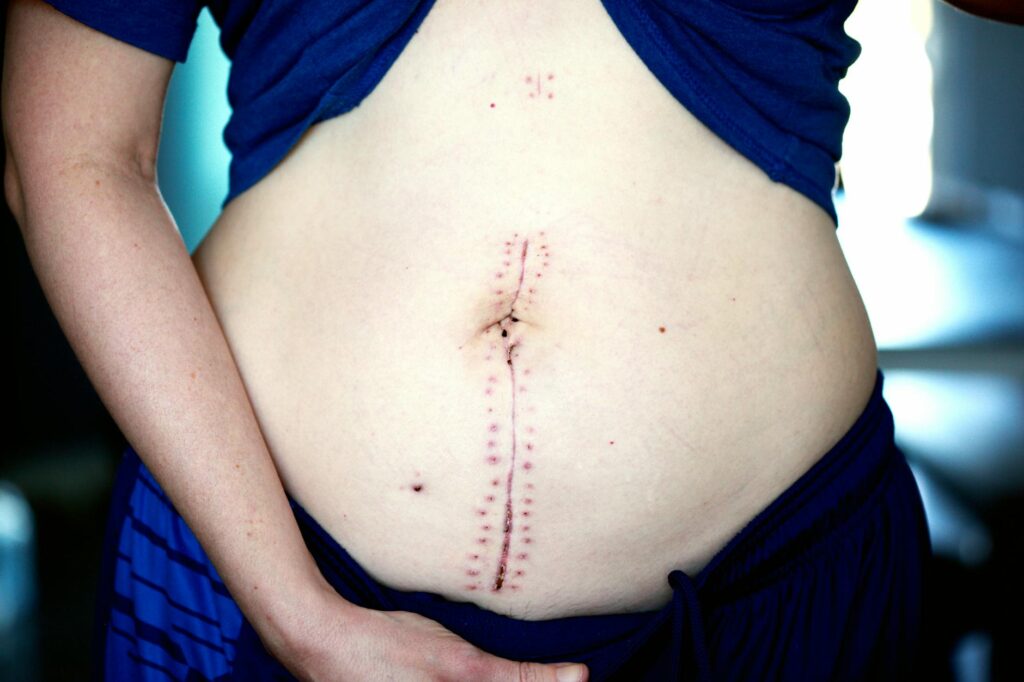
Compression after subcision primarily works by minimizing post-procedure swelling, stabilizing the newly freed scar tissue, and creating an environment where collagen can remodel effectively beneath the skin’s surface. When a dermatologist performs subcision—cutting the fibrous bands that tether rolling scars—the area fills with blood and lymph fluid that must be managed to prevent complications and maximize the skin’s ability to form new collagen. Compression garments or dressings applied immediately after the procedure reduce this fluid accumulation, which directly translates to less bruising, faster healing, and better long-term scar improvement. This article covers how compression works mechanically during healing, the optimal timeline and types of compression to use, how it interacts with collagen remodeling, practical considerations for different scar locations, and realistic expectations for combining compression with other treatments.
Table of Contents
- How Does Compression Support the Healing Response After Subcision?
- Compression Timing and Duration – When to Apply and for How Long
- The Impact of Compression on Collagen Remodeling and Scar Improvement
- Choosing the Right Compression Method – Garments, Tape, and Custom Dressings
- When Compression Falls Short – Limitations and Complications
- Combining Compression with Topical and Injectable Post-Subcision Care
- Long-Term Outcomes and Setting Realistic Scar Expectations
- Conclusion
- Frequently Asked Questions
How Does Compression Support the Healing Response After Subcision?
When subcision is performed, the dermatologist deliberately creates controlled trauma to break the scar’s attachment to deeper skin layers. This immediately triggers bleeding and inflammatory fluid accumulation in the treatment area.
Compression counteracts this by applying consistent, gentle pressure that keeps the wound surfaces in closer contact, reduces the space available for fluid to collect, and minimizes the risk of hematoma (blood clots) or seroma (fluid pockets) formation. For someone receiving subcision on their cheeks for rolling acne scars, compression applied within hours of treatment can prevent the kind of dramatic swelling and bruising that might otherwise last three to four weeks—instead reducing it to one to two weeks. The pressure also stabilizes the newly freed scar tissue, preventing it from re-tethering while the body lays down new collagen fibers in a more organized pattern.

Compression Timing and Duration – When to Apply and for How Long
The first 48 to 72 hours after subcision are the most critical window for compression, when swelling and bleeding risk are highest. Most dermatologists recommend continuous or near-continuous compression during this period—either through pressure dressings left in place or a compression garment worn throughout the day and night.
However, the pressure must be moderate rather than tourniquet-tight; excessive compression can impair blood flow and delay healing. After the acute phase, many dermatologists recommend tapering to daytime-only compression for another one to two weeks, with the understanding that some swelling naturally continues for weeks afterward. A key limitation here is that compression consistency matters: if a patient removes their compression garment frequently or inconsistently during the critical 72-hour window, the benefit drops significantly, and they may end up with the same level of bruising and swelling as if they hadn’t compressed at all.
The Impact of Compression on Collagen Remodeling and Scar Improvement
Beneath the visible swelling, subcision’s benefit comes from triggering a controlled healing cascade where new collagen fills the space below the scar. Compression doesn’t directly accelerate collagen production, but by reducing inflammation and stabilizing the wound architecture, it allows collagen fibers to organize along tension lines in a more functional way rather than forming random, disorganized scar tissue.
In the weeks following subcision with proper compression, the body’s fibroblasts (collagen-producing cells) migrate into the treated area, and the resulting collagen tends to be more elastic and less restrictive than the original scar tissue. Studies on surgical wound healing show that moderate compression reduces excessive inflammatory markers and can slightly improve final scar texture compared to untreated controls. However, compression alone won’t correct all subcision results—if the dermatologist didn’t cut deep enough or release all the tethering fibers, compression won’t compensate for that technical limitation.

Choosing the Right Compression Method – Garments, Tape, and Custom Dressings
The method of compression varies by the location and size of the treated area. Small areas, like a few acne scars on the cheeks, might use medical-grade compression tape or adhesive bandages that stay in place for 48 to 72 hours. Larger treatment areas or full-face subcision may require a compression garment—some dermatologists use elastic face masks or custom-wrapped pressure dressings, while others recommend compression sleeves or garments designed for post-procedural use.
Prescription-grade compression garments (Class II or III) provide more consistent, measurable pressure than off-the-shelf elastic bandages and are worth the extra cost if your insurance covers them. A practical tradeoff exists between comfort and effectiveness: tighter compression is more effective at reducing swelling but becomes uncomfortable and can restrict normal facial movement for eating or sleeping. Many patients find the sweet spot is compression firm enough to feel stable but loose enough to tolerate continuously for 2-3 days.
When Compression Falls Short – Limitations and Complications
Compression is highly effective at reducing post-procedure fluid accumulation, but it cannot prevent all complications and has defined limits. Patients on blood thinners or anticoagulants may still develop significant bruising despite compression, because their bleeding is driven by medication rather than just the local trauma.
Additionally, some patients develop persistent seroma (fluid pockets) even with optimal compression—this is usually a sign that the dermatologist should perform drainage, which compression alone won’t resolve. Another limitation: compression doesn’t reduce pain, and some patients find the pressure uncomfortable enough that they remove the garment prematurely, defeating its purpose. If a patient has very thin, fragile skin or a tendency toward keloid or hypertrophic scarring, compression may need to be gentler or applied for a shorter duration, as aggressive compression can sometimes irritate sensitive skin or rarely contribute to keloid formation.
Combining Compression with Topical and Injectable Post-Subcision Care
While compression manages swelling, dermatologists often prescribe complementary treatments to optimize results. A typical post-subcision regimen combines compression with topical retinoids (starting one to two weeks after the procedure, once initial healing is underway), vitamin C serums for antioxidant support, and sometimes injectable fillers or steroid injections placed weeks later to further elevate depressed scars.
Compression and retinoids work synergistically: compression reduces inflammation that could be triggered by retinoid irritation, and once the skin is healed enough for retinoids, they promote collagen remodeling in the newly released scar area. Using topical vitamin C while wearing compression is generally safe—the compression doesn’t significantly interfere with product absorption—though some serums are occlusive and can feel uncomfortable under tight garments.
Long-Term Outcomes and Setting Realistic Scar Expectations
The benefit of compression appears in two phases: immediate (reduced swelling and bruising over days to weeks) and delayed (improved final scar appearance over months). Because collagen remodeling continues for three to six months post-subcision, the true final result doesn’t emerge until months later—not immediately after compression is discontinued.
Patients who properly compress for the first two to three weeks typically see 30 to 40% improvement in rolling scars by the three-month mark, with additional subtle improvement through six months. This improvement comes from the combination of the subcision cut itself, the inflammatory response it triggers, and the collagen reorganization that compression helps facilitate. As new subcision techniques develop and dermatologists gain more experience with extended compression protocols (some now recommend low-level compression even into week four), outcomes continue to improve slightly, though the gains are incremental rather than revolutionary.
Conclusion
Compression after subcision is a simple, evidence-backed tool that reduces swelling, prevents complications, and optimizes the collagen remodeling process that actually improves rolling scars. The critical window is the first 72 hours, where consistent, moderate compression has the most measurable impact on bruising and fluid accumulation.
However, compression is one component of scar improvement—the subcision procedure itself must be technically sound, and post-procedure care must include appropriate retinoids and sun protection for best results. If you’re considering subcision for rolling acne scars, discuss compression protocols with your dermatologist, have a plan for obtaining the appropriate compression garment before your appointment, and understand that the most dramatic improvements appear over months, not days, as new collagen fills the treated area.
Frequently Asked Questions
How tight should compression be after subcision?
Compression should feel firm and supportive but not painfully tight. A good test is that you can slip one finger under the edge of the garment or dressing. If you can’t get any finger underneath, it’s too tight and risks cutting off blood flow.
Can I shower or bathe while wearing compression after subcision?
Most dermatologists recommend keeping compression dressings dry for the first 48 to 72 hours. If you need to bathe, many recommend removing the dressing, bathing quickly, patting skin dry thoroughly, and reapplying the dressing immediately. Ask your dermatologist for specific instructions, as some use waterproof dressings that can stay on.
Will compression prevent keloid scars or hypertrophic scars from forming?
Moderate compression may slightly reduce the risk of keloid or hypertrophic scarring by controlling inflammation, but it’s not a guarantee. Patients with a personal or family history of keloids should discuss this risk with their dermatologist, as keloid tendency is genetic, and compression alone won’t prevent them in predisposed individuals.
How long after subcision can I resume normal activities while wearing compression?
Most patients can resume light daily activities immediately—working at a desk, walking, eating—while wearing compression. Strenuous exercise, heavy lifting, and activities that increase blood pressure should be avoided for one to two weeks, as they increase swelling despite compression.
Is compression necessary if I’m not seeing much bruising or swelling after subcision?
Yes. Even if bruising isn’t visible, internal swelling and fluid accumulation still occur. Compression prevents complications like seroma and optimizes the healing environment regardless of whether you “look” swollen, so it’s recommended for all subcision patients unless contraindicated.
You Might Also Like
- Why Under-Eye Hollowing Worsens After Laser for Acne Scars
- What to Put on Your Face After CO2 Laser for Scars
- What to Avoid After Microneedling for Acne Scars
Browse more: Acne | Acne Scars | Adults | Back | Blackheads