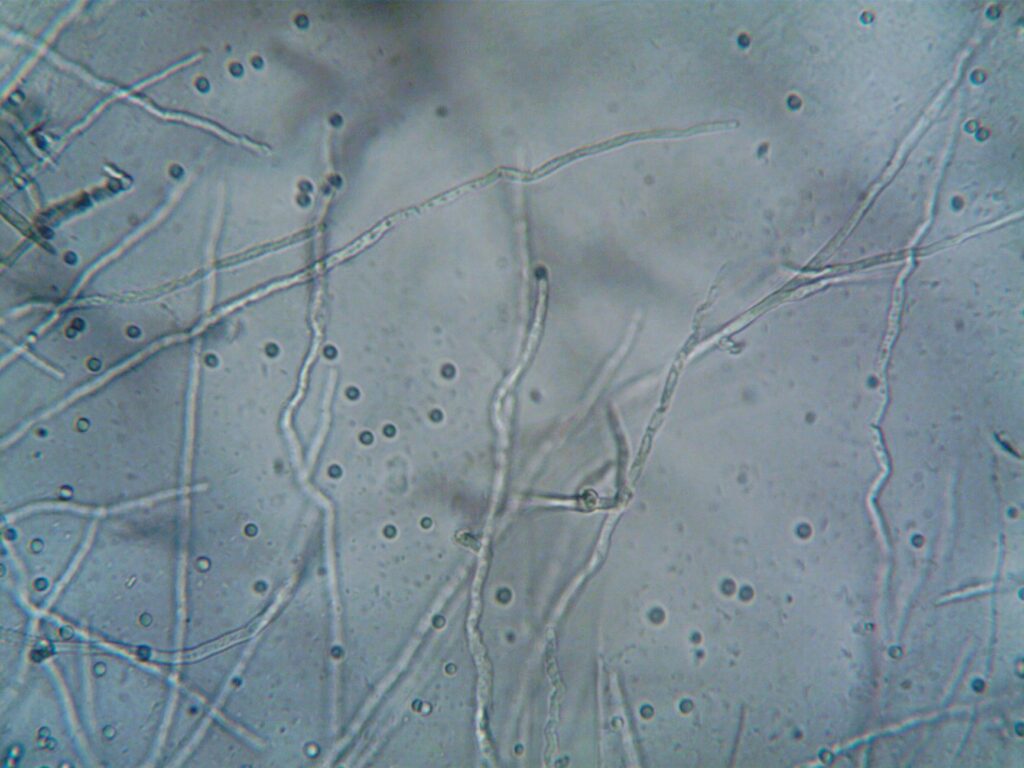
If you have fungal acne, the foods you need to cut back on are those that feed yeast internally or spike your blood sugar hard enough to increase sebum production and shift your skin’s microbial balance. That means simple sugars, refined carbohydrates, alcohol, dairy (especially whey-heavy products), and foods high in yeast or mold like aged cheeses, fermented alcohol, and certain dried fruits. Someone who switches from a breakfast of sugary cereal and orange juice to eggs and vegetables, for example, often notices their Malassezia-driven breakouts calm down within a few weeks — not because diet is a cure, but because it removes one layer of fuel from the problem. Fungal acne, technically called Malassezia folliculitis or pityrosporum folliculitis, looks like clusters of small, uniform, itchy bumps — usually on the chest, back, shoulders, and forehead. Unlike bacterial acne, it is caused by an overgrowth of Malassezia yeast, a fungus that naturally lives on everyone’s skin.
While topical antifungals are the frontline treatment, diet plays a legitimate supporting role. This article breaks down the specific food categories to avoid, explains why they matter, covers what you should eat instead, and addresses some common misconceptions about dietary approaches to fungal acne. Dietary changes alone will not resolve a full-blown case of fungal acne. But if you are already using antifungal treatments and still dealing with recurring flares, what you eat could be the overlooked factor keeping your skin from clearing. The following sections get specific about which foods matter most and which dietary advice floating around online is overblown.
Table of Contents
- Why Do Certain Foods Make Fungal Acne Worse?
- Sugars and Refined Carbohydrates That Feed Yeast Overgrowth
- The Dairy and Fungal Acne Connection
- Building an Anti-Fungal Diet That Actually Works
- Hidden Yeast and Mold Sources Most People Miss
- How Alcohol Specifically Impacts Fungal Acne
- The Emerging Role of Gut Health in Skin Fungal Conditions
- Conclusion
- Frequently Asked Questions
Why Do Certain Foods Make Fungal Acne Worse?
Malassezia yeast feeds primarily on lipids — specifically medium and long-chain fatty acids found in sebum. When your body produces more sebum, or when your internal environment becomes more hospitable to yeast overgrowth, fungal acne flares. Foods that spike blood sugar trigger a cascade: insulin rises, which increases insulin-like growth factor 1 (IGF-1), which in turn ramps up sebum production in your sebaceous glands. A 2012 study in the Journal of the Academy of Nutrition and Dietetics confirmed that high-glycemic diets were associated with increased sebum output and acne severity. While that study focused on conventional acne, the sebum mechanism applies equally to Malassezia overgrowth since the yeast depends on that same sebum for survival. There is also the gut-skin axis to consider.
Your gut microbiome influences systemic inflammation, immune regulation, and even the composition of your skin’s microbial community. Diets high in sugar and refined carbs tend to promote intestinal candida overgrowth and gut dysbiosis, which can weaken immune surveillance against fungal organisms elsewhere in the body, including on the skin. Compare two people with the same Malassezia colonization levels: the one with a balanced gut microbiome and lower systemic inflammation will typically keep the yeast in check, while the one eating processed food and sugar daily gives the yeast more room to proliferate. It is worth noting that the connection between diet and fungal acne is less studied than the connection between diet and bacterial acne. Most of the dietary recommendations are extrapolated from research on glycemic load, sebum production, candida overgrowth, and general dermatological principles rather than direct clinical trials on Malassezia folliculitis specifically. That does not make the recommendations baseless — it means you should approach dietary changes as one tool in a broader treatment plan, not a standalone fix.

Sugars and Refined Carbohydrates That Feed Yeast Overgrowth
Simple sugars are the most direct dietary contributor to yeast-friendly conditions. Table sugar, high-fructose corn syrup, candy, soda, pastries, white bread, white rice, and most breakfast cereals all cause rapid blood sugar spikes. These spikes drive insulin and IGF-1 production, which increases the oiliness of your skin. But beyond sebum, sugar also directly feeds yeast organisms in your gut. Candida albicans, a related fungal species, thrives on glucose and fructose, and an overgrowth in the gut can create systemic conditions that make Malassezia harder to control on the skin. A practical example: someone who drinks two cans of soda and eats a muffin for lunch is consuming roughly 80 to 100 grams of sugar in one sitting.
That amount can cause a blood sugar spike that takes hours to normalize, during which time sebaceous glands are actively being stimulated. Swapping that lunch for grilled chicken, a salad with olive oil, and water removes the sugar spike entirely. This does not mean you can never eat sugar again — the issue is chronic, daily overconsumption, not an occasional dessert. However, if you have insulin resistance, prediabetes, or polycystic ovary syndrome (PCOS), even moderate amounts of refined carbohydrates may affect you more severely than someone with normal insulin sensitivity. People in these categories often find that fungal acne is particularly stubborn until they address their glycemic control more aggressively. In these cases, working with a doctor or dietitian to manage blood sugar is not just a skin strategy — it is a metabolic health priority that happens to benefit the skin as well.
The Dairy and Fungal Acne Connection
Dairy is a well-established acne trigger, but its role in fungal acne specifically is more nuanced. The primary concern is whey protein, which is found in milk, yogurt, cheese, and whey protein supplements. Whey raises IGF-1 levels more than almost any other food component, and multiple studies have linked high dairy intake to increased acne severity. A 2018 meta-analysis in Nutrients found a positive association between dairy consumption (especially skim milk) and acne, likely driven by the hormonal content and IGF-1 response. For fungal acne sufferers, the mechanism is the same sebum-driven pathway. More IGF-1 means more sebum, which means more food for Malassezia. Whey protein shakes are a common culprit — gym-goers who start supplementing with whey often notice new breakouts within weeks.
Switching to a plant-based protein powder (pea protein, rice protein, hemp protein) frequently resolves this. One dermatologist on a medical forum described a patient whose persistent forehead bumps cleared within a month of stopping whey protein, despite no changes to their topical routine. That said, not all dairy is equally problematic. Fermented dairy like kefir and certain yogurts contain probiotics that may actually support gut health and immune function. The tradeoff is real: if you tolerate fermented dairy and your skin does not react to it, eliminating it entirely may not be necessary. The best approach is an elimination trial — cut all dairy for four to six weeks, then reintroduce specific types one at a time to see what your skin can handle. Butter and ghee, which are almost entirely fat with minimal whey or lactose, are generally better tolerated.

Building an Anti-Fungal Diet That Actually Works
Rather than just listing foods to avoid, it helps to know what to replace them with. A diet that discourages Malassezia overgrowth focuses on low-glycemic whole foods, lean proteins, healthy fats, and plenty of vegetables. Non-starchy vegetables like broccoli, spinach, kale, zucchini, and bell peppers form the foundation. Protein sources like chicken, turkey, fish, eggs, and legumes keep you full without spiking blood sugar. Healthy fats from olive oil, avocado, nuts, and seeds provide energy and support skin barrier function. The comparison worth making is between a generic “clean eating” approach and a targeted anti-fungal diet. Standard clean eating might include lots of fruit, honey as a sweetener, whole wheat bread, and fermented foods like kombucha.
An anti-fungal approach is more restrictive: fruit intake is limited to lower-sugar options like berries and green apples, honey is treated the same as sugar, bread is minimized even if whole grain, and fermented foods are evaluated individually. Kombucha, for instance, contains both sugar and yeast, making it a poor choice during an active fungal acne flare. The tradeoff with strict anti-fungal diets is sustainability. Going too restrictive often leads to diet fatigue and eventual bingeing, which can cause worse flares than a moderately imperfect diet maintained consistently. A reasonable middle ground is to eliminate the worst offenders — soda, candy, white bread, whey protein, and heavy alcohol — while allowing moderate portions of whole grains, whole fruits, and small amounts of dairy if tolerated. Perfection is not the goal. Reducing the overall glycemic and yeast-promoting load of your diet is.
Hidden Yeast and Mold Sources Most People Miss
Beyond the obvious sugar and dairy culprits, several foods contain yeast or mold that can exacerbate fungal conditions. Aged cheeses like blue cheese, brie, and camembert are produced using specific mold cultures. Dried fruits often harbor mold, especially if stored improperly. Peanuts and pistachios are particularly susceptible to aflatoxin-producing molds. Beer and wine contain both alcohol (which raises blood sugar and suppresses immune function) and residual yeast from fermentation. Vinegar, except for apple cider vinegar with the mother, is another fermentation product that some fungal acne sufferers find problematic. The warning here is about going overboard.
Some online anti-candida diets eliminate mushrooms, all vinegar, soy sauce, and every fermented food, creating a diet so restrictive it becomes nutritionally inadequate and psychologically unsustainable. The evidence that eating a mushroom on your salad will worsen Malassezia on your skin is essentially nonexistent. Mushrooms are not the same species as Malassezia, and digesting a fungal food does not meaningfully increase fungal colonization on your skin. Focus on the foods with strong mechanistic evidence — sugar, refined carbs, alcohol, and high-glycemic foods — rather than eliminating every food tangentially related to fungus. A more productive use of your attention is reading ingredient labels for hidden sugars. Salad dressings, pasta sauces, granola bars, flavored oatmeal, and “healthy” smoothies from chain restaurants often contain 15 to 30 grams of added sugar per serving. These hidden sources can undermine an otherwise solid diet without you realizing it.

How Alcohol Specifically Impacts Fungal Acne
Alcohol is a triple threat for fungal acne. First, it is metabolized into sugar, spiking blood glucose and insulin. Second, it directly suppresses immune function, reducing your body’s ability to keep Malassezia in check. Third, it disrupts the gut microbiome, promoting the kind of dysbiosis that allows fungal organisms to flourish systemically.
A night of heavy drinking can cause a visible flare within 24 to 48 hours in susceptible individuals — the itchy bumps seem to appear almost on schedule. If you choose to drink, clear spirits like vodka or gin mixed with soda water are the least problematic options, since they contain no residual sugar or yeast. Beer is the worst choice, combining high carbohydrate content with active yeast. Sweet cocktails, margaritas, and dessert wines fall somewhere in between. Reducing alcohol to one or two drinks per week, rather than eliminating it entirely, is a realistic harm-reduction strategy for most people.
The Emerging Role of Gut Health in Skin Fungal Conditions
Research on the gut-skin axis is accelerating, and the next few years will likely bring more targeted dietary guidance for conditions like fungal acne. Preliminary studies suggest that specific probiotic strains — particularly Lactobacillus rhamnosus and Saccharomyces boulardii — may help regulate the immune response to fungal overgrowth. S.
boulardii is especially interesting because it is a beneficial yeast that competes with pathogenic fungi in the gut, potentially reducing the systemic fungal burden that contributes to skin colonization. As microbiome testing becomes more accessible and affordable, personalized dietary recommendations based on an individual’s gut composition may replace the broad elimination diets currently used. Until then, the practical approach remains the same: reduce sugar and refined carbs, limit alcohol, manage dairy intake, support your gut with prebiotic fiber from vegetables, and treat diet as one component of a broader strategy that includes proper topical antifungal treatment and skincare routine adjustments.
Conclusion
Managing fungal acne through diet comes down to a few core principles: minimize foods that spike blood sugar and increase sebum production, reduce alcohol consumption, be strategic about dairy, and watch for hidden sugars in processed foods. The foods with the strongest evidence against them are simple sugars, refined carbohydrates, whey protein, beer, and excessively processed snack foods. You do not need to follow a militant anti-candida diet that eliminates mushrooms and every trace of fermentation — that level of restriction is unsupported by evidence and difficult to maintain. Start with the highest-impact changes first.
Cut out sugary drinks and obvious junk food, switch from whey to plant-based protein if you supplement, and reduce alcohol to occasional use. Give these changes four to six weeks alongside your topical antifungal treatment before evaluating results. If you see improvement, you have your answer. If not, the issue may be more related to your skincare routine, climate, or clothing choices than to diet. Fungal acne is multifactorial, and diet is one lever among several — but it is a lever worth pulling.
Frequently Asked Questions
Can eating too much fruit cause fungal acne flares?
Whole fruit in moderate amounts is generally fine because the fiber slows sugar absorption. However, fruit juices, dried fruits, and tropical fruits like mangoes and pineapples have high sugar concentrations that can spike blood glucose. Stick to berries, green apples, and citrus in reasonable portions if you are concerned.
Does cutting out sugar completely cure fungal acne?
No. Diet alone does not cure fungal acne. Malassezia lives on everyone’s skin, and overgrowth is driven by multiple factors including humidity, occlusive skincare products, sweating, and immune function. Dietary changes support treatment but do not replace topical antifungals like ketoconazole or pyrithione zinc.
Is the anti-candida diet the same as a fungal acne diet?
There is significant overlap, but they are not identical. Anti-candida diets often eliminate all fermented foods, mushrooms, and vinegar, which is more restrictive than necessary for fungal acne management. Fungal acne dietary strategies focus primarily on reducing sugar, refined carbs, dairy, and alcohol — the foods with the strongest mechanistic links to sebum production and yeast overgrowth.
How long does it take to see skin improvements from dietary changes?
Most people who respond to dietary changes notice a reduction in new fungal acne lesions within three to six weeks. Existing bumps still need topical treatment to clear. If you see no change after six to eight weeks of consistent dietary modification, diet is likely not a major contributing factor in your case.
Are probiotics helpful for fungal acne?
Some evidence suggests that certain probiotic strains, particularly Saccharomyces boulardii and Lactobacillus rhamnosus, may help by improving gut health and immune regulation. However, probiotic supplements are not a proven treatment for fungal acne, and results vary widely between individuals. They are worth trying as a supplement to, not a replacement for, antifungal treatment.
You Might Also Like
- Why Fungal Acne Looks Like Regular Breakouts but Isn’t
- Why Antibiotics Don’t Work for Fungal Acne
- What Is Fungal Acne and How Is It Different from Regular Acne
Browse more: Acne | Acne Scars | Adults | Back | Blackheads