (CO2, fractional) is temporary, requiring repeat sessions to maintain results, and carries risk of post-inflammatory hyperpigmentation, especially in darker skin tones. Microneedling works by inducing controlled collagen remodeling but requires a series of treatments and shows more modest results for severe atrophic scars. Chemical peels address surface texture but don’t elevate deep boxcar or rolling scars meaningfully. Subcision physically breaks scar tissue adhesions and can be combined with other treatments, but works best for tethered scars and alone doesn’t provide lifting.
Bellafill’s advantage is permanence and sustained lifting—one well-placed treatment can improve a scar for years, whereas lasers, microneedling, and peels require ongoing maintenance. The tradeoff is cost upfront (typically $800-2,000 per syringe depending on scar depth and size) and the fact that if you’re not satisfied with the result, PMMA can’t be easily removed. Some practitioners can attempt removal via punch excision or conservative extraction, but it’s not reliably reversible like dissolving a hyaluronic acid filler. For severe, extensive atrophic scarring, combination therapy often works best: subcision followed by Bellafill, or Bellafill combined with later laser resurfacing once collagen has fully matured (3-6 months post-injection). Individual scar anatomy and skin type should guide the choice, which is why dermatologic assessment before treatment is essential.
Safety Profile and What Adverse Events Actually Occurred
The FDA’s safety database for Bellafill’s nasolabial fold study (1,128 subjects) documented 1 severe adverse event (a granuloma) and 14 moderate adverse events. Granulomas—inflammatory nodules that form around foreign material—are rare but possible with PMMA fillers and may require treatment. Most reported adverse events were temporary injection-site reactions: redness, swelling, bruising, tenderness. More serious complications like infection, allergic reaction, or vascular occlusion (accidental injection into a blood vessel) are possible but uncommon when administered by trained practitioners. A critical safety point: Bellafill contains bovine collagen, and patients with bovine collagen allergy or a history of severe allergy to lidocaine should not receive it. The FDA requires an allergy test (intradermal injection of test material) 24-48 hours before the actual treatment to screen for bovine collagen sensitivity.
Approximately 3-5% of patients show mild allergy reactions on testing. This isn’t a barrier to treatment—it’s a screening step—but it means treatment can’t happen on the day of consultation; you need a separate appointment. Importantly, Bellafill has not been withdrawn from the market for safety or efficacy concerns. It remains FDA-approved and widely used, with the 5-year safety study confirming long-term tolerability. However, like any injectable, it carries inherent risks. Infection, overcorrection, asymmetry, or dissatisfaction with appearance are real possibilities, which is why choosing an experienced practitioner matters significantly.

Timeline for Results and the Collagen Maturation Phase
Results appear in stages. Immediately after injection, swelling elevates the scar further, creating an overcorrected appearance that settles within hours to days. Over the first month, the visible improvement from the collagen gel is clear, and this is when most patients see the most dramatic change. From month 1 to 4, the collagen gel is gradually absorbed, and you might notice the scar appearing slightly more depressed again as collagen resorbs—this is normal and doesn’t mean the treatment failed. Between months 1 and 6, neocollagenesis (your body’s collagen production around the PMMA microspheres) kicks in.
This is when many patients report that results actually improve again or stabilize, as your own collagen builds beneath the scar. By 6-7 months, collagen maturation is largely complete, and you see the final aesthetic result. This extended timeline is important to understand: patients expecting full results by 2 weeks will be disappointed. If you’re considering Bellafill, plan for a visible scar elevation that improves over months, not days. Touch-up injections, if needed, are typically done 2-3 weeks after the initial treatment while some original material remains in place, allowing the practitioner to refine the correction. After that, any future adjustments should wait until collagen maturation is complete at 6+ months.
The Evolving Role of PMMA in Scar Treatment
PMMA-based fillers like Bellafill represent an important evolution in scar correction because they address a fundamental problem: temporary fillers require repeat treatments, while surgical scar revision carries permanent change. Bellafill occupies a middle ground—a semi-permanent to permanent improvement that relies on stimulating your body’s own tissue regeneration rather than relying solely on the injected material. Newer research continues exploring variations on PMMA technology, including different microsphere sizes and formulations, as well as combined approaches (PMMA with other stimulating agents).
The field is also expanding into other permanent and semi-permanent fillers. However, Bellafill’s 20-year track record (FDA-approved since 2006) and substantial clinical data make it one of the most evidence-supported options in this category. As regenerative medicine advances, PMMA-based approaches will likely remain relevant, though combination therapies—PMMA plus growth factors, stem cell-conditioned media, or other collagen-stimulating treatments—may become more common.
Conclusion
PMMA in Bellafill corrects permanent scars by doing two things simultaneously: the collagen gel provides immediate mechanical filling while the PMMA microspheres create a permanent scaffold that stimulates your body to produce its own collagen. Clinical data shows 64-95% of patients with atrophic acne scars experience meaningful improvement, with results lasting at least 1 year and often much longer. This makes Bellafill distinct from temporary fillers and less invasive than surgical scar revision, though it requires experienced administration and carries the permanence of an injectable foreign material.
If you’re considering Bellafill for acne scar correction, the critical first step is a consultation with a board-certified dermatologist who can assess your scar type (Bellafill works for rolling and boxcar scars but not raised or keloid types), perform allergy testing, and discuss realistic expectations. Results unfold over months, not weeks, and while the improvement can be substantial and long-lasting, it’s not universally perfect—combination therapy with other treatments often yields the best aesthetic outcomes for extensive scarring. Understanding the mechanism, the timeline, and the limitations ensures you make an informed decision about whether this treatment aligns with your scar correction goals.
You Might Also Like
- What Juvederm Voluma Does for Acne Scar Volume Correction
- Why Medical-Grade Skincare Matters for Acne Scar Patients
- Why Bellafill Is the Only FDA-Approved Filler for Acne Scars
Browse more: Acne | Acne Scars | Adults | Back | Blackheads