Dermaplaning on active, inflamed acne is a bad idea — and most dermatologists will tell you not to do it. The procedure involves dragging a sterile surgical scalpel across the skin at a shallow angle to remove dead cells and vellus hair, and when that blade crosses over pustules, cysts, or inflamed pimples, it can spread *Cutibacterium acnes* bacteria from one lesion to unaffected areas of your face. According to the Cleveland Clinic, Texas Dermatology, and BHSkin Dermatology, dermaplaning is contraindicated on active acne precisely because of this bacterial transfer risk. The result is not smoother skin — it is more breakouts, increased swelling, and potential scarring.
That said, the picture is not entirely bleak. For people whose acne has fully cleared and who are left dealing with residual texture or shallow scarring, dermaplaning can offer real benefits: better product absorption, reduced surface bacteria, and a smoother skin surface. The distinction between active acne and post-acne skin is the single most important factor in determining whether this procedure helps or harms you. This article breaks down what actually happens when a blade meets acne-prone skin, who should avoid dermaplaning entirely, who might benefit from it, how professional treatments compare to at-home attempts, and what alternatives exist for scars that dermaplaning cannot touch.
Table of Contents
- What Does Dermaplaning Actually Do to Acne-Prone Skin?
- Side Effects and Risks You Need to Know Before Booking
- When Dermaplaning Can Actually Help Post-Acne Skin
- Professional Dermaplaning vs. At-Home Tools — What the Risk Gap Looks Like
- Who Should Not Get Dermaplaning — Hard Contraindications
- Alternatives That Work Better for Acne-Prone Skin
- Making a Smarter Decision About Dermaplaning
- Conclusion
- Frequently Asked Questions
What Does Dermaplaning Actually Do to Acne-Prone Skin?
Dermaplaning removes the outermost layer of the stratum corneum along with fine vellus hair (peach fuzz) using a single-blade surgical scalpel held at a 45-degree angle. On healthy or healed skin, this creates a temporarily smoother surface and allows serums, moisturizers, and treatments to penetrate more effectively. Texas Dermatology and BHSkin Dermatology note that by clearing away dead skin cells and surface-level bacteria, the procedure can reduce some of the buildup that contributes to clogged pores — but only when there are no active lesions present. On acne-prone skin with active breakouts, the mechanics work against you. The blade does not distinguish between healthy skin and an inflamed papule.
Scraping over a pustule ruptures it, releasing bacteria and inflammatory contents that the blade then drags across the rest of your face. Think of it like using a single cloth to wipe down a countertop that has both clean and contaminated areas — you end up spreading the problem rather than resolving it. Cosmediclasermd.com and Express Med Spa both emphasize that this mechanical disruption worsens swelling, damages the already-compromised skin barrier, and increases the risk of secondary infection or permanent scarring. It is also worth noting that the American Academy of Dermatology has not officially endorsed dermaplaning as a standard acne treatment or routine skincare procedure. The Cleveland Clinic points out that more clinical research is needed to confirm both its safety profile and its efficacy for various skin types. This does not mean the procedure is dangerous in all contexts, but it does mean that claims about dermaplaning being universally beneficial for acne-prone skin are getting ahead of the evidence.
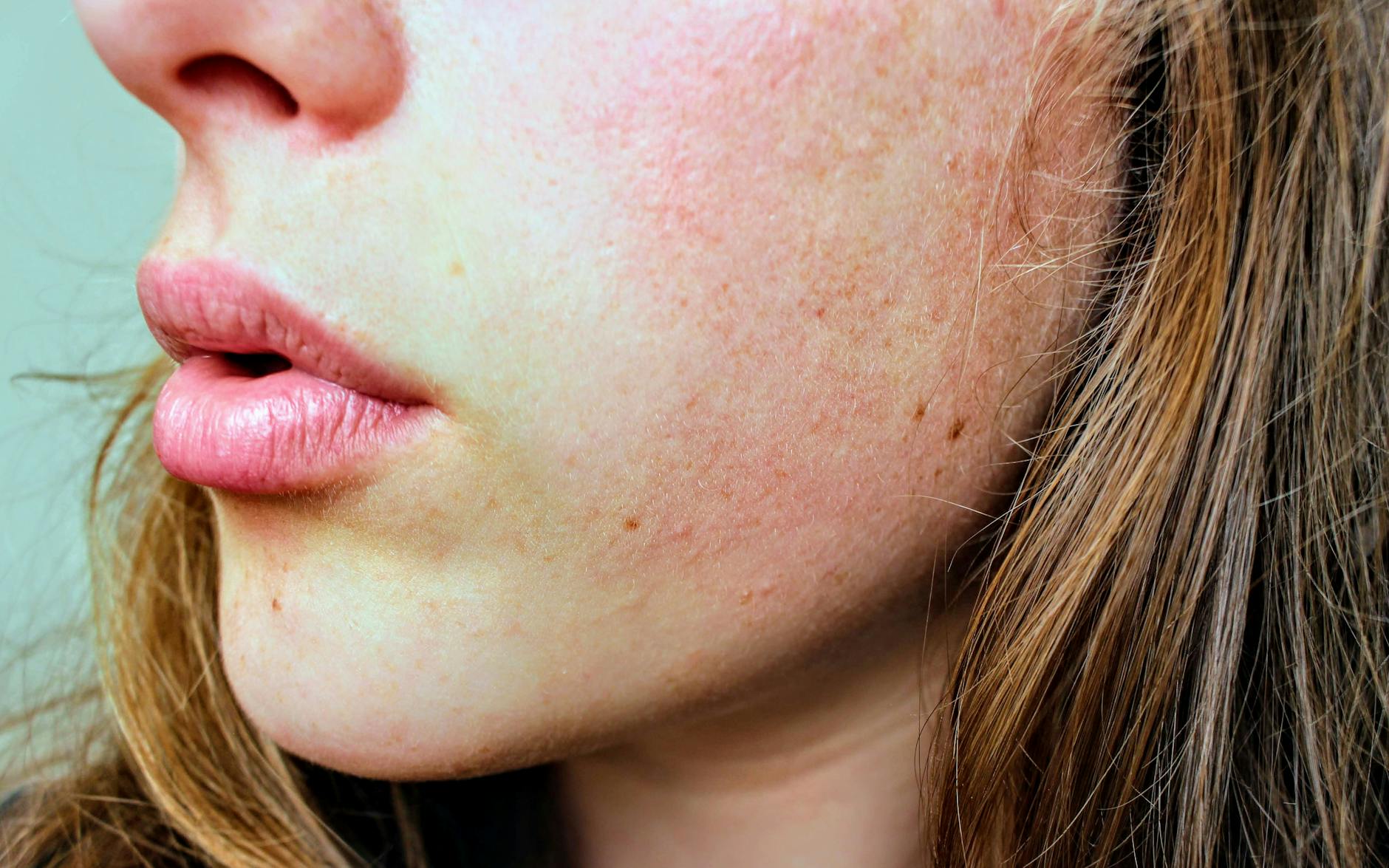
Side Effects and Risks You Need to Know Before Booking
Even on skin without active acne, dermaplaning carries a set of side effects that anyone with breakout-prone skin should weigh carefully. The most common is mild redness and irritation, which the Cleveland Clinic says typically subsides within 24 to 48 hours. For most people, this is manageable. However, if you are already dealing with a sensitized barrier — from retinoid use, recent chemical exfoliation, or a condition like rosacea — that post-procedure irritation can trigger a reactive breakout or prolonged inflammation. Increased photosensitivity is another significant concern. By removing the outermost protective layer of skin, dermaplaning leaves you more vulnerable to UV damage.
Broad-spectrum SPF 30 or higher is non-negotiable afterward, according to both the Cleveland Clinic and White Pebble Dermatology. For acne-prone individuals who already struggle with post-inflammatory hyperpigmentation, unprotected sun exposure after dermaplaning can darken existing marks and create new discoloration that takes months to fade. Then there is skin purging — a temporary increase in breakouts as clogged debris works its way to the surface after exfoliation. Curology and Kalon Dermatology both acknowledge this as a real phenomenon. The challenge for acne-prone individuals is distinguishing between a normal purge that resolves in a week or two and a genuine worsening of acne caused by bacterial spread or barrier damage. If new breakouts appear in areas you do not typically break out, or if they are deeper and more inflamed than your usual blemishes, that is more likely a sign of damage than purging. Improper technique — whether from an unlicensed provider or a DIY attempt — adds the risks of bleeding, infection, and scar formation, as Healthline and the Cleveland Clinic have both documented.
When Dermaplaning Can Actually Help Post-Acne Skin
The conversation shifts meaningfully when we talk about skin that has moved past the active breakout phase. For people with healed acne and residual textural concerns, dermaplaning offers a few legitimate advantages. Texas Dermatology and BHSkin Dermatology both note that by clearing dead skin and vellus hair, the procedure creates a smoother canvas that absorbs topical treatments more efficiently. If you are using niacinamide, azelaic acid, or other acne-preventing ingredients, better penetration means those products work harder. Mild, shallow acne scars — the kind that create a slightly uneven texture without deep pitting — can appear reduced after dermaplaning. According to Cosmediclasermd.com and Exposed Skin Care, the procedure smooths the outermost skin layer enough to soften the visual appearance of superficial scarring.
For someone with a scattering of mild rolling scars across the cheeks, a series of professional dermaplaning sessions combined with a consistent skincare routine can produce noticeable improvement in skin texture and light reflection. However, there is a hard limit to what dermaplaning can accomplish with scarring. Deep scars — ice-pick scars that create narrow, deep holes in the skin, or boxcar scars with sharp vertical edges — are not treatable with dermaplaning. A 2022 review published in the MDPI Journal of Clinical Medicine makes clear that these types of scars require more aggressive interventions: microneedling, chemical peels, fractional laser resurfacing, or subcision. If you go into dermaplaning expecting it to fix pitted scarring, you will be disappointed and out several hundred dollars. Know the type of scarring you have before you book.

Professional Dermaplaning vs. At-Home Tools — What the Risk Gap Looks Like
The difference between professional and DIY dermaplaning is not just about results — it is about safety, and this gap widens considerably for acne-prone skin. A licensed esthetician or dermatologist uses a sterile, medical-grade scalpel, maintains proper blade angle and pressure, and can assess your skin in real time, avoiding areas of irritation or emerging breakouts that you might not recognize. Express Med Spa and Kulani Spa both strongly recommend professional treatment over at-home attempts for anyone with a history of acne. At-home dermaplaning tools — typically small, single-blade razors marketed as facial exfoliators — carry higher risks across the board. Healthline notes that improper angle and excessive pressure are common with these devices, leading to nicks, micro-cuts, and uneven exfoliation. For acne-prone skin specifically, the cross-contamination risk multiplies. A professional uses a fresh blade for each pass and follows strict sanitation protocols.
At home, people frequently reuse blades, fail to sanitize properly between uses, and inadvertently drag bacteria across their face without realizing it. The tradeoff is cost. Professional dermaplaning typically runs between $100 and $250 per session, and most providers recommend treatments every three to four weeks. At-home tools cost $10 to $30 and can be used repeatedly. But for acne-prone skin, the savings are deceptive. One infected nick or one round of bacterial spread can set your skin back weeks and potentially require a dermatologist visit that costs more than the professional dermaplaning session you skipped. If budget is a genuine concern, spacing professional sessions further apart is a safer compromise than switching to DIY.
Who Should Not Get Dermaplaning — Hard Contraindications
Beyond active acne, several other conditions and medications make dermaplaning inadvisable. If you are currently using retinoids — whether prescription tretinoin or over-the-counter retinol — your skin is already in an accelerated state of cell turnover and is thinner and more sensitized than usual. Adding mechanical exfoliation on top of chemical exfoliation is a recipe for barrier destruction, redness, and rebound breakouts. Most dermatologists recommend stopping retinoid use for at least five to seven days before dermaplaning, though some advise a longer pause depending on the strength of the product. Isotretinoin (Accutane) is an absolute contraindication.
Patients on isotretinoin or those who have completed a course within the past six months have significantly compromised skin healing, and dermaplaning can cause disproportionate scarring and irritation. The Cleveland Clinic and Madison Wellness both advise consulting a dermatologist before scheduling dermaplaning if you have a history of cystic acne, rosacea, eczema, or psoriasis — conditions where the skin barrier is already under stress. There is a subtler risk that often goes undiscussed: the psychological cycle of over-treating acne-prone skin. Dermaplaning can feel productive — you are physically removing what seems like problematic buildup. But for people prone to skin-picking or compulsive skincare routines, adding another exfoliating procedure can feed a pattern of over-exfoliation that strips the barrier and triggers the very breakouts they are trying to prevent. If you find yourself constantly adding new exfoliating steps to your routine, the most effective intervention might be doing less, not more.

Alternatives That Work Better for Acne-Prone Skin
For active acne, targeted treatments will always outperform blanket exfoliation. Chemical exfoliants like salicylic acid (a beta-hydroxy acid that penetrates into pores) address acne at its source without the bacterial-spread risk of a blade. For post-acne scarring that dermaplaning cannot reach, the MDPI Journal of Clinical Medicine’s 2022 review highlights microneedling as particularly effective for atrophic scars — it stimulates collagen remodeling at controlled depths without shearing the skin surface.
Fractional laser resurfacing and medium-depth chemical peels (such as TCA peels) offer more dramatic results for deep scarring, though they come with longer downtime and higher cost. The key comparison is this: dermaplaning is a surface-level procedure that works well for surface-level concerns. When the problem extends deeper — into the dermis, into active infection, into hormonal or cystic patterns — surface-level tools are not enough, and using them anyway creates a false sense of progress while the underlying issues persist or worsen.
Making a Smarter Decision About Dermaplaning
The trajectory of dermaplaning in skincare is trending toward more nuance and better patient screening. As more dermatologists speak publicly about contraindications and the limits of the procedure, the days of one-size-fits-all exfoliation recommendations are fading. What is replacing them is a more individualized approach: assess the patient’s current skin state, check for active lesions and medication interactions, and only proceed when the conditions are clearly favorable.
If you are considering dermaplaning and have any history of acne, the smartest first step is a consultation with a board-certified dermatologist — not an esthetician, not a med spa intake form, and definitely not a social media tutorial. A dermatologist can evaluate whether your skin is in the right condition for the procedure, identify scar types that dermaplaning will not improve, and recommend alternatives where appropriate. Waiting until your skin is truly clear before booking is not overly cautious. It is the difference between a procedure that helps and one that sets you back.
Conclusion
Dermaplaning is not inherently harmful to acne-prone skin — but the timing and context determine everything. On active, inflamed acne, the blade spreads bacteria, ruptures lesions, and damages an already struggling skin barrier. On healed, clear skin with residual texture or shallow scarring, it can genuinely improve smoothness and product absorption.
The line between these two scenarios is the line between a helpful cosmetic procedure and an avoidable setback. The practical takeaways are straightforward: wait until active breakouts have fully resolved, always choose a licensed professional over at-home tools if you have a history of acne, wear broad-spectrum SPF 30 or higher after every session, and do not expect dermaplaning to address deep or pitted scars. If your acne is cystic, hormonally driven, or currently being treated with retinoids or isotretinoin, talk to a dermatologist before putting a blade anywhere near your face. There are plenty of effective treatments available — the goal is matching the right one to your skin’s current reality, not its aspirational state.
Frequently Asked Questions
Can dermaplaning cause acne breakouts?
Yes, particularly if performed on skin with active acne. The blade can transfer *Cutibacterium acnes* bacteria between blemishes and spread infection to unaffected areas. Even on clear skin, some people experience temporary skin purging — a short-lived increase in breakouts as trapped debris surfaces after exfoliation. This typically resolves within one to two weeks.
How long should I wait after a breakout before getting dermaplaning?
Wait until all active lesions — including pustules, cysts, and inflamed papules — have fully healed. This generally means no active redness, swelling, or tenderness in the area. For cystic breakouts, this can take several weeks. A dermatologist can confirm when your skin is ready.
Does dermaplaning help with acne scars?
It can improve the appearance of mild, shallow acne scars by smoothing the outermost layer of skin. However, deeper scars such as ice-pick or boxcar types require more intensive treatments like microneedling, chemical peels, or fractional laser resurfacing. Dermaplaning alone will not meaningfully reduce deep or pitted scarring.
Is at-home dermaplaning safe for acne-prone skin?
It carries significantly higher risk than professional treatment. Improper blade angle, excessive pressure, and poor sanitation increase the chances of nicks, bacterial spread, and infection. If you have acne-prone skin, professional dermaplaning by a licensed esthetician or dermatologist is strongly recommended.
Can I use retinol or retinoids before dermaplaning?
Most dermatologists advise stopping retinoid use at least five to seven days before the procedure. Retinoids thin the skin and accelerate cell turnover, making it more vulnerable to irritation and damage from mechanical exfoliation. If you are on isotretinoin, dermaplaning is contraindicated entirely.
How often can acne-prone skin safely undergo dermaplaning?
For acne-prone skin that is currently clear, most professionals recommend spacing sessions three to four weeks apart to allow the skin barrier to fully recover between treatments. More frequent sessions increase the risk of over-exfoliation, barrier damage, and reactive breakouts.
You Might Also Like
- What HydraFacial Does for Acne-Prone Skin
- What Dry Climate Does to Acne-Prone Skin
- Why Silk Pillowcases Help Acne-Prone Skin
Browse more: Acne | Acne Scars | Adults | Back | Blackheads