Hydroquinone compound creams work by inhibiting tyrosinase, the enzyme responsible for melanin production in your skin, which allows them to fade acne dark spots and post-inflammatory hyperpigmentation over time. When applied consistently at standard concentrations of 2-4%, hydroquinone can significantly reduce the appearance of these spots—70% of patients notice clearance or noticeable reduction in pigmentation within three months of twice-daily use. For someone with moderate acne scarring and stubborn brown marks left behind, a prescription 4% hydroquinone cream prescribed by a dermatologist can be one of the most clinically proven treatments available, though it comes with important limitations and safety considerations that should guide its use. This article explores exactly how hydroquinone creams treat dark spots, what the clinical evidence shows about their effectiveness, the concentrations and prescription requirements, important safety limits, potential side effects, and when they work best—or when they might not be suitable for your skin type.
Table of Contents
- How Hydroquinone Inhibits Melanin Production and Fades Dark Spots
- Clinical Effectiveness Timeline and What Research Shows
- Prescription Requirements and Available Concentrations
- Maximum Duration and the Critical Three-Month Limit
- Side Effects and Risks to Monitor
- Who Benefits Most and Skin Type Considerations
- Combining Hydroquinone with Other Acne Scar and Dark Spot Treatments
- Conclusion
How Hydroquinone Inhibits Melanin Production and Fades Dark Spots
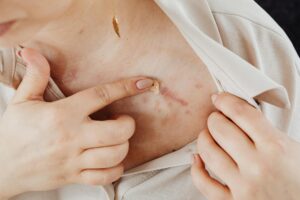
Hydroquinone works through a targeted mechanism that interrupts the melanin production process at multiple points. The cream blocks tyrosinase, the enzyme that converts L-DOPA into melanin, while simultaneously inhibiting melanosome dispersion—the process that moves melanin-containing particles throughout skin cells. This dual action prevents both the creation of new melanin and the distribution of existing melanin, which is why hydroquinone is more effective than products that only address one part of the process. When applied to a dark acne scar or post-inflammatory hyperpigmentation spot, hydroquinone gradually prevents the pigmented cells from producing and spreading melanin, allowing the skin’s natural cell turnover to bring lighter, non-pigmented skin to the surface.
The effectiveness of this mechanism is why dermatologists have recommended hydroquinone for dark spot treatment for decades. Unlike physical treatments that remove pigmented skin layers through peeling or lasers, hydroquinone works chemically from within, reducing melanin production at the source. For someone with a cluster of brown acne marks across their cheeks, consistent hydroquinone use addresses the underlying pigmentation problem rather than just temporarily masking it. However, the enzyme inhibition only works while you’re actively using the product—stopping treatment and exposing your skin to sun without protection can allow melanin production to resume and dark spots to return.

Clinical Effectiveness Timeline and What Research Shows
Clinical studies demonstrate significant results, though the timeline matters. A 2013 study found that 4% hydroquinone reduced melasma severity in 80% of patients within 12 weeks, and this same effectiveness applies to post-acne dark spots. More broadly, 70% of patients notice visible clearance or reduction in pigmentation with twice-daily 4% hydroquinone over a three-month period. However, the improvement isn’t immediate—most people begin seeing noticeable results at approximately four weeks of consistent use, with continued improvement extending to the three-month mark. Maximum effectiveness typically plateaus at six months, meaning if you’re going to see substantial improvement, it will happen within this window.
The timeline means patience is required. Someone starting hydroquinone treatment for acne dark spots shouldn’t expect visible fading within the first week or even the first two weeks. By week four, the dots may appear slightly lighter. By week 12, with consistent twice-daily application and sun protection, 70% of users see meaningful reduction. But here’s the important limitation: medical providers recommend a maximum of three months of continuous use due to the risk of exogenous ochronosis—a serious condition where prolonged hydroquinone use can paradoxically cause blue-black darkening of the skin, essentially worsening the problem you’re trying to solve. This three-month maximum means you need to use the treatment strategically and potentially cycle off to prevent this rare but permanent side effect.
Prescription Requirements and Available Concentrations
In the United States, hydroquinone is a prescription-only medication—it is not approved for over-the-counter use. The standard prescription concentrations available are 2%, 3%, and 4%, with 4% being the most commonly prescribed strength for dark spot treatment because it delivers the concentration used in clinical studies showing the 80% effectiveness rate. Prescription hydroquinone comes in various formulations including creams, gels, emulsions, lotions, and solutions, so your dermatologist can recommend the type that works best with your skin type. A 4% cream is typical for dry skin, while a gel or lotion might suit oily or combination skin types.
The prescription-only status is important because it reflects both the efficacy of the product and the need for medical oversight. Unlike many skincare products you can buy at a drugstore, hydroquinone requires a doctor’s assessment of your skin type, the extent of hyperpigmentation, and your risk factors for side effects. If you’re looking for over-the-counter alternatives, they don’t exist in most countries—you’ll need to consult a dermatologist to obtain a prescription. Some online prescription services like Nurx do offer hydroquinone through telemedicine consultations, but this still requires speaking with a medical provider. It’s also worth noting that hydroquinone is banned for cosmetic use in Japan, Australia, and the European Union, reflecting regulatory differences in how these regions approach skin-lightening treatments.

Maximum Duration and the Critical Three-Month Limit
The most important practical rule for hydroquinone use is the three-month maximum recommended by medical providers. This isn’t a suggestion—it’s a clinical safety boundary established because prolonged use increases the risk of exogenous ochronosis, a serious and potentially permanent side effect. Using 4% hydroquinone twice daily for three months is considered safe for most people and typically produces the 70-80% improvement rates shown in clinical data. Extending beyond three months continuously multiplies your risk of complications without providing additional benefits, since effectiveness plateaus at six months anyway.
Your dermatologist may recommend cycling off for a month or two, then resuming treatment if needed, rather than using it continuously longer than three months. For someone with extensive post-acne hyperpigmentation across multiple areas, this three-month window requires strategy. You might prioritize the most visible or bothersome spots during your first treatment cycle, see significant improvement by month three, then either stop and maintain results with sunscreen, or cycle off and treat other areas in a future cycle. The temporary nature of hydroquinone results—meaning that stopping treatment and sun exposure can lead to dark spots recurring—means you should plan to maintain results afterward with strict sun protection (SPF 30+) and possibly maintenance treatments separated by breaks. It’s not a one-time cure but rather a seasonal or cyclical treatment approach.
Side Effects and Risks to Monitor
While hydroquinone is generally well-tolerated, side effects are common enough that you should know what to watch for. The most frequent side effects include skin irritation, dryness, redness, and stinging, particularly in the first few weeks of use. These mild reactions often improve as your skin adjusts, though some people may need to reduce frequency to every other day. More serious but rare is exogenous ochronosis—the blue-black darkening mentioned earlier—which happens when hydroquinone is misused or used for too long, particularly in darker skin types. You might also experience contact dermatitis (allergic reaction) or post-inflammatory hyperpigmentation, where the treatment irritates the skin enough to trigger more pigmentation rather than less.
The exogenous ochronosis risk deserves emphasis because it’s the one side effect that can become permanent. If you follow the three-month maximum guideline and work with a dermatologist, your risk is low. But if someone tries to extend treatment beyond three months continuously, perhaps because they’re seeing good results and want to continue, they’re gambling with this risk. Additionally, hydroquinone works best on fair and medium skin tones. In darker skin types, there’s a higher risk that hydroquinone might not fade the dark spots as effectively, or in some cases, could worsen hyperpigmentation. This is why dermatological guidance is essential—a doctor can assess your specific skin type and determine whether hydroquinone is appropriate or whether alternative treatments like laser therapy or combination products would be safer and more effective.

Who Benefits Most and Skin Type Considerations
Hydroquinone is most effective for people with fair to medium skin tones experiencing post-inflammatory hyperpigmentation from acne. If you have acne-prone skin that tends to leave brown marks or dark spots after breakouts clear, you’re an ideal candidate. The treatment works well for people who can commit to consistent twice-daily application and strict sun protection, since sun exposure can undo progress and trigger recurrence. Someone with a few lingering dark spots from acne that cleared months ago may see dramatic improvement within three months of treatment.
However, if you have darker skin (particularly deeper skin tones), you should approach hydroquinone with caution and only under dermatological supervision. While some people with darker skin see benefit, others find that hydroquinone doesn’t reduce their hyperpigmentation as effectively, and there’s a higher risk of the treatment worsening pigmentation or causing other complications. Alternative treatments like combination formulas (hydroquinone plus other agents), laser treatments specifically designed for darker skin types, or other depigmenting agents may be more appropriate. Additionally, if you’re unwilling or unable to avoid sun exposure or can’t apply sunscreen daily, hydroquinone won’t maintain its effectiveness—the results are temporary without ongoing photoprotection.
Combining Hydroquinone with Other Acne Scar and Dark Spot Treatments
Hydroquinone often works best as part of a layered approach rather than as a standalone treatment. A dermatologist might prescribe hydroquinone 4% combined with tretinoin (a retinoid that increases cell turnover) and a mild corticosteroid, a combination that addresses pigmentation through multiple mechanisms simultaneously. Some prescription formulations already combine these ingredients. For more extensive acne scarring or very stubborn dark spots, hydroquinone might be combined with professional treatments like chemical peels, microdermabrasion, or laser therapy that physically remove pigmented skin layers while hydroquinone prevents new pigment from forming.
The combination approach often produces faster and more dramatic results than hydroquinone alone. Looking forward, newer depigmenting agents and combination therapies are being developed to address limitations of hydroquinone, particularly for darker skin types and for extending safe treatment duration. Current research continues to validate hydroquinone’s effectiveness when used appropriately, and most dermatologists still consider it a first-line treatment for acne-related dark spots. However, the field is evolving with alternative options becoming more available through prescription and medical aesthetics channels. If hydroquinone isn’t suitable for you or doesn’t produce results, your dermatologist can discuss alternatives like combination products, laser treatments, or other depigmenting agents that might address your specific dark spot concerns.
Conclusion
Hydroquinone compound creams fade acne dark spots by inhibiting tyrosinase and stopping melanin production at the cellular level, resulting in visible improvement for 70% of users within three months of twice-daily application. Clinical evidence consistently supports 4% hydroquinone as effective for post-inflammatory hyperpigmentation, with results typically becoming visible at four weeks and plateauing at six months. However, the three-month maximum use limit is critical—exceeding it risks serious side effects including permanent blue-black skin darkening, and the treatment is prescription-only in the United States because it requires medical oversight based on your skin type, extent of pigmentation, and individual risk factors.
If you’re dealing with acne-related dark spots, consulting a dermatologist is the best first step. They can assess whether hydroquinone is appropriate for your specific skin type and hyperpigmentation pattern, prescribe the correct concentration and formulation, explain the three-month usage limit and what to expect for timing, and recommend complementary treatments if needed. Combined with consistent sunscreen use and realistic expectations about the temporary nature of results, prescription hydroquinone remains one of the most clinically proven treatments for fading stubborn post-acne marks.
You Might Also Like
- Why Compound Pharmacies Offer Custom Acne Formulas
- What a Tretinoin and Niacinamide Compound Does for Acne
- Why Tretinoin Microsphere Is Better for Sensitive Acne Skin
Browse more: Acne | Acne Scars | Adults | Back | Blackheads