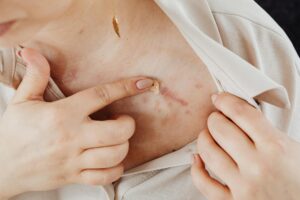
When you ignore post-acne redness, the inflammation doesn’t simply fade away on its own—it often deepens and becomes harder to treat. What starts as temporary pinkness after acne clears can persist for months or even become a chronic form of red scarring called post-inflammatory erythema (PIE) if left unaddressed. For example, someone who breaks out with moderate acne, skips sun protection and anti-inflammatory treatments during the healing phase, and continues irritating the skin with harsh products may find that their redness lingers for 12+ months instead of the typical 3-6 month healing window.
This article explains what actually happens to your skin when you ignore post-acne redness, how the inflammation progresses, what complications can develop, and why early intervention matters far more than most people realize. Post-acne redness is fundamentally different from active acne or scarring—it’s a vascular response where dilated blood vessels remain inflamed after the acne itself has healed. Ignoring it doesn’t mean it will turn into pimples again, but it does mean the underlying inflammation persists and can worsen through continued sun exposure, irritation, and lack of targeted care. Understanding this distinction is crucial because the treatment approach is entirely different from acne treatment.
Table of Contents
- How Does Untreated Post-Acne Redness Progress and Worsen?
- The Risk of Redness Becoming Permanent Post-Inflammatory Erythema
- How Continued Inflammation Increases Scarring Risk
- When Early Treatment Prevents Months of Visible Redness
- Why Some Post-Acne Redness Becomes Resistant to Treatment
- The Psychological and Social Impact of Prolonged Visible Redness
- Building a Prevention-First Approach to Post-Acne Redness
- Conclusion
How Does Untreated Post-Acne Redness Progress and Worsen?
Post-acne redness develops because acne causes inflammation that damages the small blood vessels and collagen in the skin. Once the acne lesion itself is gone, your body continues the healing process—but if you don’t support this healing with appropriate care, the inflammation lingers longer than necessary. UV exposure is one of the primary culprits that slows this process; sun damage increases inflammation and can actually deepen the redness by causing additional vascular dilation. Someone who ignores post-acne redness and spends time outdoors without SPF might see their redness remain visible or even intensify over weeks, whereas someone using sunscreen and gentle skincare will typically see faster fading.
The timeline matters significantly. During the first 2-4 weeks after acne clears, your skin is in active repair mode. If you continue using harsh actives, over-exfoliating, or picking at remaining texture during this phase, you’re essentially re-injuring the same area and restarting the inflammation cycle. This repeated irritation can extend the redness phase from the typical 3-6 months to 9-12 months or longer. Comparison: two people with identical acne breakouts—one who uses gentle cleansing and SPF during healing, one who doesn’t—often see different outcomes by month three, with the careful person showing significant fading while the other still has prominent redness.

The Risk of Redness Becoming Permanent Post-Inflammatory Erythema
When post-acne redness is ignored long enough, it can transition from temporary inflammation to a chronic condition called post-inflammatory erythema (PIE). PIE is red scarring caused by permanently dilated or damaged blood vessels that don’t return to their original diameter. The longer inflammation persists unmanaged, the higher the risk that these vascular changes become permanent. However, if you catch and treat post-acne redness during the acute phase (first 3-6 months), most cases will resolve even without intervention—but add poor lifestyle habits like sun exposure, smoking, or continued irritation, and you dramatically increase the likelihood of chronic PIE development.
One important limitation to understand: topical treatments alone are rarely effective for established PIE because the damage is vascular, not superficial. If you ignore redness long enough that it becomes PIE, topical creams won’t reverse it—you’d need professional treatments like laser therapy, intense pulsed light (IPL), or other vascular treatments. This is a critical distinction because many people assume that what works for preventing redness will also work for reversing chronic cases, which simply isn’t true. The difference between early intervention and late intervention isn’t just about comfort; it’s about whether the condition remains manageable with skincare or requires expensive professional procedures.
How Continued Inflammation Increases Scarring Risk
Prolonged post-acne redness doesn’t just stay as redness—it often accompanies and can worsen other forms of scarring. The ongoing inflammation extends the skin‘s repair timeline, which means your skin remains in a vulnerable state longer. During this extended healing phase, dehydration, continued irritation, or lack of proper support can shift the scarring pattern from mostly vascular (redness) to mixed vascular and atrophic scarring (depression or texture). Someone ignoring post-acne redness might find that six months later, not only is the redness still present, but they’ve also developed visible textural scarring that wasn’t apparent when they had active inflammation.
The relationship between redness and other scarring types is cumulative. Early inflammation management actually prevents other scarring types from forming, while neglect compounds the scarring problem. A specific example: hormonal acne that leaves redness on the jawline, when treated with sun protection and anti-inflammatory skincare, typically fades with only mild residual redness by month six. The same acne, ignored and exposed to sun repeatedly, often develops into both persistent redness and small atrophic scars that require different treatment approaches. The vascular inflammation, when chronic, seems to act as a scaffold that enables other scarring patterns to develop.
When Early Treatment Prevents Months of Visible Redness
The practical advantage of addressing post-acne redness early is substantial. Using anti-inflammatory ingredients like azelaic acid, niacinamide, or topical azithromycin during the acute phase can cut the redness duration from 6+ months to 2-4 months. Comparison: clinical studies show that sunscreen alone (SPF 30+) used consistently during post-acne healing reduces redness duration by approximately 30-40%, while combining sunscreen with targeted anti-inflammatory treatments reduces it by 50-70%. This isn’t just cosmetic convenience—every month of visible redness that you can prevent is one less month of potential sun-induced deepening or psychological impact.
The tradeoff of early intervention is minimal. Most anti-inflammatory post-acne treatments are inexpensive, well-tolerated, and don’t interfere with other skincare. The main limitation is that results take time—you won’t see dramatic improvement in week one. However, starting these treatments immediately after acne clears means you’re already several weeks ahead by month three, when the redness would have otherwise still been prominent. Delaying treatment to see if redness fades on its own is a gamble that often backfires; by the time you realize it’s not fading quickly enough, you’ve lost valuable early-intervention time and the inflammation has deepened.
Why Some Post-Acne Redness Becomes Resistant to Treatment
Not all post-acne redness responds equally to treatment, and ignoring it can transform responsive redness into resistant redness. Several factors determine whether redness will fade quickly or linger. Skin type plays a role—darker skin tones (Fitzpatrick types IV-VI) can develop longer-lasting post-inflammatory erythema due to deeper inflammation patterns, and delayed treatment in these cases has a more pronounced impact. Severity matters too; severe acne that penetrates deep into the dermis leaves more extensive vascular damage, so redness from severe acne is inherently more likely to linger even with good care, and becomes far more stubborn if ignored.
A critical warning: there’s a window of opportunity for redness management, and ignoring it closes that window. Redness that remains untreated for 12+ months transitions into a different category of concern—it’s no longer “post-acne redness” but rather chronic PIE or post-inflammatory erythema scarring. Once this transition happens, the condition requires much more aggressive treatment, and many topical options cease to be effective. This is why dermatologists emphasize early intervention; waiting to see if redness resolves on its own isn’t neutral—it’s an active choice that reduces your treatment options and increases the likelihood of long-term visibility.

The Psychological and Social Impact of Prolonged Visible Redness
Beyond the physical changes to your skin, ignoring post-acne redness often extends the psychological burden of having acne. Someone whose acne clears in two weeks but whose redness persists visibly for 8-12 months may experience frustration or social anxiety that extends far longer than the actual acne condition. This psychological impact is real and documented; people with post-acne redness report higher rates of frustration compared to those with similar acne severity but faster redness resolution. The difference often comes down to whether they received early post-acne care or were left to assume the redness would fade naturally.
A specific example: student breakouts before an important event. Acne that resolves two weeks before an event leaves them with prominent redness, but if they’ve used anti-inflammatory treatments and sunscreen during those two weeks, the redness is often 60-70% less visible. Without early intervention, the same person might still have very obvious redness at the event. This difference compounds when the redness lingers for months—what could have been a minor concern with early care becomes a months-long visibility issue with neglect.
Building a Prevention-First Approach to Post-Acne Redness
The long-term perspective on post-acne redness has shifted in recent years, with evidence increasingly pointing to prevention and early intervention as far superior to trying to treat chronic cases. Rather than waiting to see if redness fades, the current standard recommendation is to assume post-acne redness will require active support and to begin anti-inflammatory care immediately once acne clears. This proactive approach, applied consistently across your acne-prone years, prevents the accumulation of chronic PIE and keeps your skin recovery timeline shorter.
Looking forward, the recognition that post-acne redness is a distinct treatment category—separate from active acne and from post-acne scarring—means skincare and medical approaches are becoming more targeted. The days of assuming redness is just a normal part of acne recovery and will fade on its own are fading. Early, consistent care prevents months of visible redness and protects you from the risk of permanent vascular scarring. This shift from passive recovery to active management represents a significant improvement in post-acne outcomes for anyone willing to implement it during the critical first 3-6 months after acne clears.
Conclusion
Ignoring post-acne redness doesn’t mean it will disappear quickly or without consequences. Instead, untreated redness often persists for months longer than necessary, deepens through sun exposure and continued irritation, and carries a significant risk of transitioning into permanent post-inflammatory erythema (PIE) if neglected long enough. The inflammation that causes redness is actively managed by your skincare choices, sun protection habits, and whether you use targeted anti-inflammatory treatments during the critical healing phase.
The most important takeaway is that the post-acne period is not passive recovery time—it’s an active opportunity to shape your skin’s healing trajectory. Starting anti-inflammatory treatments immediately after acne clears, using consistent sunscreen, and avoiding irritants during the first 3-6 months can cut redness duration in half compared to neglect. By contrast, ignoring redness during this window often results in months of additional visibility and a higher risk of chronic scarring. The cost of early intervention is minimal, but the cost of delay—measured in months of visible redness and potential permanent damage—is substantial.
You Might Also Like
- Why Post Acne Redness Can Persist Even After Breakouts Heal
- How Blood Vessels Play a Role in Post Acne Redness
- Why Your Acne Leaves Marks Even When You Do Not Pick Your Skin
Browse more: Acne | Acne Scars | Adults | Back | Blackheads