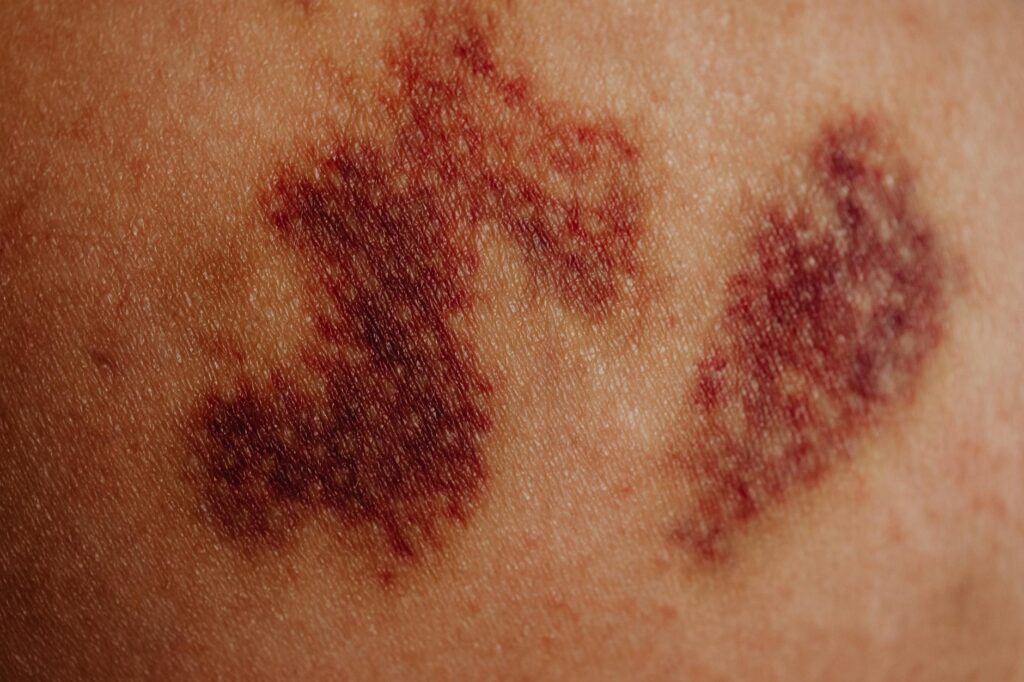
When acne inflames your skin, blood vessels in the affected area dilate and become engorged with blood, which is why the spot appears red. This isn’t a cosmetic accident—it’s your immune system responding to the bacterial infection and inflammation underneath the surface. The redness you see is literally increased blood flow to the acne site, as your body attempts to fight the infection and initiate healing. This vascular response is why some acne lesions can remain red for weeks even after the bacteria is cleared and the bump flattens out.
The biological cascade that causes this redness begins with a bacteria called *Cutibacterium acnes* (formerly *Propionibacterium acnes*), which triggers an inflammatory response in your skin. Your immune cells release chemical messengers called cytokines that signal blood vessels to expand and become more permeable. More blood in the surface layers of skin creates the characteristic red or pink appearance, while deeper inflammation can produce darker or purple-toned lesions. This article explains exactly what happens to your blood vessels during acne, why the redness persists, and what you can actually do to reduce it.
Table of Contents
- How Do Blood Vessels Respond to Acne Inflammation?
- Why Does Redness from Acne Last So Long?
- Post-Inflammatory Erythema: When Redness Lingers
- How to Reduce Redness from Active Acne
- The Role of Skin Barrier and Redness
- When Blood Vessel Changes Become Permanent
- The Future of Treating Vascular Responses in Acne
- Conclusion
How Do Blood Vessels Respond to Acne Inflammation?
Your skin contains an extensive network of tiny blood vessels (capillaries) that normally regulate temperature and deliver oxygen and nutrients to your skin cells. When acne bacteria colonize a pore and trigger inflammation, your immune system releases chemical signals that cause the smooth muscle cells surrounding these blood vessels to relax. This relaxation, called vasodilation, allows the vessels to widen significantly. A pore that would normally have minimal blood flow suddenly becomes engorged, which is why you can develop redness almost overnight on a blemish that was a closed comedone just hours before.
The increased permeability of these dilated vessels is equally important. The walls of inflamed capillaries become “leakier,” allowing more fluid and immune cells to seep into the surrounding tissue. This is why acne lesions often swell—that fluid accumulation combined with oil and dead skin cells creates pressure and visible inflammation. If you’ve ever noticed how a pimple can get redder and more swollen over a 24-hour period, this vessel response is accelerating during that time. The blood vessels aren’t being damaged; they’re functioning exactly as designed, but the intensity of the inflammatory signal is causing an exaggerated vascular response.

Why Does Redness from Acne Last So Long?
This is where the timeline of acne gets frustrating. The bacterial infection inside the lesion might be eliminated within days of treatment—or even by your skin’s own immune response—but the redness can persist for weeks. This happens because the blood vessels that dilated to fight the infection don’t immediately return to their normal diameter. Even after the inflammation subsides and the lesion flattens, the capillaries remain somewhat engorged and the surrounding tissue can retain inflammatory compounds that keep signaling these vessels to stay dilated.
The depth of the acne matters significantly here. Superficial whiteheads, which are close to the surface, may produce redness that fades within days once treated. However, deeper nodular or cystic acne can damage blood vessel walls and surrounding tissue, leading to persistent redness or even permanent scarring. Additionally, if you pick at or over-treat an acne lesion, you can create micro-tears in these fragile dilated vessels, which triggers additional inflammation and prolongs the redness. This is why dermatologists emphasize leaving acne alone—continuing to provoke the lesion keeps the inflammatory cycle running and the blood vessels dilated.
Post-Inflammatory Erythema: When Redness Lingers
After acne heals, some people develop post-inflammatory erythema (PIE), which is persistent redness without any visible bump or texture. This occurs when the blood vessels in the healed area remain dilated beyond what’s needed for healing. The overlying skin may look completely clear to the touch, but the redness suggests active or semi-active inflammation beneath the surface. PIE can last for months and is more common in people with fair or sensitive skin, though it affects all skin tones.
The mechanism behind PIE involves both persistent vasodilation and sometimes actual structural changes to the capillary network. If acne was severe or cystic, the inflammatory process may have caused permanent alterations to how blood vessels are arranged in that area. Fortunately, PIE is not the same as post-inflammatory hyperpigmentation (PIH), which is a darkening of the skin from melanin deposition rather than blood vessel changes. PIE typically responds well to time and certain treatments like laser therapy or topical niacinamide, whereas PIH requires different approaches.
How to Reduce Redness from Active Acne
The most effective approach is to minimize inflammation before and during the acne outbreak. This means using ingredients that reduce bacterial growth and calm the immune response. Niacinamide, found in many serums and moisturizers, actually helps regulate sebum production and has been shown to reduce the inflammatory markers that trigger excessive vasodilation. Salicylic acid and benzoyl peroxide work primarily by reducing the bacterial load, which decreases the inflammatory signal that tells blood vessels to dilate in the first place.
For lesions that are actively red and inflamed, topical retinoids can accelerate skin cell turnover and reduce the inflammatory response, though they typically take 2-3 weeks of consistent use to show meaningful improvement. Azelaic acid is particularly useful because it reduces both the bacterial triggers and the inflammatory cytokines directly. A practical tradeoff: stronger treatments like adapalene work faster than weaker retinoids, but they also cause more drying and irritation initially, which can ironically trigger additional inflammation in sensitive individuals. Starting with lower concentration and building tolerance is often more effective than jumping to the strongest option available.
The Role of Skin Barrier and Redness
An intact skin barrier actually helps minimize acne redness because it prevents additional irritation from triggering more inflammation. When your skin barrier is compromised—through over-washing, excessive exfoliation, or use of multiple acne treatments simultaneously—your immune system becomes hyperactive and blood vessels respond more dramatically to any perceived threat. Someone using benzoyl peroxide, vitamin C serum, and a retinoid all at once, for example, will likely experience intense redness and irritation, even though individually these are all valid acne treatments.
Be cautious with products labeled “antibacterial” or containing essential oils, as these can actually provoke inflammation in sensitive skin rather than calm it. If you notice that your acne-prone areas are becoming progressively redder despite treatment, pause and assess whether you’re overwhelming your barrier rather than whether the active ingredients aren’t working. Many people mistakenly think they need stronger treatments when what they actually need is fewer treatments with better spacing. Your blood vessels will naturally calm down once the inflammatory load decreases, which sometimes happens faster with a simpler routine than an aggressive one.

When Blood Vessel Changes Become Permanent
In severe, repeated acne, or in acne that’s been picked and manipulated, blood vessels can actually become permanently dilated or fragile. This is one reason why consistent acne treatment is preferable to letting breakouts run their course and heal on their own—repeated inflammatory cycles cause cumulative damage. Some people develop a pattern of broken capillaries or persistent vascular flushing in acne-prone areas, especially on the face and chest, which represents lasting structural changes to the vasculature.
Rosacea and acne-rosacea can develop partly from this kind of repeated vascular inflammation, creating a situation where blood vessels remain chronically dilated even after acne is controlled. If you’ve had severe acne over many years, you might notice that certain areas remain permanently slightly redder or have visible capillaries, even when clear. This is not reversible, but it’s preventable through earlier intervention and proper treatment of active acne.
The Future of Treating Vascular Responses in Acne
Newer acne treatments are beginning to target not just the bacteria or the oil production, but the inflammatory signaling pathways themselves. Some emerging research focuses on inhibiting specific cytokines that tell blood vessels to dilate, rather than just killing bacteria.
This could theoretically reduce the redness during acne without the side effects associated with traditional treatments. Laser and light-based therapies are also evolving to specifically target dilated blood vessels in post-acne redness, with improvements in precision and reduced downtime. As our understanding of the vascular component of acne improves, treatment strategies are likely to shift toward combination approaches that address both the infection and the excessive vascular response simultaneously, potentially shortening the time acne remains visible even after it’s effectively treated.
Conclusion
Acne redness is fundamentally a vascular problem caused by inflammation triggering your blood vessels to dilate and become engorged with blood. Understanding this mechanism explains why redness can persist long after the infection is cleared and why aggressive picking or constant irritation worsens the problem—you’re repeatedly triggering the vascular response. The most effective approach is to treat acne early and consistently to minimize the inflammatory signal, rather than waiting for severe lesions to appear and expecting them to fade quickly.
The takeaway for managing acne redness is prevention and patience. Use targeted ingredients like benzoyl peroxide, niacinamide, or azelaic acid to reduce inflammation, maintain a healthy skin barrier to prevent unnecessary additional inflammation, and avoid picking or over-treating lesions. If you’re dealing with stubborn post-inflammatory erythema, recognize that your skin needs time for the vasculature to normalize, and consider professional treatments like laser therapy if the redness persists beyond several months. Most importantly, consistent daily acne management today prevents the permanent vascular damage that makes redness harder to treat later.
You Might Also Like
- What Causes Redness to Linger After Acne Heals
- What Causes Sudden Acne Flare Ups Without Clear Reason
- What Causes Acne to Return After It Almost Clears Completely
Browse more: Acne | Acne Scars | Adults | Back | Blackheads