BenzaClin and Duac are essentially the same medication in different application schedules. Both contain 5% benzoyl peroxide and 1% clindamycin—a combination that tackles acne through two complementary mechanisms. The primary difference is that BenzaClin requires twice-daily application (morning and evening), while Duac is applied once daily at bedtime.
This difference matters more than you might expect: clinical data shows that Duac’s once-daily dosing often leads to better skin tolerance and improved treatment compliance, even though both formulations produce similar efficacy rates when used as directed. This article explores how these two topical antibiotics compare in mechanism, effectiveness, side effects, and practical application, so you can understand which approach might work better for your acne. Both medications work by combining benzoyl peroxide’s bacterial-killing and skin-normalizing properties with clindamycin’s antibiotic action against acne-causing bacteria. The choice between them typically comes down to lifestyle, sensitivity concerns, and how well you tolerate twice-daily versus once-daily routines.
Table of Contents
- How Do the Active Ingredients in BenzaClin and Duac Work Against Acne?
- Clinical Efficacy—Do BenzaClin and Duac Perform Similarly?
- Side Effects and Skin Irritation—Which Product Is Gentler?
- Practical Considerations—Which Dosing Schedule Works Better in Real Life?
- Antibiotic Resistance and Long-Term Use Considerations
- Drug Interactions and Compatibility with Other Acne Treatments
- Finding the Right Treatment Plan Within Your Acne Management Strategy
- Conclusion
How Do the Active Ingredients in BenzaClin and Duac Work Against Acne?
Both BenzaClin and Duac use the same active ingredients at identical concentrations, so their fundamental mechanism is identical. The clindamycin component works by binding to the bacterial ribosomal subunits in *Propionibacterium acnes*—the primary bacteria implicated in acne formation—and inhibiting peptide-bond formation, which stops the bacteria from producing the proteins it needs to survive. The benzoyl peroxide acts as a bactericidal oxidizing agent, meaning it directly kills acne bacteria rather than just inhibiting their growth.
Additionally, benzoyl peroxide is keratolytic, which means it helps dissolve dead skin cells that can clog pores, and it’s sebostatic, meaning it reduces excess oil production—a major acne trigger. The synergy between these two ingredients is what makes them effective in combination. Benzoyl peroxide is particularly valuable because it prevents bacteria from developing resistance to clindamycin, a problem that can occur when antibiotic monotherapy is used alone. Clinical studies show that combination therapy with these two agents significantly outperforms either ingredient used alone, with superior results in inflammatory lesion reduction compared to clindamycin or benzoyl peroxide as standalone treatments.

Clinical Efficacy—Do BenzaClin and Duac Perform Similarly?
Both medications have solid clinical backing for acne treatment. BenzaClin studies demonstrated a 64.1% reduction in inflammatory lesion counts and a 48.7% reduction in noninflammatory lesions after 12 weeks of use, with an average 52% decrease in inflammatory acne lesions by week 12. Duac similarly showed superiority to clindamycin alone in four out of five clinical studies and to benzoyl peroxide alone in three out of five studies for inflammatory lesion reduction. The efficacy profiles are comparable, meaning that the choice between them won’t be determined by one product being substantially more powerful than the other.
However, there’s an important caveat: these efficacy numbers assume consistent, proper use. Because BenzaClin requires twice-daily application and Duac requires only once-daily application, real-world compliance differences can significantly affect outcomes. A patient who misses or skips morning applications with BenzaClin will see reduced results over time, whereas Duac’s simpler routine may be easier to maintain consistently. Additionally, some patients discontinue BenzaClin earlier due to irritation from the twice-daily regimen, which can short-circuit treatment before the 12-week efficacy window is complete.
Side Effects and Skin Irritation—Which Product Is Gentler?
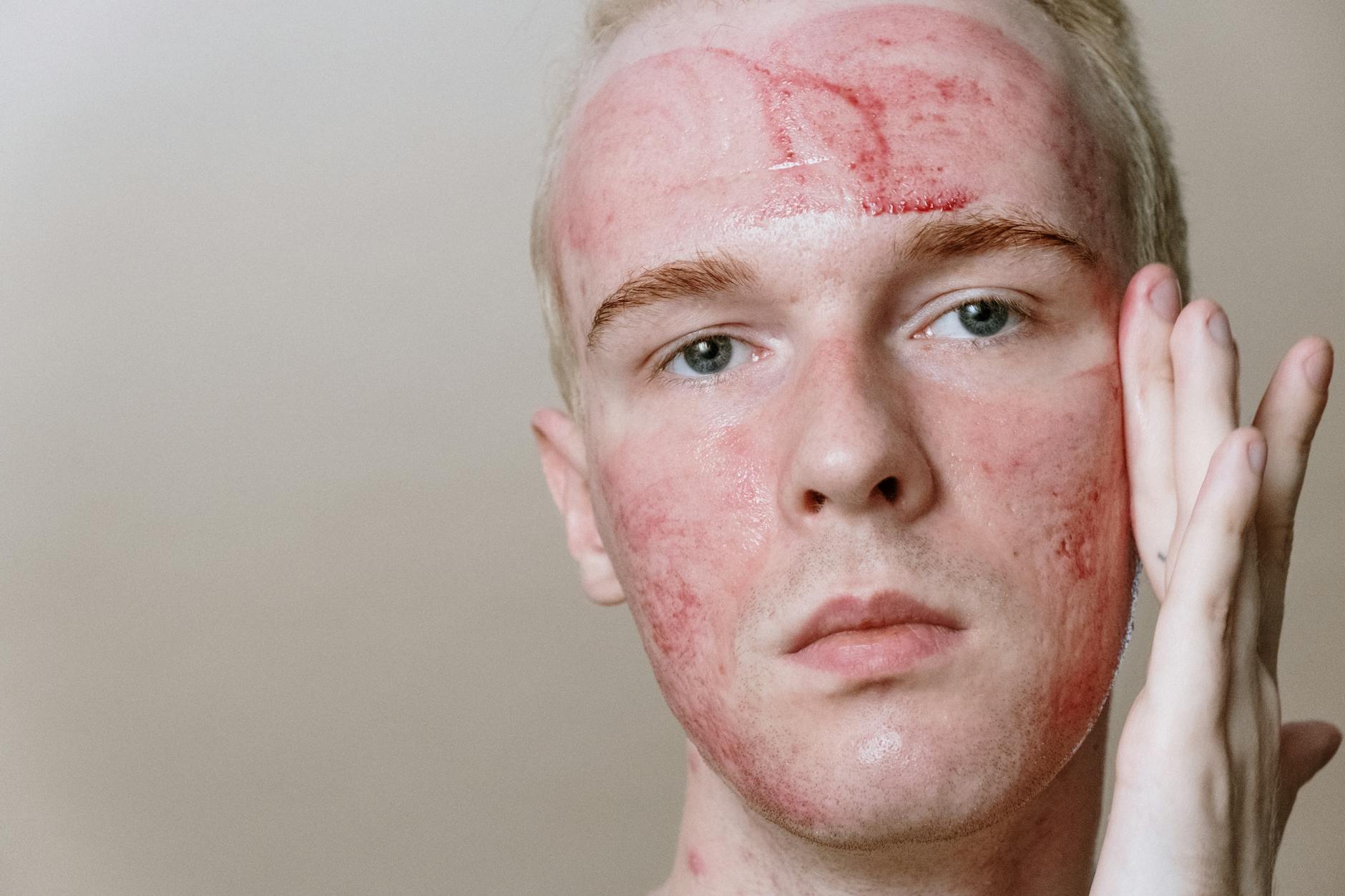
Both products cause similar types of irritation at the application site, including peeling, itching, dryness, and redness. Benzoyl peroxide and clindamycin are both known irritants, particularly when skin is just beginning treatment and hasn’t adapted to the medications. However, BenzaClin typically causes more noticeable irritation in practice because of its twice-daily dosing schedule, which means skin is exposed to the ingredients twice as often as with Duac’s once-daily bedtime application. This irritation difference is clinically meaningful.
A patient using BenzaClin might experience significant peeling and dryness throughout the day, which can be uncomfortable and cosmetically problematic in professional or social settings. Duac’s bedtime-only application means irritation typically occurs overnight, when the skin can be covered and when sleep may allow the skin to recover. For individuals with sensitive skin, rosacea-prone skin, or those using other potentially irritating products (like retinoids or vitamin C serums), Duac’s gentler schedule is often the better choice. That said, some patients tolerate BenzaClin perfectly well—it depends on individual skin sensitivity and whether the twice-daily application fits your routine.
Practical Considerations—Which Dosing Schedule Works Better in Real Life?
The application frequency difference is more than just a numbers game—it significantly impacts how these products fit into actual daily life. BenzaClin requires morning and evening application, which means you need to cleanse, apply the medication, and wait for it to dry twice every day. For people with busy schedules, irregular sleep patterns, or who travel frequently, this can be a logistical burden. Forgetting the morning application or the evening application happens more often than you might expect, and inconsistent use directly reduces efficacy.
Duac’s once-daily bedtime application is simpler to remember and integrate into a routine. You cleanse at night, apply Duac as the last step in your skincare routine, and let it work overnight. This single daily application is also gentler on your skin throughout the day, since you’re not reapplying a potentially irritating medication during daylight hours when your skin might be exposed to sun, makeup, or environmental stressors. If you’re using other acne treatments or active ingredients (like vitamin C serum or niacinamide), Duac’s once-daily approach gives you more flexibility to use these products at different times without compounding irritation.
Antibiotic Resistance and Long-Term Use Considerations
One important concern with any topical antibiotic regimen is the potential for bacterial resistance to develop over time. This is why benzoyl peroxide is included in both formulations—it reduces the risk of *Propionibacterium acnes* developing resistance to clindamycin. However, neither BenzaClin nor Duac should be used as indefinite, long-term monotherapy for acne. Most dermatologists recommend using these combination products for 8-12 weeks as an initial treatment, then reassessing.
If you’ve been using BenzaClin or Duac for several months and your acne has plateaued or started worsening despite consistent use, discuss this with your dermatologist. It may indicate either that bacteria are becoming resistant to the clindamycin component (even with benzoyl peroxide present), or that another acne driver is at play. In these situations, your dermatologist might recommend switching to a different medication class, adding an oral antibiotic, or introducing a treatment like isotretinoin for severe cases. Don’t assume that increasing frequency or doubling up on applications will help—this typically just causes more irritation without improving efficacy.

Drug Interactions and Compatibility with Other Acne Treatments
BenzaClin and Duac are generally compatible with many other acne treatments, but timing and product selection matter. If you’re using benzoyl peroxide-based products elsewhere (like a benzoyl peroxide facial wash or spot treatment), you’re getting additional benzoyl peroxide exposure. This isn’t dangerous, but it increases irritation risk, so you may want to choose other cleansing or treatment products instead.
For patients using retinoids (like tretinoin or adapalene), which are also drying and irritating, starting with Duac instead of BenzaClin reduces the cumulative irritation burden. Antibiotics used orally (like doxycycline, minocycline, or amoxicillin) can be combined with topical clindamycin, and dermatologists sometimes do this for moderate acne. However, this approach increases antibiotic exposure and resistance risk, so it’s typically only used for a limited time. Always inform your dermatologist of any other medications or topical treatments you’re using so they can assess compatibility.
Finding the Right Treatment Plan Within Your Acne Management Strategy
Choosing between BenzaClin and Duac is just one piece of a comprehensive acne strategy. These medications work best when combined with gentle cleansing, appropriate moisturizing, and sun protection (benzoyl peroxide can increase sun sensitivity). Some dermatologists recommend starting with Duac for patient tolerability reasons, especially for first-time users of combination clindamycin-benzoyl peroxide therapy.
If Duac is well-tolerated but not providing adequate results after 12 weeks, switching to BenzaClin might offer the additional benefit of twice-daily exposure and faster results—though it increases irritation risk. The future of acne treatment is moving toward combination approaches and individualized medicine. As our understanding of acne pathophysiology deepens, dermatologists increasingly tailor treatment regimens to the specific drivers of each patient’s acne (bacterial overgrowth, sebum production, inflammation, follicular keratinization, or hormonal factors). BenzaClin and Duac remain effective tools in this arsenal, but they work best as part of a broader strategy that may include lifestyle modifications, dietary adjustments, skincare routines, and periodic reassessment with a healthcare provider.
Conclusion
BenzaClin and Duac are functionally equivalent medications—both contain 5% benzoyl peroxide and 1% clindamycin—with one key practical difference: frequency of application. BenzaClin’s twice-daily regimen and Duac’s once-daily bedtime application produce comparable clinical results, with both showing approximately 50-64% reduction in inflammatory acne lesions over 12 weeks. The choice between them should prioritize your lifestyle, skin sensitivity, and ability to maintain consistent use over the course of treatment.
For most patients, especially those new to combination topical antibiotics, Duac’s once-daily application offers better tolerability and convenience without sacrificing efficacy. However, if you have mild acne and can tolerate twice-daily application without significant irritation, BenzaClin may provide faster results due to more frequent dosing. Discuss your skin type, current routine, and acne severity with your dermatologist to determine which formulation makes sense for your situation. Whichever you choose, combine it with a gentle cleanser, appropriate moisturizer, and broad-spectrum sunscreen for optimal results and skin health.
You Might Also Like
- What iUNIK Beta-Glucan Serum Does for Acne Hydration
- What Zilxi Does for Inflammatory Rosacea That Looks Like Acne
- What Twyneo Does for Acne — Tretinoin Plus Niacinamide
Browse more: Acne | Acne Scars | Adults | Back | Blackheads





