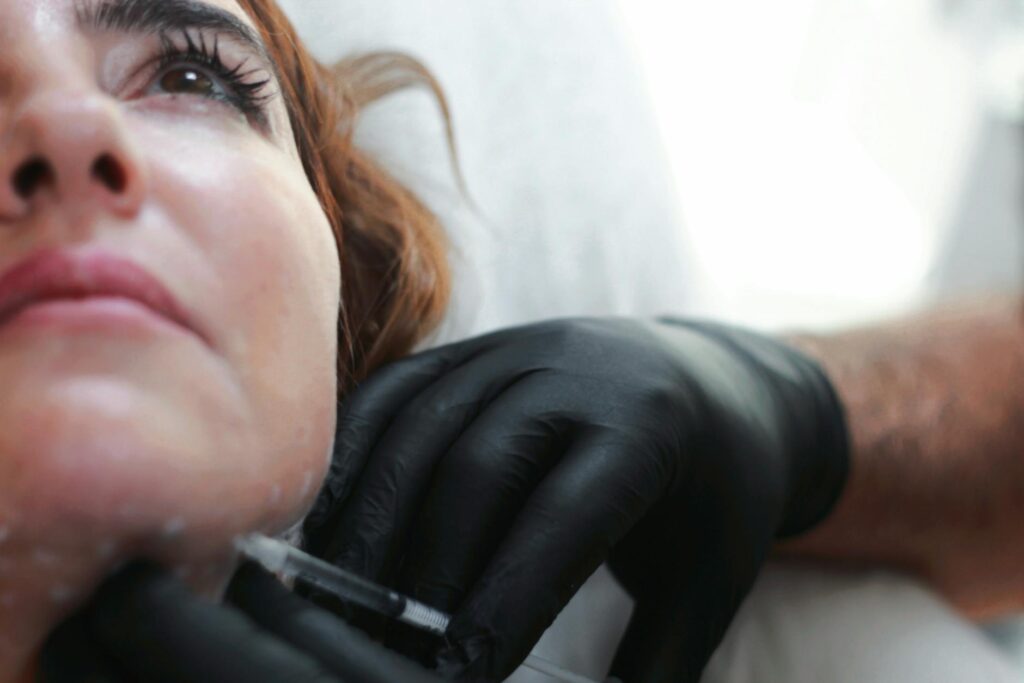
EGF injections work on acne scars by directly stimulating fibroblasts—the skin cells responsible for collagen production—through molecular signaling pathways, specifically the MAPK/ERK1/2 cascade. This activation causes fibroblasts to synthesize new collagen types I and III, the same structural proteins that create healthy skin architecture and fill in the depressed areas characteristic of atrophic acne scars. In addition to boosting collagen, EGF increases elastin and hyaluronic acid production while simultaneously suppressing pro-inflammatory cytokines like IL-1α and IL-8, which means the treatment not only rebuilds lost tissue but also creates an environment less prone to further inflammation that could worsen scarring.
The mechanism is grounded in real clinical data: studies show that patients using topical EGF for four weeks experienced significant reductions in both active acne lesions and visible scar counts, with nearly all participants reporting good to excellent improvements in their scarring. Twelve-week treatment protocols demonstrated even more dramatic improvements in atrophic scars, along with benefits to wrinkles and overall skin texture. This article explores how EGF triggers collagen synthesis, what the clinical evidence actually shows, how quickly results appear, and practical considerations for anyone considering this treatment as part of their scar management strategy.
Table of Contents
- How EGF Stimulates Collagen Synthesis in Acne Scarred Skin
- Clinical Evidence from Published Dermatological Studies
- Topical EGF Versus Injectable Administration
- Timeline and Realistic Expectations for Scar Improvement
- Variability in Results and Why Standardized Protocols Matter
- EGF Effectiveness for Darker and Skin-of-Color Populations
- Combining EGF with Laser and Other Scar-Reduction Therapies
- Conclusion
How EGF Stimulates Collagen Synthesis in Acne Scarred Skin
Epidermal growth factor is a 53-amino acid polypeptide that acts as a signaling molecule, binding to specific receptors on fibroblast cell surfaces. Once this binding occurs, it triggers the MAPK/ERK1/2 signaling pathway—a cascade of molecular events that tells fibroblasts to increase their production of structural proteins. Recombinant human EGF (rhEGF), the form used in clinical treatments, doesn’t just boost collagen; it increases expression of collagen type I (the predominant structural collagen), collagen type III (important for skin elasticity), elastin (which gives skin its bounce-back ability), and hyaluronic acid (a humectant that holds moisture in the dermis). This multi-directional approach to tissue repair distinguishes EGF from treatments that target only one component of skin integrity. Beyond building new tissue, EGF simultaneously reduces inflammation by suppressing pro-inflammatory markers like TNF-α, IL-1α, and IL-8.
This is particularly important because acne scars exist in a state of chronic inflammatory disruption; adding more collagen to inflamed tissue can actually worsen the appearance if inflammation isn’t addressed. Recombinant EGF also inhibits the inflammatory response triggered by Cutibacterium acnes (formerly Propionibacterium acnes), the bacterium responsible for acne, by reducing toll-like receptor 2 (TLR2) and NF-κB activity. This dual action—simultaneously reducing inflammation while stimulating collagen synthesis—creates conditions more favorable for actual scar remodeling rather than just filling with dead-end tissue. A practical example: someone with rolling atrophic scars (the wavy depressions most common on cheeks and temples) experiences both loss of structural collagen and ongoing low-grade inflammation in those areas. EGF addresses both problems simultaneously, which explains why patients report improvements not just in scar depth but also in skin texture and the overall appearance of affected areas, not just the scarred zones themselves.
Clinical Evidence from Published Dermatological Studies
A pilot study published in the Journal of Drugs in Dermatology examined patients using topical synthetic EGF serum applied daily for four weeks. The results were notably consistent: acne lesion counts and scar counts were significantly reduced across the cohort, and all but one patient reported “good” to “excellent” improvement in their scarring. This short timeline—just four weeks—suggests that EGF begins producing visible clinical benefit relatively quickly, though more extensive remodeling continues with longer treatment. A more comprehensive trial published in PMC examined twice-daily application of EGF serum over twelve weeks and found significantly improved atrophic acne scars, with patients also reporting improvements in wrinkles and skin texture.
This longer duration captured the deeper tissue remodeling that occurs when fibroblasts have sustained signaling to produce collagen. However, an important caveat emerged from more recent research: when EGF was combined with fractional CO2 laser therapy (a more aggressive resurfacing approach), the combination did shorten recovery time after the laser procedure and improved pore appearance, but it did not significantly enhance scar reduction beyond what the laser alone achieved. This suggests that EGF is most valuable for mild to moderate atrophic scars or as a maintenance treatment after more intensive procedures, rather than as a primary replacement for resurfacing therapies in severe scarring. The research community has noted significant variability across published studies regarding dosing protocols, administration routes (topical versus injectable), treatment frequency, and overall duration—meaning precise efficacy claims remain difficult to make without standardized protocols. The studies cited here represent the most rigorous published evidence available, but they shouldn’t be interpreted as definitive proof that all EGF formulations and delivery methods produce identical results.
Topical EGF Versus Injectable Administration
EGF is administered in two primary forms: topical serums applied to the skin surface, and injectable treatments placed directly into the dermis. Topical EGF serum is the most accessible form, available without prescription in many countries, and carries minimal risk of systemic side effects since the molecule doesn’t penetrate intact skin efficiently—it primarily affects the epidermis and superficial dermis. The clinical studies cited earlier showing four-week and twelve-week improvements all used topical formulations, making them the most evidence-backed approach for at-home treatment of acne scarring.
Injectable EGF, while theoretically capable of delivering higher concentrations directly to fibroblasts in the mid-to-deep dermis, has received less rigorous clinical validation specifically for acne scars. The advantage of injection would be achieving higher local concentrations with potentially faster results; the disadvantage is the invasiveness, cost, and lack of long-term safety data compared to topical application. Many dermatologists prefer to begin with topical EGF precisely because the clinical evidence is more substantial and the risk profile is clearer. If someone has already explored topical options and wants more aggressive treatment, injectable EGF might be considered, but this should be discussed with a dermatologist familiar with the specific formulation and its safety profile.
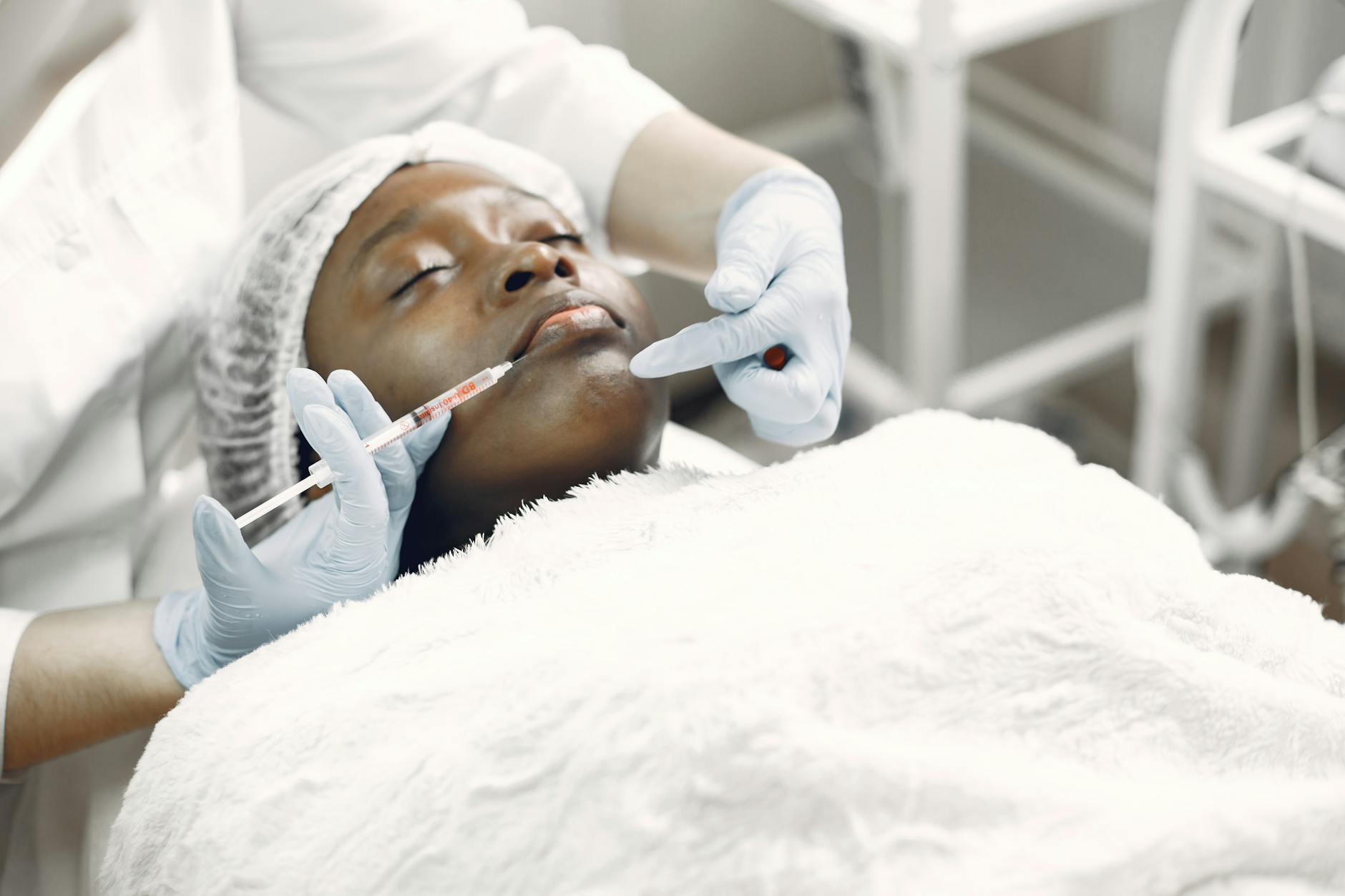
Timeline and Realistic Expectations for Scar Improvement
The clinical data suggests two distinct phases of improvement. The initial phase occurs within four weeks of starting twice-daily topical application, where visible reduction in active inflammation and initial improvements in scar appearance begin to manifest. This relatively rapid response occurs because EGF is immediately suppressing the inflammatory cytokines and initiating fibroblast signaling. However, the more substantial remodeling—filling in depressed scars and improving skin texture comprehensively—becomes more apparent by week twelve and likely continues beyond that point.
Most people should expect to use EGF serum consistently for at least twelve weeks before deciding whether it’s effective for their particular scars. This extended timeline reflects the biological reality of collagen remodeling: the body doesn’t rebuild tissue overnight. Some studies suggest ongoing improvement even beyond three months, but the most dramatic changes occur within the first twelve weeks. Importantly, this timeline assumes consistent twice-daily application; intermittent or sporadic use will produce slower, less dramatic results. Discontinuing the treatment doesn’t mean results are lost, but active fibroblast stimulation stops, so any ongoing collagen synthesis from the EGF signaling naturally tapers off.
Variability in Results and Why Standardized Protocols Matter
Not everyone responds identically to EGF treatment, and this variability is acknowledged in recent medical literature. Some individuals see dramatic improvement in rolling scars within twelve weeks, while others see modest improvement or show more benefit for wrinkles and texture than for deep scarring. This variability stems partly from differences in scar type (boxcar scars, ice-pick scars, and rolling scars may respond differently to collagen-stimulating treatments), partly from individual differences in fibroblast responsiveness, and partly from differences between EGF formulations themselves—pharmaceutical purity, concentration, and delivery mechanism vary across products.
The research community has flagged that the lack of standardized dosing and treatment protocols makes it difficult to predict precisely who will benefit and how much. One person applying EGF serum with a concentration of 50 ng/mL twice daily might experience superior results to someone applying a different formulation with a higher nominal concentration but lower bioavailability. This is why choosing a formulation that has been studied clinically (such as those used in the PMC and JDD studies cited here) is more reliable than assuming all products perform equally. Additionally, if someone has very deep or severe atrophic scarring—particularly ice-pick type scars that penetrate to the subcutis—EGF alone may not produce satisfactory results, and combination with fractional laser or microneedling might be necessary, though the evidence for combination approaches remains mixed.

EGF Effectiveness for Darker and Skin-of-Color Populations
Clinical data specifically examining EGF efficacy in darker skin types is more limited than data for lighter skin, but existing research is encouraging. A study published in the Journal of the American Academy of Dermatology documented that topical EGF serum improved atrophic acne scars in patients with darker skin types, suggesting that the underlying collagen-synthesis mechanism is not race-dependent.
This is important because many scar treatments have been optimized primarily on lighter skin, sometimes with unpredictable results or different efficacy in melanin-rich skin. However, the smaller body of evidence for skin-of-color populations means individual results may vary more, and dermatologists working with patients of color should discuss whether additional studies specific to their skin type might inform treatment decisions. EGF’s anti-inflammatory mechanism is particularly relevant for darker skin types prone to post-inflammatory hyperpigmentation, since reducing inflammation may help prevent or minimize pigmentary changes that sometimes accompany scar remodeling treatments.
Combining EGF with Laser and Other Scar-Reduction Therapies
Recent research has explored combining EGF with fractional CO2 laser resurfacing, a gold-standard approach for atrophic scarring. The combination produced shorter recovery periods after laser treatment and improved pore appearance, which is a practical benefit since fractional laser can temporarily worsen appearance during healing. However, as noted in the 2024 Journal of Cosmetic Dermatology study, the combination did not significantly enhance scar reduction itself beyond what the laser alone achieved, suggesting that EGF may be better suited as a complementary treatment for recovery and skin quality rather than as a synergistic collagen-stimulation booster when combined with aggressive ablative procedures.
The implication is that if someone is planning fractional laser for acne scars, adding EGF topically both before and after laser may improve healing comfort and final skin texture, but shouldn’t be framed as intensifying scar reduction. Conversely, for mild to moderate scars where laser isn’t appropriate, EGF monotherapy offers a gentler alternative that the clinical data supports. Combining EGF with gentler modalities like microneedling or radiofrequency has not been as rigorously studied, but the mechanism suggests potential complementary benefit since both approaches stimulate fibroblast activity through different pathways.
Conclusion
EGF injections and topical treatments work on acne scars by activating fibroblast cells to synthesize new collagen types I and III, elastin, and hyaluronic acid through the MAPK/ERK1/2 signaling pathway. The clinical evidence, primarily from topical formulation studies, shows meaningful improvements in atrophic scar appearance within four weeks and more substantial remodeling by twelve weeks, accompanied by benefits to wrinkles and overall skin texture. The mechanism simultaneously suppresses pro-inflammatory cytokines, creating conditions where tissue can truly remodel rather than simply fill with scar tissue.
The key takeaway is that EGF represents a legitimate, evidence-backed option for mild to moderate atrophic acne scarring, particularly for individuals seeking a gentler alternative to aggressive resurfacing procedures. However, standardized clinical protocols are still needed, results vary based on scar type and individual fibroblast responsiveness, and severe scarring may require combination approaches. Anyone considering EGF treatment should commit to at least twelve weeks of consistent twice-daily application and should select formulations that have been studied clinically rather than assuming all products perform equally. Consultation with a dermatologist familiar with EGF mechanisms and having realistic expectations about timeline and scar type will produce the best outcomes.
You Might Also Like
- What i-PRF vs L-PRF Means for Acne Scar Treatment Protocols
- What XoGlo Exosomes Do for Acne Scar Remodeling
- What Wnt Signaling Inhibition Does for Sebocyte Activity in Acne
Browse more: Acne | Acne Scars | Adults | Back | Blackheads