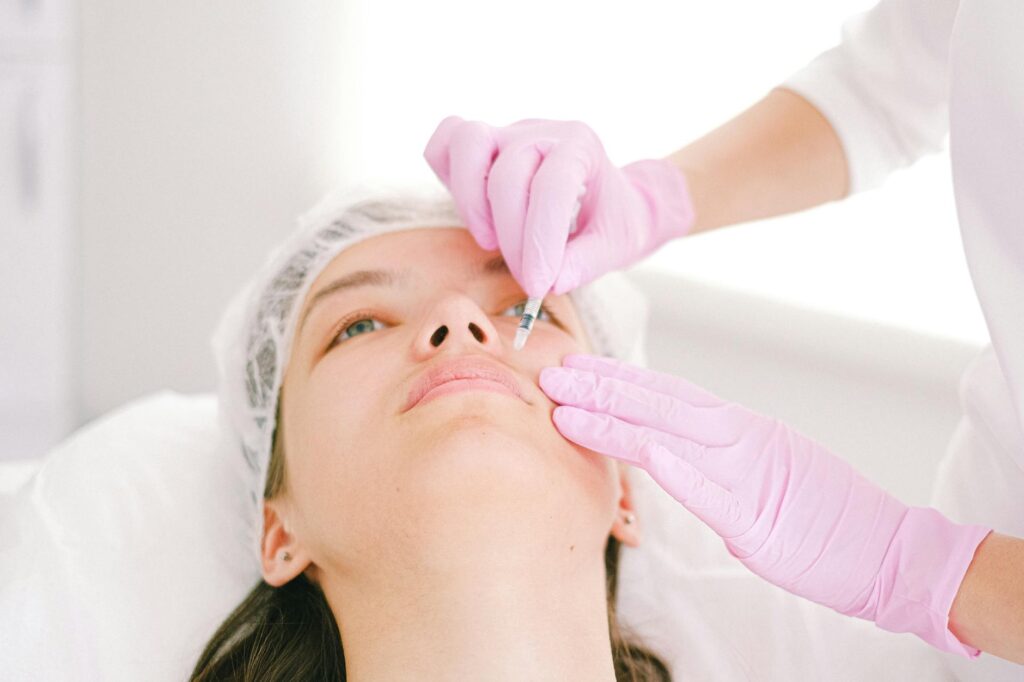
IGF-1 (Insulin-like Growth Factor 1) directly stimulates dermal fibroblasts to increase collagen production and remodeling, which is why it has become a focus in scar treatment research. When fibroblasts—the cells responsible for maintaining skin structure—are activated by IGF-1, they work harder to synthesize new collagen and break down old, disorganized collagen in scarred tissue.
This increased activity helps fill depressed scars and improve skin texture over time. For someone with rolling acne scars from years of breakouts, IGF-1 therapy essentially tells the skin’s repair cells to “get back to work,” encouraging them to rebuild the underlying structure that acne damage destroyed. This article covers how IGF-1 works at the cellular level to improve scarring, which treatments actually deliver IGF-1 to fibroblasts effectively, what the limitations are, and whether it’s a realistic option for different types of scars.
Table of Contents
- How Does IGF-1 Activate Dermal Fibroblasts to Rebuild Scar Tissue?
- Why IGF-1 Is More Effective Than Simple Collagen Injection
- Different Delivery Methods and Their Effectiveness
- Combining IGF-1 with Other Scar Treatments for Better Results
- Limitations and Factors That Reduce IGF-1 Effectiveness
- Real-World Expectations: What Improvement Actually Looks Like
- Future Developments and Emerging IGF-1 Therapies
- Conclusion
How Does IGF-1 Activate Dermal Fibroblasts to Rebuild Scar Tissue?
IGF-1 binds to specific receptors on fibroblasts, triggering a cascade of molecular signals that tells these cells to enter a more active state. Once activated, fibroblasts ramp up their production of Type I and Type III collagen—the main structural proteins in healthy skin. This is particularly important for scars because scar tissue typically has disorganized collagen fibers arranged haphazardly, unlike the neat, parallel arrays found in normal skin. An activated fibroblast population doesn’t just make more collagen; they also produce matrix metalloproteinases (MMPs), enzymes that selectively break down old, cross-linked collagen that makes scars stiff and visible.
The net result is scar remodeling rather than simple filling. In a depressed acne scar, for example, IGF-1-stimulated fibroblasts gradually rebuild the dermis beneath the scar, lifting the skin surface. However, this process is slow—real improvements typically take weeks to months—and it works best in scars that are still in an active remodeling phase (within a year or two of formation). Older scars with fully mature, calcified scar tissue respond less effectively because the fibroblasts have fewer signals telling them to keep remodeling.
Why IGF-1 Is More Effective Than Simple Collagen Injection
Unlike dermal fillers, which sit passively under the skin until your body absorbs them, IGF-1 works by activating the skin’s own repair machinery. A filler like hyaluronic acid plumps a scar immediately but provides no lasting benefit—once absorbed (usually within 6–12 months), the scar returns to its original depth. IGF-1, by contrast, encourages the skin to build its own collagen, creating changes that can persist long after treatment stops. However, IGF-1 has a critical limitation: it doesn’t reach fibroblasts easily through topical application.
The molecule is large and the skin barrier blocks it, so any IGF-1 cream you buy over the counter likely has minimal effect on actual fibroblast activity. This is why medical treatments—such as microneedling combined with IGF-1 serum, or injected growth factor solutions—are necessary to see real results. Even then, IGF-1 works best on fresh, shallow scars. A pitted ice-pick scar that’s 3mm deep won’t be fully erased by IGF-1 alone because there simply isn’t enough dermis for fibroblasts to rebuild.
Different Delivery Methods and Their Effectiveness
Microneedling with IGF-1 application is one of the most accessible medical approaches. The microneedling creates controlled micro-injuries that activate the skin’s natural healing cascade, while the IGF-1 serum applied afterward penetrates through the created channels and reaches deeper layers where fibroblasts reside. Studies show modest but measurable improvement in scar depth and texture, particularly when multiple sessions are spaced 4–6 weeks apart to allow fibroblast activity to cycle. Direct injection of IGF-1 or growth factor cocktails is more aggressive and more expensive but can deliver higher concentrations directly to the scar bed.
Some dermatologists use autologous platelet-rich plasma (PRP), which contains naturally high IGF-1 and other growth factors, injected directly into scars. PRP studies show variable results—some patients see 30–50% improvement in scar appearance, while others see minimal change. The variation depends on how active the scar is, the patient’s age and healing capacity, and whether the practitioner is skilled at delivering the treatment to the correct depth. Younger patients with newer scars generally respond better than older patients with chronic scars.

Combining IGF-1 with Other Scar Treatments for Better Results
IGF-1 therapy rarely works in isolation for moderate to severe scarring. Combining it with other modalities often produces better outcomes. For instance, using laser resurfacing (which removes the top layer of scar tissue) followed by IGF-1 treatment gives fibroblasts a “head start”—the laser removes the damaged surface, and IGF-1 stimulates rebuilding below. Some practitioners also combine IGF-1 with chemical peels or subcision (cutting the fibrous bands beneath depressed scars) to maximize remodeling potential.
The tradeoff is cost and downtime. A single microneedling with IGF-1 session might cost $400–$800 and requires minimal recovery. A series of three sessions over 12 weeks runs $1,200–$2,400. Adding laser or subcision doubles or triples the cost but may produce noticeably better results in 6–12 months. Patients with severe scarring often find combination therapy necessary, while those with mild surface irregularities might achieve acceptable results with IGF-1 alone.
Limitations and Factors That Reduce IGF-1 Effectiveness
IGF-1 stimulates fibroblast activity, but it cannot overcome all types of scarring. Box-scar (broad, shallow depressions) responds better than ice-pick scarring (narrow, deep pits) because fibroblasts can rebuild the broader surface area more effectively. In ice-pick scars, the depth often exceeds what fibroblasts can reasonably fill through collagen synthesis alone. Additionally, patients with darker skin tones sometimes experience post-inflammatory hyperpigmentation or keloid formation if IGF-1 treatment is too aggressive, requiring more conservative dosing and spacing between treatments.
Age and skin condition also matter significantly. Teenagers and people in their 20s have more robust fibroblast responses to growth factors; patients over 50 or with conditions like diabetes may see slower or less dramatic results because their fibroblasts respond more sluggishly to signals. Sun damage, smoking, and poor collagen turnover all dampen the effectiveness of IGF-1 therapy. Someone who has invested in IGF-1 treatment but continues heavy sun exposure without sunscreen will see their results fade faster because ongoing sun damage disrupts the collagen remodeling that IGF-1 initiated.

Real-World Expectations: What Improvement Actually Looks Like
Published studies on IGF-1 and similar growth factor treatments for scars typically report 30–60% improvement in scar depth and texture after a series of treatments. That sounds promising, but it’s important to understand what this means in practice. A scar that was 2mm deep might become 1.2mm deep—still visible in certain lighting but noticeably less pronounced.
Surface roughness often improves more dramatically than depth because fibroblasts can remodel the texture layer more easily. Many patients find that combining visual improvement with psychological acceptance is realistic. After three microneedling sessions with IGF-1, a person with moderate acne scarring might see about 40% improvement, which often translates to feeling significantly more confident because the scars are no longer the first thing they notice when looking in the mirror. However, complete erasure of scarring is rare unless the scars were quite shallow to begin with.
Future Developments and Emerging IGF-1 Therapies
Research into growth factor delivery is evolving rapidly. Scientists are developing new formulations—such as encapsulated IGF-1 in nanoparticles—designed to penetrate deeper into skin or last longer once applied. Some experimental approaches use gene therapy or stem cell-derived factors to stimulate fibroblast activity more durably.
These emerging therapies remain mostly in clinical trials, but within the next 5–10 years, they may offer more effective and longer-lasting scar improvement than current topical or injected IGF-1 treatments. The direction of the field suggests moving toward combination therapies that are more personalized—tailored to a patient’s skin type, scar characteristics, and healing capacity. Rather than a one-size-fits-all approach, future dermatology may involve genetic or molecular testing to predict who will respond best to IGF-1 versus other growth factors or entirely different mechanisms.
Conclusion
IGF-1 is a legitimate tool for improving acne scars by directly stimulating fibroblasts to rebuild collagen and remodel scar tissue. It works best on fresh, shallow to moderate scars and when delivered through medical treatments like microneedling, PRP injection, or direct infusion. Results are gradual, taking 2–6 months to become apparent, and improvement typically ranges from 30–60% rather than complete scar elimination.
If you have active acne scarring and are considering treatment, IGF-1 therapy—especially combined with complementary modalities like laser or microneedling—is worth discussing with a board-certified dermatologist. Realistic expectations and patience are essential; you’re asking your skin cells to do repair work that takes time, not seeking an instant fix. A skilled practitioner can help you determine whether IGF-1 is appropriate for your specific scars and whether it should be combined with other treatments for optimal results.
You Might Also Like
- What ADSC-Exosome Combination Does for Fibroblast Activity in Scars
- What Wnt Signaling Inhibition Does for Sebocyte Activity in Acne
- What Platelet-Rich Fibrin (PRF) Does vs PRP for Acne Scars
Browse more: Acne | Acne Scars | Adults | Back | Blackheads