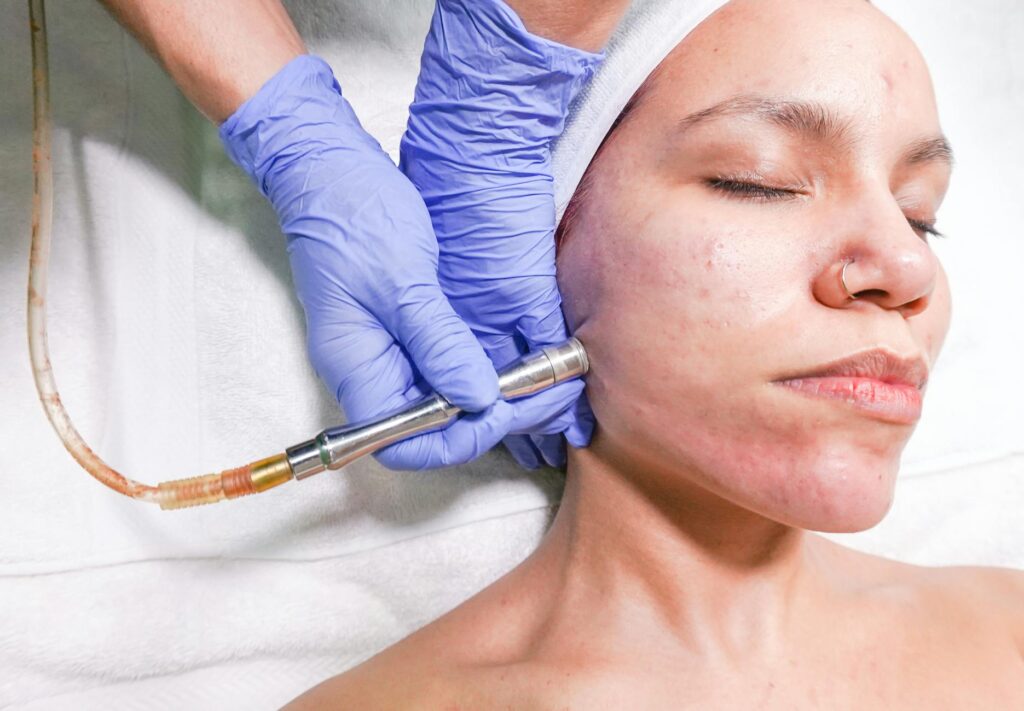
Ozone therapy at dermatology clinics claims to treat acne by using ozone gas or ozonated oils to reduce bacteria and inflammation, but scientific evidence does not support these claims. The FDA classifies ozone as a toxic gas without proven medical benefits and has not authorized it for any medical condition, including acne. Despite this regulatory stance, some clinics across the United States advertise ozone therapy for acne treatment, particularly in states with “health freedom” legislation that allow unapproved treatments. This article examines what ozone therapy purports to do, what the actual research shows, and how it compares to treatments with established evidence for acne.
Table of Contents
- How Clinics Claim Ozone Therapy Treats Acne
- What Scientific Studies Actually Show About Effectiveness
- FDA Regulatory Status and What It Means
- How Ozone Therapy Is Administered in Clinical Settings
- Comparing Ozone to Treatments with Proven Evidence
- Why People Still Pursue Ozone Therapy Despite Lack of Evidence
- What the Future May Hold for Ozone in Dermatology
- Conclusion
How Clinics Claim Ozone Therapy Treats Acne
Practitioners who offer ozone therapy argue that ozone has antimicrobial, anti-inflammatory, and wound-healing properties that theoretically could benefit acne-prone skin. The proposed mechanism involves oxidative reactions where ozone interacts with biological membranes to kill bacteria and reduce inflammation. Acne, caused primarily by the bacterium *Cutibacterium acnes* (formerly *Propionibacterium acnes*), develops when pores become blocked and bacteria multiply, triggering an immune response.
If ozone could effectively target these bacteria and calm inflammation, it might theoretically help—but this is where theory diverges sharply from evidence. Clinics offer ozone therapy through several methods: local subcutaneous injections near affected areas, topical applications of ozonated water, or ozonated olive oil preparations that patients use at home. A patient receiving subcutaneous ozone injection for acne would have small amounts of gas injected into or under the skin, intended to kill acne bacteria and reduce cyst formation. Topical ozonated products are marketed as gentler alternatives that supposedly deliver ozone’s benefits without needles, though how effectively ozone survives in bottled solutions remains unclear.

What Scientific Studies Actually Show About Effectiveness
The most significant problem with ozone therapy for acne is that clinical evidence simply does not support its use. A systematic review of ozone therapy for dermatological conditions published in peer-reviewed research concluded that “it is still not possible to support an evidence level of ozone therapy for treatment of acne” due to significant methodological limitations in existing studies. These limitations include inadequate sample sizes, lack of proper control groups, and insufficient documentation of adverse effects. More concerning, specific studies examining ozone’s effect on acne showed no benefit.
One trial found that high-frequency ozone treatment produced no reduction in acne lesion count compared to a control group that received only standard skin cleansing. Additionally, laboratory research testing topical ozone gas against *Cutibacterium acnes* bacteria found it to be ineffective at killing the primary acne-causing organism. These results suggest that even if clinics administer ozone exactly as intended, the treatment may not address the biological drivers of acne. The research shows “significant methodological shortcomings” with inadequate information on patient blinding, control factors, and long-term adverse effects—meaning that better-designed trials are needed before any conclusions can be drawn.
FDA Regulatory Status and What It Means
The FDA classifies ozone as a toxic gas and explicitly states that it has “no known useful medical application in specific, adjunctive, or preventive therapy” (21 CFR 801.415). The agency has not approved ozone for treatment of any medical condition, including acne, skin infections, or wound healing. This is not a gray area or a matter of incomplete review—the FDA’s position reflects decades of evidence and regulatory assessment.
Clinics that advertise ozone therapy for acne are promoting an unapproved medical treatment. Why do some clinics continue to offer it? In states with less restrictive regulations or “health freedom” laws, dermatology and cosmetic practices can advertise ozone therapy with FDA disclaimers, essentially telling patients “the FDA says this doesn’t work, but we’ll provide it anyway if you want it.” This creates a situation where patients may encounter marketing claims that sound scientific and hopeful while regulatory agencies have determined the treatment lacks demonstrated benefit. The existence of clinics offering a treatment does not mean the treatment is effective—it means a market exists for unproven options.

How Ozone Therapy Is Administered in Clinical Settings
If you visit a clinic offering ozone therapy for acne, the procedure would likely involve one of three delivery methods. Subcutaneous injection involves using a small needle to introduce ozone gas directly into or beneath acne lesions or affected skin areas—a procedure that carries risks of infection, tissue damage, and the systemic effects of injecting gas into tissue planes. The patient may experience discomfort, bruising, or temporary swelling at injection sites.
Topical ozonated water or oil is applied directly to the skin, either as a rinse, mask, or moisturizer; this is presented as lower-risk but raises questions about how long ozone remains active in a liquid product and whether it penetrates skin effectively. Some clinics combine ozone with other treatments, such as applying it alongside conventional acne medications or light therapy, which makes it harder to determine what, if anything, is actually responsible for any improvement. A patient might see some acne improvement and attribute it to ozone when the improvement actually resulted from the conventional treatment or simply natural skin healing. Without proper clinical trials using matched comparison groups, it is impossible to know whether ozone contributes any benefit.
Comparing Ozone to Treatments with Proven Evidence
The contrast between ozone therapy and evidence-based acne treatments is stark. Topical retinoids (vitamin A derivatives like tretinoin or adapalene) have decades of research showing they reduce acne lesion counts by 40-80% and prevent new lesions from forming. Benzoyl peroxide kills acne bacteria and is supported by extensive clinical evidence. Oral antibiotics like doxycycline reduce bacterial load and inflammation, with well-documented efficacy.
Isotretinoin (Accutane) is reserved for severe acne but can completely clear acne and prevent scarring in most patients—with trade-offs in side effects that are well-understood and monitored. Ozone therapy, by contrast, lacks even a single well-designed clinical trial showing it works better than placebo or standard care. If you have moderate acne, a dermatologist would likely recommend a topical retinoid, benzoyl peroxide, or both—treatments that work—rather than an unproven injection. For severe acne, isotretinoin is a real option despite its risks, because the evidence of benefit is unambiguous. Ozone therapy occupies a unique category: heavily marketed, frequently offered, but with no credible evidence of effectiveness and regulatory agencies explicitly saying it doesn’t work.

Why People Still Pursue Ozone Therapy Despite Lack of Evidence
Patient interest in ozone therapy for acne stems from several understandable sources. Some people have had negative experiences with conventional acne treatments—isotretinoin’s side effects, antibiotics’ concerns about resistance, or topical treatments’ irritation—and seek alternatives. Others are drawn to treatments framed as “natural” or “holistic,” even though natural does not equal safe or effective. Clinics offering ozone benefit from the perception that it is a cutting-edge or exclusive treatment, and marketing materials often highlight theoretical mechanisms without acknowledging the absence of clinical proof.
Additionally, acne improvement is common over time simply due to skin maturation and natural healing, independent of any treatment. A patient receiving ozone therapy who sees their acne improve may attribute the improvement to the treatment, even though the same improvement might have occurred with proper cleansing and sunscreen alone. This is why clinical trials with control groups exist—to separate real treatment effects from coincidental improvement. Without such trials for ozone therapy, personal stories of improvement tell us very little about whether the treatment caused the result.
What the Future May Hold for Ozone in Dermatology
Ozone therapy’s status in clinical dermatology is unlikely to change dramatically without rigorous research demonstrating efficacy. Well-designed, adequately powered clinical trials with proper blinding and control groups are the only way to establish whether ozone therapy has any role in acne treatment.
Such trials have not been conducted, and given that simpler, cheaper, and more effective acne treatments already exist, there is little commercial incentive to fund expensive trials for ozone. Some dermatologists keep an eye on research suggesting ozone may have immunomodulatory effects in other conditions, but for acne specifically, the existing evidence—including studies showing no effect against the primary acne bacterium—suggests that ozone is unlikely to emerge as a valid treatment. If you are considering ozone therapy for acne in 2026, you are essentially enrolling yourself in an uncontrolled experiment without regulatory oversight or evidence of benefit.
Conclusion
Ozone therapy at clinics does not have credible evidence showing it treats acne effectively. The FDA classifies ozone as a toxic gas without proven medical benefits and has not approved it for any condition. Studies that have examined ozone for acne treatment have shown no benefit over control groups, and laboratory research found ozone ineffective against the primary acne-causing bacterium.
Despite this lack of evidence, some clinics continue to advertise ozone therapy, particularly in regulatory environments that allow unapproved treatments. If you are dealing with acne, science-backed options like topical retinoids, benzoyl peroxide, and oral antibiotics have strong evidence of effectiveness. For severe acne resistant to these approaches, isotretinoin remains the most powerful option. Consulting a dermatologist who stays current with acne research will connect you with treatments proven to work rather than unproven therapies that sound promising but lack the evidence to back up their claims.
You Might Also Like
- What Wnt Signaling Inhibition Does for Sebocyte Activity in Acne
- What TNF-Alpha Blocking Does for Inflammatory Acne
- What Naltrexone Low-Dose Does for Inflammatory Skin and Acne
Browse more: Acne | Acne Scars | Adults | Back | Blackheads