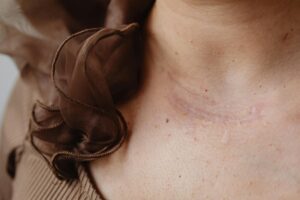
When inflammation occurs in your skin—whether from acne, eczema, an injury, or a dermatologic procedure—your body triggers a cascade of immune responses that ultimately stimulate your melanocytes to produce excess melanin. This overproduction of melanin is called post-inflammatory hyperpigmentation (PIH), and it’s one of the most common reasons people develop dark marks or patches on their skin long after the original inflammation has resolved. The mechanism is straightforward: inflammatory cytokines, prostaglandins, and reactive oxygen species released during the inflammatory response directly activate the enzymes responsible for melanin synthesis, causing melanocytes to go into overdrive.
This overproduced melanin then transfers to surrounding skin cells in the epidermis, and in some cases, leaks deeper into the dermis where it becomes harder to treat. This article explores what actually happens at the cellular level when inflammation triggers melanin production, why certain skin types are more susceptible to post-inflammatory hyperpigmentation, the difference between surface-level and deep hyperpigmentation, and what emerging research reveals about managing this common concern. Whether you’re dealing with acne-induced dark marks, eczema flares, or skin trauma, understanding the mechanism behind hyperpigmentation after inflammation is the first step toward prevention and treatment.
Table of Contents
- How Do Inflammatory Molecules Trigger Excess Melanin Production?
- What Molecular Mechanisms Drive Melanin Synthesis During Inflammation?
- Which Skin Types Are Most Vulnerable to Post-Inflammatory Hyperpigmentation?
- What’s the Difference Between Epidermal and Dermal Hyperpigmentation?
- How Do Macrophages and Oxidative Stress Perpetuate Hyperpigmentation?
- What Do Recent Studies Reveal About Synthetic Melanin and Wound Healing?
- Looking Forward: Managing Melanin Overproduction After Inflammation
- Conclusion
How Do Inflammatory Molecules Trigger Excess Melanin Production?
When your skin experiences inflammation, multiple signaling molecules flood the affected area. The primary culprits are inflammatory cytokines and mediators including IL-1, IL-6, TNF-α, IL-18, IL-33, GM-CSF, and prostaglandins E2 and D2. These molecules don’t randomly circulate—they directly bind to receptors on melanocytes and stimulate the production of tyrosinase, the master enzyme that catalyzes the entire melanin synthesis pathway. Think of tyrosinase as the factory supervisor: when inflammatory signals activate it, the melanin factory ramps up production significantly beyond normal baseline levels. IL-18 plays a particularly important role in this process.
This cytokine directly upregulates tyrosinase activity and simultaneously promotes the expression of tyrosinase-related proteins 1 and 2 (TYRP-1 and TYRP-2), which function as essential cofactors that accelerate melanin production. In essence, IL-18 doesn’t just turn up the volume on melanin production—it amplifies the entire manufacturing process. This is why IL-18 is considered one of the most potent inflammatory triggers for hyperpigmentation. The timeline matters here: melanin overproduction doesn’t happen immediately. It typically begins within days of the inflammatory insult and can peak weeks or even months later, which is why hyperpigmentation often appears as a delayed consequence. A person might notice their acne lesions have healed, but the dark marks persist or even darken further as the inflammatory response continues at the cellular level, driving continued melanin synthesis.

What Molecular Mechanisms Drive Melanin Synthesis During Inflammation?
The molecular machinery behind melanin overproduction involves two interconnected pathways: direct enzyme activation and oxidative stress amplification. During inflammation, reactive oxygen species (ROS)—unstable molecules released by immune cells and damaged tissue—accumulate in the affected area. These reactive oxygen species don’t just cause oxidative damage; they actively increase the expression of melanin-synthesizing enzymes, creating a feedback loop where inflammation → ROS production → increased enzyme expression → more melanin. This dual mechanism means that even after the initial inflammatory trigger resolves, the lingering oxidative stress can continue to drive hyperpigmentation.
However, it’s important to recognize that not all inflammation produces the same degree of hyperpigmentation. The intensity and duration of the inflammatory response, the type of inflammatory mediators present, and the individual’s baseline melanocyte reactivity all influence the final outcome. For example, a single bout of acne in someone with light skin might leave minimal discoloration, while the same lesion in someone with darker skin can result in significant pigmentation changes. This isn’t because darker skin is inherently more prone to inflammation—it’s because melanocytes in darker skin types are already producing more melanin at baseline and respond more dramatically to inflammatory signals.
Which Skin Types Are Most Vulnerable to Post-Inflammatory Hyperpigmentation?
Post-inflammatory hyperpigmentation is significantly more prevalent in individuals with Fitzpatrick skin types IV, V, and VI (darker skin tones). The epidemiological data is clear and consistent: while PIH can occur in any skin type, darker-skinned individuals experience it at higher rates and with greater severity. The reason is biological: melanocytes in Fitzpatrick IV-VI skin types produce more melanin under normal conditions and are inherently more reactive to inflammatory stimuli. When that inflammatory trigger arrives—acne, dermatitis, trauma, a laser procedure—these melanocytes respond with disproportionately higher melanin production. This difference has significant clinical implications.
A dermatologic procedure like a chemical peel or laser treatment that might leave barely perceptible marks in lighter skin can result in persistent hyperpigmentation in darker skin. This is why dermatologists often adjust treatment protocols based on skin type, using lower laser intensities, gentler chemical concentrations, or longer intervals between treatments for darker skin types. The goal is to achieve the desired therapeutic effect while minimizing the inflammatory response that could trigger excessive melanin production. The most common triggers for PIH across all skin types are acne vulgaris, atopic dermatitis, impetigo, physical trauma, and dermatologic procedures. Acne is by far the most prevalent cause, particularly in teenagers and young adults, making post-acne marks a widespread concern. Understanding your skin type and how your melanocytes typically respond to inflammation can help guide preventive strategies, from being more cautious with active treatments to choosing gentler skincare approaches during inflammatory conditions.

What’s the Difference Between Epidermal and Dermal Hyperpigmentation?
Not all hyperpigmentation is equal. The location of the excess melanin fundamentally changes both the appearance and the treatability of the marks. Epidermal post-inflammatory hyperpigmentation occurs when excess melanin remains in the epidermis, the outermost layer of skin. Under the microscope, you see increased melanin within keratinocytes and sometimes within melanocytes themselves. Clinically, epidermal PIH appears as a brown discoloration and has a better prognosis—these marks typically fade gradually over months to a few years as the skin naturally sheds the pigmented cells. Dermal hyperpigmentation, by contrast, occurs when melanin leaks deeper into the dermis where it’s engulfed by macrophages.
Once melanin is phagocytosed by dermal macrophages, the timeline for resolution extends dramatically. Clinically, dermal PIH appears blue-gray or slate-colored rather than brown, and it persists much longer because macrophages don’t naturally exfoliate like epidermal cells do. In some cases, dermal PIH can take years to resolve or may become permanent. This distinction is critical when choosing treatments: topical depigmenting agents work reasonably well on epidermal PIH but have minimal impact on dermal hyperpigmentation, which often requires procedural approaches or patience for natural resolution. The depth of pigmentation can often be predicted by the original inflammatory trigger. Superficial inflammation (like mild acne or surface irritation) typically results in epidermal PIH, while deeper inflammation or trauma tends to produce the more problematic dermal form. Similarly, certain skin types are more prone to dermal involvement; darker skin types show higher rates of dermal PIH, which contributes to the greater clinical challenge of managing post-inflammatory marks in these populations.
How Do Macrophages and Oxidative Stress Perpetuate Hyperpigmentation?
Emerging research has revealed a nuanced understanding of how the skin healing phase contributes to melanin production. During skin healing, macrophages undergo a phenotypic shift from an M1 (pro-inflammatory) state to an M2 (anti-inflammatory, tissue-remodeling) state. Counterintuitively, while M2 macrophages are typically associated with tissue repair and reduced inflammation, they’re also potent stimulators of melanin synthesis. When melanocytes interact with M2 macrophages, melanin production increases significantly, driven by vascular endothelial growth factor (VEGF) signaling. This means that even as inflammation subsides and healing progresses, the reparative phase itself continues to stimulate melanin production. Oxidative stress compounds this problem. Reactive oxygen species generated during the inflammatory phase don’t disappear once the acute inflammation resolves.
These molecules persist and continue to upregulate melanin-synthesizing enzymes. The combination of M2 macrophage signals plus ongoing oxidative stress creates an extended window during which melanin production remains elevated. This explains why hyperpigmentation often continues to darken or develop weeks after the original inflammation has clinically resolved. The skin appears to be healing, but at the cellular level, melanocyte stimulation continues. This mechanism also explains why antioxidant treatments can be helpful in managing PIH. By reducing oxidative stress through vitamin C, ferulic acid, or other antioxidants, you’re theoretically dampening one of the drivers of continued melanin synthesis during the healing phase. However, once melanin has been produced and transferred to keratinocytes or engulfed by dermal macrophages, antioxidants cannot reverse the pigmentation—they can only potentially slow further melanin production.

What Do Recent Studies Reveal About Synthetic Melanin and Wound Healing?
A landmark 2023 study published in Nature Regenerative Medicine investigated synthetic melanin nanoparticles as a therapeutic approach to expedite skin healing and potentially modulate inflammation-related pigmentation. The findings were striking: topical synthetic melanin particles reduced skin edema (swelling), decreased eschar detachment time (the time it takes for dead tissue to shed), and increased overall wound healing rate in both animal models and human skin explants. More importantly, these synthetic melanin particles suppressed pro-inflammatory gene activity, essentially dampening the inflammatory environment that drives endogenous melanin overproduction. The mechanism appears to involve synthetic melanin’s ability to scavenge reactive oxygen species and dampen immune activation.
Rather than trying to block melanin synthesis directly—which is difficult given the multiple inflammatory mediators involved—this approach uses synthetic melanin’s biophysical properties to reduce the oxidative stress and inflammatory signals that drive both excessive melanin production and tissue damage. While this research is preliminary and not yet available as a consumer product, it demonstrates a novel therapeutic direction: using melanin itself as a therapeutic agent to accelerate healing and reduce the inflammatory cascade that leads to hyperpigmentation. The implications are significant. If synthetic melanin can suppress pro-inflammatory gene activity while accelerating healing, it might eventually offer a way to minimize hyperpigmentation risk in people undergoing inflammatory skin conditions or procedures. For now, this remains a research avenue, but it underscores an important principle: understanding the biology of melanin production during inflammation opens doors to unconventional treatments that work with the body’s natural processes rather than simply trying to suppress them.
Looking Forward: Managing Melanin Overproduction After Inflammation
Current management strategies for post-inflammatory hyperpigmentation focus on three approaches: prevention during the inflammatory phase, topical depigmentation after PIH develops, and procedural treatments for persistent marks. Prevention is most effective because it addresses the root cause—the inflammatory stimulus itself. In acne management, using non-irritating products, appropriate acne treatments that minimize inflammation, and sun protection all reduce the risk of PIH development. For other inflammatory conditions like eczema, strict emolliation and anti-inflammatory treatments similarly minimize hyperpigmentation risk. As research continues, the understanding of melanin’s role in the inflammatory and healing process is evolving.
Rather than viewing melanin purely as a cosmetic problem, emerging evidence suggests that controlled melanin production may actually participate in tissue repair. This shifts the perspective: instead of aggressively blocking all melanin synthesis, the goal becomes optimizing the inflammatory response to minimize excessive melanin production while preserving the beneficial aspects of the healing process. Future treatments will likely target specific inflammatory mediators (like IL-18) or macrophage signaling rather than attempting to shut down the entire melanin synthesis pathway. The trajectory of research suggests that personalized approaches based on skin type, the nature of the inflammatory trigger, and individual melanocyte reactivity will become standard. What works to prevent or treat PIH in someone with Fitzpatrick type II skin may be inadequate for someone with type VI skin. As our understanding of the molecular mechanisms deepens, so too will our ability to intervene more precisely, potentially offering better outcomes for the millions of people who develop hyperpigmentation as a consequence of inflammation.
Conclusion
When melanin production increases after inflammation, it’s not a random or unavoidable consequence—it’s the result of specific molecular signals triggered by inflammatory cytokines, prostaglandins, and oxidative stress acting directly on melanocytes. IL-18, IL-1, IL-6, TNF-α, and other inflammatory mediators activate tyrosinase and related enzymes, driving melanin synthesis precisely when your skin doesn’t need excess pigmentation. The severity and persistence of post-inflammatory hyperpigmentation depends on where the melanin deposits (epidermal marks fade faster than dermal), which skin type you have (darker skin types are more susceptible), and how intensely the inflammatory response occurred.
The most practical takeaway is that prevention during the inflammatory phase is infinitely easier than treating established hyperpigmentation. Managing acne gently, protecting skin from trauma, being cautious with aggressive procedures, and using sun protection all reduce your risk. If hyperpigmentation does develop, understanding whether it’s epidermal or dermal helps set realistic expectations for treatment timelines. And as research continues to reveal new mechanisms—from the role of M2 macrophages to the potential of synthetic melanin—more targeted interventions may eventually offer faster resolution of these stubborn post-inflammatory marks.
You Might Also Like
- How Inflammation Impacts Skin Even After Acne Clears
- What Happens When You Change Products Too Frequently
- Why Using Too Many Products Can Worsen Acne
Browse more: Acne | Acne Scars | Adults | Back | Blackheads