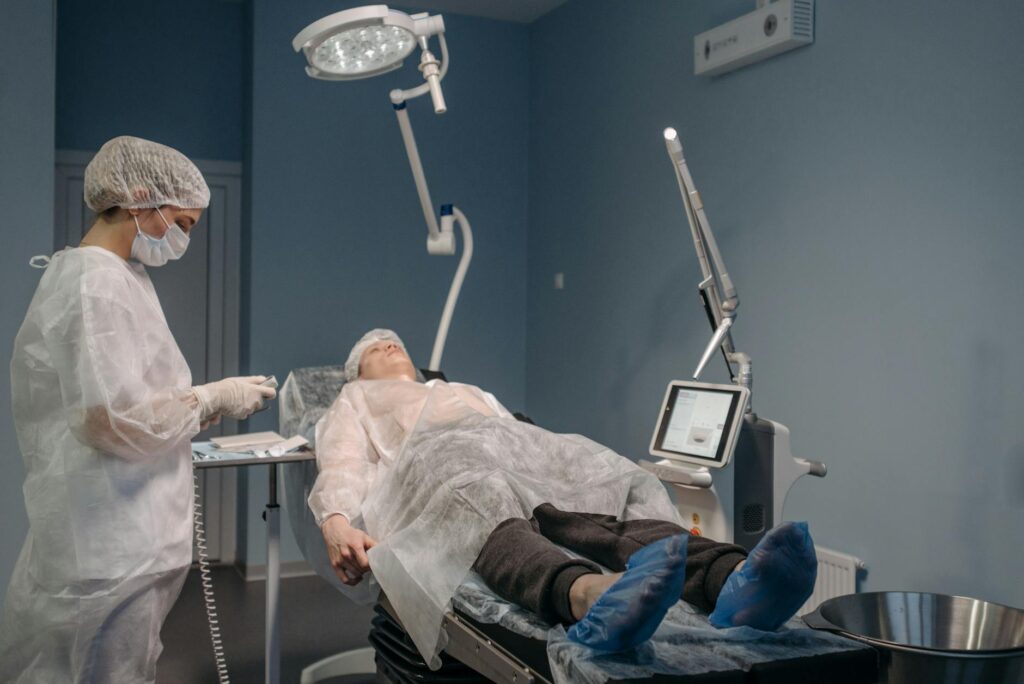
Herpes simplex prophylaxis before laser scar treatment is preventive antiviral therapy given to patients with a history of oral herpes (HSV-1) to prevent the virus from reactivating during and after laser skin resurfacing procedures. When you undergo laser treatment for acne scars—especially ablative laser treatments like CO2 lasers—the procedure creates controlled trauma to the skin that can trigger dormant herpes simplex virus to reactivate, even in patients who haven’t had an outbreak in years. Prophylaxis, meaning preventive treatment, uses oral antiviral medications started before the procedure to block this reactivation and protect your healing skin. This article covers what triggers HSV reactivation during laser treatment, which medications dermatologists use, proper timing and dosing protocols, effectiveness rates, and current medical guidelines for prophylaxis.
The importance of prophylaxis extends beyond preventing an annoying cold sore. If HSV does reactivate after laser scar treatment, it can cause delayed healing, infection, increased scarring, and potentially worse aesthetic outcomes than the original acne scars. For someone investing in laser treatment to improve their skin, an HSV flare-up during recovery can derail months of healing. That’s why dermatologists routinely recommend prophylaxis for anyone with a known history of herpes, and they often offer it as standard protocol before aggressive laser procedures regardless of outbreak history.
Table of Contents
- How Laser Treatments Trigger Herpes Simplex Reactivation in the Skin
- Why Prophylaxis Prevents HSV Reactivation While Healing
- FDA-Approved Antiviral Medications for HSV Prophylaxis
- Timing Your Prophylaxis Around Your Laser Procedure
- Effectiveness Rates and Why Prophylaxis Almost Always Works
- Who Needs Prophylaxis and Risk Stratification
- Current Medical Guidelines and the Standard of Care
- Conclusion
How Laser Treatments Trigger Herpes Simplex Reactivation in the Skin
CO2 laser resurfacing and other ablative laser procedures work by vaporizing damaged skin layers to stimulate collagen remodeling and scar revision. This controlled thermal injury is effective for treating acne scars, but it creates significant skin trauma that can activate latent HSV-1 virus hiding in nerve cells. The virus responds to the inflammatory cascade and tissue injury triggered by the laser, essentially “waking up” the dormant infection during the body’s healing phase. Research shows that HSV-1 reactivation following ablative laser procedures can lead to persistent infection, delayed wound healing, post-inflammatory hyperpigmentation, and severe scarring that can actually worsen the original scar you were trying to treat.
The risk is measurable and significant. In a 500-patient study of ablative laser procedures, postoperative HSV-1 infection occurred in 7.4% of patients—meaning roughly one in 14 people experienced reactivation. However, this statistic comes from patients who did not receive prophylaxis. Among patients who receive appropriate antiviral prophylaxis, reactivation rates drop dramatically to near zero, which is why prophylaxis has become standard preventive care rather than an optional add-on.
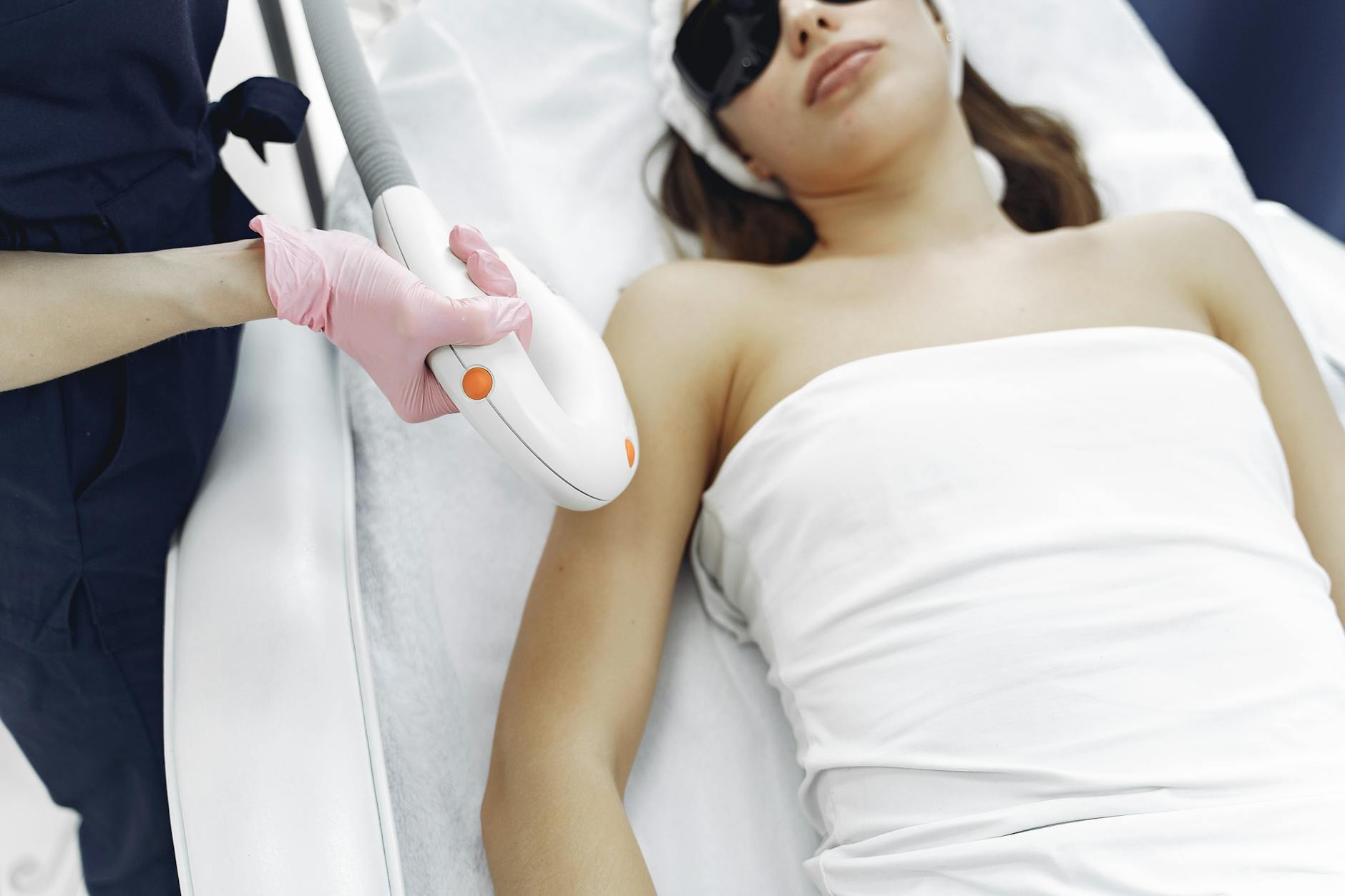
Why Prophylaxis Prevents HSV Reactivation While Healing
Antiviral medications work by inhibiting the enzymes that allow HSV to replicate within your cells. When you start prophylaxis before laser treatment, the medication circulates throughout your body and builds up in the treated skin tissue. During the high-risk healing period when the laser injury would normally trigger viral reactivation, the antiviral is already present to suppress any viral activity before it can cause an outbreak. Think of it like placing a guard at the door to prevent the virus from multiplying.
However, prophylaxis only works if it’s present in sufficient concentration before the trigger event (the laser procedure) occurs. Starting antivirals the morning of surgery might be too late, which is why guidelines recommend starting at least 12 to 24 hours before treatment. Additionally, prophylaxis continues throughout the critical healing window—typically 10 to 14 days after the procedure—because that’s when the immune system is most disrupted and the virus is most likely to reactivate. If you stop the medication too early or never start it before the procedure, the protective effect doesn’t exist.
FDA-Approved Antiviral Medications for HSV Prophylaxis
Three FDA-approved antiviral medications are standard options for HSV prophylaxis before laser procedures: valacyclovir, famciclovir, and acyclovir. Valacyclovir, taken at 500 mg twice daily for 10 to 14 days, achieved 100% effectiveness in preventing HSV reactivation with no adverse effects reported in clinical studies. This makes it one of the most reliable and commonly prescribed options. Famciclovir, dosed at 250 mg twice daily for 14 days, is also highly effective and has been specifically studied for preventing facial HSV reactivation after cosmetic procedures. Acyclovir, the older option, requires dosing of 400 mg every 8 hours (three times daily) for 14 days, and must be started at least 2 days before treatment—a more demanding schedule than the newer alternatives.
The choice between these medications often comes down to dosing frequency and cost. Valacyclovir and famciclovir require only twice-daily dosing, making them more convenient than acyclovir’s three-times-daily requirement. Valacyclovir also tends to be the most cost-effective, especially with generic availability. Acyclovir requires dosing to begin at least 2 days before treatment, while valacyclovir was shown to be 100% effective even when started the day before or the day of surgery, offering more scheduling flexibility. Your dermatologist will choose based on your medical history, kidney function, and any other medications you’re taking.
Timing Your Prophylaxis Around Your Laser Procedure
The timing of when you start prophylaxis is critical to its effectiveness. Medical guidelines recommend beginning antiviral therapy at least 12 to 24 hours before your laser procedure, with valacyclovir being effective even when started as late as the day of surgery. Most dermatologists recommend starting the day before to ensure stable drug levels in your system during the procedure. You then continue taking the medication for 10 to 14 days after treatment to cover the high-risk healing window when viral reactivation is most likely.
A typical prophylaxis schedule with valacyclovir might look like: start 500 mg twice daily on day minus-one (the day before your laser appointment), continue twice daily through day 14 post-procedure. For acyclovir, which requires more advance planning, you’d begin the dose (400 mg three times daily) at least 2 days before your appointment. The trade-off is that starting prophylaxis requires coordinating with your dermatology office in advance so you can fill the prescription and begin the medication at the right time. Missing the start window can reduce effectiveness, so this isn’t something to start casually the morning of your procedure. Discuss the exact timeline with your dermatologist when you book your laser treatment, so there’s no confusion about when to start and stop.
Effectiveness Rates and Why Prophylaxis Almost Always Works
When patients receive appropriate prophylaxis, HSV reactivation rates after laser procedures are near zero—compared to the 7.4% baseline risk in untreated patients. The 100% effectiveness rate for valacyclovir, documented in clinical studies, is exceptionally high for any preventive medication. This dramatic reduction in risk is why prophylaxis is considered a routine part of laser scar treatment for anyone with a history of herpes. The medications are not experimental or controversial; they’re standard evidence-based prevention.
However, effectiveness depends entirely on adherence. If you stop taking the medication early because your skin feels better, or if you miss doses because you’re busy, the virus can reactivate. Additionally, prophylaxis only prevents HSV reactivation triggered by the laser; if you develop a separate HSV outbreak from other triggers (stress, illness, sun exposure) during the healing window, the outcome can be complicated by the fact that your healing skin is still fragile. This is why dermatologists recommend avoiding other known HSV triggers during recovery, such as extreme stress or excessive sun exposure, even while taking prophylaxis.

Who Needs Prophylaxis and Risk Stratification
Not every patient requires prophylaxis, but identifying who does prevents unnecessary medication while protecting high-risk patients. If you have a documented history of oral herpes (cold sores or HSV-1 outbreaks, even if it’s been years), prophylaxis is indicated before ablative laser procedures. Even patients who haven’t had an outbreak in decades carry dormant virus in nerve cells and face reactivation risk during significant skin trauma.
Conversely, patients with no history of herpes simplex—whether they’ve never had an outbreak or they’re genuinely HSV-negative—don’t require prophylaxis because there’s no dormant virus to reactivate. Current guidelines recommend that prophylaxis be offered routinely for all CO2 laser resurfacing procedures, regardless of outbreak history, because the benefit-to-risk ratio is so favorable. The medications are well-tolerated, inexpensive, and the prevention is nearly 100% effective. Even if you’re unsure whether you’ve ever had herpes, erring on the side of prophylaxis is often the pragmatic choice, especially for expensive or extensive laser procedures where a complications like HSV reactivation would be costly and disappointing.
Current Medical Guidelines and the Standard of Care
Dermatologic societies now include anti-HSV prophylaxis as a standard recommendation for patients with prior herpetic outbreaks after aesthetic procedures, and many recommend it routinely for all CO2 laser resurfacing procedures as a matter of default protocol. This shift reflects the accumulated evidence showing that prophylaxis is safe, effective, inexpensive, and prevents a known complication. It’s moved from optional to standard-of-care in most practices.
If your dermatologist doesn’t mention prophylaxis before booking your laser treatment, you should ask whether they recommend it, especially if you have any history of cold sores or oral herpes. The evolving standard also reflects recognition that HSV reactivation during laser healing isn’t just a minor cosmetic inconvenience—it’s a medical complication that can delay healing by weeks and potentially worsen scarring outcomes. As laser treatments for acne scars become more common and as patients invest more significantly in their skin, preventing foreseeable complications through simple prophylaxis makes both clinical and patient-centered sense. Looking forward, prophylaxis will likely remain standard preventive care for all ablative laser procedures, with the focus shifting toward better patient education so people understand why they’re taking the medication and why adherence matters.
Conclusion
Herpes simplex prophylaxis before laser scar treatment is a proven, evidence-based preventive strategy that uses antiviral medications to prevent HSV-1 reactivation during and after ablative laser procedures. The need for prophylaxis is driven by a well-documented risk: laser-induced skin trauma can activate dormant herpes virus, leading to delayed healing, infection, and potentially worse scarring. Three FDA-approved antiviral medications—valacyclovir, famciclovir, and acyclovir—are safe, well-tolerated options, with valacyclovir being the most convenient and cost-effective for most patients.
If you’re planning laser scar treatment and have any history of oral herpes, discuss prophylaxis with your dermatologist well in advance so you can start the medication at the correct time and maintain it through the critical healing window. Even if you’re unsure about your herpes status, asking about prophylaxis is reasonable for significant laser procedures. The medication is inexpensive insurance against a complication that could undermine your entire laser investment.
You Might Also Like
- Why Aquaphor Is Recommended After Laser Scar Treatment
- What Hypopigmentation Risk from Laser Scar Treatment Looks Like
- What Combination Scar Treatment Protocols Look Like
Browse more: Acne | Acne Scars | Adults | Back | Blackheads